Irritable Bowel Syndrome in Children
Return to Overview PageDefinition & Facts
In this section:
- What is IBS?
- Does IBS have another name?
- Are there different types of IBS in children?
- How common is IBS in children?
- Which children are more likely to develop IBS?
What is IBS?
Irritable bowel syndrome (IBS) is a group of symptoms that occur together, including repeated pain in the abdomen and changes in bowel movements, which may be diarrhea, constipation, or both. With IBS, a child has these symptoms without any visible signs of damage or disease in the digestive tract.
IBS is a functional gastrointestinal (GI) disorder. Functional GI disorders, which doctors now call disorders of gut-brain interactions, are related to problems with how the brain and gut work together. These problems can cause the gut to be more sensitive and change how the muscles in the bowel contract. If a child’s gut is more sensitive, the child may feel more abdominal pain. Changes in how the muscles in the bowel contract lead to diarrhea, constipation, or both.

Does IBS have another name?
In the past, doctors called IBS colitis, mucous colitis, spastic colon, nervous colon, and spastic bowel.
Are there different types of IBS in children?
Experts have defined four types of IBS in children. Each type has a different pattern of changes in bowel movements or abnormal bowel movements. Knowing which type of IBS a child has may help the doctor treat IBS symptoms.
IBS with constipation (IBS-C)
In IBS-C, more than a quarter of stools are hard or lumpy, and less than a quarter of stools are loose or watery.
IBS with diarrhea (IBS-D)
In IBS-D, more than a quarter of stools are loose or watery, and less than a quarter of stools are hard or lumpy.
IBS with mixed bowel habits (IBS-M)
In IBS-M, more than a quarter of stools are hard or lumpy, and more than a quarter of stools are loose or watery.
IBS unsubtyped (IBS-U)
In IBS-U, less than a quarter of stools are hard or lumpy, and less than a quarter of stools are loose or watery.
How common is IBS in children?
Studies suggest that about 5 percent of children ages 4 to 18 years old have IBS.1
Which children are more likely to develop IBS?
IBS is more common in children who have a history of- bacterial infections in the digestive tract
- certain emotional or mental health problems, such as stress, depression, and anxiety
- events during infancy or early childhood that cause pain or inflammation such as allergies, infections, or surgery
- experiencing child abuse
- family members with IBS
References
Symptoms & Causes
What are the symptoms of IBS in children?
In children with irritable bowel syndrome (IBS), the most common symptoms are
- pain in the abdomen, often related to bowel movements
- changes in bowel movements, which may be diarrhea, constipation, or both, depending on which type of IBS a child has
Other symptoms of IBS in children may include
IBS can be painful, but it doesn’t lead to other health problems or damage the digestive tract.
To diagnose IBS, your child’s doctor will look for a certain pattern in your child’s symptoms over time. IBS is a chronic disorder, meaning it lasts a long time, often years. However, the symptoms may come and go.

What causes IBS in children?
Doctors aren’t sure what causes IBS in children. Experts think that a combination of problems may lead to IBS. Different factors may cause IBS in different children.
Functional gastrointestinal (GI) disorders such as IBS are problems with brain-gut interaction—how the brain and gut work together. Experts think that problems with brain-gut interaction may affect how the body works and cause IBS symptoms. For example, some children with IBS may feel pain when a normal amount of gas or stool is in their gut. In some children with IBS, food may move too slowly through the digestive tract.
Certain problems —such as bacterial infections in the digestive tract, emotional and mental health problems, early life events that cause stress or inflammation and child abuse —are more common in children with IBS. Experts think these problems may play a role in causing IBS. Changes in the microbiome—the bacteria in the digestive tract that help with digestion—may also play a role.
Research suggests that genes may make some children more likely to develop IBS.
Diagnosis
How do doctors diagnose IBS in children?
To diagnose irritable bowel syndrome (IBS), doctors review a child’s symptoms and medical and family history and perform a physical exam. In some cases, doctors may order tests to rule out other health problems.
