Research Updates
Development of risk prediction equations for chronic kidney disease: Researchers from the NIDDK-funded Chronic Kidney Disease Prognosis Consortium (CKD-PC), including those from the NIDDK Phoenix Epidemiology and Clinical Research Branch, found that readily available demographic, clinical and laboratory data could be used to predict the risk of CKD. Using CKD-PC data, the researchers developed risk prediction equations from more than five million people in 34 cohorts worldwide to accurately determine five-year risk for CKD. The new algorithms use age, sex, race/ethnicity, history of cardiovascular disease, smoking history, hypertension, body mass index, kidney function values (for those without diabetes) and also HbA1c and diabetes medicines (for those with diabetes), to help identify people at increased risk of CKD. Early risk detection of CKD can lead to early prevention and intervention strategies. Further study is needed to determine whether use of these equations to identify people at risk of developing CKD will improve clinical care and patient outcomes. This research was published online in the Journal of the American Medical Association in November.
Pilot study tests doses of oral sodium bicarbonate supplementation in people with CKD: Some research suggests that oral sodium bicarbonate supplementation may preserve kidney function in patients with chronic kidney disease (CKD). However, research has not established the best dose to use in phase-3 trials seeking to answer this question. Researchers from the NIDDK-funded Bicarbonate Administration to Stabilize eGFR (BASE) study conducted a multicenter randomized, double-blind, placebo-controlled pilot study to assess the safety and effectiveness of two different doses of sodium bicarbonate – a higher dose, and a lower dose. The team found that both doses of the sodium bicarbonate were safe and could be used for subsequent studies. These findings were published in the Journal of the American Society of Nephrology in January.
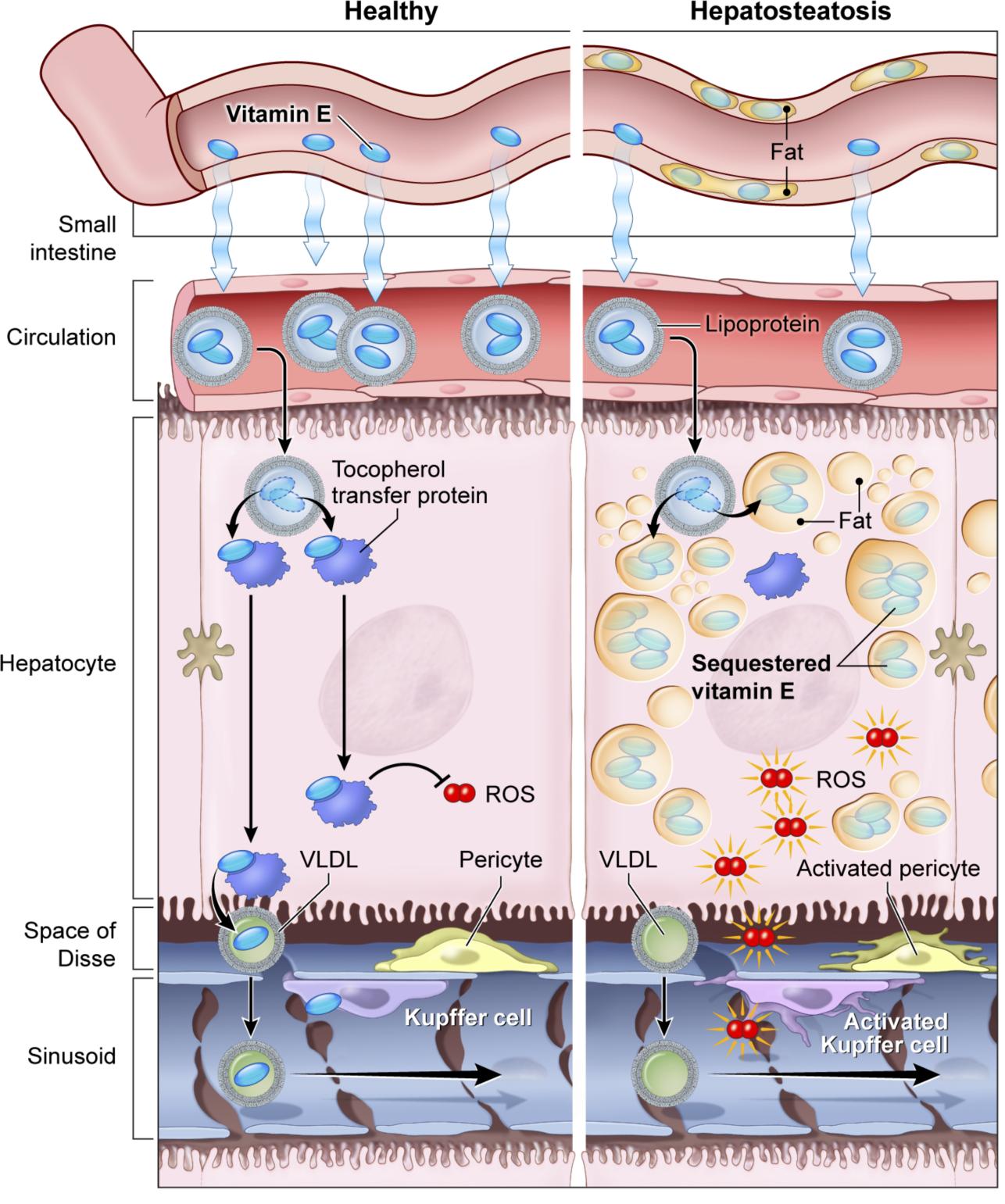
Fatty liver due to obesity could cause localized vitamin E deficiency: Extra fat in the liver, also called fatty liver, may interfere with tissue levels of fat-soluble vitamins such as vitamin E and has the potential to contribute to disease development, according to a recent NIDDK study. Researchers studied how vitamin E was brought into and released by the liver in healthy women and women with obesity and fatty liver. They found that while vitamin E was rapidly removed from circulation by the liver in both groups, the women who had fatty liver showed lower levels of vitamin E reentering the bloodstream, suggesting that excess fat in the liver stores vitamin E, making it less available within liver cells and for release. The researchers also measured fluorescently labeled vitamin E activity in human liver cells with excess fat and in mice with high fat diets. They saw that the labeled vitamin E was “trapped” in the fat in liver cells. Additional research is needed to evaluate the physiological effects of this type of localized vitamin deficiency and to better understand the role of vitamin E supplementation in fatty liver disease progression and prevention. This work was published in JCI Insight External link in December.
