Research Updates
Surgical and drug treatment options lead to similar outcomes for diabetic eye disease
 Andrew Antoszyk, M.D., with a patient. Image courtesy of Andrew Antoszyk
Andrew Antoszyk, M.D., with a patient. Image courtesy of Andrew Antoszyk
Surgical and injectable drug approaches are equally effective for treating bleeding inside the eye caused by proliferative diabetic retinopathy (PDR), according to a clinical study funded by NIDDK and other NIH institutes through the DRCR Retina Network (DRCR.net). PDR involves the growth of new, abnormal blood vessels in the light-sensing retina that are prone to bleeding, causing vision loss. Researchers compared anti-vascular endothelial growth factor (VEGF) eye injections versus removal of blood via vitrectomy surgery and laser photocoagulation. Both treatments improved central vision for the majority of participants during the two-year study, although approximately one-third of the participants eventually needed both anti-VEGF injections and surgery. The results, which will help guide treatment for people with PDR and bleeding inside the eye, were published in the Journal of the American Medical Association in December.
Combined risk score enhances prediction of type 1 diabetes among susceptible youth
Using a combination of known type 1 diabetes risk factors to create a person’s personal risk score better predicts the development of the disease in children, a recent NIDDK-funded study shows. Researchers from The Environmental Determinants of Diabetes in the Young (TEDDY) tested different risk-predicting mathematical models using data collected from 8,676 participants during the first 10 years of life. After comparing the predictive ability of the models, which used different combinations of risk factors such as age, genetic risk, family history, and environmental factors, the team determined that a three-factor model using a genetic risk score, family history, and autoantibodies performed best. While further validation is needed, the potential public health utility of screening infants to identify those at high risk and needing frequent evaluation prior to disease onset is significant. This research was published in Nature Medicine in August, and was selected as one of 2020’s top advances in genomic medicine by The American Journal of Human Genetics.
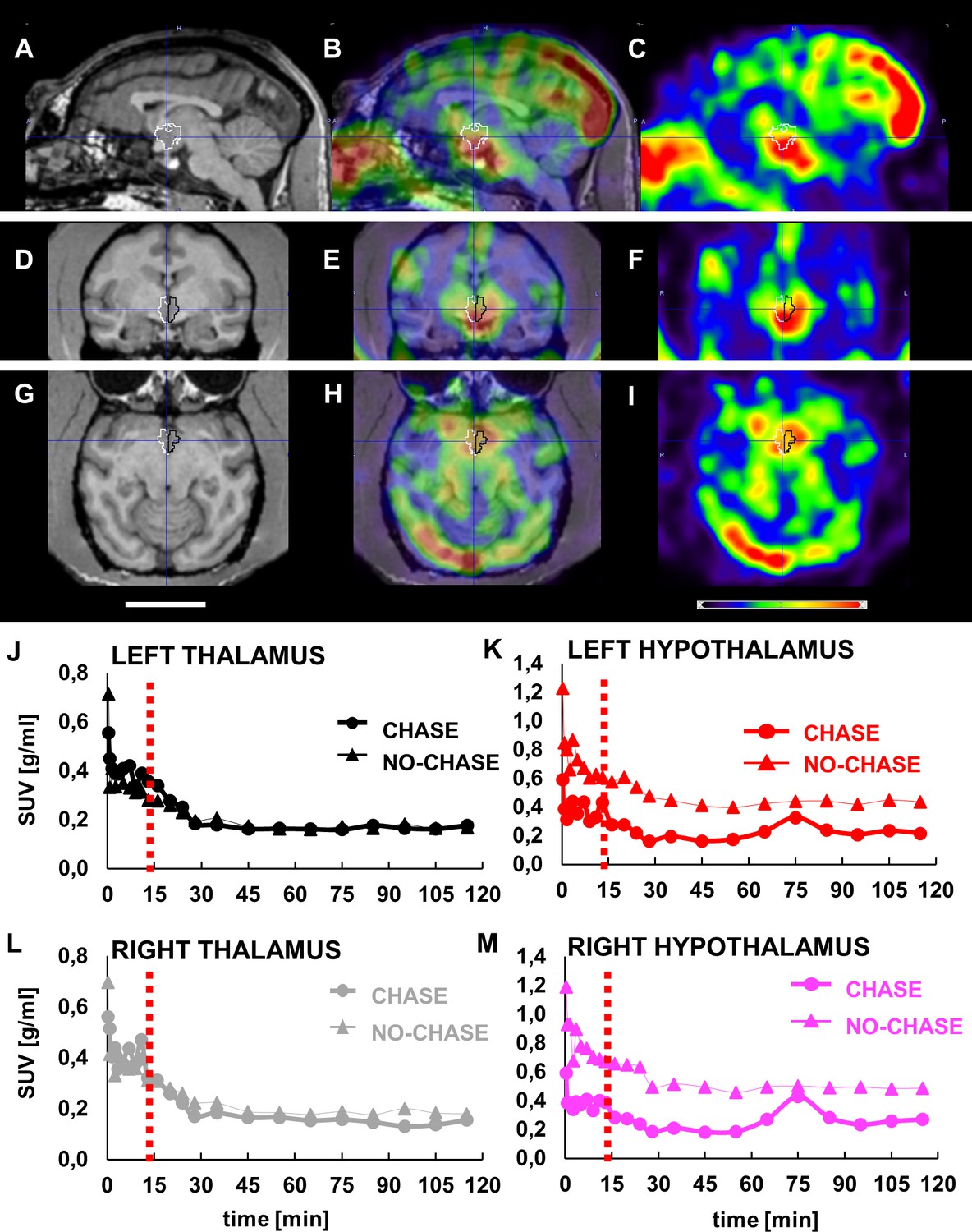
Hormone identified that suppresses hunger in primates and people
In a series of studies in primates and people, a team of researchers found that the hormone Lipocalin-2 (LCN2) suppresses appetite. First, the team examined how LCN2 functioned in people and found that among people of normal weight, blood levels of LCN2 increase after a meal, but among people with overweight or obesity, LCN2 levels were inconsistent, and sometimes decreased after a meal. LCN2 levels also correlated with feelings of hunger and fullness, with people showing increased levels of LCN2 when they