Liver Biopsy
On this page:
- What is a liver biopsy?
- Are there different types of liver biopsy?
- Why do doctors use liver biopsy?
- How do I prepare for a liver biopsy?
- How do doctors perform a liver biopsy?
- What should I expect after a liver biopsy?
- What are the risks of liver biopsy?
- Seek care right away
What is a liver biopsy?
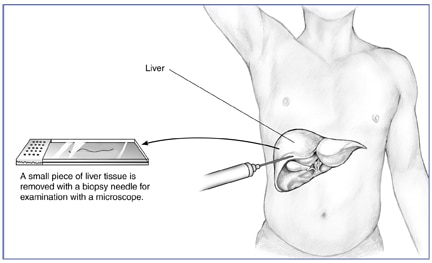
A liver biopsy is a procedure in which a doctor takes a small piece of tissue from your liver. A pathologist will examine the tissue with a microscope to look for signs of damage or disease.
Are there different types of liver biopsy?
Yes. In each type of liver biopsy, doctors take the sample of liver tissue in a different way. Common types of liver biopsy are described below.
Percutaneous liver biopsy
In percutaneous liver biopsy, the doctor inserts a needle through your skin in the upper part of the abdomen to take a small piece of your liver tissue.
Percutaneous liver biopsy is the most common type of liver biopsy and has been performed routinely for many years. Your doctor may perform an ultrasound or computed tomography (CT) scan to be sure that the needle is positioned in the correct place.
Transjugular liver biopsy
In transjugular liver biopsy, a doctor inserts a needle into a vein in your neck called the jugular vein. The doctor passes the needle through your veins to your liver to take a small piece of tissue.
Doctors usually perform transjugular biopsy in people who have a higher risk of problems with percutaneous liver biopsy. For example, bleeding after a percutaneous biopsy is more likely in people who have problems with blood clotting. In people who have ascites—a buildup of fluid in the abdomen that is a complication of cirrhosis—percutaneous biopsy is difficult because the liver is too far away from the skin and hard to target.
Transjugular biopsy also allows doctors to measure pressure in the veins of the liver at the same time that they perform the biopsy.
Surgical liver biopsy
If you need a liver biopsy and you are having surgery for other reasons, a doctor may perform a liver biopsy during the surgery.
Why do doctors use liver biopsy?
Doctors use liver biopsy to
- diagnose liver diseases when doctors can’t confirm a diagnosis with blood or imaging tests
- find out how severe the liver damage or disease is
- help determine the best treatment for liver damage or disease
- find out how a treatment for liver disease is working
How do I prepare for a liver biopsy?
To prepare for a liver biopsy talk with your doctor, have blood and imaging tests if needed, arrange for a ride home after the procedure, and follow your doctor’s instructions about fasting before the procedure.
Talk with your doctor
Talk with your doctor about what you can expect before, during, and after the liver biopsy.
Also talk with your doctor about any allergies and medical conditions you have and all the prescribed and over-the-counter medicines, vitamins, and supplements you take, including
- aspirin or medicines that contain aspirin
- blood thinners
- complementary or alternative medicines
- diabetes medicines
- dietary supplements
- nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen and naproxen, or medicines that contain NSAIDs
Your doctor may ask you to temporarily stop taking medicines that affect blood clotting or interact with sedatives. You may receive sedatives during a liver biopsy to help you relax and stay comfortable.
Have blood and imaging tests
Before you have a liver biopsy, your doctor may order blood tests to find out how well your blood clots. For blood tests, a health care professional will take blood samples and send the samples to a lab.
Severe liver disease, inherited bleeding disorders such as hemophilia, and other health conditions may cause problems with blood clotting. If you have problems with blood clotting, your doctor may give you a transfusion of platelets or clotting factors just before a liver biopsy. Your doctor may also recommend a transjugular liver biopsy instead of a percutaneous liver biopsy.
Your doctor may also order imaging tests to view your liver and surrounding organs and find the best place to insert the biopsy needle. Imaging tests may include
- ultrasound, which uses a device called a transducer that bounces safe, painless sound waves off organs to create images of their structure
- CT scan, which uses a combination of x-rays and computer technology to create images
Arrange for a ride home
For safety reasons, most people cannot drive home after a liver biopsy. You will need to make plans for getting a ride home after a liver biopsy.
Follow your doctor’s instructions about fasting before the procedure
Doctors may ask people to fast—not eat or drink anything—for several hours before a liver biopsy. In some cases, doctors ask patients to eat a small snack a few hours before a liver biopsy. Instructions about fasting vary, and doctors may give different instructions for different types of biopsy. Follow your doctor’s instructions.
