How Can You Use Teleophthalmology to Prevent Vision Loss in Patients with Diabetes?
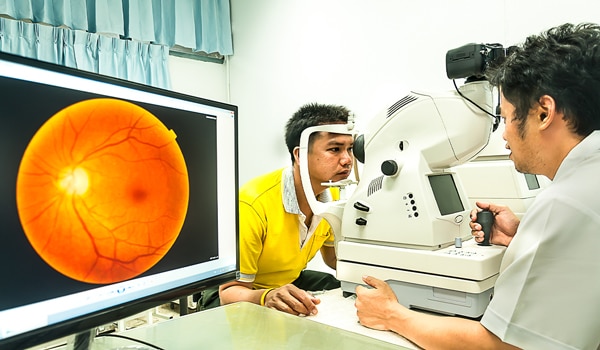
Are you ready to use teleophthalmology to prevent vision loss in patients with diabetes?
According to the Centers for Disease Control and Prevention, more than 37 million people have diabetes in the United States. People with diabetes can develop advanced eye disease, leaving them at high risk of going blind. But because they have no vision loss or other symptoms, many people with diabetic eye disease do not seek medical help. Teleophthalmology, which uses remote ophthalmic imaging via telecommunication technologies, can be a good tool to prevent this serious diabetes complication.
Rajeev Ramchandran, MD, is a retina specialist working on multiple research projects using teleophthalmology. Below, he shares his insights about this tool.
Q: What eye diseases are most common for patients with diabetes? What is the risk of vision loss?
A: Diabetic retinopathy is the leading cause of blindness in the population from ages 20 to 74 in the United States. About 30 to 40% of patients with diabetes have diabetic retinopathy, which is when the layer of the eye called the retina is damaged by diseased and leaking blood vessels. Many patients with diabetes have high blood pressure, which is also a risk factor for developing retinopathy. For patients that have had diabetes for 15 years or more, about 80 to 90% have some form of retinopathy. Cataracts and glaucoma can also affect the eyes of people who have diabetes.
Q: What are the recommendations for eye disease screening in patients with diabetes?
A: The American Diabetes Association and the American Academy of Ophthalmology agree that we should check the eyes of patients with type 1 diabetes within five years after the diagnosis. Patients with type 2 diabetes often don’t get diagnosed until they’ve had the disease a few years, so they should get an eye exam at the time of their diagnosis. The patient should have a follow-up exam every year.
Patients who have diabetes and are planning to get pregnant should get an eye exam before pregnancy to know their baseline retinopathy status. They should get subsequent eye exams as soon as they’re pregnant and in each trimester, because diabetic retinopathy can rapidly get worse if it’s present during pregnancy.
Q: Why is it important for health care professionals to improve screening for diabetic eye diseases and the referral of patients to specialized care?
A: Diabetes affects all the blood vessels in the body, but the eye is the only place where you can directly examine them. The blood vessels in the eye are the same caliber and size as the blood vessels found in the kidneys, the heart, the brain, and around the nerves in the legs and arms.
Retinopathy often is silent. There are no changes in vision, or any pain or discomfort in the eye, until the disease is very advanced. The diagnosis should be done at the right time to avoid vision loss. Ophthalmologists, specifically retinal specialists, can treat vision-threatening retinopathy with eye injections of anti-vascular endothelial growth factor (anti-VEGF) antibodies to help decrease the edema, the leaking of blood vessels, and the production of new abnormal blood vessels. The retinopathy may regress and sometimes even reverse itself.
Q: How do the social determinants of health affect outcomes for patients at risk of diabetic eye disease?
A: Many patients with diabetes do not know about the risk of vision loss, do not have insurance, and do not have transportation to even see a primary care doctor. Many also have trouble keeping up with managing their diabetes and high blood pressure. To be screened for eye disease with an eye doctor, the patient needs to take time from work, have a dilated eye exam, and have someone to go with them to the exam. There are a lot of priorities in life before getting an eye exam, especially if the patient feels that their vision is fine.
