Acid Reflux (GER & GERD) in Adults
Return to Overview PageDefinition & Facts
In this section:
- What is GER?
- Does GER have another name?
- How common is GER?
- What is GERD?
- How common is GERD?
- Who is more likely to have GERD?
- What are the complications of GERD?
What is GER?
Gastroesophageal reflux (GER) happens when your stomach contents come back up into your esophagus. Many people have GER once in a while, and GER often happens without causing symptoms. In some cases, GER may cause heartburn, also called acid indigestion.
 Gastroesophageal reflux (GER) may cause heartburn.
Gastroesophageal reflux (GER) may cause heartburn.Does GER have another name?
Doctors also refer to GER as
- acid indigestion
- acid reflux
- acid regurgitation
- heartburn
- reflux
How common is GER?
Having GER once in a while is common.
What is GERD?
Gastroesophageal reflux disease (GERD) is a more severe and long-lasting condition in which GER causes repeated symptoms that are bothersome or leads to complications over time.
If you think you may have GERD, you should see your doctor.
How common is GERD?
Researchers estimate that about 20 percent of people in the United States have GERD.1
Who is more likely to have GERD?
Anyone can develop GERD. You are more likely to have GERD if you
- are overweight or have obesity
- are a pregnant woman
- take certain medicines
- smoke or are regularly exposed to secondhand smoke
What are the complications of GERD?
Without treatment, GERD can sometimes cause serious complications over time, such as esophagitis, esophageal stricture, and Barrett’s esophagus, as well as complications outside the esophagus.
Esophagitis
Esophagitis is inflammation in the esophagus. Esophagitis may cause ulcers and bleeding in the lining of the esophagus. Chronic esophagitis increases the chance of developing esophageal stricture and Barrett’s esophagus.
Esophageal stricture
An esophageal stricture happens when your esophagus becomes too narrow. Esophageal strictures can lead to problems with swallowing.
Barrett’s esophagus
GERD can sometimes lead to Barrett’s esophagus, a condition in which tissue that is similar to the lining of your intestine replaces the tissue lining your esophagus. A small number of people with Barrett’s esophagus develop a type of cancer called esophageal adenocarcinoma.
Complications outside the esophagus
Some people with GERD develop complications outside the esophagus, in the mouth, throat, or lungs. These complications may include
- asthma
- chronic cough
- hoarseness
- laryngitis—inflammation of your voice box that can cause you to lose your voice for a short time
- wearing away of tooth enamel
References
Symptoms & Causes
What are the symptoms of GER and GERD?
Gastroesophageal reflux (GER) and gastroesophageal reflux disease (GERD) commonly cause symptoms such as
- heartburn, a painful, burning feeling in the middle of your chest, behind your breastbone, rising from the lower tip of your breastbone toward your throat
- regurgitation, or stomach contents coming back up through your esophagus and into your throat or mouth, which may cause you to taste food or stomach acid
However, not all adults with GERD have heartburn or regurgitation. Other symptoms may include
- chest pain
- nausea
- problems swallowing or pain while swallowing
- symptoms of complications in the mouth, throat, or lungs, such as chronic cough or hoarseness
 Symptoms of GERD may include chronic cough.
Symptoms of GERD may include chronic cough.
You should see a doctor if you think you have GERD, or if your symptoms don’t get better with over-the-counter medicines or lifestyle changes.
You should also see a doctor if you have symptoms that could be related to GERD complications or other serious health problems, such as
- chest pain
- loss of appetite
- persistent vomiting
- problems swallowing or pain while swallowing
- signs of bleeding in the digestive tract, such as
- vomit that contains blood or looks like coffee grounds
- stool that contains blood or looks black and tarry
- unexplained weight loss
What causes GER and GERD?
Your lower esophageal sphincter and diaphragm most often prevent GER, which is when stomach contents come back up into your esophagus. However, many people have GER once in a while.
GERD may develop if your lower esophageal sphincter becomes weak or relaxes when it shouldn’t. Factors that may affect the lower esophageal sphincter and lead to GERD include
- being overweight or having obesity
- being pregnant
- smoking or inhaling secondhand smoke
Some medicines can cause GERD or make GERD symptoms worse. Examples include
- benzodiazepines, sedatives that make you calmer or sleepy
- calcium channel blockers, which are used to treat high blood pressure
- certain asthma medicines
- nonsteroidal anti-inflammatory drugs (NSAIDs)
- tricyclic antidepressants
A hiatal hernia can also increase the chance of getting GERD or make GERD symptoms worse. A hiatal hernia is a condition in which the opening in your diaphragm lets the upper part of the stomach move up into your chest.
