Diabetes, Gum Disease, & Other Dental Problems
On this page:
- How can diabetes affect my mouth?
- What are the most common mouth problems from diabetes?
- How will I know if I have mouth problems from diabetes?
- What should I do if I have mouth problems from diabetes?
- How can I prepare for dental work?
- How can I keep my mouth healthy?
- Clinical Trials for Diabetes and Gum Disease
Diabetes affects many parts of your body, including your mouth. People with diabetes are more likely to have gum disease, cavities, and other problems with their teeth and gums.1 And some of these mouth problems can make your diabetes worse.
Taking good care of your teeth and gums, including getting regular cleanings and needed treatments, will help you prevent these problems or stop them from getting worse. Keeping your mouth healthy will also make it easier for you to manage your diabetes and prevent diabetes-related health problems, such as heart disease and kidney disease.1
 Good dental care can prevent mouth problems and help you manage your diabetes.
Good dental care can prevent mouth problems and help you manage your diabetes.How can diabetes affect my mouth?
Diabetes can affect your mouth by changing your saliva—the fluid that keeps your mouth wet. Saliva helps prevent tooth decay by washing away pieces of food, preventing bacteria from growing, and fighting the acids produced by bacteria. Saliva also has minerals that help protect tissues in your mouth and fight tooth decay.
Diabetes and some medicines used to treat diabetes can cause the salivary glands in your mouth to make less saliva. When less saliva flows, the risk for dental cavities, gum disease, and other mouth problems increases.
Diabetes can also increase the amount of glucose in your saliva. Diabetes occurs when your blood glucose level, also called blood sugar, is too high. High levels of glucose in your blood can also cause glucose to build up in your saliva. This glucose can feed harmful bacteria that combine with food to form a soft, sticky film called plaque, which causes cavities. If you don’t remove plaque, it can also build up on your teeth near your gum line and harden into a deposit called tartar, which can cause gum disease.
Untreated, these mouth problems can lead to tooth loss. Almost 25% of U.S. adults with diabetes ages 50 and older have severe tooth loss, compared with about 16% of those without diabetes.2
