Diagnosis of Crohn’s Disease
How do doctors diagnose Crohn’s disease?
To diagnose Crohn’s disease, doctors review your medical and family history, perform a physical exam, and order medical tests. Doctors order tests to
- confirm the diagnosis of Crohn’s disease
- find out how severe the inflammation is and where in the gastrointestinal (GI) tract the inflammation is located
- rule out other health problems—such as infections, irritable bowel syndrome, or ulcerative colitis—that may cause symptoms similar to those of Crohn’s disease
Medical and family history
To help diagnose Crohn’s disease, your doctor will ask about your symptoms, your medical history, and any medicines you take. Your doctor will also ask about lifestyle factors, such as smoking, and about your family history.
Physical exam
During a physical exam, a doctor most often
- checks for bloating in your abdomen, or belly
- listens to sounds within your abdomen using a stethoscope
- presses on your abdomen to feel for tenderness or masses
- performs a full-body exam to check for weight loss and inflammation in other parts of the body and to rule out other causes of your symptoms
What tests do doctors use to diagnose Crohn’s disease?
Your doctor may perform blood tests, stool tests, endoscopy, and imaging tests to help diagnose Crohn’s disease.
Lab tests
Blood tests
A health care professional may take a blood sample from you and send the sample to a lab to test for changes in
- red blood cells. If you have fewer than normal red blood cells, you may have anemia.
- white blood cells. When your white blood cell count is higher than normal, you may have inflammation or infection somewhere in your body.
- c-reactive protein. When your c-reactive protein level is high, you may have inflammation in your body.
Stool tests
A health care professional may give you a container for catching and storing the stool. You will receive instructions on where to send or take the container to be studied. Doctors use stool tests to look for inflammation and rule out certain infections.
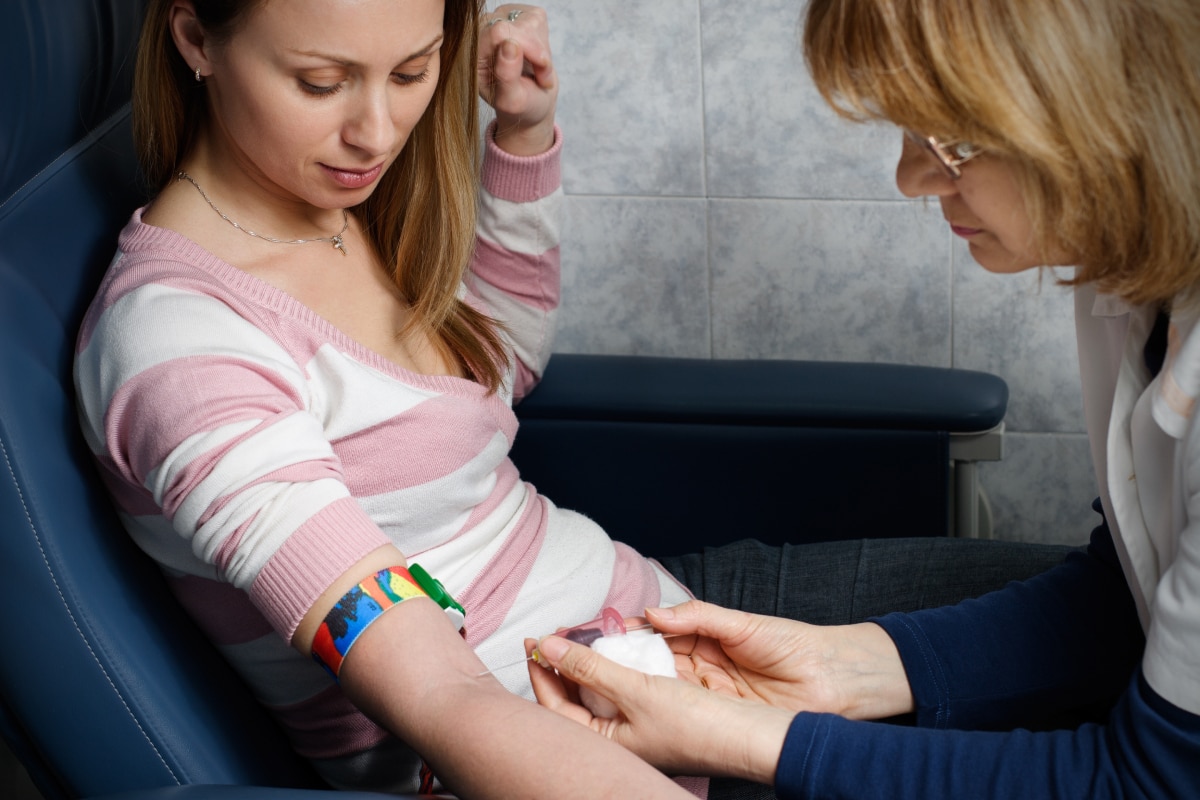 Doctors use blood tests to check for signs of anemia or inflammation in your body.
Doctors use blood tests to check for signs of anemia or inflammation in your body.
Endoscopy
Endoscopy tests are the most accurate way to diagnose Crohn’s disease and rule out other health problems.
During an endoscopy, doctors use an endoscope—a long, flexible, narrow tube with a light and tiny camera on one end—to view inside the GI tract. Doctors may take biopsies during endoscopy tests to help diagnose Crohn’s disease.
Endoscopy tests include
- colonoscopy, which doctors use to see inside your rectum, colon, and ileum
- enteroscopy, which doctors use to see inside your small intestine
- upper GI endoscopy, which doctors use to see inside your esophagus, stomach, and duodenum
Capsule endoscopy
Capsule endoscopy tests check for signs of Crohn’s disease in the small intestine.
For a capsule endoscopy test, you swallow a capsule that contains a tiny camera. You also wear a device, called a recorder. As the capsule passes through your GI tract, the camera records and sends images to the recorder. You will return the recorder to your doctor, who will download and review the images. The capsule will leave your body during a bowel movement. You can safely flush the capsule down the toilet.
Imaging tests
Doctors may order imaging tests, including
- computed tomography (CT) scans, which use a combination of x-rays and computer technology to create images
- magnetic resonance imaging (MRI), which takes pictures of the body’s internal organs and soft tissues without using x-rays
- upper GI series, which uses x-rays and a chalky liquid called barium to view the upper GI tract, including the small intestine
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