felt more full after a meal. Then in primates, the researchers used imaging to look at LCN2 in the brain and saw that the hormone bound to the hypothalamus, the area in the brain that controls appetite and energy balance. The researchers also found that in lean primates who were given LCN2 the hormone acted as an appetite suppressant. The animals ate 20-30% less than when they were not given the hormone. Additional studies are needed to determine if LCN2 may have clinical use to treat obesity in humans. This research, supported through NIDDK funding, was published in eLife in November.
Study confirms gastrointestinal symptoms are common in youth with type 2 diabetes taking metformin
A team, led by scientists at NIDDK and Washington D.C.’s Children’s National Hospital, analyzed medical records of 488 adolescents with type 2 or prediabetes seen in an outpatient clinic from 2016-2019. In youth who visited the clinic twice in one year, the researchers also studied how gastrointestinal (GI) symptoms changed when metformin treatment began, was discontinued, or was switched from standard to extended release form. The results showed that metformin use in youth was associated with high rates of GI symptoms, such as diarrhea and abdominal pain. The prevalence of GI side effects was similar for both standard release and extended release metformin, a finding that, to the researchers’ knowledge, has not been previously reported. Published in Pediatric Diabetes in November, the study underscores the need for strategies to reduce GI symptoms in youth taking metformin, thereby improving quality of life and medication adherence. Metformin is the only oral medication approved by the U.S. Food and Drug Administration to treat type 2 diabetes in children.
Researchers propose that humidity from masks may lessen severity of COVID-19
 NIDDK’s Dr. Joseph Courtney breathes into sealed box to measure humidity of inhaled air.
NIDDK’s Dr. Joseph Courtney breathes into sealed box to measure humidity of inhaled air.A new study from NIDDK’s Laboratory of Chemical Physics found that face masks substantially increase the humidity of the air that the mask-wearer breathes in. The researchers tested four common types of masks: an N95 mask, a three-ply disposable surgical mask, a two-ply cotton-polyester mask, and a heavy cotton mask. All four masks increased the level of humidity of inhaled air, but to varying degrees. This higher level of humidity in inhaled air, the researchers suggest, could help explain documented findings showing that wearing masks is linked to lower disease severity in people infected with SARS-CoV-2, because hydration of the respiratory tract is known to promote clearance of inhaled particles from the lungs. The study, which published in February in the Biophysical Journal, adds evidence for yet another benefit of wearing masks to help combat respiratory diseases such as COVID-19. Watch a video about the research here.
