Managing Chronic Kidney Disease
If you have chronic kidney disease (CKD), you can take steps to protect your kidneys from more damage.
The sooner you know you have kidney disease, the better. The steps you take to protect your kidneys from damage also may help prevent heart disease—and improve your health overall. Making these changes when you have no symptoms may be hard, but it’s worthwhile.
Control your blood pressure
The most important step you can take to treat kidney disease is to control your blood pressure. High blood pressure can damage your kidneys. You can protect your kidneys by keeping your blood pressure at or less than the goal set by your health care provider. For most people, the blood pressure goal is less than 140/90 mm Hg.
Work with your health care provider to develop a plan to meet your blood pressure goals. Steps you can take to meet your blood pressure goals may include eating heart-healthy and low-sodium meals, quitting smoking, being active, getting enough sleep, and taking your medicines as prescribed.
Meet your blood glucose goal if you have diabetes
To reach your blood glucose goal, check your blood glucose level regularly. Use the results to guide decisions about food, physical activity, and medicines. Ask your health care provider how often you should check your blood glucose level.
Your health care provider will also test your A1C. The A1C is a blood test that measures your average blood glucose level over the past 3 months. This test is different from the blood glucose checks you do regularly. The higher your A1C number, the higher your blood glucose levels have been during the past 3 months. Stay close to your daily blood glucose numbers to help you meet your A1C goal.
The A1C goal for many people with diabetes is below 7 percent. Ask your health care provider what your goal should be. Reaching your goal numbers will help you protect your kidneys. Learn more about how to manage diabetes.
Work with your health care team to monitor your kidney health
The tests that health care providers use to test for kidney disease can also be used to track changes to kidney function and damage. Kidney disease tends to get worse over time. Each time you get checked, ask your provider how the test results compare to the last results. Your goals will be to
- keep your GFR the same
- keep your urine albumin the same or lower
Your health care provider will also check your blood pressure and, if you have diabetes, your A1C level, to make sure you are meeting your blood pressure and blood glucose goals.
Bring this document to your appointment to help keep track of your kidney test results (PDF, 262 KB) .
How can I prepare for visits with my health care provider?
The more you plan for your visits, the more you will be able to learn about your health and treatment options.
Make a list of questions
It’s normal to have a lot of questions. Write down your questions as you think of them so that you can remember everything you want to ask when you see your health care provider. You may want to ask about what tests are being done, what test results mean, or the changes you need to make to your diet and medicines.
Sample questions to ask your provider for people with kidney disease
About your tests
- What is my GFR? What does that mean?
- Has my GFR changed since last time?
- What is my urine albumin? What does it mean?
- Has my urine albumin changed since the last time it was checked?
- Is my kidney disease getting worse?
- Is my blood pressure where it needs to be?
About treatment and self-care
- What can I do to keep my disease from getting worse?
- Do any of my medicines or doses need to be changed?
- What time of day should I take each of my medicines?
- Do I need to change what I eat?
- Will you refer me to a dietitian for diet counseling?
- When will I need to see a nephrologist (kidney specialist)?
- Do I need to worry about dialysis or a kidney transplant?
- What do I need to do to protect my veins?
About complications
- What other health problems may I face because of my kidney disease?
- Should I be looking for any symptoms? If so, what are they?
Bring a friend or relative with you for support
A trusted friend or family member can take notes, ask questions you may not have thought of, offer support, and help remember what the provider said during the visit. Talk ahead of time about what you want to get out of the visit and the role you would like your friend or relative to play.
Who is part of my health care team?
The following health care providers may be part of the health care team involved in your treatment:

Primary care provider. Your primary care provider (PCP)—doctor, nurse practitioner, or physician assistant—is the person you see for routine medical visits. Your PCP may monitor your kidney health and help you manage your diabetes and high blood pressure. A PCP also prescribes medicines and may refer you to specialists.
Nurse. A nurse may help with your treatment and teach you about monitoring and treating kidney disease, as well as managing your health conditions. Some nurses specialize in kidney disease.
Registered dietitian. A registered dietitian is a food and nutrition expert who helps people create a healthy eating plan when they have a health condition such as kidney disease. Dietitians can help you by creating an eating plan based on how your kidneys are doing. “Renal dietitians” often work in dialysis centers and are specially trained to work with people with kidney failure.
Diabetes educator. A diabetes educator teaches people with diabetes how to manage their disease and handle diabetes-related problems.
Pharmacist. A pharmacist educates you about your medicines and fills your prescriptions. An important job for the pharmacist is to review all of your medicines, including over-the-counter (OTC) medicines, and supplements, to avoid unsafe combinations and side effects.
Social worker. When you are close to needing dialysis, you may have a chance to meet with a social worker. A dialysis social worker helps people and their families deal with the life changes and costs that come with having kidney disease and kidney failure. A dialysis social worker also can help people with kidney failure apply for help to cover treatment costs.
Nephrologist. A nephrologist is a doctor who is a kidney specialist. Your PCP may refer you to a nephrologist if you have a complicated case of kidney disease, your kidney disease is quickly getting worse, or your kidney disease is advanced.
Take medicines as prescribed
Many people with CKD take medicines prescribed to lower blood pressure, control blood glucose, and lower cholesterol.
Two types of blood pressure medicines, ACE inhibitors and ARBs, may slow kidney disease and delay kidney failure, even in people who don’t have high blood pressure. The names of these medicines end in –pril or –sartan.
Many people need to take two or more medicines for their blood pressure. You may also need to take a diuretic, sometimes called a water pill. The aim is to meet your blood pressure goal. These medicines may work better if you limit your salt intake.
Know that your medicines may change over time
Your health care provider may change your medicines as your kidney disease gets worse. Your kidneys don’t filter as well as they did in the past, and this can cause an unsafe buildup of medicines in your blood. Some medicines can also harm your kidneys. As a result, your provider may tell you to
- take a medicine less often or take a smaller dose
- stop taking a medicine or switch to a different one
Your pharmacist and health care provider need to know about all the medicines you take, including OTC medicines, vitamins, and supplements.