Review of a child’s symptoms
The doctor will ask about a child’s symptoms and look for a certain pattern in the symptoms to diagnose IBS.
The doctor may diagnose IBS if a child has pain in his or her abdomen at least 4 days each month along with one or more of the following symptoms
- pain related to bowel movements. For example, the pain may improve or get worse after bowel movements.
- a change in how often a child has a bowel movement.
- a change in the way a child’s stools look.
The doctor may diagnose IBS if
- the child has had symptoms for at least 2 months
- the child’s symptoms can’t be fully explained by another health problem
If a child has pain in the abdomen and constipation, the doctor may ask questions about how the pain is related to constipation. If abdominal pain goes away when the constipation goes away, the child may have a functional GI disorder called functional constipation instead of IBS.
The doctor will also ask about symptoms that could suggest a child has another health problem instead of IBS. These symptoms include
- arthritis
- bleeding from the rectum, bloody stools, or stools that are black and tarry
- disease in the tissues around the rectum
- nighttime diarrhea
- persistent pain in the upper or lower right side of the abdomen
- persistent vomiting
- problems or pain when swallowing
- unexplained fever
- weight loss, slowed growth, or delayed puberty
Medical and family history
The doctor will ask about the child’s
- diet and foods that may be related to symptoms
- history of emotional or mental health problems
- history of health problems other than IBS that could be causing the child’s symptoms
- medicines
- recent infections
- stressful events related to the start of symptoms
The doctor will also ask about the child’s family history of IBS and digestive diseases and disorders, such as celiac disease, inflammatory bowel disease, or peptic ulcer disease.
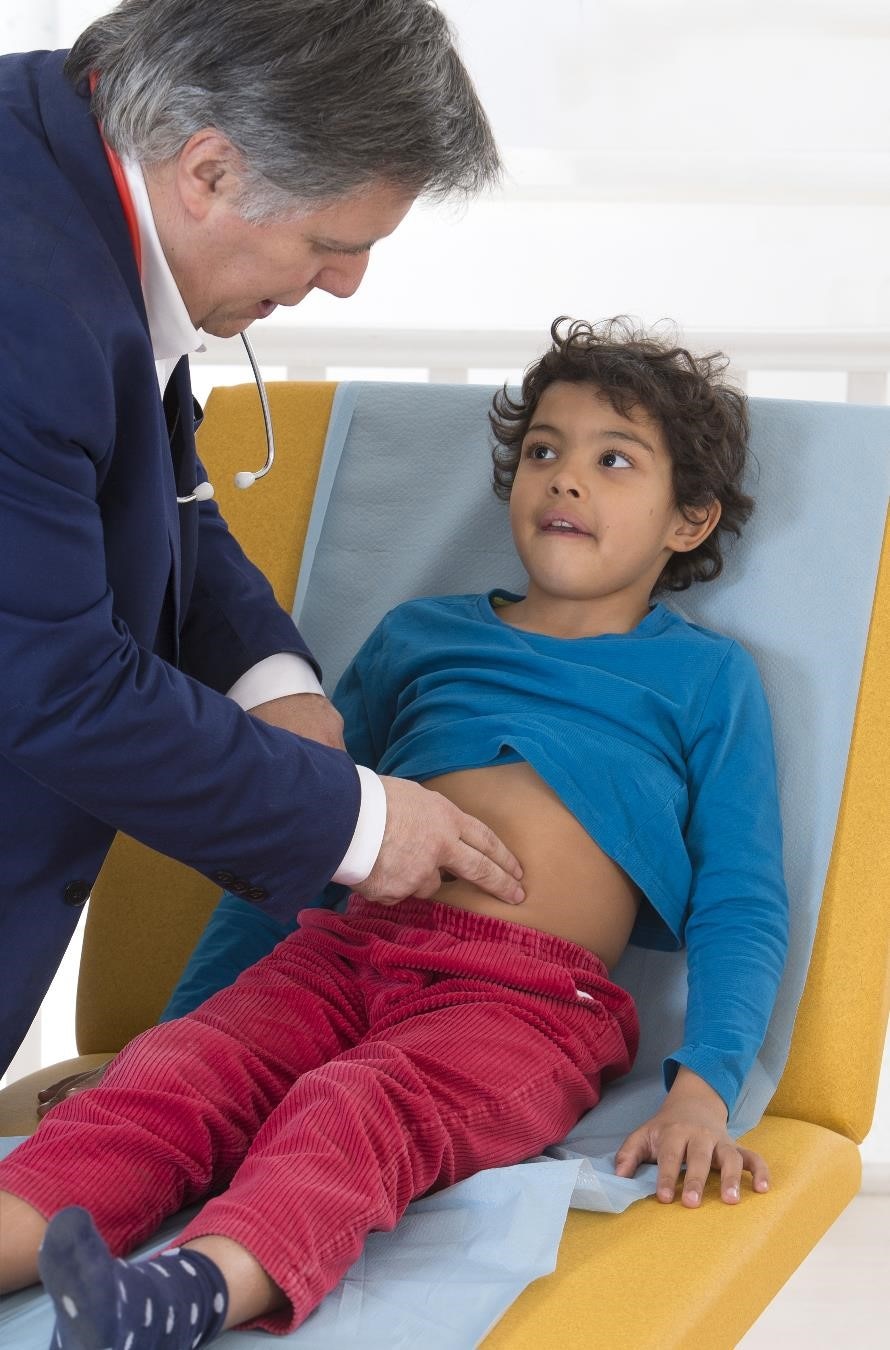
Physical exam
During a physical exam, a child’s doctor usually
- checks for lumps or swelling in the abdomen
- checks height and weight
- examines the child’s body for signs of health problems other than IBS
- listens to sounds in the abdomen using a stethoscope
- taps on the abdomen to check for tenderness or pain
What tests do doctors use to diagnose IBS in children?
The doctor may order blood tests, stool tests, and other tests to check for health problems other than IBS that could be causing a child’s symptoms.
Blood test
A health care professional will take a blood sample and send the sample to a lab. Doctors use blood tests to check for conditions other than IBS, including anemia, infection, and digestive diseases.
