Research Updates
NIDDK study describes physiologic relevance of surface protein receptors in human brown fat.

Using brown fat cells made from the deep neck fat of humans, the researchers found that beta-3-adrenergic receptors (beta-3-AR) play a critical role in regulating heat generation and fat metabolism. Beta-3-AR are protein receptors found on the surface of brown fat cells and are known to increase body temperature in rodents in response to cold. This study, which was published in JCI Insight in June, broadened understanding of the role of beta-3-AR in humans, and the findings suggest that drugs activating the beta-3-AR could help treat metabolic disorders.
To learn more, watch a video about the research with the study’s first author, NIDDK postdoctoral fellow Dr. Cheryl Cero.
Study finds sleep linked to academic achievement in adolescents.
An international research team, including scientists from NIDDK, found that Icelandic adolescents who went to bed earlier and had more consistent sleep schedules were more likely to have a higher combined score on standardized national examinations in Icelandic, English, and math. The study, which involved 103 male and 150 female 15-year-olds, analyzed whether the quantity, quality, consistency, and timing of sleep was associated with academic test performance. While males on average had later bedtimes than female participants, the results showed no clear differences between males and females in the relationships between sleep measures and exam scores. Unlike most previous studies of this age group, which have largely relied on self-reported measures, this exploratory study used wrist sensors to accurately measure sleep patterns and obtained standardized national test scores to quantify academic performance. The findings suggest the importance of early and consistent sleep schedules on adolescents’ academic performance. The study published in the Journal of Sleep Research in June.
Natural microbiome exposure in early life may help later curb obesity in mice.
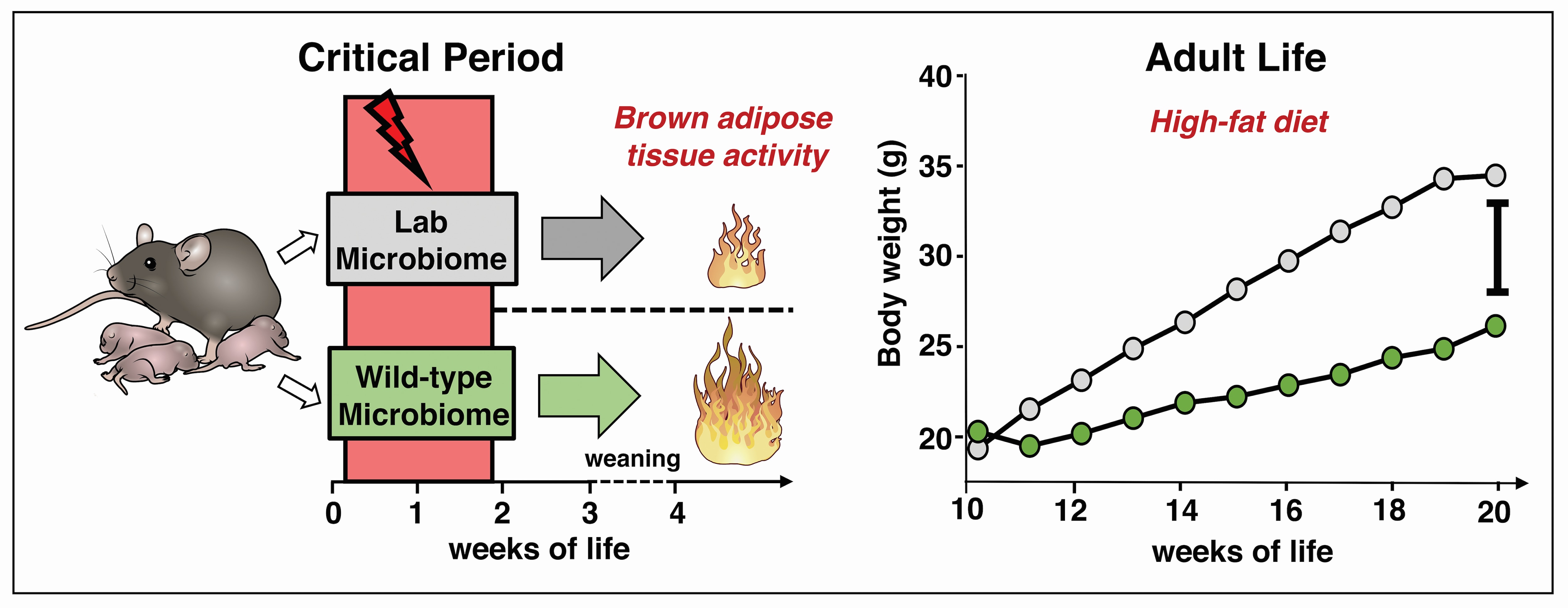
Researchers from NIDDK and the NIH’s National Cancer Institute found that mice exposed to a natural gut microbiome in the first few weeks of life may be more protected against excess weight gain later in life. Researchers used the wilding mouse model, a breed of mice with acquired microbes and pathogens of wild mice. (Read more about wildings on NIH’s news page). In this study, standard laboratory mice, who have had no natural microbiome exposure, were compared to wildlings, who were both fed a high fat diet for 10 weeks. Wildlings displayed significantly reduced weight gain compared to laboratory mice. Exposure to microbes in early life but not in adult life resulted in protection against excessive weight gain. Translation of these results to humans may help identify early-life treatments against obesity. This research published in the Journal of Nature Metabolism in August.
Airborne transmission of SARS-CoV-2 through speech a main contributor to rapid spread.

