Diagnosis of GER & GERD
How do doctors diagnose GER & GERD?
In most cases, doctors diagnose gastroesophageal reflux (GER) and gastroesophageal reflux disease (GERD) by reviewing your symptoms and medical history. If your symptoms suggest you have GERD, your doctor may recommend treatment with medicines and lifestyle changes, instead of doing tests.
Your doctor may recommend medical tests if
- your symptoms suggest you might have a complication of GERD
- your symptoms suggest that you might have another health problem that causes symptoms similar to those of GERD
- your symptoms don’t improve after treatment with medicines and lifestyle changes
Your doctor may refer you to a gastroenterologist to diagnose and treat GERD.
What tests do doctors use to diagnose GERD?
Your doctor may order one or more of the following tests to help diagnose GERD and check for GERD complications or other health problems.
Upper gastrointestinal (GI) endoscopy
Upper GI endoscopy is a procedure in which a doctor uses an endoscope—a flexible tube with a camera—to see the lining of your upper GI tract, including your esophagus, stomach, and duodenum. During upper GI endoscopy, a doctor may obtain biopsies by passing an instrument through the endoscope to take small pieces of tissue from the lining of your esophagus. A pathologist will examine the tissue under a microscope. Doctors may order an upper GI endoscopy to check for complications of GERD or problems other than GERD that may be causing your symptoms.
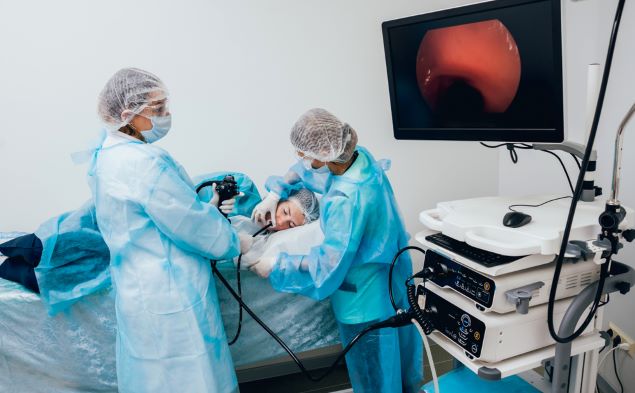 Your doctor may order an upper GI endoscopy to help diagnose GERD.
Your doctor may order an upper GI endoscopy to help diagnose GERD.
Esophageal pH monitoring
Esophageal pH monitoring is the most accurate way to detect stomach acid in the esophagus. Two types of esophageal pH monitoring are
- catheter monitoring, in which a health care professional passes one end of a catheter—a thin, flexible tube—through your nose and into your esophagus to measure acid and nonacid reflux
- capsule monitoring, in which a health care professional uses an endoscope to place a small, wireless capsule on the lining of your esophagus to measure acid reflux
During esophageal pH monitoring, you’ll wear a monitor that receives information from the catheter or capsule and tracks information about your diet, sleep, and symptoms. Your doctor will use this information to see how your diet, sleep, and symptoms relate to acid reflux in your esophagus. Doctors may order this test to confirm the diagnosis of GERD or to find out if GERD treatments are working.
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.

