Celiac Disease
Return to Overview PageDefinition & Facts
On this page:
- What is celiac disease?
- Does celiac disease have other names?
- How common is celiac disease?
- Who is more likely to develop celiac disease?
- What other health problems do people with celiac disease have?
- What are the complications of celiac disease?
What is celiac disease?
Celiac disease is a chronic digestive and immune disorder that damages the small intestine. The disease is triggered by eating foods containing gluten. Gluten is a protein found naturally in wheat, barley, and rye, and is common in foods such as bread, pasta, cookies, and cakes. Many products contain gluten, such as prepackaged foods, lip balms and lipsticks, toothpastes, vitamin and nutrient supplements, and, rarely, medicines.
 Celiac disease is triggered by eating foods containing gluten, like wheat.
Celiac disease is triggered by eating foods containing gluten, like wheat.Celiac disease can be serious. The disease can cause long-lasting digestive problems and keep your body from getting all the nutrients it needs. Celiac disease can also affect the body outside the small intestine.
Celiac disease is different from gluten sensitivity or wheat intolerance. If you have gluten sensitivity, you may have symptoms like those of celiac disease, such as abdominal pain and tiredness. Unlike celiac disease, gluten sensitivity does not damage the small intestine.
Celiac disease is also different from a wheat allergy, a type of food allergy. In both cases, your body’s immune system reacts to wheat. However, some symptoms of wheat allergies, such as having itchy eyes or a hard time breathing, are different from celiac disease. Wheat allergies also do not cause long-term damage to the small intestine.
Does celiac disease have other names?
Celiac disease is also called celiac sprue, nontropical sprue, and gluten-sensitive enteropathy.
How common is celiac disease?
Many people who have celiac disease have not been diagnosed. However, experts estimate about 2 million people in the United States have celiac disease and about 1 percent of people around the world have celiac disease.1,2
Who is more likely to develop celiac disease?
Celiac disease can only occur in people who have certain genes. You are more likely to develop celiac disease if someone in your family has the disease.
Celiac disease affects children and adults in all parts of the world. In the United States, celiac disease is more common among white Americans than among other racial or ethnic groups. A celiac disease diagnosis is more common in females than in males.1
Celiac disease is also more common in people who have certain chromosomal disorders, such as Down syndrome, Turner syndrome, and Williams syndrome.
What other health problems do people with celiac disease have?
Experts have found that some people have both celiac disease and other disorders related to the immune system. These disorders include
- type 1 diabetes
- thyroid diseases, such as Hashimoto’s disease, Graves’ disease, Addison’s disease, and primary hyperparathyroidism
- selective immunoglobulin A (IgA) deficiency, a condition in which your body makes little or no IgA, an antibody that fights infections
- rheumatic diseases, such as Sjögren’s syndrome
- liver diseases, such as autoimmune hepatitis, primary sclerosing cholangitis, and primary biliary cholangitis
What are the complications of celiac disease?
Long-term complications of celiac disease include
- accelerated osteoporosis or bone softening, known as osteomalacia
- anemia
- malnutrition, a condition in which you don’t get enough vitamins, minerals, and other nutrients you need to be healthy
- nervous system problems
- problems related to the reproductive system
Rare complications can include
- adenocarcinoma, a type of cancer of the small intestine
- liver damage, which may lead to cirrhosis or liver failure
- non-Hodgkin lymphoma
In rare cases, you may continue to have trouble absorbing nutrients even though you have been following a strict gluten-free diet. If you have this condition, called refractory celiac disease, your small intestine is severely damaged and can’t heal. You may need to receive intravenous (IV) nutrients and specialized treatment.
References
Symptoms & Causes
What are the symptoms of celiac disease?
