Food Poisoning
Return to Overview PageDefinition & Facts
On this page:
- What is food poisoning?
- How common is food poisoning?
- Who is more likely to get food poisoning?
- What are the complications of food poisoning?
What is food poisoning?
Food poisoning, also called foodborne illness, is an infection or irritation of your digestive tract that spreads through food or drinks. Viruses, bacteria, and parasites cause most food poisoning. Harmful chemicals may also cause food poisoning.
Food poisoning is most often acute, meaning it happens suddenly and lasts a short time. Most cases of food poisoning last less than a week, and most people get better on their own without treatment. In some cases, food poisoning can last longer or lead to serious complications.1
How common is food poisoning?
Each year, about 48 million people in the United States have food poisoning. Food poisoning causes about 3,000 deaths in the United States each year.2
Who is more likely to get food poisoning?
Although anyone can get food poisoning, some people are more likely to get food poisoning than others, including
- infants and children
- pregnant women and their fetuses
- older adults
- people with weak immune systems
People in these groups are also more likely to have severe symptoms or complications of food poisoning. Food safety is especially important for people in these groups. Learn more about food safety for people who are more likely to get food poisoning and have complications.

What are the complications of food poisoning?
In some cases, food poisoning can lead to dehydration, hemolytic uremic syndrome, or other complications. However, serious complications are uncommon. In most cases, food poisoning lasts only a short time, and most people recover without developing complications.
Dehydration
Dehydration is the most common complication of food poisoning. When food poisoning causes you to vomit or have diarrhea, your body loses fluids and electrolytes. If you don’t replace those fluids and electrolytes, you may become dehydrated. When you are dehydrated, your body doesn’t have enough fluid and electrolytes to work properly. See a list of symptoms of dehydration.
Dehydration is especially dangerous in children, older adults, and people with weakened immune systems. If you are dehydrated, see a doctor right away to prevent serious health problems. Without treatment, dehydration can lead to problems such as organ damage, shock, coma, or even death.
Hemolytic uremic syndrome
Hemolytic uremic syndrome (HUS) is a kidney condition that happens when red blood cells are destroyed and block the kidneys’ filtering system. If your kidneys stop working, you have acute kidney injury—the sudden and temporary loss of kidney function.
The most common cause of HUS is infection with a strain of Escherichia coli (E. coli) bacterium called E. coli O157:H7, although other bacteria and viruses may also cause this condition. HUS is most common in children younger than age 5. 3, 4
See a list of symptoms of HUS.
Other complications
In some cases, food poisoning may lead to serious health problems such as
- health problems during pregnancy and pregnancy complications. Some types of food poisoning during pregnancy can cause complications, such as dehydration, for the pregnant woman or can affect the fetus. For example, food poisoning by the bacterium Listeria can cause miscarriage or stillbirth.
- Guillain-Barre syndrome, which may occur after food poisoning caused by bacteria or viruses, most commonly Campylobacter jejuni.
- irritable bowel syndrome, which may occur after food poisoning caused by various bacteria, viruses, or parasites.
- problems breathing due to botulism—a rare type of food poisoning caused by Clostridium botulinum and sometimes by Clostridium butyricum or Clostridium baratii—and some forms of fish and shellfish poisoning, which affect the nervous system and may paralyze the muscles that control your breathing.
- reactive arthritis, which may occur after food poisoning by certain bacteria, viruses, and parasites, including Campylobacter jejuni and Salmonella.
References
Symptoms & Causes
On this page:
- What are the symptoms of food poisoning?
- What are the symptoms of dehydration?
- Seek care right away
- What causes food poisoning?
- What kinds of microbes cause food poisoning?
- How do harmful chemicals cause food poisoning?
What are the symptoms of food poisoning?
Common symptoms of food poisoning include
Symptoms range from mild to severe and may last from a few hours to several days.
Less commonly, some types of food poisoning—such as botulism and fish and shellfish poisoning—can affect your nervous system. Symptoms may include
- blurred vision
- headache
- paralysis
- tingling or numbness of your skin
- weakness
People with nervous system symptoms should see a doctor or go to an emergency room right away.
