Diabetic Eye Disease
On this page:
- What is diabetic eye disease?
- How does diabetes affect my eyes?
- How common is diabetic eye disease?
- Who is more likely to develop diabetic eye disease?
- What are the symptoms of diabetic eye disease?
- When should I see a doctor right away?
- How do doctors diagnose eye problems from diabetes?
- How do doctors treat diabetic eye disease?
- What can I do to protect my eyes?
- What if I already have some vision loss from diabetes?
What is diabetic eye disease?
Diabetic eye disease is a group of eye problems that can affect people with diabetes. These conditions include diabetic retinopathy, diabetic macular edema, cataracts, and glaucoma.
Over time, diabetes can cause damage to your eyes that can lead to poor vision or even blindness. But you can take steps to prevent diabetic eye disease, or keep it from getting worse, by taking care of your diabetes.
The best ways to manage your diabetes and keep your eyes healthy are to
- manage your blood glucose, blood pressure, and cholesterol, sometimes called the diabetes ABCs
- If you smoke, get help to quit smoking
- have a dilated eye exam once a year
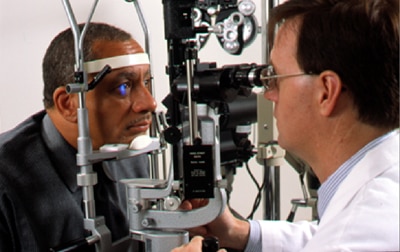
Often, there are no warning signs of diabetic eye disease or vision loss when damage first develops. A full, dilated eye exam helps your doctor find and treat eye problems early—often before much vision loss can occur.
How does diabetes affect my eyes?
Diabetes affects your eyes when your blood glucose, also called blood sugar, is too high.
In the short term, you are not likely to have vision loss from high blood glucose. People sometimes have blurry vision for a few days or weeks when they’re changing their diabetes care plan or medicines. High glucose can change fluid levels or cause swelling in the tissues of your eyes that help you to focus, causing blurred vision. This type of blurry vision is temporary and goes away when your glucose level gets closer to normal.
If your blood glucose stays high over time, it can damage the tiny blood vessels in the back of your eyes. This damage can begin during prediabetes, when blood glucose is higher than normal, but not high enough for you to be diagnosed with diabetes. Damaged blood vessels may leak fluid and cause swelling. New, weak blood vessels may also begin to grow. These blood vessels can bleed into the middle part of the eye, lead to scarring, or cause dangerously high pressure inside your eye.
Most serious diabetic eye diseases begin with blood vessel problems. The four eye diseases that can threaten your sight are
Diabetic retinopathy
The retina is the inner lining at the back of each eye. The retina senses light and turns it into signals that your brain decodes, so you can see the world around you. Damaged blood vessels can harm the retina, causing a disease called diabetic retinopathy.
In early diabetic retinopathy, blood vessels can weaken, bulge, or leak into the retina. This stage is called nonproliferative diabetic retinopathy.
If the disease gets worse, some blood vessels close off, which causes new blood vessels to grow, or proliferate, on the surface of the retina. This stage is called proliferative diabetic retinopathy. These abnormal new blood vessels can lead to serious vision problems.


Diabetic macular edema
The part of your retina that you need for reading, driving, and seeing faces is called the macula. Diabetes can lead to swelling in the macula, which is called diabetic macular edema. Over time, this disease can destroy the sharp vision in this part of the eye, leading to partial vision loss or blindness. Macular edema usually develops in people who already have other signs of diabetic retinopathy.
Glaucoma
Glaucoma is a group of eye diseases that can damage the optic nerve—the bundle of nerves that connects the eye to the brain. Diabetes doubles the chances of having glaucoma, which can lead to vision loss and blindness if not treated early.
Symptoms depend on which type of glaucoma you have. Learn more about glaucoma.

Cataracts
The lenses within our eyes are clear structures that help provide sharp vision—but they tend to become cloudy as we age. People with diabetes are more likely to develop cloudy lenses, called cataracts. People with diabetes can develop cataracts at an earlier age than people without diabetes. Researchers think that high glucose levels cause deposits to build up in the lenses of your eyes.

