Interstitial Cystitis (Painful Bladder Syndrome)
Return to Overview PageDefinition & Facts
In this section:
- What is IC?
- How common is IC?
- Who is more likely to develop IC?
- What other health problems do people with IC have?
- What are the complications of IC?
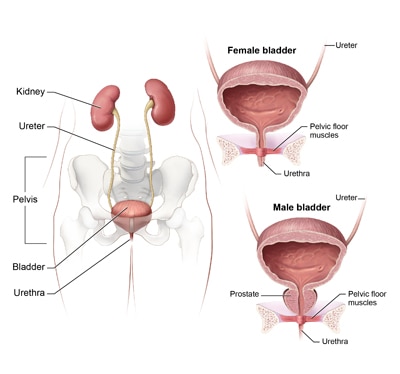
What is IC?
Interstitial cystitis (IC), also called bladder pain syndrome, is a chronic, or long-lasting, condition that causes painful urinary symptoms. Symptoms of IC may be different from person to person. For example, some people feel mild discomfort, pressure, or tenderness in the pelvic area. Other people may have intense pain in the bladder or struggle with urinary urgency, the sudden need to urinate, or frequency, the need to urinate more often.
Health care professionals diagnose IC by ruling out other conditions with similar symptoms.
Researchers don’t know the exact cause of IC. Some researchers believe IC may result from conditions that cause inflammation in various organs and parts of the body.
Severe IC symptoms can affect your quality of life. You may feel like you can’t exercise or leave your home because you have to use the bathroom too often, or perhaps your relationship is suffering because sex is painful.
Working with health care professionals, including a urologist or urogynecologist, along with a pain specialist, may help improve your IC symptoms.
How common is IC?
IC is common. The condition may affect between 3 million and 8 million women and between 1 million and 4 million men in the United States.1
Who is more likely to develop IC?
IC can occur at any age, including during childhood, but is most common in adult women and men. About twice as many women are affected as men.1 However, more men may struggle with IC than researchers originally thought.
Some research suggests that women are more likely to develop IC if they have a history of being sexually abused or physically traumatized.2
What other health problems do people with IC have?
Many women with IC are more likely to have other conditions such as irritable bowel syndrome, fibromyalgia, and chronic fatigue syndrome.3 Allergies and some autoimmune diseases are also associated with IC.4
Vulvodynia, which is chronic pain in the vulva that often causes a burning or stinging feeling, or rawness, is commonly associated with IC.2 Vulvodynia has symptoms that overlap with IC.
What are the complications of IC?
The symptoms of IC—such as urgency, frequency, and pain—may lead you to decrease your physical and social activity and negatively affect your quality of life.
Women with pelvic pain or vulvodynia often have pain during sexual intercourse, which can damage your relationships and self-image. Men also can experience pelvic pain that causes uncomfortable or painful sex. Sometimes sex can increase bladder pain attacks, also called symptom flares.
Sexual complications may cause people to avoid further intimacy, possibly leading to depression and guilt. Like many people who deal with chronic pain, people with IC are more likely to struggle with sleep loss due to the frequent need to urinate, and with anxiety and depression.5
Medical tests such as pelvic exams and Pap tests often are painful for women with IC symptoms, especially those who may have pelvic floor muscle spasm. Don’t avoid these tests. Talk with a health care professional about how to make pelvic exams and Pap tests more comfortable and how often you should have them.
References
Symptoms & Causes
What are the symptoms of IC?
People with interstitial cystitis (IC) have repeat discomfort, pressure, tenderness or pain in the bladder, lower abdomen, and pelvic area. Symptoms vary from person to person, may be mild or severe, and can even change in each person as time goes on.
Symptoms may include a combination of these symptoms:
Urgency
Urgency is the feeling that you need to urinate right now. A strong urge is normal if you haven't urinated for a few hours or if you have been drinking a lot of liquids. With IC, you may feel pain or burning along with an urgent need to urinate before your bladder has had time to fill.
Frequency
Frequency is urinating more often than you think you should need to, given the amount of liquid you are drinking. Most people urinate between four and seven times a day. Drinking large amounts of liquid can cause more frequent urinating. Taking blood pressure medicines called diuretics, or water pills, can also cause more frequent urinating. Some people with IC feel a strong, painful urge to urinate many times a day.
Pain
As your bladder starts to fill, you may feel pain—rather than just discomfort—that gets worse until you urinate. The pain usually improves for a while once you empty your bladder. People with IC rarely have constant bladder pain. The pain may go away for weeks or months and then return. People with IC sometimes refer to an attack of bladder pain as a symptom flare.
