Prostate Tests
On this page:
- What are prostate tests?
- Why do health care professionals use prostate tests?
- What steps will your health care professional take before ordering prostate tests?
- What prostate tests do health care professionals use?
- What additional tests do health care professionals use?
- How do I prepare for prostate tests?
- What should I expect after prostate tests?
- What are the risks of prostate tests?
What are prostate tests?
Prostate tests are performed to check for problems with your prostate. The tests can show if your prostate is enlarged, if it is causing bladder problems, or if there are signs of cancer.
.jpg) Side view of the male urinary tract. The prostate is below the bladder and surrounds the urethra at the neck of the bladder. Urine flows from the bladder through the prostate and leaves your body from the urethra.
Side view of the male urinary tract. The prostate is below the bladder and surrounds the urethra at the neck of the bladder. Urine flows from the bladder through the prostate and leaves your body from the urethra.
Why do health care professionals use prostate tests?
Different prostate problems can have similar symptoms. A medical exam followed by prostate testing is important for diagnosing your problem.
Health care professionals may recommend prostate tests if you have symptoms such as
- urinary frequency, urinary urgency, or nocturia
- trouble starting a urine stream or a weak or interrupted urine stream
- urine blockage
- urinary retention
- bladder control problems, known as urinary incontinence
- urine with an unusual color or odor
- painful urination or painful ejaculation
What steps will your health care professional take before ordering prostate tests?
Before ordering any prostate tests, your health care professional will review your medical history, including any major illnesses or surgeries, perform a physical exam, and may ask
- if you have a family history of prostate problems
- when your problem or symptoms started and how often they occur
- whether you consume caffeine and alcohol
- how much water or other liquids you typically drink each day
Some prostate problems may require a series of medical exams and tests for diagnosis.
What prostate tests do health care professionals use?
Health care professionals may use the following tests to diagnose prostate problems.
Digital rectal exam
Many health care professionals perform a digital rectal exam (DRE) as part of a routine physical exam for males ages 50 or older. Some males may start receiving a DRE as part of a physical exam earlier, at age 40, whether or not they have any urinary problems.
