Appendicitis
Return to Overview PageDefinition & Facts
In this section:
- What is appendicitis?
- How common is appendicitis?
- Who is more likely to develop appendicitis?
- What are the complications of appendicitis?
What is appendicitis?
Appendicitis is inflammation of your appendix, a finger-like pouch attached to your large intestine. The appendix is in the lower-right area of your abdomen, or belly.
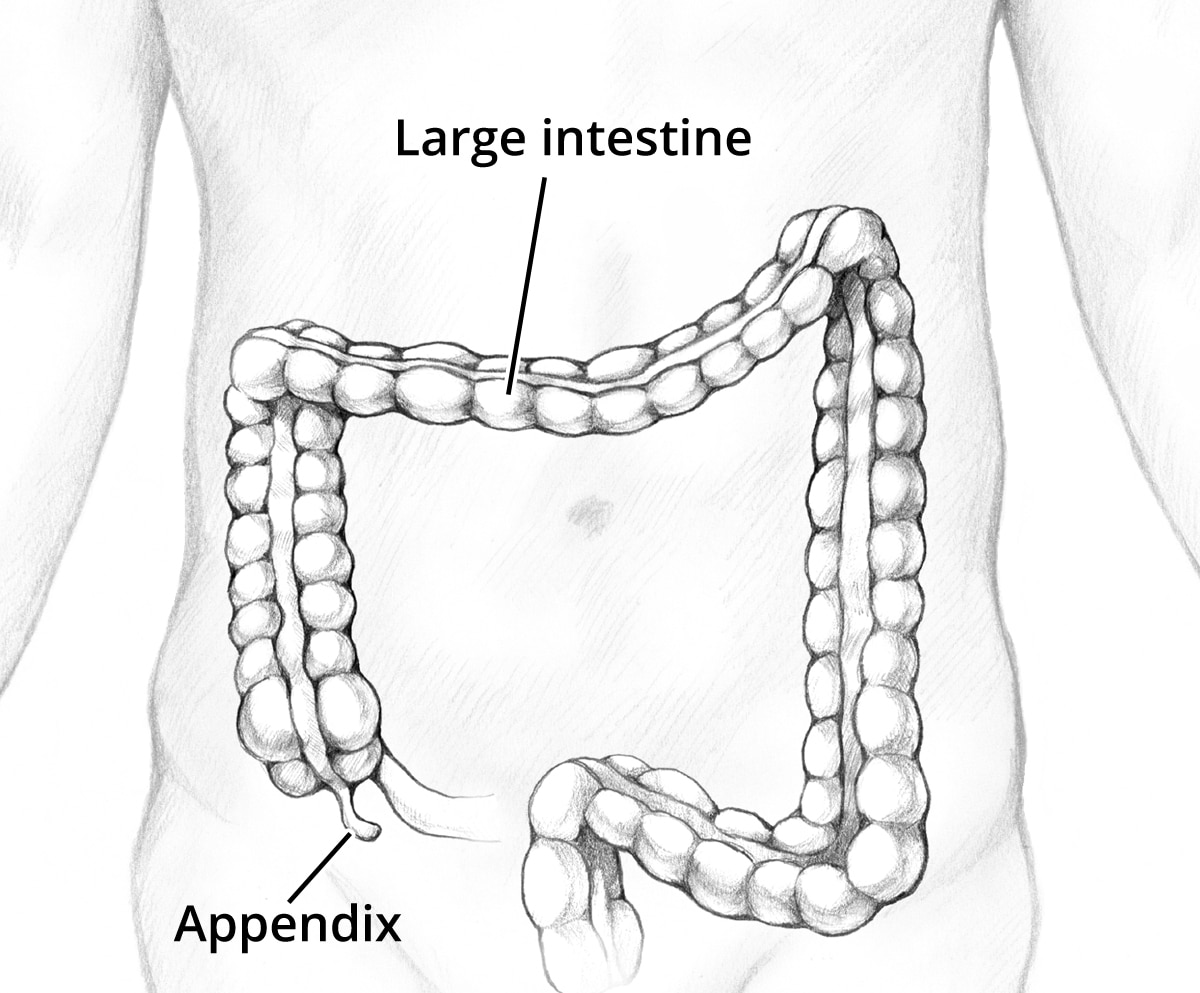 Your appendix is in the lower-right area of your abdomen, near where the small intestine attaches to the large intestine.
Your appendix is in the lower-right area of your abdomen, near where the small intestine attaches to the large intestine.How common is appendicitis?
