Link to Source page: /health-information/kidney-disease/lupus-nephritis
Current page state: This syndication page is Published
Lupus Nephritis
On this page:
- What is lupus nephritis?
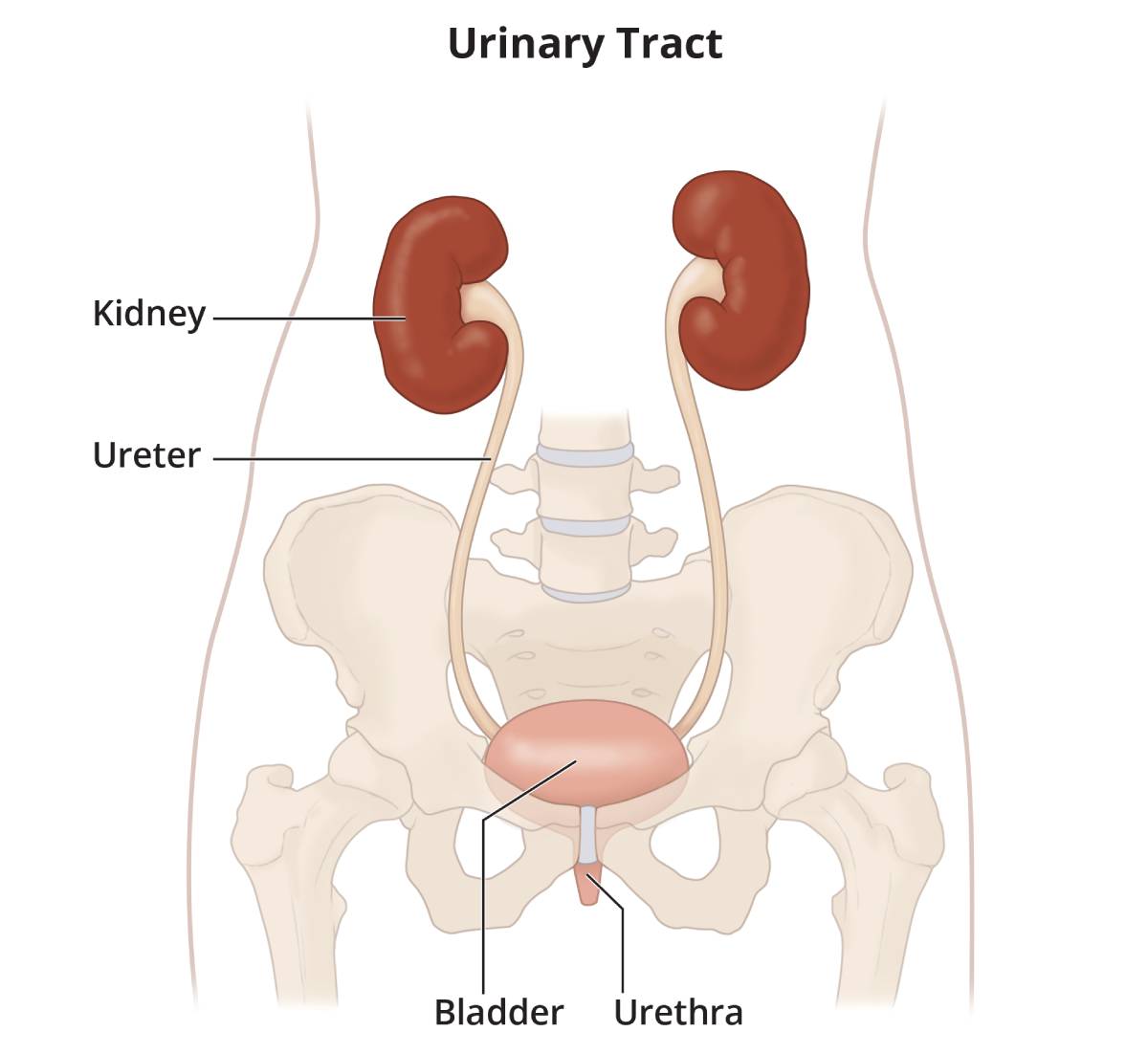
- What do your kidneys do?
- Who gets lupus?
- How common is lupus nephritis?
- Who is more likely to develop lupus nephritis?
- What are the symptoms of lupus nephritis?
- What tests do health care professionals use to diagnose lupus nephritis?
- How do doctors treat lupus nephritis?
- What should I eat if I have lupus nephritis?
- What are the complications of lupus nephritis?
- Clinical Trials
What is lupus nephritis?
Lupus nephritis is a type of kidney disease caused by systemic lupus erythematosus (SLE or lupus). Lupus is an autoimmune disease—a disorder in which the body’s immune system attacks the body’s own cells and organs. Kidney disease caused by lupus may get worse over time and lead to kidney failure. If your kidneys fail, you will need dialysis or a kidney transplant to maintain your health.
Who gets lupus?
Lupus is much more common in women than in men and most often strikes during the child-bearing years. Nine out of 10 people who have lupus are women. Lupus is also more common in people of African or Asian background. African Americans and Asian Americans are about 2 to 3 times more likely to develop lupus than Caucasians.1 In the United States, 1 out of every 250 African American women will develop lupus.2
How common is lupus nephritis?
Kidney damage is one of the more common health problems caused by lupus. In adults who have lupus, as many as 5 out of 10 will have kidney disease. In children who have lupus, 8 of 10 will have kidney disease.3
Who is more likely to develop lupus nephritis?
African Americans, Hispanics/Latinos, and Asian Americans are more likely to develop lupus nephritis than Caucasians.4 Lupus nephritis is more common in men than in women.5
What are the symptoms of lupus nephritis?
The symptoms of lupus nephritis may include foamy urine and edema—swelling that occurs when your body has too much fluid, usually in the legs, feet, or ankles, and less often in the hands or face. You may also develop high blood pressure.
Kidney problems often start at the same time or shortly after lupus symptoms appear and can include
- joint pain or swelling
- muscle pain
- fever with no known cause
- a red rash, often on the face, across the nose and cheeks, sometimes called a butterfly rash because of its shape

