Hyperthyroidism (Overactive Thyroid)
On this page:
- What is hyperthyroidism?
- How common is hyperthyroidism?
- Who is more likely to develop hyperthyroidism?
- Is hyperthyroidism during pregnancy a problem?
- What are the complications of hyperthyroidism?
- What are the symptoms of hyperthyroidism?
- What causes hyperthyroidism?
- How do doctors diagnose hyperthyroidism?
- How do doctors treat hyperthyroidism?
- How does eating, diet, and nutrition affect hyperthyroidism?
- Clinical Trials for Hyperthyroidism
What is hyperthyroidism?
Hyperthyroidism, also called overactive thyroid, is when the thyroid gland makes more thyroid hormones than your body needs. The thyroid is a small, butterfly-shaped gland in the front of your neck. Thyroid hormones control the way the body uses energy, so they affect nearly every organ in your body, even the way your heart beats. With too much thyroid hormone, many of your body’s functions speed up.
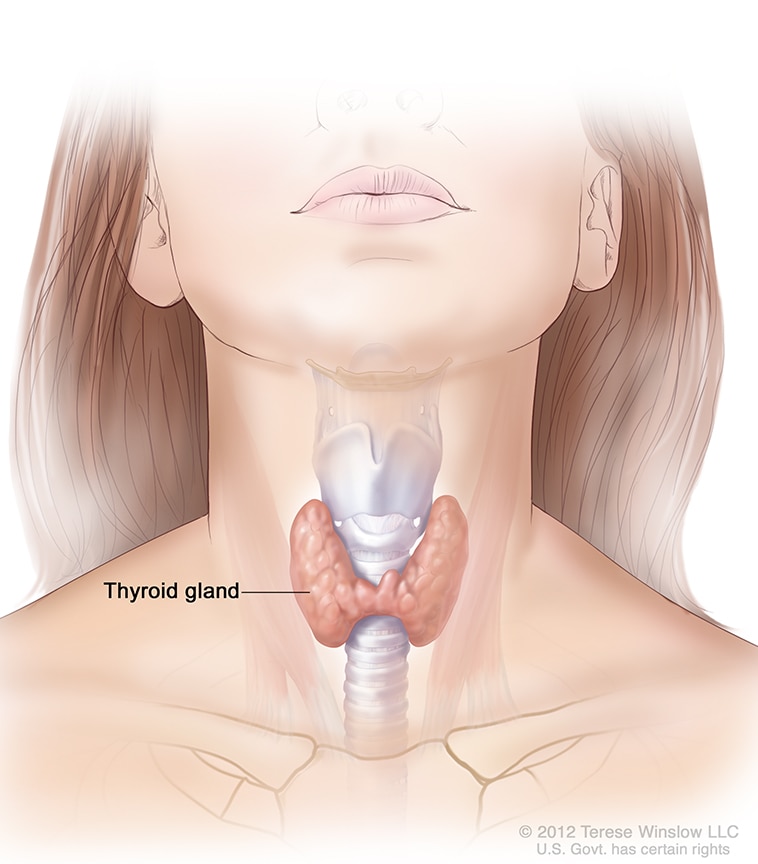 The thyroid is a small gland in your neck that makes thyroid hormones.
The thyroid is a small gland in your neck that makes thyroid hormones.
How common is hyperthyroidism?
About 1 out of 100 Americans ages 12 years and older have hyperthyroidism.1
Who is more likely to develop hyperthyroidism?
Hyperthyroidism is more common in women and people older than 60.2 You are more likely to have hyperthyroidism if you
- have a family history of thyroid disease
- have other health problems, including
- pernicious anemia, a condition caused by a vitamin B12 deficiency
- type 1 or type 2 diabetes
- primary adrenal insufficiency, a disorder of hormones
- eat large amounts of food containing iodine, such as kelp
- use medicines that contain iodine
- use nicotine products3
- were pregnant within the past 6 months
Is hyperthyroidism during pregnancy a problem?
Mild hyperthyroidism during pregnancy is usually not a problem. But severe hyperthyroidism during pregnancy, when untreated, can affect both the mother and the baby. If you have hyperthyroidism and plan to get pregnant or become pregnant, work with your doctor to get the disease under control.
 Be sure your hyperthyroidism is under control before becoming pregnant.
Be sure your hyperthyroidism is under control before becoming pregnant.What are the complications of hyperthyroidism?
Untreated, hyperthyroidism can cause serious health problems, including
- an irregular heartbeat that can lead to blood clots, stroke, heart failure, and other heart-related problems
- an eye disease called Graves’ ophthalmopathy
- thinning bones, osteoporosis, and muscle problems
- menstrual cycle and fertility issues
What are the symptoms of hyperthyroidism?