Some people may have pain without urgency or frequency. This pain may come from a spasm in the pelvic floor muscles, the group of muscles that is attached to your pelvic bones and supports your bladder, bowel, and uterus or prostate. Pain from pelvic floor muscle spasm may get worse during sex.
What causes IC?
Researchers are working to understand the causes of IC and to find treatments that work. Even though the exact cause of IC is unknown, you may find that certain events or factors start, or trigger, your symptom flares. Symptom flares can make your IC feel worse. Some people have reported that their symptom flares happen when they6
- are stressed, or have certain emotions, such as anger or sadness
- have sex
- have a menstrual cycle
- have a urinary tract infection
- urinate or hold urine for too long
- skip meals or are dehydrated
- feel changes in the seasons or the weather
- have allergies
- go through sudden or bumpy movements
- take certain medicines or forget to take their medicines
- wear tight pants and undergarments
- use laundry detergents with certain chemicals or are in pool water with certain chemicals
- use certain brands of toilet paper
- do certain physical activities, like pushing or lifting heavy objects
- stand for long periods of time
- have a Pap smear
- take antidepressants, sinus medicines, or pain relievers
Talk with your health care professional about flare management. If you know which factors make your symptoms flare, you may wish to avoid them. However, if factors that affect your health—like having sex, having a Pap smear, or taking certain medicines—make your symptom flares occur, talk with your health care professional right away.
You may also want to learn more about which foods and drinks may trigger your symptom flares.
References
Diagnosis
How do health care professionals diagnose IC?
Health care professionals will use your medical history, a physical exam, and lab tests to diagnose IC.
A health care professional will ask if you have a history of health problems related to IC. He or she will ask questions about your symptoms and other questions to help find the cause of your bladder problems.
If you are a woman who has IC symptoms, a health care professional may also perform a pelvic exam. During the pelvic exam, the health care professional will check your pelvic floor muscles to see if any of your painful symptoms are related to spasm in your pelvic floor muscles.
For men, a health care professional may perform a digital rectal exam to check for prostate problems and to check your pelvic floor muscles.
Doctors diagnose IC based on
- pain in or near the bladder, usually with urinary frequency and urgency
- the absence of other diseases and conditions that could cause similar symptoms, such as urinary tract infections (UTIs), bladder cancer, endometriosis in women, or prostatitis—infection or inflammation of the prostate—in men.
What tests do doctors use to diagnose IC?
A health care professional may use the following tests to look inside your urethra and bladder, and may even take a tissue sample from inside your bladder. The health care professional will use tests to rule out certain diseases and conditions, such as UTI and bladder cancer. If the test results are normal and all other diseases and conditions are ruled out, your doctor may diagnose IC.
Urinalysis and urine culture
At the doctor’s office, you may be given a cup to take into the bathroom. A health care professional will give you instructions for collecting urine in the cup. White and red blood cells and bacteria in the urine may indicate a UTI, which can be treated with an antibiotic.
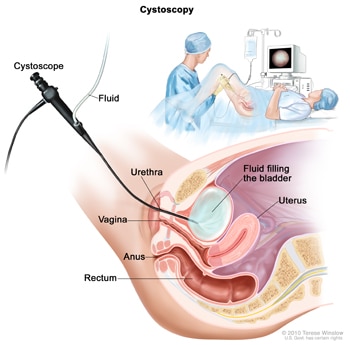
Cystoscopy
Doctors may use cystoscopy to look inside the urethra and bladder. Doctors use a cystoscope, a tubelike instrument, to look for bladder ulcers, cancer, swelling, redness, and signs of infection.
Treatment
How do doctors treat IC?
Researchers have not found one treatment for interstitial cystitis (IC) that works for everyone. Doctors aim current treatments at relieving symptoms in each person on an individual basis.
A health care professional will work with you to find a treatment plan that meets your needs. Your plan may include
- lifestyle changes
- bladder training
- physical therapy
- medicines
- bladder procedures
Some treatments may work better for you than others. You also may need to use a combination of these treatments to relieve your symptoms.
A health care professional may ask you to fill out a form, called a symptom scale, with questions about how you feel. The symptom scale may allow a health care professional to better understand how you are responding to treatment.
You may have to try several different treatments before you find one that works for you. Your symptoms may disappear with treatment, a change in what you eat, or without a clear reason. Even when your symptoms go away, they may return after days, weeks, months, or even years. Researchers do not know why. With time, you and your doctor should be able to find a treatment that gives you some relief and helps you cope with IC.
