Anemia of Inflammation or Chronic Disease
On this page:
- What is anemia of inflammation?
- Why is anemia of inflammation also called anemia of chronic disease?
- Are there other types of anemia?
- How common is anemia of inflammation?
- Who is more likely to have anemia of inflammation?
- Does anemia of inflammation lead to other health problems?
- What are the symptoms of anemia of inflammation?
- What causes anemia of inflammation?
- Chronic conditions that cause anemia of inflammation
- Other causes of inflammation that may lead to anemia
- How do health care professionals diagnose anemia of inflammation?
- How do health care professionals treat anemia of inflammation?
- Can I prevent anemia of inflammation?
- How does eating, diet, and nutrition affect anemia of inflammation?
- Clinical Trials for Anemia of Inflammation
- What are clinical trials for anemia of inflammation?
- What clinical studies for anemia of inflammation are looking for participants?
What is anemia of inflammation?
Anemia of inflammation, also called anemia of chronic disease or ACD, is a type of anemia that affects people who have conditions that cause inflammation, such as infections, autoimmune diseases, cancer, and chronic kidney disease (CKD).
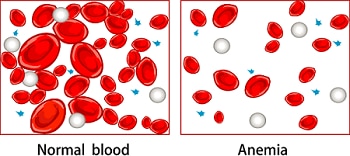
Anemia is a condition in which your blood has fewer red blood cells than normal. Your red blood cells may also have less hemoglobin than normal. Hemoglobin is the iron-rich protein that allows red blood cells to carry oxygen from your lungs to the rest of your body. Your body needs oxygen to work properly. With fewer red blood cells or less hemoglobin, your body may not get enough oxygen.
In anemia of inflammation, you may have a normal or sometimes increased amount of iron stored in your body tissues, but a low level of iron in your blood. Inflammation may prevent your body from using stored iron to make enough healthy red blood cells, leading to anemia.
Why is anemia of inflammation also called anemia of chronic disease?
Anemia of inflammation is also called anemia of chronic disease because this type of anemia commonly occurs in people who have chronic conditions that may be associated with inflammation.
Are there other types of anemia?
There are many types of anemia. Common types include
- iron-deficiency anemia, a condition in which the body’s stored iron is used up, causing the body to make fewer healthy red blood cells. In people with iron-deficiency anemia, iron levels are low in both body tissues and the blood. This is the most common type of anemia.
- pernicious anemia, which is caused by a lack of vitamin B12.
- aplastic anemia, a condition in which the bone marrow doesn’t make enough new red blood cells, white blood cells, and platelets because the bone marrow’s stem cells are damaged.
- hemolytic anemia, a condition in which red blood cells are destroyed earlier than normal.
How common is anemia of inflammation?
Anemia of inflammation is the second most common type of anemia, after iron-deficiency anemia.1
Who is more likely to have anemia of inflammation?
While anemia of inflammation can affect people of any age, older adults are more likely to have this type of anemia because they are more likely to have chronic diseases that cause inflammation. In the United States, about 1 million people older than age 65 have anemia of inflammation.2
Does anemia of inflammation lead to other health problems?
Anemia of inflammation is typically mild or moderate, meaning that hemoglobin levels in your blood are lower than normal but not severely low. If your anemia becomes severe, the lack of oxygen in your blood can cause symptoms, such as feeling tired or short of breath. Severe anemia can become life-threatening.
In people who have CKD, severe anemia can increase the chance of developing heart problems.
What are the symptoms of anemia of inflammation?
Anemia of inflammation typically develops slowly and may cause few or no symptoms. In fact, you may only experience symptoms of the disease that is causing anemia and not notice additional symptoms.
Symptoms of anemia of inflammation are the same as in any type of anemia and include
- a fast heartbeat
- body aches
- fainting or feeling dizzy or light-headed
- feeling tired or weak
- getting tired easily during or after physical activity
- pale skin
- shortness of breath
What causes anemia of inflammation?
Experts think that when you have an infection or disease that causes inflammation, your immune system causes changes in how your body works that may lead to anemia of inflammation.
- Your body may not store and use iron normally.
- Your kidneys may produce less erythropoietin (EPO), a hormone that signals your bone marrow—the spongy tissue inside most of your bones—to make red blood cells.
- Your bone marrow may not respond normally to EPO, making fewer red blood cells than needed.
- Your red blood cells may live for a shorter time than normal, causing them to die faster than they can be replaced.
Chronic conditions that cause anemia of inflammation
Many different chronic conditions can cause inflammation that leads to anemia, including
- autoimmune diseases, such as rheumatoid arthritis or lupus
- cancer
- chronic infections, such as HIV/AIDS and tuberculosis
- CKD
- inflammatory bowel disease (IBD), such as Crohn’s disease or ulcerative colitis
- other chronic diseases that involve inflammation, such as diabetes and heart failure
In people with certain chronic conditions, anemia may have more than one cause. For example
- Causes of anemia in CKD may include inflammation, low levels of EPO due to kidney damage, or low levels of the nutrients needed to make red blood cells. Hemodialysis to treat CKD may also lead to iron-deficiency anemia.