In the United States, appendicitis is the most common cause of acute abdominal pain for which you need surgery. About 5 to 9 of every 100 people develop appendicitis at some point.1
Who is more likely to develop appendicitis?
Appendicitis is slightly more common among males than females. It happens more often in people in their teens and 20s, but it may happen in people of any age, including older adults.1
What are the complications of appendicitis?
Untreated appendicitis can cause your appendix to burst. A burst appendix could lead to complications. One such complication, peritonitis, is a serious infection that can spread in your abdomen. Another possible complication is an abscess of the appendix called an appendiceal abscess.
References
Symptoms & Causes
What are the symptoms of appendicitis?
The most common symptom of appendicitis is pain in your abdomen, or belly. If you have appendicitis, the pain in your abdomen may
- begin near your belly button and move lower and to your right
- start suddenly and may even wake you if you’re sleeping
- get worse when you move around, take deep breaths, cough, or sneeze
- be severe and may feel different than any pain you’ve ever felt
- happen before other symptoms, and worsen in a matter of hours
 The most common symptom of appendicitis is abdominal pain that may feel different than any pain you’ve ever felt.
The most common symptom of appendicitis is abdominal pain that may feel different than any pain you’ve ever felt.Other symptoms of appendicitis may include
However, some people who are found to have appendicitis, especially children, may not have any of these typical symptoms.2 Talk with your doctor right away if you or your child are experiencing pain or discomfort. A doctor can evaluate the symptoms you or your child are experiencing and provide a diagnosis or determine other possible reasons for complications.
Some people with appendicitis may also have bowel problems, such as
- an inability to pass gas
- constipation or diarrhea
- the feeling that having a bowel movement will relieve discomfort
What causes appendicitis?
Appendicitis can have more than one cause. In many cases, the cause is not clear. Possible causes include
- hardened stool or growths that can block the opening inside the appendix
- enlarged tissue in the wall of your appendix, caused by infection in the digestive tract or somewhere else in your body
- inflammatory bowel disease
When should I seek a doctor's help?
Appendicitis is a medical emergency that requires immediate care. See a doctor or go to the emergency room right away if you think you or your child has appendicitis. A doctor can help treat appendicitis, reduce symptoms, and lower the chance of complications.
References
Diagnosis
How do doctors diagnose appendicitis?
To diagnose appendicitis, your doctor will review your symptoms and medical history, perform a physical exam, and order lab tests and imaging tests.
Medical history
Your doctor will ask questions to help rule out other health problems. Your doctor will want to know
- when your abdominal pain began, how bad it feels, and where exactly you feel it
- when your other symptoms started
- what other medical conditions, illnesses, and operations you’ve had
- whether you use medicines or alcohol
Physical exam
During the physical exam, your doctor will check for pain in your lower-right abdomen. Your doctor may
- gently press or jiggle all areas of your abdomen
- press your right knee as you lift your leg
- flex and rotate your leg while you lie on your left side
Your doctor may also
- listen to your abdomen using a stethoscope
- do a digital rectal exam
- do a pelvic exam
Lab tests
To find out whether your abdominal pain is appendicitis or not, your doctor may order a
- blood test, which may show if you have a high white blood cell count—a sign of infection. Your blood test also may show if you have dehydration or if any fluids or electrolytes are out of balance.
- c-reactive protein (CRP) blood test to find other causes of inflammation.
- urinalysis to rule out other conditions, such as a bladder infection or a kidney stone.
- pregnancy test, if you’re a woman.
Imaging tests
Your doctor may use imaging tests to find out if your pain is caused by appendicitis.
- Abdominal ultrasound uses sound waves to create an image of your internal organs. An ultrasound doesn’t use x-rays and doesn’t expose you to radiation. Doctors use an ultrasound as the first imaging test when checking for possible appendicitis in infants, children, young adults, and pregnant women.
- Magnetic resonance imaging (MRI) scan takes pictures of your body’s internal organs and soft tissues without using x-rays. Doctors can use an MRI scan as a safe, reliable alternative to a computed tomography (CT) scan.3
- Computed tomography (CT) scan combines x-rays and computer technology to create images. If you’re a woman of childbearing age, you should have a pregnancy test before having a CT scan. The radiation from CT scans can be harmful to a developing fetus. In children, to decrease radiation exposure, a CT scan is recommended only after ultrasound and MRI.
Imaging tests can show whether your abdominal pain is caused by a blockage inside the appendix, an enlarged or burst appendix, inflammation, an abscess, or something else.