Lifestyle changes
Change your eating and drinking habits. Some people with IC find that certain foods or drinks trigger their symptoms. Others find no link between symptoms and what they eat. However, be sure to drink enough water to stay hydrated. Talk with your health care professional about how much liquid you should drink to prevent dehydration based on your health, how active you are, and where you live. Read more about eating, diet, and nutrition and how they relate to IC.
Quit smoking. Some people feel that smoking makes their IC symptoms worse. Researchers don’t know exactly how tobacco affects IC. However, smoking is a major cause of bladder cancer. If you smoke, one of the best things you can do for your bladder and overall health is to quit.
If you smoke or use other tobacco products, stop. Ask for help so you don’t have to do it alone. You can start by calling the national quitline at 1-800-QUITNOW or 1-800-784-8669. For tips on quitting, go to Smokefree.gov.
Reduce stress. Researchers don’t think stress causes IC, yet stress can trigger painful symptom flares in some people with IC. If you feel stressed, try relaxation techniques and other activities that might soothe you, such as
- looking at nature around you
- listening to soft music
- noticing smells around you
- savoring each bite of a special treat
- breathing gently
Be physically active. If you have IC, you may feel that the last thing you want to do is be physically active. However, many people feel that easy activities like walking or gentle stretching exercises help relieve symptoms.
Get support. Having the emotional support of family, friends, and other people with IC is a very important part of helping you cope. People who learn about the disorder and become involved in their own care do better than people who do not.
Bladder training
Bladder training may help your bladder hold more urine. People with bladder pain often get in the habit of using the bathroom as soon as they are aware of any need to go to avoid pain or urgency. They then feel the need to go before the bladder is really full. The body may get used to urinating often. Bladder training helps your bladder hold more urine before your body tells you to urinate.
Keep a bladder diary (PDF, 79 KB) to track how you are doing. Start by writing down the times when you urinate. For example, you may find that you return to the bathroom every 40 minutes. Try to wait a few more minutes and gradually stretch out the time between urinating. This may be easier if you are well hydrated. Read more about the importance of getting enough liquids in your diet.
If your bladder becomes painful, use the bathroom. You may find that your first urge to use the bathroom goes away if you ignore it. Find ways to relax or distract yourself when the first urge strikes.
After a week or two, you may be able to stretch the time out to 50 or 60 minutes, and you may find that the urge to urinate does not return as soon.
Bowel training
Your doctor may suggest that you try to train yourself to have a bowel movement at the same time each day to help you become more regular, also called bowel training. Consider keeping track of your bowel movements. Some people report that having regular bowel movements helps their IC symptoms. Talk with your health care professional if you are having bowel control problems, such as
Physical therapy
If you have IC symptoms or pelvic floor muscle spasm, your doctor may suggest that you work with a physical therapist who specializes in pelvic floor problems. The physical therapist will work to stretch tight pelvic floor muscles and help you keep them relaxed.
Medicines
Your doctor may suggest that you take over-the-counter (OTC) pain medicine to help control mild bladder pain, including:
- acetaminophen (Tylenol)
- aspirin (Bayer)
- ibuprofen (Advil, Motrin)
Talk with your doctor if you feel you need a stronger pain medicine. If you have severe pain, you may need your doctor to prescribe narcotic analgesics, or pain-relieving medicines, such as acetaminophen with codeine or longer-acting narcotics.
In some people, however, certain antidepressants, sinus medicines, and pain relievers may trigger symptom flares. Talk with your health care professional if these medicines make your IC worse.
Long-term use of pain medicines can be dangerous. Talk with your doctor about how to safely manage your chronic, or long-term, pain—possibly with the help of a pain specialist, a doctor who diagnoses, treats, and manages pain. You may also want to discuss alternatives to pain medicines or complementary pain medicines.
If lifestyle changes, bladder training, physical therapy, and pain medicines don’t do enough to relieve your IC symptoms, your doctor may prescribe other medicines, including:
All medicines, even OTC medicines, have side effects. Always consult a doctor before using any medicine or supplement for more than a few days.

Bladder instillation
Some people who have IC find relief after a treatment in which a doctor puts a small amount of liquid medicine into the bladder, called bladder instillation or a bladder wash or bath. The doctor guides a tube called a catheter into your bladder and slowly adds a liquid that eases irritation of the bladder wall. The liquid may be a compound called dimethyl sulfoxide (DMSO) or a solution that contains heparin, steroids, and a topical anesthetic, such as short-acting lidocaine, or long-acting marcaine.