Diagnosis
How do doctors diagnose GER & GERD?
In most cases, doctors diagnose gastroesophageal reflux (GER) and gastroesophageal reflux disease (GERD) by reviewing your symptoms and medical history. If your symptoms suggest you have GERD, your doctor may recommend treatment with medicines and lifestyle changes, instead of doing tests.
Your doctor may recommend medical tests if
- your symptoms suggest you might have a complication of GERD
- your symptoms suggest that you might have another health problem that causes symptoms similar to those of GERD
- your symptoms don’t improve after treatment with medicines and lifestyle changes
Your doctor may refer you to a gastroenterologist to diagnose and treat GERD.
What tests do doctors use to diagnose GERD?
Your doctor may order one or more of the following tests to help diagnose GERD and check for GERD complications or other health problems.
Upper gastrointestinal (GI) endoscopy
Upper GI endoscopy is a procedure in which a doctor uses an endoscope—a flexible tube with a camera—to see the lining of your upper GI tract, including your esophagus, stomach, and duodenum. During upper GI endoscopy, a doctor may obtain biopsies by passing an instrument through the endoscope to take small pieces of tissue from the lining of your esophagus. A pathologist will examine the tissue under a microscope. Doctors may order an upper GI endoscopy to check for complications of GERD or problems other than GERD that may be causing your symptoms.
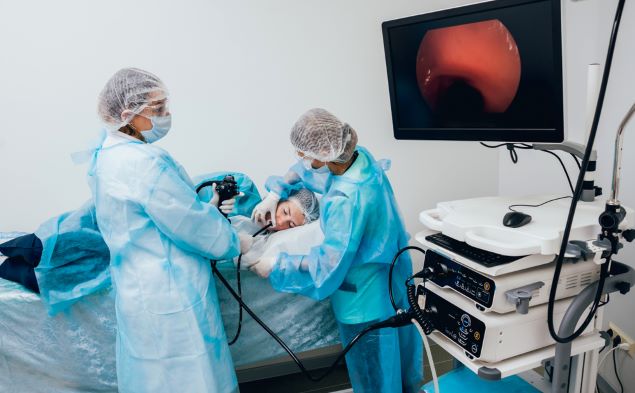 Your doctor may order an upper GI endoscopy to help diagnose GERD.
Your doctor may order an upper GI endoscopy to help diagnose GERD.
Esophageal pH monitoring
Esophageal pH monitoring is the most accurate way to detect stomach acid in the esophagus. Two types of esophageal pH monitoring are
- catheter monitoring, in which a health care professional passes one end of a catheter—a thin, flexible tube—through your nose and into your esophagus to measure acid and nonacid reflux
- capsule monitoring, in which a health care professional uses an endoscope to place a small, wireless capsule on the lining of your esophagus to measure acid reflux
During esophageal pH monitoring, you’ll wear a monitor that receives information from the catheter or capsule and tracks information about your diet, sleep, and symptoms. Your doctor will use this information to see how your diet, sleep, and symptoms relate to acid reflux in your esophagus. Doctors may order this test to confirm the diagnosis of GERD or to find out if GERD treatments are working.
Treatment
How do doctors treat GER and GERD?
Your doctor may recommend that you make lifestyle changes and take medicines to manage symptoms of gastroesophageal reflux (GER) or gastroesophageal reflux disease (GERD). In some cases, doctors may also recommend surgery.
Lifestyle changes
Lifestyle changes may reduce your symptoms. Your doctor may recommend
- losing weight if you’re overweight or have obesity
- elevating your head during sleep by placing a foam wedge or extra pillows under your head and upper back to incline your body and raise your head off your bed 6 to 8 inches
- quitting smoking, if you smoke
- changing your eating habits and diet
Over-the-counter and prescription medicines
You can buy many GERD medicines over the counter. However, if you have symptoms that will not go away with over-the-counter medicines, you should talk with your doctor. Your doctor may prescribe one or more medicines to treat GERD.
Antacids. Doctors may recommend antacids to relieve mild heartburn and other mild GER and GERD symptoms. Antacids are available over the counter. Antacids can help relieve mild symptoms. However, you shouldn’t use these medicines every day or for severe symptoms, except after discussing your antacid use with your doctor. These medicines can have side effects, such as diarrhea or constipation.
H2 blockers. H2 blockers lower the amount of acid your stomach makes. H2 blockers can help heal the esophagus, but not as well as proton pump inhibitors (PPIs) can. You can buy H2 blockers over the counter, or your doctor can prescribe one.
Proton pump inhibitors (PPIs). PPIs lower the amount of acid your stomach makes. PPIs are better at treating GERD symptoms than H2 blockers, and they can heal the esophageal lining in most people with GERD. You can buy PPIs over the counter, or your doctor can prescribe one. Doctors may prescribe PPIs for long-term GERD treatment.