- People with IBD may have both iron-deficiency anemia due to blood loss and anemia of inflammation.
- In people who have cancer, anemia may be caused by inflammation, blood loss, and cancers that affect or spread to the bone marrow. Cancer treatments such as chemotherapy and radiation therapy may also cause or worsen anemia.
Other causes of inflammation that may lead to anemia
While anemia of inflammation typically develops slowly, anemia of critical illness is a type of anemia of inflammation that develops quickly in patients who are hospitalized for severe acute infections, trauma, or other conditions that cause inflammation.
In some cases, older adults develop anemia of inflammation that is not related to an underlying infection or chronic disease. Experts think that the aging process may cause inflammation and anemia.
How do health care professionals diagnose anemia of inflammation?
Health care professionals use a medical history and blood tests to diagnose anemia of inflammation.
Medical history
A health care professional will ask about your history of infections or chronic diseases that may lead to anemia of inflammation.
Blood tests
Health care professionals use blood tests to check for signs of anemia of inflammation, other types of anemia, or other health problems. A health care professional will take a blood sample from you and send the sample to a lab to test.
Blood count tests can check many parts and features of your blood, including
- the number of red blood cells
- the average size of red blood cells
- the amount of hemoglobin in your blood and in your red blood cells
- the number of developing red blood cells, called reticulocytes, in your blood
Some of these blood count tests and others may be combined in a test called a complete blood count. A blood smear may be used to examine the size, shape, and number of red blood cells in your blood.
A health care professional may also use blood tests to check the amount of iron in your blood and stored in your body. These tests may measure
- iron in your blood
- transferrin, a protein in your blood that carries iron
- ferritin, the protein that stores iron in your body’s cells
A health care professional may diagnose anemia of inflammation if blood test results suggest that you have anemia, a low level of iron in your blood, and a normal level of iron stored in your body tissues.
If blood test results suggest you have anemia of inflammation but the cause is unknown, a health care professional may perform additional tests to look for the cause.

How do health care professionals treat anemia of inflammation?
Health care professionals treat anemia of inflammation by treating the underlying condition and by treating the anemia with medicines and occasionally with blood transfusions.
Treating the underlying condition
Health care professionals typically treat anemia of inflammation by treating the underlying condition that is causing inflammation. If treatments are available that can reduce the inflammation, the treatments may cause the anemia to improve or go away. For example, taking medicines to treat inflammation in rheumatoid arthritis can improve anemia.
Medicines
A health care professional may prescribe the erythropoiesis-stimulating agents (ESAs) epoetin alpha or darbepoetin alpha to treat anemia related to CKD, chemotherapy treatments for cancer, or certain treatments for HIV. ESAs cause the bone marrow to make more red blood cells. Health care professionals typically give ESAs as shots and may teach you how to give yourself these shots at home. A health care professional may prescribe iron supplements, given as pills or shots, to help ESAs work.
If you’re on hemodialysis, you may be able to receive intravenous (IV) ESAs and iron supplements during hemodialysis. Read more about treatments for anemia in CKD.
Blood transfusions
In some cases, health care professionals may use blood transfusions to treat severe anemia of inflammation. A blood transfusion can quickly increase the amount of hemoglobin in your blood and boost oxygen.
Can I prevent anemia of inflammation?
Experts have not yet found a way to prevent anemia of inflammation. For some chronic conditions that cause inflammation, treatments may be available to reduce or prevent the inflammation that can lead to anemia. Talk with your doctor about treatments and follow the treatment plan your doctor recommends.
How does eating, diet, and nutrition affect anemia of inflammation?
If you have a chronic condition that is causing anemia of inflammation, follow the advice of your doctor or dietitian about healthy eating and nutrition.
Clinical Trials for Anemia of Inflammation
The National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) and other components of the National Institutes of Health (NIH) conduct and support research into many diseases and conditions, including blood diseases.
What are clinical trials for anemia of inflammation?
Clinical trials—and other types of clinical studies—are part of medical research and involve people like you. When you volunteer to take part in a clinical study, you help doctors and researchers learn more about disease and improve health care for people in the future.
Researchers are studying many aspects of anemia of inflammation, including new treatments for this condition.
Find out if clinical studies are right for you.
What clinical studies for anemia of inflammation are looking for participants?
You can find clinical studies on anemia of inflammation at ClinicalTrials.gov. In addition to searching for federally funded studies, you can expand or narrow your search to include clinical studies from industry, universities, and individuals; however, the NIH does not review these studies and cannot ensure they are safe. Always talk with your health care provider before you participate in a clinical study.
References
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
The NIDDK would like to thank:
Robert T. Means, Jr., M.D., East Tennessee State University Quillen College of Medicine