Symptoms of celiac disease vary widely, and a person may have multiple symptoms that come and go. If you have celiac disease, you may have digestive problems or other symptoms. Digestive symptoms are more common in children than in adults. Digestive symptoms of celiac disease may include
- bloating
- chronic diarrhea
- constipation
- gas
- lactose intolerance due to damage to the small intestine
- loose, greasy, bulky, and bad-smelling stools
- nausea or vomiting
- pain in the abdomen
For children with celiac disease, being unable to absorb nutrients at a time when they are so important to normal growth and development can lead to
- damage to the permanent teeth’s enamel
- delayed puberty
- failure to thrive, meaning that an infant or a child weighs less or is gaining less weight than expected for his or her age
- mood changes or feeling annoyed or impatient
- slowed growth and short height
- weight loss
Some people with celiac disease have symptoms that affect other parts of the body. These symptoms may include
- dermatitis herpetiformis
- fatigue, or feeling tired
- joint or bone pain
- mental health problems, such as depression or anxiety
- nervous system symptoms, such as headaches, balance problems, seizures, or peripheral neuropathy
- reproductive problems in women and girls—which may include infertility, delayed start of menstrual periods, missed menstrual periods, or repeated miscarriages—and male infertility
- symptoms involving the mouth, such as canker sores; a dry mouth; or a red, smooth, shiny tongue
Most people with celiac disease have one or more symptoms before they are diagnosed and begin treatment. Symptoms typically improve and may go away after a person begins eating a gluten-free diet. Symptoms may return if a person consumes small amounts of gluten.
Depending on how old you are when a doctor diagnoses your celiac disease, some symptoms, such as short height and tooth defects, may not improve. People with celiac disease who have no symptoms can still develop complications over time if they do not get treatment.
Dermatitis herpetiformis
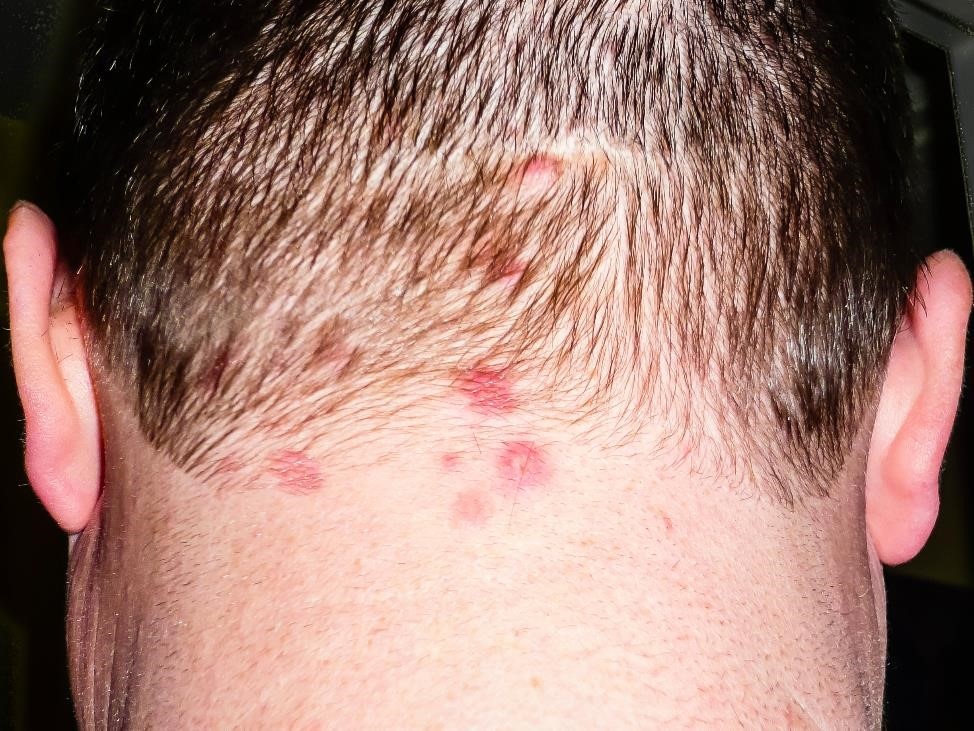 Dermatitis herpetiformis
Dermatitis herpetiformis
Dermatitis herpetiformis is an itchy, blistering skin rash that usually appears on the elbows, knees, buttocks, back, or scalp. Among people with untreated celiac disease, about 2 to 3 percent of children and 10 to 20 percent of adults have dermatitis herpetiformis.3 Some people with celiac disease may have the rash and no other symptoms. After a person starts a gluten-free diet, the rash may take some time to heal and may return if a person consumes small amounts of gluten.
What causes celiac disease?
Research suggests that celiac disease only occurs in people who have certain genes and eat food that contains gluten. Experts are studying other factors that may play a role in causing the disease.