During a DRE, your health care professional will feel your prostate for any abnormalities that could need more tests. The DRE may be slightly uncomfortable, but it is brief. You will either stand and bend forward or lie on your side on the exam table with your knees bent for the exam.
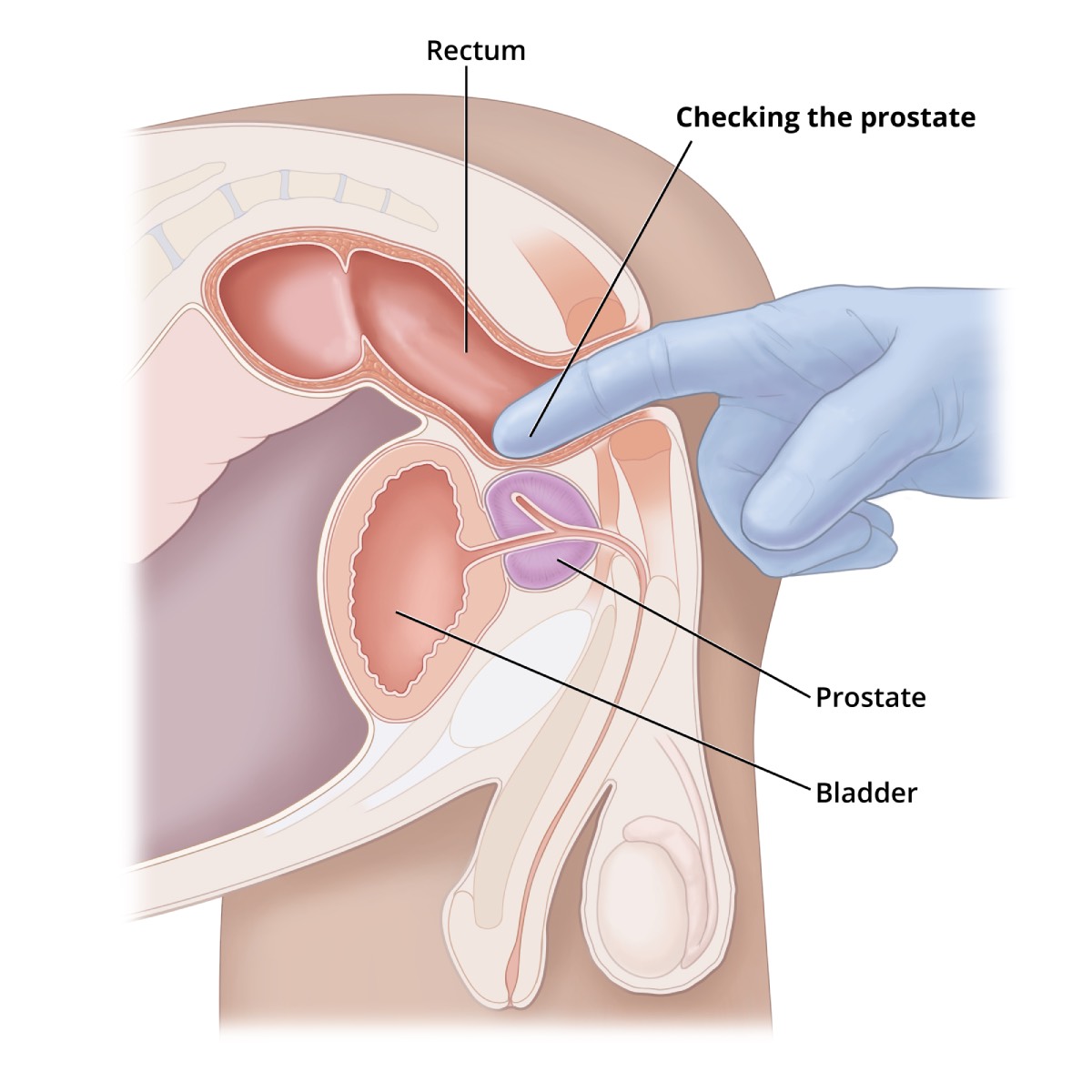 During a digital rectal exam, your health care professional slides a gloved, lubricated finger into your rectum and feels your prostate.
During a digital rectal exam, your health care professional slides a gloved, lubricated finger into your rectum and feels your prostate.
If an infection is suspected, your health care professional might gently massage the prostate to collect a sample of fluid to examine under a microscope. The DRE may also help determine if a prostate biopsy or other tests are needed, especially if your health care professional feels a mass within the prostate.
Prostate-specific antigen test
Prostate-specific antigen (PSA) is a protein made only by the prostate gland. The PSA test is a blood test that measures the amount of PSA protein in your blood.
The PSA test is most often used along with the DRE to rule out prostate cancer. Finding high levels of PSA in your blood could be a sign of prostate cancer or of less serious problems, such as benign prostatic hyperplasia or prostatitis.
The PSA test is a screening test that may be difficult to interpret, particularly if the test has been only done once. The difficulties in interpreting the PSA can lead to potentially unnecessary prostate biopsies and treatment.1 For example,
- the PSA test is known to have false-positive and false-negative results. Repeating the test and establishing a trend for your number is helpful to reduce some of this inaccuracy.
- a high PSA level could be a sign of prostate cancer, but it could also indicate other problems with the prostate.
- follow-up diagnostic tests, such as a prostate biopsy, could cause side effects, including bleeding and infection.
If you are between the ages of 55 and 69, the PSA test may be recommended for you to consider. If you are age 70 or older, the test is not usually recommended. Talk with your health care professional about any concerns and whether the PSA test is right for you.
Prostate health index
The prostate health index (PHI), approved by the U.S. Food and Drug Administration, combines your PSA score in a mathematical formula with results from two additional blood tests. Your health care professional may order those two additional blood tests if your PSA score is between 4 and 10. The PHI measures your risk for prostate cancer more accurately, and it might save you an unnecessary biopsy.2
Biopsy
Most prostate biopsies are guided by transrectal ultrasound (TRUS). However, health care professionals are increasingly using more targeted and accurate imaging techniques with biopsies.