How common is diabetic eye disease?
Diabetic retinopathy
About one in three people with diabetes who are older than age 40 already have some signs of diabetic retinopathy.1 Diabetic retinopathy is the most common cause of vision loss in people with diabetes. Each person’s outlook for the future, however, depends in large part on regular care. Finding and treating diabetic retinopathy early can reduce the risk of blindness by 95 percent.
Glaucoma and cataracts
Your chances of developing glaucoma or cataracts are about twice that of someone without diabetes.
Who is more likely to develop diabetic eye disease?
Anyone with diabetes can develop diabetic eye disease. Your risk is greater with
- high blood glucose that is not treated
- high blood pressure that is not treated
High blood cholesterol and smoking may also raise your risk for diabetic eye disease.
Some groups are affected more than others. African Americans, American Indians and Alaska Natives, Hispanics/Latinos, Pacific Islanders, and older adults are at greater risk of losing vision or going blind from diabetes.
If you have diabetes and become pregnant, you can develop eye problems very quickly during your pregnancy. If you already have some diabetic retinopathy, it can get worse during pregnancy. Changes that help your body support a growing baby may put stress on the blood vessels in your eyes. Your health care team will suggest regular eye exams during pregnancy to catch and treat problems early and protect your vision.
Diabetes that occurs only during pregnancy, called gestational diabetes, does not usually cause eye problems. Researchers aren't sure why this is the case.
Your chances of developing diabetic eye disease increase the longer you have diabetes.
What are the symptoms of diabetic eye disease?
Often there are no early symptoms of diabetic eye disease. You may have no pain and no change in your vision as damage begins to grow inside your eyes, particularly with diabetic retinopathy.
When symptoms do occur, they may include
- blurry or wavy vision
- frequently changing vision—sometimes from day to day
- dark areas or vision loss
- poor color vision
- spots or dark strings (also called floaters)
- flashes of light
Talk with your eye doctor if you have any of these symptoms.
When should I see a doctor right away?
Call a doctor right away if you notice sudden changes to your vision, including flashes of light or many more spots (floaters) than usual. You also should see a doctor right away if it looks like a curtain is pulled over your eyes. These changes in your sight can be symptoms of a detached retina, which is a medical emergency.
How do doctors diagnose eye problems from diabetes?
Having a full, dilated eye exam is the best way to check for eye problems from diabetes. Your doctor will place drops in your eyes to widen your pupils. This allows the doctor to examine a larger area at the back of each eye, using a special magnifying lens. Your vision will be blurry for a few hours after a dilated exam.
Your doctor will also
- test your vision
- measure the pressure in your eyes
Your doctor may suggest other tests, too, depending on your health history.
Most people with diabetes should see an eye care professional once a year for a complete eye exam. Your own health care team may suggest a different plan, based on your type of diabetes and the time since you were first diagnosed.
How do doctors treat diabetic eye disease?
Your doctor may recommend having eye exams more often than once a year, along with management of your diabetes. This means managing your diabetes ABCs, which include your A1c, blood pressure, and cholesterol; and quitting smoking. Ask your health care team what you can do to reach your goals.

Doctors may treat advanced eye problems with medicine, laser treatments, surgery, or a combination of these options.
Medicine
Your doctor may treat your eyes with anti-VEGF medicine, such as aflibercept, bevacizumab, or ranibizumab. These medicines block the growth of abnormal blood vessels in the eye. Anti-VEGF medicines can also stop fluid leaks, which can help treat diabetic macular edema.
The doctor will inject an anti-VEGF medicine into your eyes during office visits. You'll have several treatments during the first few months, then fewer treatments after you finish the first round of therapy. Your doctor will use medicine to numb your eyes so you don’t feel pain. The needle is about the thickness of a human hair.
Anti-VEGF treatments can stop further vision loss and may improve vision in some people.
Laser Treatment
Laser treatment, also called photocoagulation, creates tiny burns inside the eye with a beam of light. This method treats leaky blood vessels and extra fluid, called edema. Your doctor usually provides this treatment during several office visits, using medicine to numb your eyes. Laser treatment can keep eye disease from getting worse, which is important to prevent vision loss or blindness. But laser treatment is less likely to bring back vision you’ve already lost compared with anti-VEGF medicines.
There are two types of laser treatment:
- Focal/grid laser treatment works on a small area of the retina to treat diabetic macular edema.
- Scatter laser treatment, also called panretinal photocoagulation (PRP), covers a larger area of the retina. This method treats the growth of abnormal blood vessels, called proliferative diabetic retinopathy.
Vitrectomy
Vitrectomy is a surgery to remove the clear gel that fills the center of the eye, called the vitreous gel. The procedure treats problems with severe bleeding or scar tissue caused by proliferative diabetic retinopathy. Scar tissue can force the retina to peel away from the tissue beneath it, like wallpaper peeling away from a wall. A retina that comes completely loose, or detaches, can cause blindness.
During vitrectomy, a clear salt solution is gently pumped into the eye to maintain eye pressure during surgery and to replace the removed vitreous. Vitrectomy is done in a surgery center or hospital with pain medicine.
Cataract Lens Surgery
In a surgery center or hospital visit, your doctor can remove the cloudy lens in your eye, where the cataract has grown, and replace it with an artificial lens. People who have cataract surgery generally have better vision afterward. After your eye heals, you may need a new prescription for your glasses. Your vision following cataract surgery may also depend on treating any damage from diabetic retinopathy or macular edema.
What can I do to protect my eyes?
To prevent diabetic eye disease, or to keep it from getting worse, manage your diabetes ABCs: your A1c, blood pressure, and cholesterol; and quit smoking if you smoke. Read more information on how to manage diabetes.
Also, have a dilated eye exam at least once a year—or more often if recommended by your eye care professional. These actions are powerful ways to protect the health of your eyes—and can prevent blindness.
The sooner you work to manage your diabetes and other health conditions, the better. And, even if you’ve struggled in the past to manage your health, taking better care of yourself now can protect your eyes for the future. It’s never too late to begin.
What if I already have some vision loss from diabetes?
Ask your eye care professional to help you find a low vision and rehabilitation clinic. Special eye care professionals can help you manage vision loss that cannot be corrected with glasses, contact lenses, medicine, or surgery. Special devices and training may help you make the most of your remaining vision so that you can continue to be active, enjoy hobbies, visit friends and family members, and live without help from others.
References
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
The NIDDK would like to thank:
Neil M. Bressler, MD, The Wilmer Eye Institute, Johns Hopkins University School of Medicine; Emily Chew, MD, National Eye Institute (NEI)