What tests do health care professionals use to diagnose lupus nephritis?
Lupus nephritis is diagnosed through urine and blood tests and a kidney biopsy.
Urine Test
Your health care professional uses a urine sample to look for blood and protein in your urine. You collect the urine sample in a container in a health care professional’s office or lab. For the test, a nurse or technician places a strip of chemically treated paper, called a dipstick, into the urine. Patches on the dipstick change color when blood or protein is present. A high level of protein or a high number of red blood cells in the urine means kidney damage. The urine will also be examined under a microscope to look for kidney cells.
Blood Test
Your health care professional uses a blood test to check your kidney function. The blood test measures creatinine, a waste product from the normal breakdown of muscles in your body. Your kidneys remove creatinine from your blood. Health care professionals use the amount of creatinine in your blood to estimate your glomerular filtration rate (GFR). As kidney disease gets worse, the level of creatinine goes up.
Read more about blood and urine tests for kidney disease.
Kidney Biopsy
A kidney biopsy is a procedure that involves taking a small piece of kidney tissue for examination under a microscope. A doctor performs the biopsy in a hospital using imaging techniques such as ultrasound or a computed tomography (CT) scan to guide the biopsy needle into the kidney. Health care professionals numb the area to limit pain and use light sedation to help you relax during the procedure.
The kidney tissue is examined in a lab by a pathologist—a doctor who specializes in diagnosing diseases.
A kidney biopsy can
- confirm a diagnosis of lupus nephritis
- find out how far the disease has progressed
- guide treatment
The American College of Rheumatology recommends biopsies for people with signs of active lupus nephritis who have not yet been treated.3 Early diagnosis and prompt treatment may help protect your kidneys.
How do doctors treat lupus nephritis?
Health care professionals treat lupus nephritis with medicines that suppress your immune system so it stops attacking and damaging your kidneys. Goals of treatment are to
- reduce inflammation in your kidneys
- decrease immune system activity
- block your body’s immune cells from attacking the kidneys directly or making antibodies that attack the kidneys
Medicines
Your health care professional may prescribe a corticosteroid, usually prednisone, and a medicine to suppress your immune system, such as cyclophosphamide or mycophenolate mofetil, and hydroxychloroquine, a medicine for people who have SLE.
Lupus nephritis can cause high blood pressure in some people. You may need more than one kind of medicine to control your blood pressure. Blood pressure medicines include:
- ACE inhibitors and ARBs, with drug names that end in –pril or –sartan.
- diuretics
- beta blockers
- calcium channel blockers
ACE inhibitors and ARBs may help protect your kidneys, and diuretics help your kidneys remove fluid from your body.
Read more about medicines and treatment for high blood pressure.

What should I eat if I have lupus nephritis?
If you have kidney disease, you may need to change what you eat. Dietitians are nutrition experts who can advise you about healthy eating and meal planning. Find a registered dietitian who can help you. Eating the right foods can help you manage your kidney disease. If you have high blood pressure, eating foods with less sodium (a part of salt) may help you lower your blood pressure.
Read more about eating right for chronic kidney disease.

What are the complications of lupus nephritis?
Treatment works well to control lupus nephritis, so you may not have complications.
Between 10 to 30 percent of people who have lupus nephritis develop kidney failure.6 Learn more about what happens if your kidneys fail.
The most severe form of lupus nephritis, called diffuse proliferative nephritis, can cause scars to form in the kidneys. Scars are permanent, and kidney function often declines as more scars form. Early diagnosis and treatment may help prevent long-lasting damage.
People who have lupus nephritis are at a high risk for cancer, primarily B-cell lymphoma—a type of cancer that begins in the cells of the immune system. They are also at a high risk for heart and blood vessel problems.
References
Clinical Trials
The National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) and other components of the National Institutes of Health (NIH) conduct and support research into many diseases and conditions.
What are clinical trials, and are they right for you?
Clinical trials are part of clinical research and at the heart of all medical advances. Clinical trials look at new ways to prevent, detect, or treat disease. Researchers also use clinical trials to look at other aspects of care, such as improving the quality of life for people with chronic illnesses. Find out if clinical trials are right for you.
What clinical trials are open?
Clinical trials that are currently open and are recruiting can be viewed at www.ClinicalTrials.gov.
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
The NIDDK would like to thank:
The National Institute of Arthritis and Musculoskeletal and Skin Diseases