What are the most common mouth problems from diabetes?
Gum disease
Gum disease, also called periodontal gum disease, is the most common and serious mouth problem related to diabetes. Untreated, the disease advances in stages, from inflamed gums to tooth loss. High levels of blood glucose increase the risk that gum disease will progress from mild to severe.1
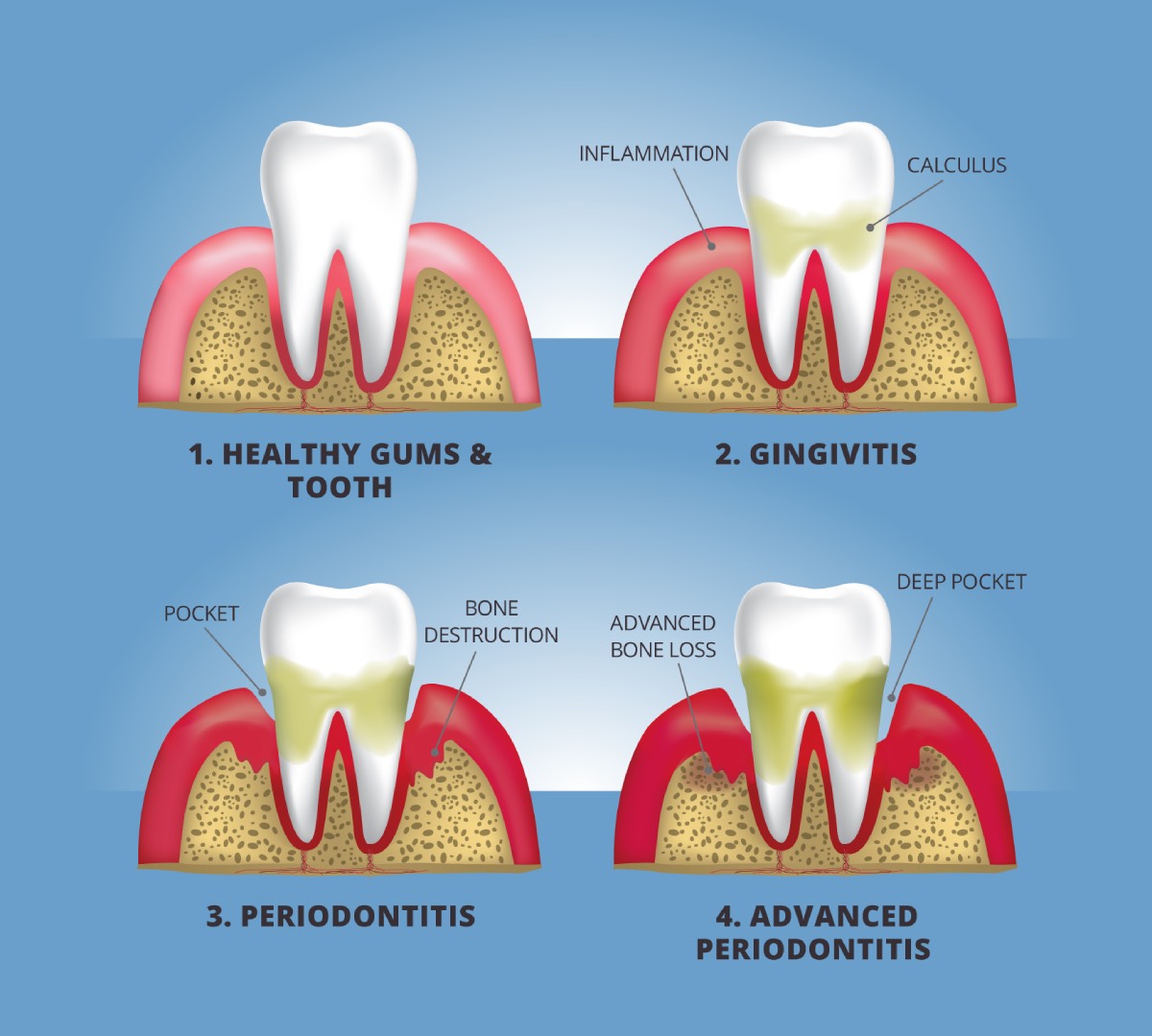 Gum disease advances in stages, from inflamed gums to tooth loss.
Gum disease advances in stages, from inflamed gums to tooth loss.
Gingivitis, or inflamed gums
The first stage of gum disease is gingivitis, a mild inflammation of the soft tissues around your teeth. Gingivitis develops when plaque and tartar build up on your teeth near your gum line, irritating and inflaming your gums. As a result, your gums may become red and swollen, and may bleed easily.
Periodontitis
Untreated, gingivitis can progress to periodontitis, an infection of the gums and bone that hold your teeth in place. Your gums may pull away from your teeth, forming pockets that slowly become infected. The bacteria in your mouth and your body’s response to the infection start to break down the bone and tissue that hold your teeth in place. If periodontitis is not treated, the teeth can become loose and may even need to be removed.
Other common mouth problems
In addition to gum disease, diabetes also increases your risk for3
- dental cavities
- dry mouth, a lack of saliva that can cause sores, ulcers, and infections
- thrush, a fungal infection that causes painful, white patches in your mouth
- burning mouth syndrome, a burning feeling inside your mouth caused by uncontrolled blood glucose levels
- changes in the way foods and beverages taste
These mouth problems, as well as tooth loss, can make it harder for you to follow a healthy meal plan that will help you manage your diabetes.
How will I know if I have mouth problems from diabetes?
Check your mouth for signs and symptoms of problems from diabetes, such as1
- gums that are
- red, swollen, or bleeding
- receding
- pulling away from your teeth
- loose teeth
- increasing spaces between your teeth
- dry mouth, an important sign of diabetes
- bad breath that doesn’t go away when you brush your teeth
 Check your mouth for signs of problems from diabetes.
Check your mouth for signs of problems from diabetes.