PPIs are generally safe and effective. Side effects are uncommon and may include headache, diarrhea, and upset stomach. Research also suggests that taking PPIs may increase the chance of Clostridioides difficile (C. diff) infection. Experts are still studying the effects of taking PPIs for a long time or in high doses. Talk with your doctor about the risks and benefits of taking PPIs.
 Your doctor may prescribe one or more medicines to treat GERD.
Your doctor may prescribe one or more medicines to treat GERD.Other medicines. If antacids, H2 blockers, and PPIs don’t improve your symptoms, your doctor may recommend other medicines.
Surgery and other medical procedures
Your doctor may recommend surgery if your GERD symptoms don’t improve with lifestyle changes and medicines, or if you wish to stop taking long-term GERD medicines to manage symptoms. You’re more likely to develop complications from surgery than from medicines.
Fundoplication. Fundoplication is the most common surgery for GERD. In most cases, it leads to long-term improvement of GERD symptoms. During the operation, a surgeon sews the top of your stomach around the end of your esophagus to add pressure to the lower esophageal sphincter and help prevent reflux.
Surgeons may perform fundoplication as laparoscopic or open surgery. In laparoscopic fundoplication, which is more common, surgeons make small cuts in the abdomen and insert special tools to perform the operation. Laparoscopic fundoplication leaves several small scars. In open fundoplication, surgeons make a larger cut in the abdomen.
Weight-loss surgery, also called metabolic and bariatric surgery. If you have GERD and obesity, your doctor may recommend weight-loss surgery, most often gastric bypass surgery. Weight-loss surgery can help you lose weight and reduce GERD symptoms.
Endoscopy. In a small number of cases, doctors may recommend procedures that use endoscopy to treat GERD. For endoscopy, doctors insert an endoscope—a small, flexible tube with a light and camera—through your mouth and into your esophagus. Doctors may use endoscopic procedures to sew the top of your stomach around the lower esophageal sphincter or to deliver radiofrequency energy to the sphincter. Doctors don’t use these procedures often.
Eating, Diet, & Nutrition
How can changes in my eating habits improve GERD symptoms?
If you have gastroesophageal reflux disease (GERD) and you are overweight or have obesity, your doctor may suggest losing weight to reduce your GERD symptoms. Your doctor can recommend a healthy eating plan to help you lose weight.
If you have GERD symptoms at night or when you’re lying down, eating meals at least 3 hours before you lie down or go to bed may improve symptoms.2
What should I avoid eating if I have GERD symptoms?
Some people who have GERD find that certain foods or drinks trigger symptoms or make symptoms worse. Foods and drinks that have been commonly linked to GERD symptoms include
- acidic foods, such as citrus fruits and tomatoes
- alcoholic drinks
- chocolate
- coffee and other sources of caffeine
- high-fat foods
- mint
- spicy foods
Talk with your doctor about your diet and foods or drinks that seem to increase your symptoms. Your doctor may recommend reducing or avoiding certain foods or drinks to see if GERD symptoms improve.
 If you are overweight or have obesity, your doctor may suggest losing weight to reduce your GERD symptoms.
If you are overweight or have obesity, your doctor may suggest losing weight to reduce your GERD symptoms.References
Clinical Trials
The NIDDK conducts and supports clinical trials in many diseases and conditions, including digestive diseases. The trials look to find new ways to prevent, detect, or treat disease and improve quality of life.
What are clinical trials for GER & GERD?
Clinical trials—and other types of clinical studies—are part of medical research and involve people like you. When you volunteer to take part in a clinical study, you help doctors and researchers learn more about disease and improve health care for people in the future.
Researchers are studying many aspects of gastroesophageal reflux disease (GERD), such as
- how diet affects symptoms
- new ways to diagnose the disease
- new treatments for GERD
- risk factors for GERD complications, such as Barrett’s esophagus and esophageal cancer
Find out if clinical studies are right for you.
Watch a video of NIDDK Director Dr. Griffin P. Rodgers explaining the importance of participating in clinical trials.
What clinical studies for GER & GERD are looking for participants?
You can view a filtered list of clinical studies on GERD that are federally funded, open, and recruiting at ClinicalTrials.gov. You can expand or narrow the list to include clinical studies from industry, universities, and individuals; however, the NIH does not review these studies and cannot ensure they are safe. Always talk with your health care provider before you participate in a clinical study.
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
The NIDDK would like to thank:
Nicholas J. Shaheen, M.D., M.P.H., University of North Carolina School of Medicine
