Definition & Facts of Intestinal Pseudo-obstruction
In this section:
- What is intestinal pseudo-obstruction?
- Are there different types of intestinal pseudo-obstruction?
- How common is intestinal pseudo-obstruction?
- Who is more likely to have intestinal pseudo-obstruction?
- What are the complications of intestinal pseudo-obstruction?
What is intestinal pseudo-obstruction?
Intestinal pseudo-obstruction is a rare condition in which you have symptoms of intestinal obstruction, but doctors can’t find anything blocking your intestines. In intestinal pseudo-obstruction, nerve or muscle problems slow or stop the movement of food, fluid, air, and waste through your intestines.
The intestines are part of the digestive tract and are made up of the
- small intestine, which includes the duodenum, jejunum, and ileum. Most food digestion and nutrient absorption happen in your small intestine.
- large intestine, which includes the appendix, cecum, colon, and rectum. The large intestine takes in water from stool and changes stool from a liquid to a solid form.
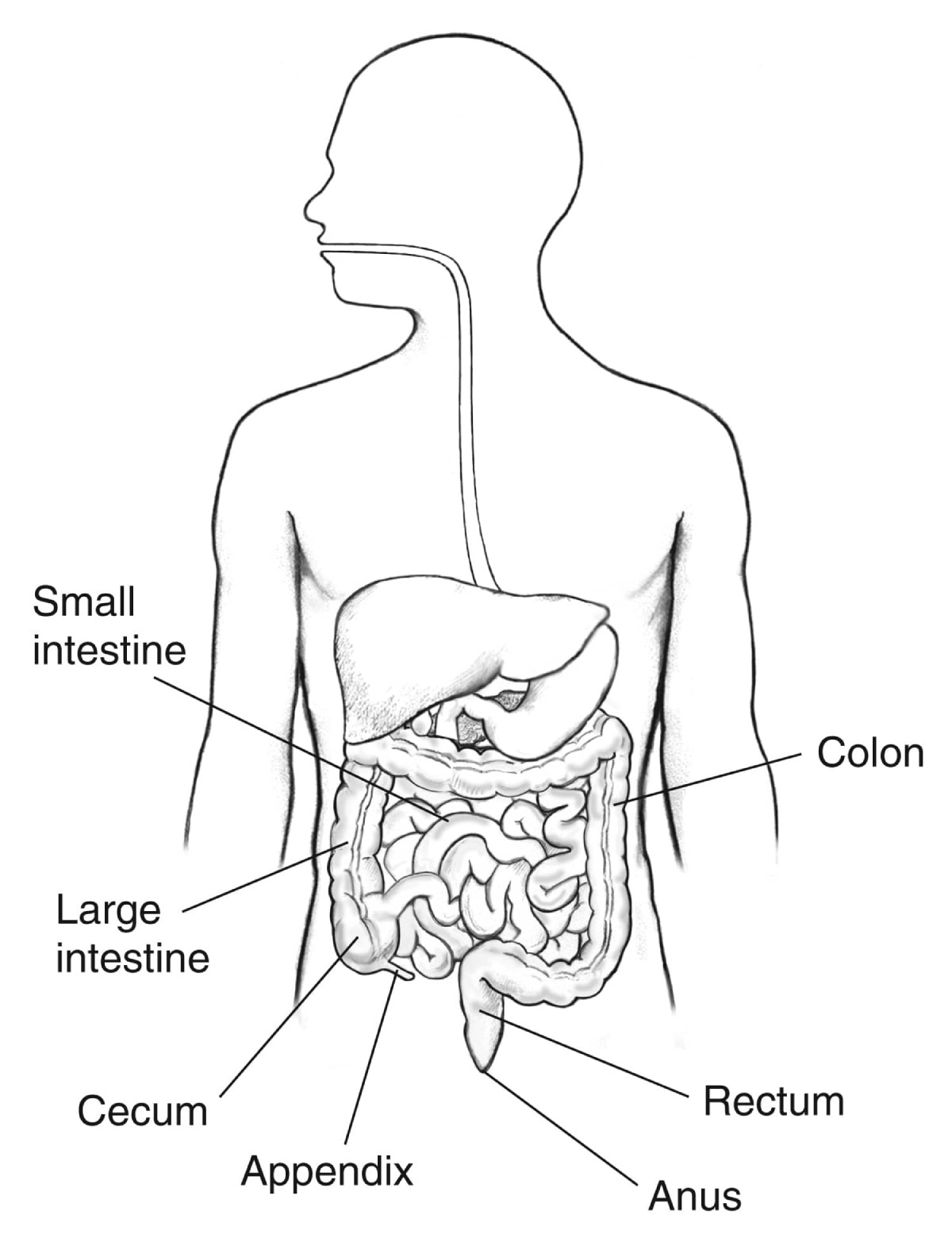 The gastrointestinal tract
The gastrointestinal tract
Are there different types of intestinal pseudo-obstruction?
The two main types of intestinal pseudo-obstruction are chronic intestinal pseudo-obstruction and acute colonic pseudo-obstruction.
Chronic intestinal pseudo-obstruction
Chronic intestinal pseudo-obstruction lasts a long time. This condition most often affects the small intestine or the colon, but it may affect other parts of the digestive tract, such as the stomach or esophagus.
Experts group chronic intestinal pseudo-obstruction into primary and secondary forms, depending on its cause.
Acute colonic pseudo-obstruction
Acute colonic pseudo-obstruction occurs suddenly and lasts a short time. This condition affects the colon. Other names for this condition include Ogilvie syndrome and colonic ileus.
How common is intestinal pseudo-obstruction?
Intestinal pseudo-obstruction is rare, and finding out how many people have it is difficult.
In the United States, research suggests that about 100 infants are born with chronic intestinal pseudo-obstruction each year.1 Research conducted in Japan found that about 8 to 10 out of every 1 million people have chronic intestinal pseudo-obstruction.1 Experts don’t know how many teens or adults experience chronic intestinal pseudo-obstruction unrelated to symptoms in infancy, or the first year of life.
Experts think that about 100 out of every 100,000 people admitted to the hospital develop acute colonic pseudo-obstruction.2
Who is more likely to have intestinal pseudo-obstruction?
Chronic intestinal pseudo-obstruction can occur in people of any age, but it most often occurs in children and young adults. In about 80% of cases, chronic intestinal pseudo-obstruction starts to cause symptoms in the first year of life.3,4
Acute colonic pseudo-obstruction is more common in older adults. The condition most often occurs in people who are hospitalized for another reason, such as severe illness, injury, or surgery.
What are the complications of intestinal pseudo-obstruction?
Chronic intestinal pseudo-obstruction and acute colonic pseudo-obstruction may lead to different complications.
Chronic intestinal pseudo-obstruction
Over time, chronic intestinal pseudo-obstruction may lead to
- malnutrition and weight loss.
- small intestinal bacterial overgrowth, an increase in the number of bacteria or a change in the type of bacteria in the small intestine. This bacterial overgrowth can affect the small intestine’s ability to absorb nutrients, including fat and fat-soluble vitamins A, D, E, and K.
- intestinal failure, which means the small intestine can’t absorb enough nutrients and water to maintain health or support growth.
Acute colonic pseudo-obstruction
Acute colonic pseudo-obstruction may cause severe swelling of the colon, which can lead to complications such as
- lack of blood flow to part of the colon.
- a perforation, or hole, in the wall of the colon. A perforation can allow the contents of the colon to spill into the abdominal cavity, which may lead to peritonitis—an infection of the lining of the abdominal cavity. Peritonitis may sometimes spread to the bloodstream, which can be life threatening.
References
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