TRUS-guided biopsy
TRUS is most often used to examine the prostate and is usually combined with a biopsy. A health care professional inserts a probe that is slightly larger than a finger into the rectum next to the prostate. The ultrasound image shows the size of the prostate and might identify abnormal-looking areas within the prostate, such as tumors. Your health care professional will perform a biopsy by inserting a needle through the rectum next to the ultrasound probe or through the perineum into several areas of the prostate. Tissue samples are removed and examined by a pathologist to see if any of them are cancerous. This technique has the risk of missing tumors that are outside the sampling areas.
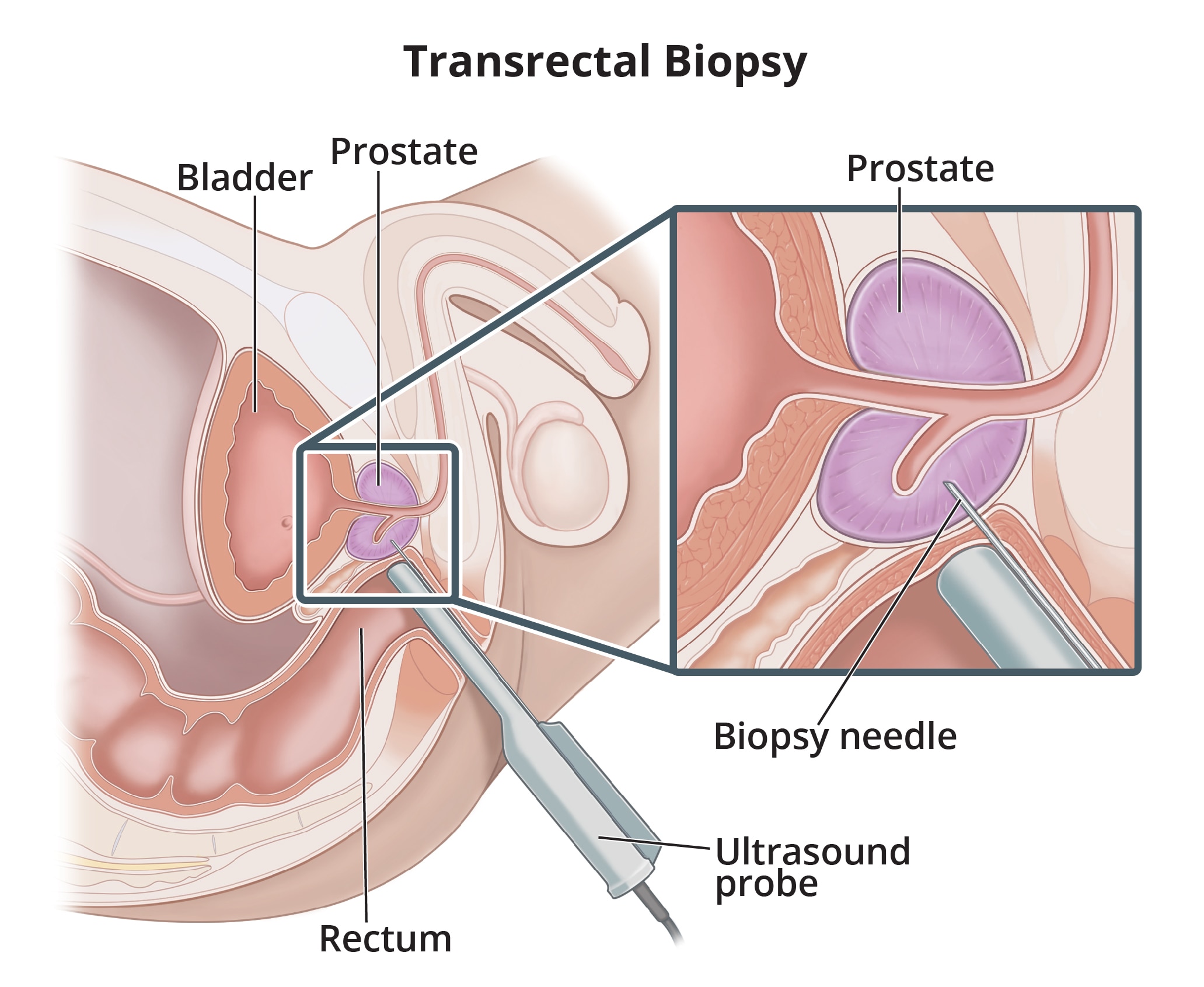 During a transrectal biopsy, a health care professional inserts an ultrasound probe into the rectum to see where the tumor is, then inserts a needle into the prostate to remove a tissue sample.