NIH study compares low-fat, plant-based diet to low-carb, animal-based diet
View full-sized image Examples of dinners given to study participants: low-carb, animal-based diet (left) and low-fat, plant-based diet (right).People on a low-fat, plant-based diet ate fewer daily calories but had higher insulin and blood glucose (sugar) levels, compared to when they ate a low-carbohydrate, animal-based diet, according to a small but highly controlled study led by NIDDK researchers. The study compared the effects of the two diets on calorie intake, hormone levels, body weight, and more.
Examples of dinners given to study participants: low-carb, animal-based diet (left) and low-fat, plant-based diet (right).People on a low-fat, plant-based diet ate fewer daily calories but had higher insulin and blood glucose (sugar) levels, compared to when they ate a low-carbohydrate, animal-based diet, according to a small but highly controlled study led by NIDDK researchers. The study compared the effects of the two diets on calorie intake, hormone levels, body weight, and more.
In the study, 20 adults without diabetes spent four weeks in the NIH Clinical Center’s Metabolic Clinical Research Unit and received either a plant-based, low-fat diet or an animal-based, low-carbohydrate, ketogenic diet for two weeks, immediately followed by two weeks on the alternate diet. Participants ate 550 to 700 calories less per day on the low-fat diet than on the low-carb diet, but the low-carb diet resulted in lower and steadier insulin and blood glucose levels. Participants lost weight on both diets, but only the low-fat diet led to a significant loss of body fat. The findings, published in January in Nature Medicine, broaden understanding of how restricting dietary carbohydrates or fats may impact health.
NIH scientists identify nutrient that helps prevent bacterial infection in mice
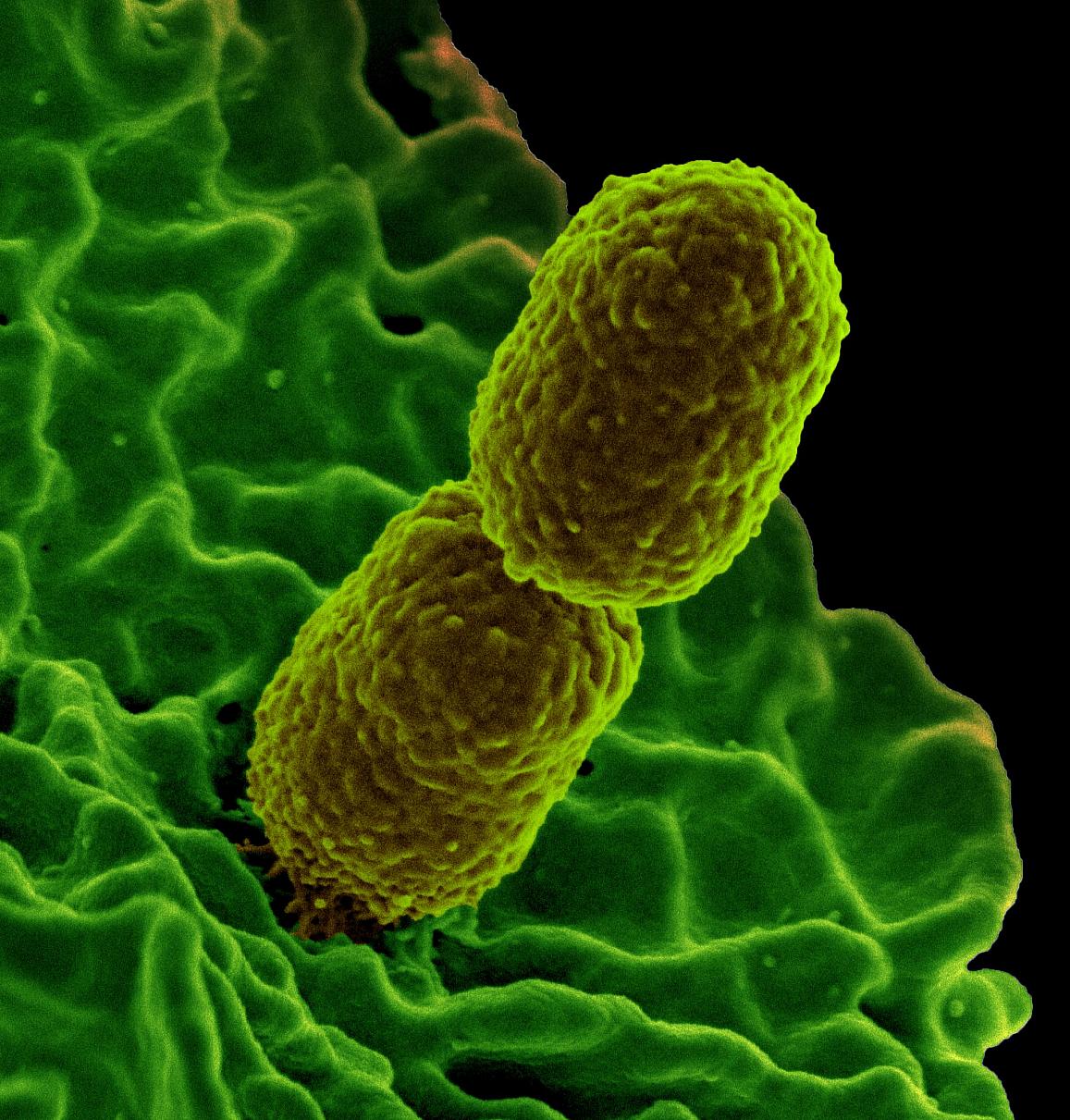 Colorized scanning electron micrograph showing carbapenem-resistant Klebsiella pneumoniae interacting with a human neutrophil. Credit: NIAID
Colorized scanning electron micrograph showing carbapenem-resistant Klebsiella pneumoniae interacting with a human neutrophil. Credit: NIAID
Scientists studying the body’s natural defenses against bacterial infection have identified a nutrient—taurine—that helps the gut recall prior infections and kill invading bacteria, such as Klebsiella pneumoniae (Kpn). The finding, published in the journal Cell by scientists from NIDDK and other NIH institutes could aid efforts seeking alternatives to antibiotics.