Impaired metabolic flexibility predicts future weight gain in healthy adults: Researchers from the NIDDK Phoenix Epidemiology and Clinical Research Branch and their collaborators found that people with impaired metabolic flexibility to high-fat overfeeding are more susceptible to weight gain over time. Metabolic flexibility is the ability to adapt metabolism according to the energy source (e.g., carbohydrates, fats, and protein) and is likely determined by genetics. The researchers assessed energy expenditure and other measures of metabolism in 79 healthy participants during various feeding scenarios, including 24-hour fasting and a high-fat overfeeding diet. These measurements assessed participants’ abilities to switch from carbohydrate metabolism to fat metabolism in a high-fat diet setting or vice-versa in a high-carbohydrate diet. The team found that participants who had the smallest changes in their metabolic rates during a 24-hour high-fat diet, suggesting their bodies did not promptly switch to fat-metabolism pathways, were the most likely to experience weight gain both six and 12 months later. Additionally, for the first time in humans, they showed that metabolic flexibility to different diets is highly consistent within a given person, suggesting that metabolic flexibility is an intrinsic characteristic that helps define an individual’s metabolic profile. This research was published in Diabetes in November.
NIH strategic plan details pathway to achieving hepatitis B cure: A new strategic plan from the National Institutes of Health outlines efforts to intensify ongoing hepatitis B research with the goals of developing a cure and improving scientific understanding of the virus while creating improved strategies for screening and treating patients. The Strategic Plan for Trans-NIH Research to Cure Hepatitis B (PDF, 624 KB) focuses on three key research areas: better understanding hepatitis B biology, development and sharing of tools and resources to support fundamental research and product development, and strategies to cure and prevent hepatitis B infection.
More kidneys from donors with acute kidney injury may be viable for transplantation: Many kidneys with acute kidney injury (AKI) are not used in transplants, but NIDDK-supported research finds they are as effective as kidneys without acute kidney injury. Researchers conducted a “virtual” clinical trial using donor and transplant registry data to compare 5-year kidney graft survival after transplantation from donors with and without AKI. They found that recipients of kidneys from deceased donors with AKI were at increased risk of delayed graft function, but the donor AKI status had no association with graft failure. More research and evaluation are necessary before changes occur in the recovery practices and use of kidneys with AKI, but this research suggests that potentially more kidneys could be available that have previously been discarded. This research was published in the Journal of the American Medical Association in January.