Stool test
The doctor will give the child or a caregiver a container for catching and holding a stool sample, along with instructions on where to send or take the kit for testing. Doctors use stool tests to check for blood in stool or other signs of infections or diseases. A doctor may also do a rectal exam, sometimes during the physical exam, to check for constipation, tenderness in the rectum, and other problems.
Other tests
The doctor may perform other tests to rule out health problems that cause symptoms similar to IBS symptoms. The doctor will decide whether the child needs other tests based on
- blood or stool test results
- a family history of digestive diseases
- symptoms that could be signs of another condition or disease
Other tests may include
- imaging tests such as abdominal ultrasound
- upper GI endoscopy with a biopsy to check for celiac disease or other problems in the upper GI tract
- colonoscopy to check for problems in the lower GI tract such as inflammatory bowel disease
Treatment
How do doctors treat IBS in children?
Doctors may treat irritable bowel syndrome (IBS) in children by recommending changes in what a child eats, mental health therapies, probiotics, and medicines. A child may have to try a few treatments to see what works best. Your child’s doctor can help find the right treatment plan.
If a child has pain in the abdomen and constipation, the doctor may recommend treatments for constipation first. If abdominal pain goes away when the constipation has been treated, the child may have a functional GI disorder called functional constipation instead of IBS.
Changes in what a child eats
Your child’s doctor or dietitian can help plan a well-balanced diet. Read more about eating, diet, and nutrition for IBS.
Mental health therapies
Mental health therapies may improve IBS symptoms, help children cope with symptoms, and prevent symptoms from interfering with school and other activities. Therapies doctors may recommend for children with IBS include
- cognitive behavioral therapy, which focuses on helping change thought and behavior patterns
- gut-directed hypnotherapy, in which a therapist uses hypnosis, a trance-like state in which the child is relaxed or focused

Probiotics
Your child’s doctor may recommend probiotics to help treat IBS symptoms. Probiotics are live microorganisms, most often bacteria, that may be similar to microorganisms that are normally in the digestive tract. Researchers are still studying the use of probiotics to treat IBS.