Genes
Celiac disease almost always occurs in people who have one of two groups of normal gene variants, called DQ2 and DQ8. People who do not have these gene variants are very unlikely to develop celiac disease. About 30 percent of people have DQ2 or DQ8. However, only about 3 percent of people with DQ2 or DQ8 develop celiac disease.4
Researchers are studying other genes that may increase the chance of developing celiac disease in people who have DQ2 or DQ8.
Gluten
Consuming gluten triggers the abnormal immune system response that causes celiac disease. However, not all people who have the gene variants DQ2 or DQ8 and eat gluten develop the disease. Research suggests that among children with a genetic predisposition for celiac disease, those who eat more gluten in early childhood may have a greater risk for celiac disease.5
Other factors
Researchers are studying other factors that may increase a person’s chances of developing celiac disease. For example, research suggest that a higher number of infections in early life and certain digestive tract infections may increase the risk. Experts also think changes in the microbiome—the bacteria in the digestive tract that help with digestion—could play a role in the development of celiac disease.
References
Diagnosis
How do doctors diagnose celiac disease?
Doctors use information from your medical and family history, a physical exam, a dental exam, and medical test results to look for signs that you might have celiac disease and should be tested. Doctors typically diagnose celiac disease with blood tests and biopsies of the small intestine.
Medical and family history
Your doctor will ask about your symptoms. Celiac disease isn’t diagnosed based on symptoms alone because some of the symptoms are like the symptoms of other digestive disorders, such as irritable bowel syndrome (IBS) or lactose intolerance. Some people with celiac disease have symptoms that affect parts of the body outside the digestive tract.
The doctor will review your medical history, including your history of conditions that are more common in people who have celiac disease. Your doctor will also ask about your family’s medical history and whether anyone in your family has been diagnosed with celiac disease.
 Your doctor will ask about your symptoms, medical history, and family medical history.
Your doctor will ask about your symptoms, medical history, and family medical history.Physical exam
During a physical exam, a doctor may
- check for signs of weight loss or growth problems
- examine your skin for rashes, such as dermatitis herpetiformis
- listen to sounds in the abdomen using a stethoscope
- tap on the abdomen to check for pain or swelling
In some cases, a dentist may notice signs of celiac disease during an exam. Celiac disease may cause problems with the teeth and mouth, such as defects in tooth enamel or canker sores.
What tests do doctors use to diagnose celiac disease?
Doctors most often use blood tests and biopsies of the small intestine to diagnose or rule out celiac disease. Doctors don’t recommend starting a gluten-free diet before diagnostic testing because a gluten-free diet can affect test results.
In some cases, doctors may order additional tests, such as skin biopsies and genetic tests, to help diagnose or rule out celiac disease.
Blood tests
A health care professional will take a blood sample from you and send the sample to a lab. Blood tests can show levels of certain antibodies that are often higher than normal in people who have untreated celiac disease. Blood tests may also show signs of health problems that could be related to celiac disease, such as anemia.
Biopsies of the small intestine
A doctor obtains biopsies of the small intestine during an upper GI endoscopy. For an upper GI endoscopy, a doctor uses an endoscope—a flexible tube with a camera—to see the lining of your upper GI tract, including the first part of your small intestine. The doctor passes an instrument through the endoscope to take small pieces of tissue from your small intestine. A pathologist will examine the tissue under a microscope to look for signs of celiac disease.
Skin biopsies
A doctor may order skin biopsies if you have a rash that could be dermatitis herpetiformis. For skin biopsies, a doctor removes small pieces of skin tissue on and next to the rash. A pathologist will examine the tissue under a microscope to look for signs of dermatitis herpetiformis.
Genetic testing
In some cases, a health care professional may take a blood sample or use a swab to collect cells from the inside of your cheek. The sample will be tested for groups of gene variants called DQ2 and DQ8. If you do not have these gene variants, you are very unlikely to have celiac disease.
Having DQ2 or DQ8 alone does not mean you have celiac disease. Most people with these gene variants do not develop celiac disease. If you do have DQ2 or DQ8, your doctor may recommend additional tests to check for or rule out celiac disease.
Do doctors screen for celiac disease?