Symptoms of hyperthyroidism can vary from person to person and may include4
- weight loss despite an increased appetite
- rapid or irregular heartbeat
- nervousness, irritability, trouble sleeping, fatigue
- shaky hands, muscle weakness
- sweating or trouble tolerating heat
- frequent bowel movements
- an enlargement in the neck, called a goiter
In older adults, hyperthyroidism is sometimes mistaken for depression or dementia. Older adults may have different symptoms, such as loss of appetite or withdrawal from people, than younger adults with hyperthyroidism. You may want to ask your doctor about hyperthyroidism if you or your loved one shows these symptoms.
What causes hyperthyroidism?
Hyperthyroidism has several causes, including
- Graves’ disease
- overactive thyroid nodules
- inflammation of the thyroid gland, called thyroiditis
- too much iodine
- too much thyroid hormone medicine
- a noncancerous tumor of the pituitary gland
Graves’ disease
Graves’ disease, the most common cause of hyperthyroidism, is an autoimmune disorder. With this disease, your immune system attacks the thyroid and causes it to make too much thyroid hormone.
Overactive thyroid nodules
Overactive thyroid nodules, or lumps in your thyroid, are common and usually not cancerous. However, one or more nodules may become overactive and produce too much thyroid hormone. Overactive nodules are found most often in older adults.
Thyroiditis
Thyroiditis is inflammation of your thyroid gland. Some types of thyroiditis can cause thyroid hormone to leak out of your thyroid gland into your bloodstream. As a result, you may develop symptoms of hyperthyroidism.
The types of thyroiditis that can cause hyperthyroidism include
- subacute thyroiditis, which involves a painfully inflamed and enlarged thyroid.
- postpartum thyroiditis, which can develop after a woman gives birth.
- painless thyroiditis, which is similar to postpartum thyroiditis, but occurs in the absence of pregnancy. Your thyroid may be enlarged. Experts think painless thyroiditis is probably an autoimmune condition.
Thyroiditis can also cause symptoms of hypothyroidism, or underactive thyroid. In some cases, after your thyroid is overactive for a period of time, it may become underactive.
Too much iodine
Your thyroid uses iodine to make thyroid hormone. How much iodine you consume affects how much thyroid hormone your thyroid makes. In some people, consuming large amounts of iodine may cause the thyroid to make too much thyroid hormone.
Some cough syrups and medicines, including some heart medicines, may contain a lot of iodine. Seaweed and seaweed-based supplements also contain a lot of iodine.
Too much thyroid hormone medicine
Some people who take thyroid hormone medicine for hypothyroidism may take too much. If you take thyroid hormone medicine, see your doctor at least once a year to have your thyroid hormone levels checked. You may need to adjust your dose if your doctor finds your thyroid hormone level is too high.
Some other medicines may also interact with thyroid hormone medicine and raise hormone levels. If you take thyroid hormone medicine, ask your doctor about interactions when starting new medicines.
Noncancerous tumor
In some rare cases, a noncancerous tumor of the pituitary gland, located at the base of the brain, can cause hyperthyroidism.
How do doctors diagnose hyperthyroidism?
 A blood test might confirm a diagnosis of hyperthyroidism.
A blood test might confirm a diagnosis of hyperthyroidism.
Your doctor will take a medical history and perform a physical exam. A hyperthyroidism diagnosis can’t be based on symptoms alone because many of its symptoms are the same as those of other diseases. That’s why your doctor may use several thyroid blood tests and imaging tests to confirm the diagnosis and find its cause.
Because hyperthyroidism can cause fertility problems, women who have trouble getting pregnant often get tested for thyroid problems.
How do doctors treat hyperthyroidism?
Your doctor will treat your hyperthyroidism to bring your thyroid hormone levels back to normal. Treating the disease will prevent long-term health problems, and it will relieve uncomfortable symptoms. No single treatment works for everyone.
Your treatment depends on what’s causing your hyperthyroidism and how severe it is. When recommending a treatment, your doctor will consider
- your age
- possible allergies to or side effects of the medicines
- other conditions, such as pregnancy or heart disease
- whether you have access to an experienced thyroid surgeon
Treatment options
Hyperthyroidism is usually treated with medicines, radioiodine therapy, or thyroid surgery.
Beta-blockers
Beta-blockers are drugs that block the action of substances, such as adrenaline, on nerve cells. They cause blood vessels to relax and widen.
- Pros
- They can reduce symptoms—such as tremors, rapid heartbeat, and nervousness—until other treatments start working.
- They can make you feel better within hours.
- Cons
- They don’t stop thyroid hormone production.
Antithyroid medicines
Antithyroid therapy is the simplest way to treat hyperthyroidism. Methimazole is used most often. Propylthiouracil is often used for women during the first 3 months of pregnancy because methimazole can, on rare occasions, harm the fetus.
- Pros
- They cause the thyroid to make less thyroid hormone.
- Some patients’ symptoms from Graves’ disease may go away temporarily after taking antithyroid drugs.