During a transrectal biopsy, a health care professional inserts an ultrasound probe into the rectum to see where the tumor is, then inserts a needle into the prostate to remove a tissue sample.
Magnetic resonance imaging/TRUS-fusion-guided biopsy
A health care professional will take an image of your prostate during magnetic resonance imaging (MRI). The health care professional will load the MRI image into special software where it is fused with real-time TRUS images. The combined images allow for targeted guidance and precise biopsy of any concerning areas. These targeted biopsies might be combined with a systematic biopsy to sample other parts of the prostate.
MRI-guided biopsy
During an MRI, biopsy needles are inserted through the rectum or perineum into targeted areas seen on the MRI. This technique is not used often because it can be complicated and expensive.
Cognitive fusion
MRI images are taken before and during a TRUS biopsy to provide guidance on biopsy targets. This technique is more accurate at finding prostate cancer than a TRUS biopsy alone. However, health care professionals must have special training in this technique to perform it, and there may not be a professional available in your area.
What additional tests do health care professionals use?
Your health care professional may order additional tests for more information, such as
- urinalysis to see if you have an infection in your bladder
- urodynamic tests to measure the pressure in your bladder while you urinate to see if your bladder is obstructed
- cystoscopy to make sure your urinary symptoms are not due to bladder cancer or a bladder stone and to check your prostate’s shape and size
- ultrasound of the abdomen to see if there are any blockages in your urinary tract, including the kidneys
- MRI or computed tomography (CT) scans to identify abnormalities in the urinary tract
How do I prepare for prostate tests?
Some tests may require preparation, while others may not. You may need to
- drink two to three glasses of water, without going to the bathroom, about an hour before some abdominal ultrasounds or some urodynamic tests
- if prescribed, take antibiotics to prevent infection before tests that involve inserting instruments into the urethra or rectum, or before biopsy
Ask your health care professional if there is anything you need to do before your test.
What should I expect after prostate tests?
You may feel some discomfort shortly after your tests, but you can usually go back to your normal activities. Some people may experience additional symptoms after certain prostate tests.
DRE
You may bleed slightly from the rectum afterward. This is more likely to happen if you have hemorrhoids or anal fissures, which are small tears in your anus that may cause itching, pain, or bleeding.
PSA
You may have slight pain or bruising at the spot where the needle was inserted to draw the blood, but most symptoms go away quickly.
Prostate biopsy
You may see some blood in your urine or ejaculate, or from your rectum for a short while after the procedure. You may be asked to take antibiotics to prevent infection.
It may take several days to weeks to get your test results. Your health care professional will talk with you about the results and ways to treat the problem.
What are the risks of prostate tests?
Risks of side effects or complications from prostate tests vary. Before any test, talk with your health care professional about risks, benefits, and potential complications.
Low-risk prostate tests include the PSA test, DRE, ultrasound, and MRI. Prostate biopsy may have a higher risk for side effects or complications such as
- blood in the urine or ejaculate, or rectal bleeding—these may be temporary
- urinary tract infections
- severe infection of the blood, called sepsis
- urinary retention or erectile dysfunction
- injury to the wall of the rectum
Seek care right away
After a prostate test, call or see a health care professional right away if you
- feel severe discomfort
- feel pain when urinating, have cloudy urine, or cannot urinate
- have blood in your urine or ejaculate, or coming from the rectum or around your anus
- have a fever or chills
References
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
NIDDK would like to thank:
R. Charles Welliver Jr., M.D., Albany Medical College