Screening is testing for diseases when you have no symptoms. Doctors in the United States do not routinely screen people for celiac disease. However, blood relatives of people with celiac disease and those with type 1 diabetes should talk with their doctor about their chances of getting the disease to see if they should be tested.
Treatment
How do doctors treat celiac disease?
Gluten-free diet
Doctors treat celiac disease by helping people to follow a gluten-free diet. Gluten is a protein found naturally in certain grains, including wheat, barley, and rye. Gluten is also added to many other foods and products. In people who have celiac disease, consuming gluten triggers an abnormal immune system reaction that damages the small intestine.
 A registered dietitian will teach you how to avoid gluten while following a healthy diet.
A registered dietitian will teach you how to avoid gluten while following a healthy diet.Symptoms greatly improve for most people with celiac disease who stick to a gluten-free diet. For most people, following a gluten-free diet will heal damage in the small intestine and prevent more damage. Many people see symptoms improve within days to weeks of starting the diet.6
Your doctor will explain the gluten-free diet and may refer you to a registered dietitian who specializes in treating people who have celiac disease. The dietitian will teach you how to avoid gluten while following a healthy diet and recommend substitutes for foods that contain gluten. He or she will help you
- check food and product labels for gluten
- design everyday meal plans
- make healthy choices about foods and drinks
Avoiding medicines and other products that may contain gluten
In addition to prescribing a gluten-free diet, your doctor will want you to avoid all hidden sources of gluten. If you have celiac disease, ask a pharmacist about ingredients in
- herbal and nutritional supplements
- prescription and over-the-counter medicines
- vitamin and mineral supplements
Medicines are rare sources of gluten. Even if gluten is present in a medicine, it is likely to be in such small quantities that it would not cause any symptoms.
Other products can be hidden sources of gluten. You may take in small amounts of gluten if you consume these products, use them around your mouth, or transfer them from your hands to your mouth by accident. Products that may contain gluten include
- children’s modeling dough, such as Play-Doh
- cosmetics
- lipstick, lip gloss, and lip balm
- skin and hair products
- toothpaste and mouthwash
- communion wafers
Reading product labels can sometimes help you avoid gluten. Some companies label their products as being gluten-free. In the United States, products labelled gluten-free must have less than 20 parts per million of gluten, which should not be a problem for the vast majority of people. If a label doesn’t tell you what is in a product, ask the company that makes the product for an ingredients list. You cannot assume that the product is gluten-free.
Treatments for symptoms or complications
A gluten-free diet will treat or prevent many of the symptoms and complications of celiac disease. Some symptoms may take longer to get better than others, and some symptoms may need additional help.
Dermatitis herpetiformis may not go away until a person has been following a gluten-free diet for 6 months to 2 years.7 In some cases, doctors may prescribe a medicine, such as dapsone, to help treat dermatitis herpetiformis until the rash is under control with a gluten-free diet alone.
In untreated celiac disease, damage to the small intestine can lead to malabsorption and malnutrition. When you are diagnosed with celiac disease, your doctor may test you for low levels of certain vitamins and minerals and may recommend or prescribe supplements if you need them. For safety reasons, talk with your doctor before using dietary supplements, such as vitamins, or any complementary or alternative medicines or medical practices.
When you are diagnosed with celiac disease, your doctor may recommend additional testing if you are at risk for certain complications. For example, doctors may order a bone mineral density test to check for osteoporosis.
Follow-up
Your doctor may recommend regular follow-up visits to make sure symptoms and health problems related to celiac disease are improving on a gluten-free diet. Follow-up may include blood tests to check levels of certain antibodies, which are higher in untreated celiac disease but typically return to normal after treatment. In some cases, doctors may recommend additional biopsies to find out if the small intestine has healed.
What if a gluten-free diet isn't working?
If you continue to have celiac disease symptoms while you are following a gluten-free diet, talk with your doctor or a registered dietitian, who can help you find the cause. In about 20 percent of people with celiac disease, symptoms continue or come back even while they are following a gluten-free diet.7 Symptoms may be caused by consuming small amounts of gluten, other health problems, or refractory celiac disease.