In this study, the scientists transferred gut microbiota that had experienced prior infection into germ-free mice and found that the transferred microbiotia helped prevent infection with Kpn. The team identified a class of bacteria — Deltaproteobacteria — involved in fighting these infections, and discovered taurine was the trigger for Deltaproteobacteria activity. The researchers found that a single mild infection is sufficient to prepare the microbiota to resist subsequent infection, and that the liver and gallbladder — which synthesize and store bile acids containing taurine — can develop long-term infection protection.
Earlier bariatric surgery more likely to result in long-term type 2 diabetes remission
NIDDK-supported research compared type 2 diabetes prevalence and remission rates seven years after Roux-en-Y gastric bypass and laparoscopic gastric banding among participants of the Longitudinal Assessment of Bariatric Surgery-2 (LABS-2) study. This follow-up study confirmed the initial study results, which showed that the likelihood of type 2 diabetes remission in those with severe obesity is greater when surgery is performed on younger individuals, soon after diabetes diagnosis, and among those whose diabetes is controlled with fewer medications and no insulin. The study also found that remission was more likely among those who undergo Roux-en-Y gastric bypass versus banding. The study was published online in December in the Journal of Clinical Endocrinology & Metabolism.
Health care spending reductions from intensive lifestyle programs did not persist after intervention stopped
A cost analysis of the NIDDK-funded Look AHEAD: Action for Health in Diabetes randomized clinical trial found that health care use and spending associated with an intensive lifestyle intervention for type 2 diabetes increased over time after the intervention ended. The Look AHEAD study, which evaluated the use of an intensive lifestyle intervention for weight loss and diabetes management in people with type 2 diabetes, initially showed that the intervention was associated with weight reduction, improved diabetes control, and a reduction in health care costs in participants during the study. However, four years after the study ended, there was no reduction in total health care spending among those who received the intervention compared to participants in the control group. These findings suggest that intensive lifestyle interventions targeted to patients with type 2 diabetes may need to be sustained to reduce long-term health care spending. The study was published in JAMA Open Network in November.