What are the symptoms of dehydration?
Symptoms of dehydration, the most common complication of food poisoning, may include the following in adults
- extreme thirst and dry mouth
- urinating less than usual
- light-headedness; dizziness, which may occur when the person stands up; or fainting
- feeling tired
- dark-colored urine
- decreased skin turgor, meaning that when you pinch and release the person’s skin, it does not flatten back to normal right away
- sunken eyes or cheeks
If you are the parent or caretaker of an infant or a young child with symptoms of food poisoning, you should watch for the following signs of dehydration
- thirst and dry mouth
- urinating less than usual, or no wet diapers for 3 hours or more
- lack of energy
- no tears when crying
- decreased skin turgor, meaning that when you pinch and release the child’s skin, it does not flatten back to normal right away
- sunken eyes or cheeks
Anyone with signs or symptoms of dehydration should see a doctor or go to an emergency room right away. A person with severe dehydration may need treatment at a hospital.
Seek care right away
Food poisoning can become dangerous if it leads to severe dehydration or other complications. The symptoms listed below may suggest that an adult or child has a severe form of food poisoning, dehydration or other complications, or a serious health problem other than food poisoning. Anyone with these signs or symptoms should see a doctor right away.
Adults
Adults with any of the following symptoms should see a doctor right away
- change in mental state, such as irritability, lack of energy, or confusion
- high fever
- vomiting often
- six or more loose stools in a single day
- diarrhea that continues for more than 3 days
- nervous system symptoms
- severe pain in the abdomen or rectum
- stools that are black and tarry or contain blood or pus
- symptoms of dehydration or other complications
Adults should also see a doctor if they aren’t able to drink enough liquids or oral rehydration solutions—such as Pedialyte, Naturalyte, Infalyte, and CeraLyte—to prevent dehydration or if they do not improve after drinking oral rehydration solutions.
Older adults, pregnant women, and adults with a weakened immune system or another health condition should also see a doctor right away if they have any symptoms of food poisoning.
Infants and children
If an infant or child has signs or symptoms of food poisoning, don’t hesitate to call a doctor for advice. Diarrhea is especially dangerous in newborns and infants, leading to severe dehydration in just a day or two. A child with symptoms of dehydration can die within a day if left untreated.
If you are the parent or caretaker of an infant or child with any of the following signs or symptoms, seek a doctor’s help right away
- change in the child’s mental state, such as irritability or lack of energy
- diarrhea lasting more than a day
- any fever in infants
- high fever in older children
- frequent loose stools
- vomiting often
- nervous system symptoms
- severe pain in the abdomen or rectum
- signs or symptoms of complications, such as dehydration or hemolytic uremic syndrome
- stools that are black and tarry or contain blood or pus
You should also seek a doctor’s help right away if a child has signs or symptoms of food poisoning and the child is an infant, was born prematurely, or has a history of other medical conditions. Also seek a doctor’s help right away if the child is not able to drink enough liquids or oral rehydration solutions to prevent dehydration or if the child does not improve after drinking oral rehydration solutions.

What causes food poisoning?
Infections with microbes—viruses, bacteria, and parasites—cause most food poisoning.2 Harmful chemicals also cause some cases of food poisoning.
Microbes can spread to food at any time while the food is grown, harvested or slaughtered, processed, stored, shipped, or prepared.
Some harmful microbes may already be present in foods when you buy them. Foods that may contain microbes include
- fresh produce
- raw or undercooked meat, poultry, and eggs
- dairy products and fruit juices that have not been pasteurized—heated to kill harmful microbes
- fish and shellfish
- foods that people handle during preparation, sometimes called “deli foods,” such as sliced meat, salads and cut fruit, sandwiches, and baked goods
- processed and ready-to-eat meats such as hot dogs or deli meat
- foods that are not properly canned or sealed
If you don’t keep raw foods—such as beef, poultry, seafood, and eggs—separate from other foods, microbes from the raw foods can spread to other foods. Microbes can also spread from raw foods to your hands, kitchen utensils, cutting boards, and kitchen surfaces during food preparation. If you don’t wash your hands, utensils, cutting boards, and surfaces completely after they have come into contact with raw foods, they can spread microbes to other foods.