What should I do if I have mouth problems from diabetes?
See your dentist right away if you notice any signs or symptoms of mouth problems. Your dentist is an important ally in keeping your mouth healthy and treating mouth problems before they become serious.
If you have diabetes
- tell your dentist about your diabetes, including how long you’ve had the disease, any diabetes-related problems you may have, and any medicines you take
- keep your dentist updated on any changes to your health, including any increase in your blood glucose levels
- ask how often you should come in for regular cleanings and checkups
- follow your dentist’s advice on how to prevent and treat mouth problems from diabetes
If you feel nervous about visiting the dentist, tell your dentist and the staff about your feelings. Your dentist can adapt the treatment to your needs.
 If you notice any mouth problems, see your dentist right away.
If you notice any mouth problems, see your dentist right away.How can I prepare for dental work?
High blood glucose increases the risk for infections after mouth surgery and can also take your mouth longer to heal. Tell your doctor if you will be having oral surgery or other extensive dental work. To help you prepare for and heal after the procedure, ask your doctor
- how often you should check your blood glucose before and after the procedure
- what, if any, changes you should make to your medicines, such as changing the dose or the time you take a medicine
- how to best treat any soreness after the procedure
How can I keep my mouth healthy?
Keep your mouth healthy (PDF, 242.78 KB) by taking these steps
- Keep your blood glucose numbers within your target range. Your doctor can help set your target and explain what to do if your numbers are too high or too low.
- Consume healthy meals and beverages and follow the meal plan you and your doctor or registered dietitian have worked out.
- Visit your dentist regularly. Ask your dentist how to take care of your teeth at home, including the cleaning tools and products you should use. Your dentist can recommend a cleaning routine tailored to your needs.
Taking good care of your teeth is not always easy. Challenges can include finding a dentist nearby who can help you develop a dental routine that works for you and being able to afford dental care and related products. If you are worried about costs, consider free or low-cost dental care options, such as
- community health centers across the country that provide free or reduced-cost health services, including dental care.
- Medicaid, a state-run program that provides medical benefits to eligible individuals and families. Most states offer limited dental services for adults, while some provide comprehensive services.
Don’t let these concerns stop you from having regular checkups. Waiting too long to take care of your mouth may make things worse.
Smoking raises your risk for many diabetes problems and mouth problems. If you smoke or use other tobacco products, stop. Ask for help so you don’t have to do it alone. You can start by calling the National Quitline at 1-800-QUITNOW or 1-800-784-8669. For tips on quitting, visit Smokefree.gov.
Clinical Trials for Diabetes and Gum Disease
The NIDDK conducts and supports clinical trials in many diseases and conditions, including diabetes. The trials look to find new ways to prevent, detect, or treat disease and improve quality of life.
What are clinical trials for diabetes and gum disease?
Clinical trials—and other types of clinical studies—are part of medical research and involve people like you. When you volunteer to take part in a clinical study, you help doctors and researchers learn more about disease and improve health care for people in the future.
Researchers are studying many aspects of diabetes and gum disease, such as how certain genes may play a role in diabetes, gum disease, heart disease, and bone loss.
Find out if clinical studies are right for you.
Watch a video of NIDDK Director Dr. Griffin P. Rodgers explaining the importance of participating in clinical trials.
What clinical studies for diabetes and gum disease are looking for participants?
You can find clinical studies on diabetes and gum disease at ClinicalTrials.gov. In addition to searching for federally funded studies, you can expand or narrow your search to include clinical studies from industry, universities, and individuals; however, the National Institutes of Health does not review these studies and cannot ensure they are safe. Always talk with your health care provider before you participate in a clinical study.
References
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
The NIDDK would like to thank:
Timothy Iafolla, D.M.D., M.P.H., Chief, Program Analysis and Reporting Branch, Office of Science Policy & Analysis, NIDCR, and Dena Fischer, D.D.S., M.S.D., M.S., Director, NIDCR Center for Clinical Research and Director, Clinical Trials & Practice-based Research Program