To be safe, talk with your child’s doctor before using probiotics or any other complementary or alternative medicines or practices. If your child’s doctor recommends probiotics, talk with the doctor about how much probiotics your child should take and for how long.
Medicines
In some cases, doctors may recommend medicines to help relieve your child’s IBS symptoms. Don’t give your child medicines to treat IBS unless told to do so by your child’s doctor. The type of medicine the doctor recommends will depend on your child’s symptoms. Recommended medicines might include
Eating, Diet, & Nutrition
Can changes in what a child eats help treat IBS symptoms?
In some cases, doctors may recommend changes in what a child eats to help treat IBS symptoms. Talk with your child’s doctor about your child’s diet and whether certain foods appear to be related to IBS symptoms. The doctor may refer your child to a dietitian.
Research suggests that some children with IBS may benefit from reducing the amount of FODMAPs—carbohydrates that are hard to digest—in their diet. For some children with IBS, doctors or dietitians may recommend a low FODMAP diet. With the guidance of a doctor or dietitian, the child would eat less of certain foods that contain FODMAPs for a short time and then gradually add those foods back into his or her diet.
Talk with your child’s doctor or dietician before making any changes to your child’s diet to try to treat IBS symptoms. Proper nutrition is important for growth and development. Trained professionals can help you and your child plan a well-balanced diet and develop or maintain healthy eating habits.

Clinical Trials
The NIDDK conducts and supports clinical trials in many diseases and conditions, including digestive diseases. The trials look to find new ways to prevent, detect, or treat disease and improve quality of life.
Why are clinical trials with children important?
Children respond to medicines and treatments differently than adults. The way to get the best treatments for children is through research designed specifically for them.
We have already made great strides in improving children's health outcomes through clinical trials—and other types of clinical studies. Vaccines, treatments for children with cancer, and interventions for premature babies are just a few examples of how this targeted research can help. However, we still have many questions to answer and more children waiting to benefit.
The data gathered from trials and studies involving children help doctors and researchers
- find the best dose of medicines for children
- find treatments for conditions that only affect children
- treat conditions that behave differently in children than in adults
- understand the differences in children as they grow
How do I decide if a clinical trial is right for my child?
We understand you have many questions, want to weigh the pros and cons, and need to learn as much as possible. Deciding to enroll in a study can be life changing for you and for your child. Depending on the outcome of the study, your child may find relief from their condition, see no benefit, or help to improve the health of future generations.
Talk with your child and consider what would be expected. What could be the potential benefit or harm? Would you need to travel? Is my child well enough to participate? While parents or guardians must give their permission, or consent, for their children to join a study, the children must also agree to participate, if they are capable (verbal). In the end, no choice is right or wrong. Your decision is about what is best for your child.
The National Institutes of Health (NIH) is committed to ensuring you get all the information you need to feel comfortable and make informed decisions. The safety of children remains the utmost priority for all NIH research studies. For more resources to help decide if clinical trials are right for your child, visit Clinical Trials and You: Parents and Children.
What aspects of IBS are being studied in children?
Researchers study many aspects of IBS such as
- how the microbiome and diet affect IBS symptoms
- the management of digestive disorders such as IBS
- the relationship between chronic abdominal pain and intestinal inflammation
Watch a video of NIDDK Director Dr. Griffin P. Rodgers explaining the importance of participating in clinical trials.
What clinical studies for IBS are available for child participants?
You can view a filtered list of clinical studies on IBS in children that are federally funded, open, and recruiting at ClinicalTrials.gov. You can expand or narrow the list to include clinical studies from industry, universities, and individuals; however, the NIH does not review these studies and cannot ensure they are safe. If you find a trial you think may be right for your child, talk with your child’s doctor about how to enroll.
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
The NIDDK would like to thank:
Carlo Di Lorenzo, M.D., Nationwide Children's Hospital