Q: What is teleophthalmology, and how can it help prevent blindness in patients with diabetes?
A: Teleophthalmology relies on digital photography of the retina, in many cases taken through undilated pupils. About 90 to 95% of the time you can get a good picture, but some cameras can have a better image of the peripheral retina than others. The exam is done at the primary care office, or in another non-eye-care setting. Some primary care offices may use artificial intelligence (AI) to evaluate the photos and get an immediate diagnosis, but in others the eye doctor reads the images in a remote location and sends the report and management plan back to the primary care clinic.
Teleophthalmology allows health care professionals to triage patients and know who needs urgent care. Around 30 to 40% of the patients may have retinopathy—and as much as 60 to 70% in underserved populations—but only 10 to 15% will need urgent care to prevent vision loss.
Teleophthalmology also increases access to care for underserved populations by removing limits such as waiting time to see the eye doctor, time away from work, and the need for a companion to travel to see an eye doctor.
Even with the use of teleophthalmology, a person still needs to see the eye doctor for a full eye exam, but maybe every 3 years or longer if their diabetes is well controlled and they do not have retinopathy or other eye diseases such as cataracts or glaucoma on a teleophthalmology exam. Some places, like Veterans Affairs clinics, have been doing remote eye exams for a few decades. They now also check for glaucoma, cataracts, and other eye diseases using multiple diagnostic tools.
Q: How can you implement teleophthalmology in primary care, and what are the main resources that you need?
A: Some of the factors to consider are workflows, awareness of the need for the eye exams, technology, and training.
- Workflows in a primary care office will need to incorporate eye testing as part of the routine exam for patients with diabetes, including vision testing and reading of the images by AI or the eye doctor.
- Staff need to be aware of how teleophthalmology fits into their own workflow and what the value is for patients.
- Cameras and other technology are getting more affordable, and they are user-friendly. Some even have automated systems such as auto-focusing and auto-positioning.
- Anybody in the clinic can be trained to take the photos; it doesn’t have to be a medical professional. The photos can then be read by an eye doctor or an AI program.
Q: Can a health care professional bill for this service? Do all health insurers cover this service?
A: To be able to bill insurance, a physician’s order is needed.
Insurance reimbursement for teleophthalmology services is not consistent yet, but it became more flexible because of the restrictions during the pandemic. In order for insurance to cover the exam, the office where the services take place and the eye doctor reading the images must be licensed in the same state as the patient undergoing the teleophthalmology exam.
Medicare, which is the most common insurance for people over age 65, does not cover teleophthalmology on a nationwide basis. In some cases, only a full eye exam is covered. The codes used to bill for teleophthalmology service may vary depending on who owns the equipment and if the service is provided by the eye doctor, a primary care doctor, or a technician.
Q: What research is being conducted on teleophthalmology?
A: Researchers are studying many aspects of teleophthalmology programs, including
- outcomes of having cameras in clinics, such as how many people are screened, how many diseases are found, and how many people return to get eye care if they have a disease
- the quality of the photos and the role of AI
- how to make cameras smaller, more affordable, and provide better pictures
- how to improve workflows and processes to serve more patients and provide eye care in a non-eye-care location
- how these programs can increase patient education and awareness about eye exams, including teaching health care professionals how to approach patients with low health literacy and other social determinants of health that become stressors and make eye care less of a priority
I am working on a research project including eight safety net clinics where we are targeting underserved populations to evaluate the use of teleophthalmology. We are also part of a National Institutes of Health grant evaluating teleophthalmology in rural areas. So far, we’ve doubled the rates of eye exams in the first year and have sustained this increase over the last four years. We have also connected a lot of patients back to eye care. Now that we’ve worked on the process of getting people back into eye care, we’re trying to learn to what extent their vision was saved or improved.
We are also trying to see if we can bring the eye doctor to the patients. We have a mobile van that goes to areas with high numbers of patients to do general eye exams. We are not treating patients with retinopathy yet in these cases, but we could do that in the future.
Do you have experience using teleophthalmology? Tell us about it in the comments below.