Microbes can cause food poisoning if you don’t take steps to kill or slow the growth of microbes in food. Microbes can grow if people don’t cook food thoroughly, keep cooked food hot, or promptly refrigerate or freeze food that can spoil.
Microbes present in the stool or vomit of people who are infected can also spread to food and cause food poisoning. People may spread these microbes to foods and drinks, especially if they don’t wash their hands thoroughly after using the bathroom, after changing a diaper, and before preparing foods and drinks.
Find tips to keep food safe and help prevent food poisoning.
What kinds of microbes cause food poisoning?
Viruses
Viruses invade normal cells in your body. Many viruses cause infections that can be spread from person to person.
If water comes into contact with stools of infected people, the water may become contaminated with a virus. The contaminated water can spread the virus to foods. For example, if contaminated water is used to water or wash produce, the virus can spread to the produce. Similarly, shellfish that were living in contaminated water could contain a virus.
If people who are infected with a virus prepare or handle foods, they may spread the virus to the foods.
Common viruses that cause food poisoning include norovirus and hepatitis A.
Bacteria
Bacteria are tiny organisms that can cause infection or disease. Bacteria can enter your body through contaminated food or water.
Bacteria grow quickly when the temperature of food is between 40 and 140 degrees. Keeping food colder than 40 degrees in a refrigerator or freezer can slow or stop the growth of bacteria. Cooking food thoroughly often kills bacteria.
Many types of bacteria can cause food poisoning, including
- certain types of Salmonella
- certain types of Clostridium, including the common C. perfringens and the less common C. botulinum, which causes an illness called botulism
- certain types of Campylobacter, including C. jejuni
- Staphylococcus aureus, also called staph
- Escherichia coli, also called E. coli
- certain types of Vibrio
- Listeria monocytogenes, also called Listeria
Parasites
Parasites are tiny organisms that live inside other organisms. Parasites can enter your body through food or water and settle in your digestive tract. In developed countries such as the United States, parasitic infections are rare.
Parasites that cause food poisoning include
- Toxoplasma gondii, which causes an illness called toxoplasmosis
- Giardia
- Cryptosporidium, which causes an illness called cryptosporidiosis or crypto
Travelers’ diarrhea
People who travel from the United States to developing countries may develop travelers’ diarrhea. Eating food or drinking water contaminated with bacteria, parasites, or viruses causes travelers’ diarrhea. Although travelers’ diarrhea is most often acute, some parasites cause diarrhea that lasts longer.
How do harmful chemicals cause food poisoning?
Harmful chemicals may be present in certain foods, including
- fish and shellfish that contain toxins produced by algae or bacteria
- certain types of wild mushrooms
- unwashed produce that contains large amounts of chemical pesticides
Diagnosis
How do doctors diagnose food poisoning?
Doctors often diagnose food poisoning based on your symptoms. If your symptoms are mild and last only a short time, you typically won’t need tests.
In some cases, a medical history, a physical exam, stool tests, and blood tests can help diagnose food poisoning. Your doctor may perform additional tests to check for complications or to rule out other health problems. Your doctor may need to contact the health department to report your illness.
Medical history
Your doctor will ask you about your symptoms, for example
- what symptoms you have
- how long you have had symptoms
- how often you have had symptoms
Your doctor will also ask about
- what you recently ate and drank
- whether you know other people who have recently had similar symptoms
- recent travel to developing countries
- current and past medical conditions
- prescription and over-the-counter medicines you take
Physical exam
During a physical exam, your doctor may
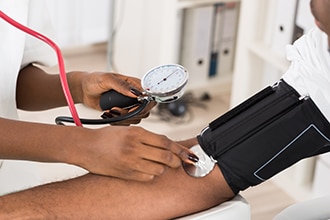
- check your blood pressure and pulse for signs of dehydration
- examine your body for signs of fever or dehydration
- use a stethoscope to listen to sounds in your abdomen
- tap on your abdomen to check for tenderness or pain
Sometimes, doctors perform a digital rectal exam to check for blood in your stool. Blood in your stool may be a sign of an infection with bacteria or parasites.