Consuming small amounts of gluten
If your symptoms continue or come back after you start a gluten-free diet, you may still be eating or drinking a small amount of gluten. Keep a food journal and talk with your doctor and a registered dietitian about your diet and products you use that might contain gluten. Finding and avoiding all sources of gluten may help your symptoms improve. Hidden sources of gluten include additives made with wheat, such as
- modified food starch
- malt flavoring
- preservatives
- stabilizer
Other health problems
Your doctor may order tests to confirm the diagnosis of celiac disease and check for other health problems. Health problems that cause symptoms similar to those of celiac disease and may occur along with celiac disease include irritable bowel syndrome, lactose intolerance, microscopic colitis, problems with the pancreas, or small intestinal bacterial overgrowth.
Refractory celiac disease
Refractory celiac disease is a rare condition in which symptoms and damage to the small intestine continue or come back, even while a person is following a strict gluten-free diet. Refractory celiac disease may lead to complications, such as malnutrition or a type of cancer called enteropathy-associated T-cell lymphoma.
Doctors may recommend additional testing and treatments to diagnose and manage refractory celiac disease.
References
Eating, Diet, & Nutrition
On this page:
- How will I need to change my diet if I have celiac disease?
- What foods and drinks contain gluten?
- How can I identify and avoid foods and drinks that contain gluten?
- What should I eat if I have celiac disease?
- Should I start a gluten-free diet before I talk with my doctor?
How will I need to change my diet if I have celiac disease?
If you have celiac disease, you will need to remove foods and drinks that contain gluten from your diet. Following a gluten-free diet can relieve celiac disease symptoms and heal damage to the small intestine. People with celiac disease need to follow a gluten-free diet for life to prevent symptoms and intestinal damage from coming back. Your doctor or a registered dietitian can guide you on what to eat and drink to maintain a balanced diet.
If you or your child has been diagnosed with celiac disease, you may find support groups helpful as you learn about and adjust to a gluten-free lifestyle. Your doctor or a registered dietitian may be able to recommend support groups and other reliable sources of information.
What foods and drinks contain gluten?
Gluten occurs naturally in certain grains, including
- wheat and types of wheat, such as durum, emmer, semolina, and spelt
- barley, which may be found in malt, malt extract, malt vinegar, and brewer’s yeast
- rye
- triticale, a cross between wheat and rye
Gluten is found in foods that contain ingredients made from these grains, including baked goods, baking mixes, breads, cereals, and pastas. Drinks such as beer, lagers, ale, flavored liquors, and malt beverages may also contain gluten.
Many food ingredients and additives—such as colorings, flavorings, starches, and thickeners—are made from grains that contain gluten. These ingredients are added to many processed foods, including foods that are boxed, canned, frozen, packaged, or prepared. Therefore, gluten may be found in a variety of foods, including candy, condiments, hot dogs and sausages, ice cream, salad dressing, and soups.
Cross-contact
Cross-contact occurs when foods or products that contain gluten come into contact with gluten-free foods. Cross-contact can spread gluten to gluten-free foods, making the gluten-free foods unsafe for people with celiac disease to consume. Cross-contact can occur at any time, including when foods are grown, processed, stored, prepared, or served.
How can I identify and avoid foods and drinks that contain gluten?
A registered dietitian can help you learn to identify and avoid foods and drinks that contain gluten when you shop, prepare foods at home, or eat out.
For example, when you shop and eat at home
- carefully read food labels to check for grains that contain gluten—such as wheat, barley, and rye—and ingredients or additives made from those grains.
- check for gluten-free food labeling.
- don't eat foods if you aren’t sure whether they contain gluten. If possible, contact the company that makes the food or visit the company’s website for more information.
- store and prepare your gluten-free foods separately from other family members’ foods that contain gluten to prevent cross-contact.
When you eat out at restaurants or social gatherings
- before you go out to eat, search online for restaurants that offer a gluten-free menu.
- review restaurant menus online or call ahead to make sure a restaurant can accommodate you safely.
- at the restaurant, let the server know that you have celiac disease. Ask about food ingredients, how food is prepared, and whether a gluten-free menu is available. Ask to talk with the chef if you would like more details about the menu.
- when attending social gatherings, let the host know you have celiac disease and find out if gluten-free foods will be available. If not, or if you are unsure, bring gluten-free foods that are safe for you to eat.
What should I eat if I have celiac disease?
