How Can You Help Patients Use New Diabetes Technologies?
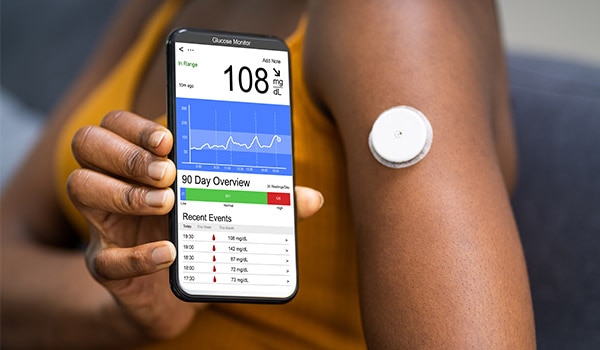
New technologies can improve diabetes outcomes. Learn how health care professionals can help patients access and use these tools.
Diabetes technologies aren’t reaching everyone who could potentially benefit. Dr. Tamara K. Oser, a primary care doctor and diabetes researcher, discusses how health care professionals can put diabetes technologies into practice.
Q: What technology tools are available for people with diabetes?
A: We’ve seen an expansion in the world of diabetes technologies that, if used the right way, can improve diabetes care. We now have continuous glucose monitors (CGMs), insulin pumps that are increasingly automated, connected insulin pens, and apps. Health care professionals and people with diabetes can use technology in many ways to foster diabetes self-management education and support.
Q: How can new technologies benefit people who have diabetes?
A: More evidence is emerging about the benefits of diabetes technologies. For instance, continuous glucose monitoring is associated with improved clinical, psychosocial, and behavioral outcomes, especially for people who have type 1 diabetes or type 2 diabetes that requires intensive insulin therapy. Evidence is also emerging about the benefits of continuous glucose monitoring for people with type 2 diabetes on basal insulin, and even for people with type 2 diabetes who are not on insulin.
However, just having a technology tool doesn’t necessarily improve outcomes. Health care professionals and patients with diabetes also need education about how to use the device, how to engage with the data, and how to communicate with each other about the data. For example, when patients start to use CGMs, health care professionals should ask them how often they want to receive CGM alarms. If you don’t have this conversation, patients may get too many alarms and develop alarm fatigue—meaning they no longer respond appropriately to alarms—and stop using the device.
There are also exciting advances in insulin pump therapy, including automated insulin delivery systems and work being done to expand access to these technologies as well.
Q: Are diabetes technologies made available to everyone who could benefit from them?
A: No. One study found that continuous glucose monitoring reached about 30% of people with type 1 diabetes in the T1D Exchange Registry, who mostly received care from endocrinologists at academic medical centers. However, we can assume that continuous glucose monitoring is less common among people who receive care from community medical practices, which is where most Americans receive care. We know that about 50% of adults with type 1 diabetes and 90% of adults with type 2 diabetes receive diabetes care from primary care providers, but most of the studies on diabetes technologies are conducted through endocrinology practices at academic medical centers.
So, there may be a geographic disparity in access to diabetes technologies. Our research team is working on many projects to address that geographic disparity and help implement diabetes technologies in primary care.
Q: Are there other disparities in the use of diabetes technologies? How do social determinants of health affect how people with diabetes access and use technology tools?
A: There are also socioeconomic, racial, and ethnic disparities in the use of diabetes technologies. Compared with the white population, racial and ethnic minority groups have higher rates of diabetes and often have worse diabetes outcomes. Patients from racial and ethnic minority groups and patients of lower socioeconomic status are less likely to be offered diabetes technologies.
However, studies have shown that when these patients are given access to diabetes technologies, they have outcomes that are similar to those of white patients or patients with higher socioeconomic status. At the Federally Qualified Health Center where I care for a large immigrant and refugee population, I’ve used CGMs with my patients, and they’ve done brilliantly.
One reason for disparities in access to diabetes technologies may be implicit bias that affects which patients are offered diabetes technologies. As health care professionals, we need to address our unconscious biases about which patients may or may not benefit from technologies. Other reasons for disparities include physician shortages and restrictive insurance eligibility criteria.
We have a lot of work to do to address disparities. This is a topic I’m very passionate about—making sure certain populations aren’t left behind as diabetes technologies advance.
Q: What are the barriers to using diabetes technologies—both for health care professionals and for people with diabetes?
A: Compared with endocrinology practices in academic medical centers, primary care practices and community endocrinology practices have different resources and workflows, and how we implement diabetes technology in each setting will be different.
One way that primary care practices can address limitations, in terms of time and workflow, is to engage the entire health care team—including diabetes care and education specialists, clinical pharmacists, health coaches, and patient navigators—in implementing diabetes technologies. A recent Association of Diabetes Care and Education Specialists technology summit brought together a multidisciplinary group of health care professionals to discuss broadening access to diabetes technologies. I also worked with the American Academy of Family Physicians on a Transformation in Practice Series course that provides a comprehensive approach to implementing continuous glucose monitoring in primary care.
For patients with diabetes, one barrier is lack of access, either because they aren’t offered diabetes technologies or because they lack insurance coverage for technologies. However, even if patients have access, lack of education and support can be a barrier to using diabetes technologies effectively.
Q: What role can a diabetes care and education specialist (DCES) play in helping people with diabetes overcome barriers to using new technologies?
A: A DCES can serve as a technology champion. Any practice that has a DCES is set up for a much greater likelihood of success. The DCES can partner with the patient and the rest of the health care team to address issues related to diabetes technologies, including
- engaging in shared decision making with patients about the type of diabetes technology they’re interested in using
- handling insurance issues
- educating patients about how to use technology tools and data
- collaborating with the rest of the primary care or endocrinology team
However, our team, in partnership with the American Academy of Family Physicians National Research Network and other practice-based research networks, conducted a national survey of 656 primary care providers, and only 36% had a DCES in their practice, even part time. Because the majority of primary care practices don’t have access to that valuable resource, we need to consider how a DCES may be able to support multiple practices through telehealth or other novel ways of providing care.
Q: How can other health care professionals integrate technology into diabetes care?
A: Practices that don’t have a DCES might have a pharmacist, a health coach, or a case manager who can serve as a technology champion or work as part of a multidisciplinary team to help integrate technology into diabetes care.
Health care professionals can also tailor their approach. If your primary care practice isn’t currently using diabetes technology, you might start by choosing a technology that will be most relevant to your patient population. You can then identify members of your health care team who can help implement diabetes technology with patients.
Also, patients may benefit from a diabetes technology even if they aren’t able or don’t want to use every aspect of the technology. I have patients who don't have a smartphone or don’t want to use an app, and they just use a reader for continuous glucose monitoring. The reader captures important metrics that we go over together, and I’ve seen huge improvements in diabetes management.
Q: What research is being conducted on the use of diabetes technologies?
A: This is an exciting field, and lots of research is going on right now. My research group is studying ways to implement CGM and automated insulin delivery systems in primary care. Other research groups are conducting a study to compare fingerstick blood glucose monitoring to CGMs in primary care practices. Other studies are looking at insulin dosing algorithms in patients using CGMs or fingerstick blood glucose monitoring in a wide range of practice settings.
Many studies are looking at how to use diabetes technology to help patients with self-management and education. The COVID-19 pandemic has demonstrated the benefits of remote monitoring and alternative care models outside the clinic walls.
How do you help patients with diabetes learn about and use diabetes technologies? Tell us below in the comments.