- Cons
- Antithyroid medicines can cause side effects, including
- allergic reactions, such as rashes and itching
- a decrease in the number of white blood cells in your body, which can lower resistance to infection
- liver failure, in rare cases
- Antithyroid medicines
- don’t provide a permanent cure, but they may allow symptoms to go away temporarily in the case of Graves’ disease
- may take several weeks or months for thyroid hormone levels to move into the normal range
- take about 1–2 years of total average treatment time, but can continue for many years
- are not used to treat hyperthyroidism caused by thyroiditis
- Antithyroid medicines can cause side effects, including
Seek care right away
 Antithyroid therapy is the easiest way to treat hyperthyroidism.
Antithyroid therapy is the easiest way to treat hyperthyroidism.
Call your doctor right away if you have any of the following symptoms
- fatigue or weakness
- dull pain in your abdomen
- loss of appetite
- skin rash, itching, or easy bruising
- yellowing of your skin or whites of your eyes, called jaundice
- constant sore throat
- fever, chills, or constant sore throat
Radioiodine therapy is a common and effective treatment. You can take radioactive iodine-131 by mouth as a capsule or liquid.
 Taking radioactive iodine-131 is a common and effective treatment.
Taking radioactive iodine-131 is a common and effective treatment.
- Pros
- Radioiodine therapy slowly destroys the cells of the thyroid gland that produce thyroid hormone.
- Radioiodine therapy does not affect other body tissues.
- Cons
- You might need more than one treatment to bring thyroid hormone levels into the normal range, but beta-blockers can control symptoms between treatments.
- Radioiodine therapy isn’t used for women who are pregnant or breastfeeding. It can harm the fetus’ thyroid and can be passed from mother to child in breast milk.
Almost everyone who gets radioiodine therapy later develops hypothyroidism. But hypothyroidism is easier to treat than hyperthyroidism by using a daily thyroid hormone medicine, and it causes fewer long-term health problems.
Surgery to remove part or most of the thyroid gland is used less often to treat hyperthyroidism. Sometimes doctors use surgery to treat people with large goiters or pregnant women who cannot take antithyroid medicines.
 In some cases, doctors use surgery to remove part or most of the thyroid gland.
In some cases, doctors use surgery to remove part or most of the thyroid gland.- Pros
- When part of the thyroid is removed, your thyroid hormone levels may return to normal.
- Cons
- Thyroid surgery requires general anesthesia, which can cause a condition called thyroid storm—a sudden, severe worsening of symptoms. Taking antithyroid medicines before surgery can help prevent this problem.
When part of your thyroid is removed, you may develop hypothyroidism after surgery and need to take thyroid hormone medicine. If your whole thyroid is removed, you will need to take thyroid hormone medicine for life. After surgery, your doctor will continue to check your thyroid hormone levels.
Researchers are looking into new ways to treat hyperthyroidism. An example is radiofrequency ablation (RFA), a new approach to treating thyroid nodules that cause hyperthyroidism.5,6 RFA is used mainly in cases where medicines or surgery won’t help, and is not yet widely available.
How does eating, diet, and nutrition affect hyperthyroidism?
Your thyroid uses iodine to make thyroid hormones. If you have Graves’ disease or another autoimmune thyroid disorder, you may be sensitive to harmful side effects from iodine. Eating foods that have large amounts of iodine—such as kelp, dulse, or other kinds of seaweed—may cause or worsen hyperthyroidism. Taking iodine supplements can have the same effect. Talk with members of your health care team about
- what foods to limit or avoid
- any iodine supplements you take
- any cough syrups or multivitamins you take because they may contain iodine
Clinical Trials for Hyperthyroidism
The NIDDK conducts and supports clinical trials in many diseases and conditions, including endocrine diseases. The trials look to find new ways to prevent, detect, or treat disease and improve quality of life.
What are clinical trials for hyperthyroidism?
Clinical trials—and other types of clinical studies—are part of medical research and involve people like you. When you volunteer to take part in a clinical study, you help doctors and researchers learn more about disease and improve health care for people in the future.
Researchers are studying many aspects of hyperthyroidism, such as its natural history, clinical presentation, and genetics.
Find out if clinical studies are right for you.
Watch a video of NIDDK Director Dr. Griffin P. Rodgers explaining the importance of participating in clinical trials.
What clinical studies for hyperthyroidism are looking for participants?
You can view a filtered list of clinical studies on hyperthyroidism that are open and recruiting at www.ClinicalTrials.gov. You can expand or narrow the list to include clinical studies from industry, universities, and individuals; however, the NIH does not review these studies and cannot ensure they are safe. Always talk with your health care provider before you participate in a clinical study.
References
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
The NIDDK would like to thank:
Thanh D. Hoang, D.O., FACP, FACE, CAPTAIN (select), Walter Reed National Military Medical Center