If you have celiac disease, you will need to follow a gluten-free diet. Your doctor and a registered dietitian can help you plan a healthy, balanced diet to make sure that you get the nutrients you need.
Gluten-free foods
Many foods, such as meat, fish, fruits, vegetables, rice, and potatoes, without additives or some seasonings, are naturally gluten-free. Flour made from gluten-free foods, such as potatoes, rice, corn, soy, nuts, cassava, amaranth, quinoa, buckwheat, or beans are safe to eat.
You can also buy packaged gluten-free foods, such as gluten-free types of baked goods, bread, and pasta. These foods are available from many grocery stores, restaurants, and at specialty food companies. Packaged gluten-free foods tend to cost more than the same foods that have gluten, and restaurants may charge more for gluten-free types of foods.
Talk with your doctor or a registered dietitian about whether you should include oats in your diet and how much. Research suggests that most people with celiac disease can safely eat moderate amounts of oats. If you do eat oats, make sure they are gluten-free. Cross-contact between oats and grains that contain gluten is common and can make oats unsafe for people with celiac disease.
 Many foods are naturally gluten-free.
Many foods are naturally gluten-free.
Gluten-free labeling
The U.S. Food and Drug Administration (FDA) requires that foods labeled “gluten-free” meet specific standards. One requirement is that foods with the terms “gluten-free,” “no gluten,” “free of gluten,” or “without gluten” on the label must contain less than 20 parts per million of gluten. This amount of gluten is too small to cause problems in most people with celiac disease.
The FDA rule does not apply to foods regulated by the U.S. Department of Agriculture, including meat, poultry, and some egg products. The rule also does not apply to most alcoholic beverages, which are regulated by the U.S. Department of the Treasury.
Should I start a gluten-free diet before I talk with my doctor?
No. If you think you might have celiac disease, you should talk with your doctor about testing to diagnose celiac disease before you begin a gluten-free diet. If you avoid gluten before you have testing, the test results may not be accurate.
Also, if you start avoiding gluten without advice from a doctor or a registered dietitian, your diet may not provide enough of the nutrients you need, such as fiber, iron, and calcium. Some packaged gluten-free foods may be higher in fat and sugar than the same foods that contain gluten. If you are diagnosed with celiac disease, your doctor and dietitian can help you plan a healthy gluten-free diet.
If you don’t have celiac disease or another health problem related to gluten, your doctor may not recommend a gluten-free diet. In recent years, more people without celiac disease have begun avoiding gluten, believing that a gluten-free diet is healthier or could help them lose weight. However, researchers have found no evidence that a gluten-free diet promotes better health or weight loss for the general population.8
Reference
Clinical Trials
The NIDDK conducts and supports clinical trials in many diseases and conditions, including digestive diseases. The trials look to find new ways to prevent, detect, or treat disease and improve quality of life.
What are clinical trials for celiac disease?
Clinical trials—and other types of clinical studies—are part of medical research and involve people like you. When you volunteer to take part in a clinical study, you help doctors and researchers learn more about disease and improve health care for people in the future.
Researchers are studying many aspects of celiac disease, including possible new treatments for the condition.
Find out if clinical studies are right for you.
What clinical studies for celiac disease are looking for participants?
You can view a filtered list of clinical studies on celiac disease that are federally funded, open, and recruiting at ClinicalTrials.gov. You can expand or narrow the list to include clinical studies from industry, universities, and individuals; however, the NIH does not review these studies and cannot ensure they are safe. Always talk with your health care provider before you participate in a clinical study.
Watch a video of NIDDK Director Dr. Griffin P. Rodgers explaining the importance of participating in clinical trials.
What have we learned about celiac disease from NIDDK-funded research?
The NIDDK has supported many studies to learn more about celiac disease.
- The Environmental Determinants of Diabetes in the Young (TEDDY) study is examining factors that affect the development of type 1 diabetes and celiac disease in children who have genetic risk factors for these conditions.
- An NIDDK-supported study found that, in the United States, people living north of 35 degrees north latitude—sometimes called the 35th parallel north—were more likely to have celiac disease than people living south of 35 degrees north latitude.
- NIDDK-supported researchers found that reovirus infection may trigger celiac disease in people who have genetic risk factors for the disease.
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
The NIDDK would like to thank:
Joseph A. Murray, M.D., Mayo Clinic