How do doctors perform a liver biopsy?
Doctors perform a liver biopsy at a hospital or outpatient center.
Percutaneous liver biopsy
The doctor will find the best place to insert the biopsy needle by tapping on your abdomen or by using ultrasound or a CT scan. Doctors may also use ultrasound or CT scans to guide the biopsy needle during the procedure.
You’ll receive a local anesthetic to numb the area where the doctor will insert the biopsy needle. If needed, you may also receive sedatives and pain medicine.
You will be asked to lie on your back and rest your right hand above your head. The doctor will make a small cut in the right side of your abdomen and insert the biopsy needle. You may be asked to breathe out and hold your breath while the sample of liver tissue is taken.
After the biopsy, the doctor will place a bandage over the cut on your abdomen. You may be asked to lie on your right side after the biopsy, and you will need to remain lying down for a few hours. Health care professionals will typically check your vital signs regularly for 2 to 4 hours after the procedure.1
Transjugular liver biopsy
The doctor will use ultrasound to find the best place on your neck to access your jugular vein. During the procedure, the doctor will use ultrasound to view your jugular vein and will use fluoroscopy, a type of x-ray imaging, to view the veins between your neck and your liver.
You’ll receive a local anesthetic to numb the area on your neck where the doctor will insert the biopsy needle. You may also receive sedatives and pain medicine.
You will be asked to lie on your back and turn your head to the side. The doctor will make a small cut on your neck and use a needle to make a small hole in your jugular vein. The doctor will insert a thin, flexible tube, called a catheter, through your veins to your liver. The doctor will thread a biopsy needle through the catheter and into your liver to take a tissue sample.
After the biopsy, the doctor will place a bandage over the cut on your neck. You will need to remain lying down and have your vital signs regularly checked for at least 4 hours after the procedure.2
Surgical liver biopsy
You will receive anesthesia for surgery. Doctors can perform a liver biopsy during open surgery or laparoscopic surgery. In open surgery, doctors make a large cut to open the abdomen. In laparoscopic surgery, doctors make small cuts in the abdomen and insert special tools to view or repair organs and tissues.
What should I expect after a liver biopsy?
Following a liver biopsy, you—or a friend or family member who is with you if you’re still groggy—will receive instructions on how to care for yourself after the procedure. You should follow all instructions. Instructions may vary, depending on the type of liver biopsy you had.
Talk with your doctor about when you can resume your usual activities. After a liver biopsy, doctors often recommend avoiding intense activity and heavy lifting for up to 1 week.
After a liver biopsy, a pathologist will examine the biopsy tissue with a microscope to look for signs of damage or disease. Biopsy results typically take a few days or longer to come back.

What are the risks of liver biopsy?
The risks of liver biopsy include complications such as the following.
Bleeding
Internal bleeding is a serious complication of liver biopsy. Bleeding may cause signs and symptoms such as pain that is severe or that lasts more than a few hours after the biopsy, low blood pressure, and a fast heartbeat. You may need treatment at a hospital, blood transfusions, and sometimes surgery or another procedure to stop the bleeding.
Bleeding occurs in about 1 out of every 500 liver biopsies. Severe bleeding occurs in 1 out of every 2,500 to 10,000 liver biopsies.1
Pain
Pain is the most common complication after a liver biopsy. Pain often occurs in the upper right abdomen or right shoulder. In most cases, the pain is mild and goes away within a few hours after the biopsy. If pain is severe or lasts longer, it could be a sign of internal bleeding.
Talk with your doctor if you have any pain after a liver biopsy. Your doctor may recommend or prescribe medicines for pain. If the pain is not mild or does not go away within several hours after the biopsy, your doctor may order tests to find the cause of the pain.
Other complications
Uncommon complications that may occur after a liver biopsy include
- infection, which may lead to sepsis
- a collapsed lung, called a pneumothorax
- a buildup of blood in the space between the lung and the chest wall, called hemothorax
- injury to other organs
Seek care right away
If you have any of the following symptoms after a liver biopsy, seek medical help right away
- bleeding, pain, redness, or swelling at the biopsy site or where the doctor made a cut to insert the biopsy needle
- dizziness, fainting, or weakness
- fever
- nausea or vomiting
- pain in your abdomen, shoulder, or chest
- problems breathing or shortness of breath
- racing or pounding of your heart
- stool that contains blood or is black and tarry
- swelling or bloating of your abdomen
References
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
The NIDDK would like to thank:
Don C. Rockey, M.D., Medical University of South Carolina