Imaging tests can also show if your abdominal pain and other symptoms are not caused by appendicitis, but rather by other conditions such as
- abdominal adhesions
- inflammatory bowel disease, including long-lasting disorders such as Crohn’s disease and ulcerative colitis
- intestinal obstruction
- pelvic inflammatory disease
- kidney stones
- problems with the reproductive system in women
References
Treatment
In this section:
- How do doctors treat appendicitis?
- What if the surgeon finds a normal appendix?
- Can doctors treat appendicitis without surgery?
- How do doctors treat complications of a burst appendix?
- What complications may occur after an appendectomy?
- What should I expect after surgery to treat appendicitis?
How do doctors treat appendicitis?
Doctors typically treat appendicitis by removing the appendix. This surgery is called an appendectomy. Surgeons perform the operation with general anesthesia in a hospital. Your doctor will recommend surgery if you have ongoing or long-lasting abdominal pain and fever, or if you show signs of a burst appendix and infection. Prompt surgery decreases the chances that your appendix will burst and cause additional health complications.
A surgeon removes your appendix either by
- laparoscopic surgery, in which the surgeon makes a small incision, or cut, in the abdomen and inserts a laparoscope—a thin tube with a tiny video camera and light attached—to view the inside of your abdomen. Surgeons may make one or more additional small incisions and insert tools to remove or repair organs and tissues.
- open laparotomy, in which the surgeon uses a single, larger incision in the lower-right area of your abdomen.
Laparoscopic surgery is becoming increasingly common. It generally leads to fewer complications, such as hospital-related infections, and it has a shorter recovery time. After examining your condition and past medical history, your surgeon will recommend the best method for you.
What if the surgeon finds a normal appendix?
In some cases, a surgeon may find a normal appendix during surgery. If this happens, some surgeons usually remove the appendix so you don’t develop appendicitis in the future. Sometimes surgeons find a different problem, and they may correct it during surgery.
Can doctors treat appendicitis without surgery?
Anyone who might have appendicitis is treated with antibiotics before surgery. Some people may improve with the antibiotics and not need surgery.
Some mild cases of appendicitis may be treated with antibiotics alone. Researchers are studying who might safely avoid surgery based on their symptoms, test results, health, and age, but surgery remains the standard of care.
How do doctors treat complications of a burst appendix?
Treating the complications of a burst appendix will depend on which complication develops: peritonitis or an abscess.
Peritonitis
If you don’t get treated quickly, peritonitis can threaten your life. In most cases, a surgeon will immediately perform a laparotomy: first, to clean the inside of your abdomen to prevent infection, and then to remove your appendix.
Abscess
Doctors typically drain the pus from an abscess to allow it to heal.
What complications may occur after an appendectomy?
Surgery to remove your appendix is generally safe. However, complications are possible. Complications after laparoscopic surgery or open laparotomy may include
- infection of the surgical site
- an abscess that forms inside your abdomen
- a fistula, or abnormal passage, that forms between your intestine or stomach and your skin
- a small bowel obstruction
- ileus, a condition in which your bowel does not work correctly
- abdominal adhesions, or bands of scar-like tissue that form inside your abdomen
What should I expect after surgery to treat appendicitis?
After surgery, you will likely recover completely from appendicitis and won’t need to make changes to your diet, exercise, or lifestyle. Surgeons generally recommend you limit physical activity for the first 3 to 5 days after laparoscopic surgery and for the first 10 to 14 days after a laparotomy. Talk with your surgeon about your recovery plan.
Clinical Trials
The NIDDK conducts and supports clinical trials in many diseases and conditions, including digestive diseases. The trials look to find new ways to prevent, detect, or treat disease and improve quality of life.
What are clinical trials for appendicitis?
Clinical trials—and other types of clinical studies—are part of medical research and involve people like you. When you volunteer to take part in a clinical study, you help health care professionals and researchers learn more about disease and improve health care for people in the future.
Researchers are studying many aspects of appendicitis, such as improved diagnosis and treatment.
Find out if clinical trials are right for you.
Watch a video of NIDDK Director Dr. Griffin P. Rodgers explaining the importance of participating in clinical trials.
What clinical trials for appendicitis are looking for participants?
You can find clinical studies on appendicitis disease at ClinicalTrials.gov. In addition to searching for federally funded studies, you can expand or narrow your search to include clinical studies from industry, universities, and individuals; however, the National Institutes of Health does not review these studies and cannot ensure they are safe. Always talk with your health care professional before you participate in a clinical study.
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
The NIDDK would like to thank:
Thomas H. Chun, M.D., M.P.H., Hasbro Children’s Hospital