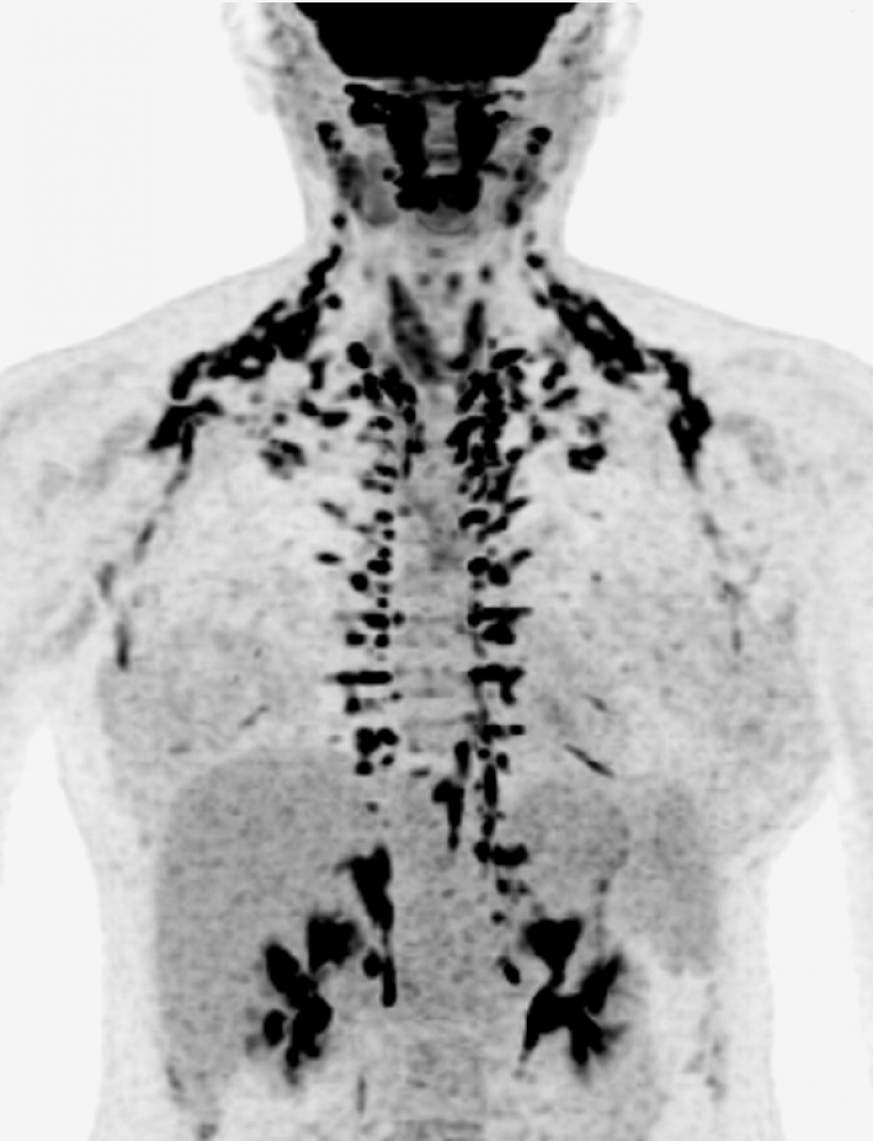
Drug increases brown fat activity in healthy women: A recent NIDDK study conducted at the National Institutes of Health found that chronic treatment with mirabegron, a drug approved to treat overactive bladder, activated brown fat in a small group of healthy women and had several other beneficial metabolic effects. Brown fat, or brown adipose tissue, is a form of fat that burns calories to generate heat. Fourteen women aged 18-40 of diverse ethnicities participated in the study at the NIH Clinical Center’s Metabolic Clinical Research Unit. For four weeks, each participant received daily doses of 100 mg of mirabegron, an amount exceeding the 50 mg maximum dosage approved by the U.S. Food and Drug Administration. At four weeks, the participants’ brown fat activity had more than doubled since the first day, though their body weight and body mass stayed the same. Other metabolic benefits included increased energy expenditure; higher levels of HDL (high-density lipoprotein) cholesterol — often referred to as “good” cholesterol — and bile acids, which help digest fats and regulate cholesterol; and improved regulation of blood glucose. The research, led by Aaron Cypess, M.D., Ph.D., from the Division of Intramural Research, was published in January in the Journal of Clinical Investigation.

Growth phases in early life associated with type 1 diabetes risk: Researchers from the NIDDK-funded The Environmental Determinants of Diabetes in the Young (TEDDY) study found that growth rates of infants and children at high genetic risk for type 1 diabetes (T1D) affected their risk of later developing pancreatic islet autoimmunity (IA) and eventually progressing to T1D. The international study team evaluated growth data from 7,522 children from the United States and Europe who had genetic risk factors for T1D, and found that those who developed IA had higher birth weight and a more rapid weight gain during infancy than those without IA. An increased risk of progressing from IA to T1D was observed among children who had a slower height growth rate during infancy and a faster height growth rate during early childhood. These results were published in Diabetes Care in January.