Earlier research by a team of NIDDK researchers and others found that speech-generated droplets are dispersed and suspended into the air and could carry a large amount of the SARS-CoV-2 virus in both those showing symptoms and asymptomatic individuals. This finding strongly implicates airborne transmission of the virus through talking as a main contributor to its spread. In their review, the NIDDK authors summarized the published research to-date on different modes of SARS-CoV-2 transmission, including breathing, speaking, coughing, and sneezing, to assess what primarily drives transmission of SARS-CoV-2. The researchers found strong evidence that airborne transmission of SARS-CoV-2 is the leading pathway for transmitting COVID-19, and that unmasked speech in confined spaces poses the greatest risk to people. This research published in the Journal of Internal Medicine in June. improvement in visual outcomes.
Largest study of type 1 diabetes genetics identifies new potential risk factors and drug targets.
In the largest and most ancestrally diverse analysis of type 1 diabetes genetics, conducted among 61,427 people with the disease, their relatives, and people without type 1 diabetes, researchers identified 78 regions in the genome that may affect risk, 36 of which were new. By integrating evidence from various types of analyses, the authors prioritized potential drug targets that could be tested for type 1 diabetes treatment or prevention. Some of these drugs are already used to treat autoimmune diseases and a few are also already being tested in clinical trials for type 1 diabetes. These findings were published in Nature Genetics in June.
Serious complications from youth-onset type 2 diabetes arise by young adulthood.
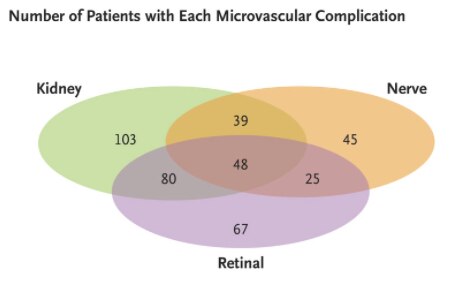
A recent NIDDK-supported study found that people with type 2 diabetes diagnosed during youth have a high risk of developing complications at early ages and have a greater chance of multiple complications within 15 years after diagnosis. Results from the Treatment Options for Type 2 Diabetes in Adolescents and Youth (TODAY) follow-up study show that 60% of participants had at least one diabetes-related complication such as heart disease, kidney disease, or diabetic foot complications, and nearly a third of participants had two or more complications after 15 years. The average age of participants after the TODAY2 follow-up was 26 years. TODAY2 involved 500 original participants from the 2004 TODAY study, which was the first major comparative effectiveness trial for the treatment of type 2 diabetes in youth. The findings were published in July in the New England Journal of Medicine.
NIDDK-supported research describes characteristics of type 1 diabetes diagnosed in youth between ages six and 12.

Researchers from the international The Environmental Determinants of Diabetes in the Young (TEDDY) study discovered that TEDDY participants who progressed to diabetes between age six and 12 were more likely to have autoantibodies to the pancreatic enzyme glutamic acid decarboxylase (GAD autoantibodies) while those developing the disease before age six more likely had first-appearing insulin autoantibodies (IA antibodies). In addition, the rate of progression to type 1 diabetes was slower in participants if multiple autoantibodies appeared after age six than if they were present before the age of six. Among children six and older with multiple autoantibodies, family history did not appear to have a role in whether the child progressed to diabetes. These findings were published in Diabetologia in July.
