Kidney Stones
View or Print All Sections
Definition & Facts
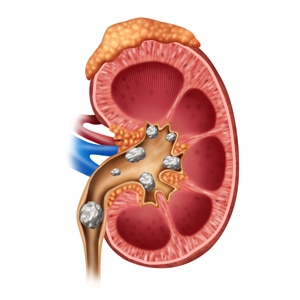
A kidney stone is a solid, pebble-like piece of material that can form in one or both of your kidneys when high levels of certain minerals are in your urine. Kidney stones rarely cause permanent damage if treated by a health care professional.
Symptoms & Causes
You may have a kidney stone if you feel a sharp pain in your back, side, lower abdomen, or groin; or have blood in your urine. If you have a small stone that easily passes through your urinary tract, you may not have symptoms at all.
Diagnosis
Health care professionals use your medical history, a physical exam, and tests to diagnose kidney stones. The tests may also be able to show problems that caused a kidney stone to form.
Treatment
Health care professionals may treat your kidney stones by removing the kidney stone or breaking it into small pieces. You may be able to prevent kidney stones by drinking enough water, changing the way you eat, or taking medicines.
Eating, Diet, & Nutrition
If you have kidney stones, drink lots of water unless otherwise directed by a health care professional. You may be able to prevent future kidney stones by making changes in how much sodium, animal protein, calcium, and oxalate you consume.
Clinical Trials
The National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) and other components of the National Institutes of Health (NIH) conduct and support research into many diseases and conditions.
Related Conditions & Diseases
Related Diagnostic Tests
The Urinary Tract & How it Works
The urinary tract is the body’s drainage system for removing urine, which is composed of wastes and extra fluid. In order for normal urination to occur, all body parts in the urinary tract need to work together in the correct order.
Additional Languages
This content is also available in:
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.