Stool tests
A health care professional will give you a container for catching and storing the stool. You will receive instructions on where to send or take the container for analysis. Stool tests can show the presence of viruses, bacteria, or parasites.
Blood tests
A health care professional may take a blood sample from you and send the sample to a lab. Blood tests can show signs of certain infections or signs of complications such as dehydration.
Treatment
How can I treat food poisoning?
In most cases, people with food poisoning get better on their own without medical treatment. You can treat food poisoning by replacing lost fluids and electrolytes to prevent dehydration. In some cases, over-the-counter medicines may help relieve your symptoms.
When you have food poisoning, you may vomit after you eat or lose your appetite for a short time. When your appetite returns, you can most often go back to eating your normal diet, even if you still have diarrhea. Find tips on what to eat when you have food poisoning.
If your child has symptoms of food poisoning, such as vomiting or diarrhea, don’t hesitate to call a doctor for advice.
Replace lost fluids and electrolytes
When you have food poisoning, you need to replace lost fluids and electrolytes to prevent dehydration or treat mild dehydration. You should drink plenty of liquids. If vomiting is a problem, try sipping small amounts of clear liquids. Replacing lost fluids and electrolytes is the most important treatment for food poisoning.
Adults. Most adults with food poisoning can replace fluids and electrolytes with liquids such as
- water
- fruit juices with water added to dilute the juice
- sports drinks
- broths
Eating saltine crackers can also help replace electrolytes.
Older adults, adults with a weakened immune system, and adults with severe diarrhea or symptoms of dehydration should drink oral rehydration solutions, such as Pedialyte, Naturalyte, Infalyte, and CeraLyte. Oral rehydration solutions are liquids that contain glucose and electrolytes.
Children. If your child has food poisoning, you should give your child an oral rehydration solution—such as Pedialyte, Naturalyte, Infalyte, and CeraLyte—as directed. Talk with a doctor about giving these solutions to your infant. Infants should drink breast milk or formula as usual.
Over-the-counter medicines
In some cases, adults can take over-the-counter medicines such as loperamide (Imodium) and bismuth subsalicylate (Pepto-Bismol, Kaopectate) to treat diarrhea caused by food poisoning.
These medicines can be dangerous for infants and children. Talk with a doctor before giving your child an over-the-counter medicine.
If you have bloody diarrhea or fever—signs of infections with bacteria or parasites—don’t use over-the-counter medicines to treat diarrhea. See a doctor for treatment.
How do doctors treat food poisoning?
To treat food poisoning caused by bacteria or parasites, your doctor may prescribe antibiotics or medicines that target parasites, in addition to rehydration solutions.
In some cases, doctors may recommend probiotics. Probiotics are live microbes, most often bacteria, that may be similar to microbes you normally have in your digestive tract. Studies suggest that some probiotics may help shorten a bout of diarrhea. Researchers are still studying the use of probiotics to treat food poisoning. For safety reasons, talk with your doctor before using probiotics or any other complementary or alternative medicines or practices. This is especially important when children, older adults, or those with weak immune systems have diarrhea.
Doctors may need to treat people with life-threatening symptoms and complications—such as severe dehydration, hemolytic uremic syndrome, or paralysis—in a hospital.
How can I prevent food poisoning?
You can prevent some food poisoning by properly storing, cooking, cleaning, and handling foods. For example,
- keep raw meat, poultry, seafood, and eggs separate from other foods
- prepare salads and refrigerate them before handling raw meat, poultry, seafood, or eggs
- promptly refrigerate or freeze foods that can spoil
- wash your hands with soap and water before and after handling food
- wash fruits and vegetables before eating, cutting, or cooking
- cook foods long enough and at high enough temperatures to kill harmful microbes
- wash utensils and surfaces after each use
- don’t eat foods that can spoil that have been sitting out for more than 2 hours, or in temperatures over 90 degrees, for more than 1 hour

Food safety is especially important for people who are more likely to get food poisoning and related complications, including
- infants and children
- pregnant women and their fetuses
- older adults
- people with weak immune systems
Find tips on food safety for people in these groups.