Be careful about the over-the-counter medicines you take
If you take OTC or prescription medicines for headaches, pain, fever, or colds, you may be taking nonsteroidal anti-inflammatory drugs (NSAIDs). NSAIDs include commonly used pain relievers and cold medicines that can damage your kidneys and lead to acute kidney injury, especially in those with kidney disease, diabetes, and high blood pressure.
Ibuprofen and naproxen are NSAIDs. NSAIDs are sold under many different brand names, so ask your pharmacist or health care provider if the medicines you take are safe to use.
You also can look for NSAIDs on Drug Facts labels like the one below:
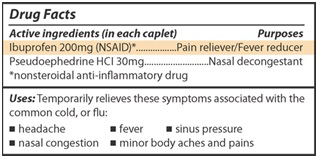
Watch a video explaining how NSAIDs can harm your kidneys.
If you have been taking NSAIDs regularly to control chronic pain, you may want to ask your health care provider about other ways to treat pain, such as meditation or other relaxation techniques. You can read more about pain management at the NIH National Center for Complementary and Integrative Health website.
Tips for managing your medicines
The next time you pick up a prescription or buy an OTC medicine or supplement, ask your pharmacist how the product may
- affect your kidneys
- affect other medicines you take
Fill your prescriptions at only one pharmacy or pharmacy chain so your pharmacist can
- keep track of your medicines and supplements
- check for harmful interactions
Keep track of your medicines and supplements:
- Keep an up-to-date list of your medicines and supplements in your wallet. Take your list with you, or bring all of your medicine bottles, to all health care visits.

Work with a dietitian to develop a meal plan
What you eat and drink can help you
- protect your kidneys
- reach your blood pressure and blood glucose goals
- prevent or delay health problems caused by kidney disease
As your kidney disease gets worse, you may need to make more changes to what you eat and drink.
A dietitian who knows about kidney disease can work with you to create a meal plan that includes foods that are healthy for you and that you enjoy eating. Cooking and preparing your food from scratch can help you eat healthier.
Nutrition counseling from a registered dietitian to help meet your medical or health goals is called medical nutrition therapy (MNT). If you have diabetes or kidney disease and a referral from your primary care provider, your health insurance may cover MNT. If you qualify for Medicare, MNT is covered.
Your health care provider may be able to refer you to a dietitian. You can also find a registered dietitian online through the Academy of Nutrition and Dietetics. Work closely with your dietitian to learn to eat right for CKD.
Make physical activity part of your routine
Be active for 30 minutes or more on most days. Physical activity can help you reduce stress, manage your weight, and achieve your blood pressure and blood glucose goals. If you are not active now, ask your health care provider about the types and amounts of physical activity that are right for you.
View physical activity and weight-management resources to help you get and stay motivated.
Aim for a healthy weight
Being overweight makes your kidneys work harder and may damage your kidneys. The NIH Body Weight Planner is an online tool to help you tailor your calorie and physical activity plans to achieve and stay at a healthy weight.
Get enough sleep
Aim for 7 to 8 hours of sleep each night. Getting enough sleep is important to your overall physical and mental health and can help you meet your blood pressure and blood glucose goals. You can take steps to improve your sleep habits.
Stop smoking
Cigarette smoking can make kidney damage worse. Quitting smoking may help you meet your blood pressure goals, which is good for your kidneys, and can lower your chances of having a heart attack or stroke. For tips on quitting, go to Smokefree.gov.
Find healthy ways to cope with stress and depression
Long-term stress can raise your blood pressure and your blood glucose and lead to depression. Some of the steps that you are taking to manage your kidney disease are also healthy ways to cope with stress. For example, physical activity and sleep help reduce stress. Listening to your favorite music, focusing on something calm or peaceful, or meditating may also help you. Learn more about healthy ways to cope with stress.
Depression is common among people with a chronic, or long-term, illness. Depression can make it harder to manage your kidney disease. Ask for help if you feel down. Seek help from a mental health professional. Talking with a support group, clergy member, friend, or family member who will listen to your feelings may help.
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