You will be asked to keep the liquid in your bladder for about 15 minutes and then release it. You can have this treatment once every week or every other week for 1 or 2 months. You may not feel any better until the third or fourth treatment.
Bladder stretching
A doctor may use a procedure called bladder stretching, or hydrodistention, to treat your bladder pain, if only for a short time. Bladder stretching occurs when a doctor stretches your bladder by filling it with fluid. You will be given a local or general anesthesia to help you tolerate the bladder stretching.
Some people have temporary relief of their symptoms after this treatment. Researchers are not exactly sure why bladder stretching helps some people. Stretching may temporarily block pain signals sent by nerves in the bladder.
Sometimes your pain symptoms may temporarily get worse 4 to 48 hours after bladder stretching. However, your pain levels should return to your previous level or improve within 2 to 4 weeks.
Surgery
Most people with IC do not require surgery. If you’ve tried every other option and your pain is still unbearable, you and your doctor may consider surgery to either
- make the bladder larger, a procedure called bladder augmentation,
- remove the bladder, called cystectomy, or
- reroute the normal flow of urine, called urinary diversion
Talk with your doctor and family about the possible benefits and side effects of bladder surgery. Surgery does not cure the pain of IC in all cases.
Eating, Diet, & Nutrition
Can what I eat or drink relieve or prevent IC?
No research consistently links certain foods or drinks to IC. However, some research strongly suggests a relationship between diet and symptoms. Healthy eating and staying hydrated are important for your overall health, including bladder health.

However, some people with IC find that certain foods or drinks trigger or worsen their symptoms. Coffee, soda, alcohol, tomatoes, hot and spicy foods, chocolate, caffeinated beverages, citrus juices and drinks, MSG, and high-acid foods can trigger IC symptoms or make them worse. Some people also note that their symptoms get worse after eating or drinking products with artificial sweeteners, or sweeteners that are not found naturally in foods and beverages.
Learning which foods trigger your symptoms or make them worse may take some effort. Keep a food diary and note the times you have bladder pain. For example, the diary might show that your symptom flares always happen after you eat tomatoes or oranges. If you find that certain foods make your symptoms worse, your health care professional and dietitian can help you avoid them with an eating plan. Find an expert to advise you on how to use nutrition and ingredient information on a food label. You can use this information to help you avoid eating or drinking things that trigger pain in your bladder.
Stopping certain foods and drinks—and then adding them back to what you normally eat and drink one at a time—may help you figure out which foods or drinks, if any, affect your symptoms. Talk with your health care professional about how much liquid you should drink to prevent dehydration based on your health, how active you are, and where you live. Water is the best liquid for bladder health.
Some doctors recommend taking an antacid with meals. This medicine reduces the amount of acid that gets into the urine.
Clinical Trials
The National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) and other components of the National Institutes of Health (NIH) conduct and support research into many diseases and conditions.
What are clinical trials, and are they right for you?
Clinical trials are part of clinical research and at the heart of all medical advances. Clinical trials look at new ways to prevent, detect, or treat disease. Researchers also use clinical trials to look at other aspects of care, such as improving the quality of life for people with chronic illnesses. Find out if clinical trials are right for you.
What clinical trials are open?
Clinical trials that are currently open and are recruiting can be viewed at www.ClinicalTrials.gov.
Watch a video of NIDDK Director Dr. Griffin P. Rodgers explaining the importance of participating in clinical trials.
What is the Multidisciplinary Approach to the Study of Chronic Pelvic Pain (MAPP) Research Network?
To better understand the causes of two chronic urinary pain disorders—interstitial cystitis (IC)-also called bladder pain syndrome, and chronic prostatitis/chronic pelvic pain syndrome (CP/CPPS)—the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) of the National Institutes of Health (NIH) established the Multidisciplinary Approach to the Study of Chronic Pelvic Pain (MAPP) Research Network.
The MAPP Research Network moves beyond typical bladder- and prostate-specific research and includes experts across a wide range of disciplines. Using a whole-body approach, MAPP Network scientists are studying the underlying source of symptoms, differing symptom profiles and patterns for patients, and possible connections between IC, CP/CPP, and other chronic conditions that are sometimes seen in IC and CP/CPPS patients, such as irritable bowel syndrome, fibromyalgia, and chronic fatigue syndrome.
Read more about the research being done by the MAPP Research Network.
For more information, visit the MAPP Research Network home page.
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