Food recalls
You can help prevent food poisoning by watching for food recalls. Companies recall foods—take foods off the market—if they find out that the foods could make people sick. If you learn that a food was recalled because it could cause food poisoning, check to see if you have the food. If you do, make sure no one eats it. You can return the food to the store or dispose of it.
Learn more about recently recalled foods.
Travelers’ diarrhea
To reduce your chances of getting travelers’ diarrhea when traveling to developing countries, avoid eating or drinking the following
- unbottled or untreated water. Also avoid brushing your teeth with unbottled or untreated water. Tap, well, lake, or river water may contain microbes.
- ice, foods, and drinks prepared with untreated tap or well water.
- unpasteurized juice, milk, and milk products like cheese or yogurt. Pasteurization kills harmful microbes.
- food or drinks from street vendors.
- warm food that was not served hot.
- raw or undercooked meat, fish, or shellfish.
- raw vegetables and fruits that you have not washed in clean water or peeled yourself.
If you are worried about travelers’ diarrhea, talk with your doctor before traveling. Your doctor may recommend ways that you can treat local water to kill or remove harmful microbes. Your doctor may also recommend that you bring antibiotics with you in case you get diarrhea during your trip. Early treatment with antibiotics can shorten a case of travelers’ diarrhea. Doctors may prescribe an antibiotic such as rifaximin (Xifaxan) or rifamycin (Aemcolo) to treat adults with travelers’ diarrhea caused by certain strains of Escherichia coli (E. coli) who do not have fever or blood in the stool. For severe travelers’ diarrhea, your doctor may prescribe azithromycin (Zithromax, Zmax) or ciprofloxacin (Cipro).
Doctors may advise some people—especially people with weakened immune systems—to take antibiotics before and during a trip to help prevent travelers’ diarrhea.
Eating, Diet, & Nutrition
What should I eat if I have food poisoning?
When you have food poisoning, you should drink plenty of liquids to replace lost fluids and electrolytes. You may vomit after you eat or lose your appetite for a short time. When your appetite returns, you can most often go back to eating your normal diet, even if you still have diarrhea.
When children have food poisoning, parents and caretakers should give children what they usually eat as soon as their appetite returns. Parents and caretakers should give infants breast milk or formula as usual.

What should I avoid eating if I have food poisoning?
For some people, certain food ingredients may make food poisoning symptoms, such as diarrhea, worse, including
- drinks with caffeine, such as coffee and tea, and some soft drinks.
- foods that are high in fat, such as fried foods, pizza, and fast foods.
- foods and drinks that contain large amounts of simple sugars, such as sweetened beverages and some fruit juices.
- milk and milk products, which contain the sugar lactose. Some people recovering from food poisoning have problems digesting lactose for up to a month or more afterward.
Research shows that following a restricted diet does not help treat diarrhea. Most experts do not recommend fasting or following a restricted diet when you have diarrhea.
Clinical Trials
The National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) and other components of the National Institutes of Health (NIH) conduct and support research into many diseases and conditions, including digestive diseases.
What are clinical trials for food poisoning?
Clinical trials—and other types of clinical studies—are part of medical research and involve people like you. When you volunteer to take part in a clinical study, you help doctors and researchers learn more about disease and improve health care for people in the future.
Researchers are studying many aspects of food poisoning, such as
- treatments for norovirus infection
- vaccines for Escherichia coli infection
- prevention of travelers’ diarrhea
Find out if clinical studies are right for you.
Watch a video of NIDDK Director Dr. Griffin P. Rodgers explaining the importance of participating in clinical trials.
What clinical studies for food poisoning are looking for participants?
You can find clinical studies on food poisoning at ClinicalTrials.gov. In addition to searching for federally funded studies, you can expand or narrow your search to include clinical studies from industry, universities, and individuals; however, the NIH does not review these studies and cannot ensure they are safe. Always talk with your health care provider before you participate in a clinical study.
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
The NIDDK would like to thank: Cynthia L. Sears, M.D., Johns Hopkins University School of Medicine
