Gastroparesis
Return to Overview PageDefinition & Facts
In this section:
- What is gastroparesis?
- How common is gastroparesis?
- Who is more likely to get gastroparesis?
- What other health problems do people with gastroparesis have?
- What are the complications of gastroparesis?
What is gastroparesis?
Gastroparesis, also called delayed gastric emptying, is a disorder that slows or stops the movement of food from your stomach to your small intestine. Normally, after you swallow food, the muscles in the wall of your stomach grind the food into smaller pieces and push them into your small intestine to continue digestion. When you have gastroparesis, your stomach muscles work poorly or not at all, and your stomach takes too long to empty its contents. Gastroparesis can delay digestion, which can lead to various symptoms and complications.
How common is gastroparesis?
Gastroparesis is not common. Out of 100,000 people, about 10 men and about 40 women have gastroparesis1. However, symptoms that are similar to those of gastroparesis occur in about 1 out of 4 adults in the United States2, 3.
Who is more likely to get gastroparesis?
You are more likely to get gastroparesis if you
- have diabetes
- had surgery on your esophagus, stomach, or small intestine, which may injure the vagus nerve. The vagus nerve controls the muscles of the stomach and small intestine.
- had certain cancer treatments, such as radiation therapy on your chest or stomach area
What other health problems do people with gastroparesis have?
People with gastroparesis may have other health problems, such as
- diabetes
- scleroderma
- hypothyroidism
- nervous system disorders, such as migraine, Parkinson’s disease, and multiple sclerosis
- gastroesophageal reflux disease (GERD)
- eating disorders
- amyloidosis
What are the complications of gastroparesis?
Complications of gastroparesis may include
- dehydration due to repeated vomiting
- malnutrition due to poor absorption of nutrients
- blood glucose, also called blood sugar, levels that are harder to control, which can worsen diabetes
- low calorie intake
- bezoars
- losing weight without trying
- lower quality of life
References
Symptoms & Causes
What are the symptoms of gastroparesis?
The symptoms of gastroparesis may include
- feeling full soon after starting a meal
- feeling full long after eating a meal
- nausea
- vomiting
- too much bloating
- too much belching
- pain in your upper abdomen
- heartburn
- poor appetite
Certain medicines may delay gastric emptying or affect motility, resulting in symptoms that are similar to those of gastroparesis. If you have been diagnosed with gastroparesis, these medicines may make your symptoms worse. Medicines that may delay gastric emptying or make symptoms worse include the following:
- narcotic pain medicines, such as codeine , hydrocodone , morphine , oxycodone , and tapentadol
- some antidepressants , such as amitriptyline , nortriptyline , and venlafaxine
- some anticholinergics —medicines that block certain nerve signals
- some medicines used to treat overactive bladder
- pramlintide
These medicines do not cause gastroparesis.

When should I seek a doctor’s help?
You should seek a doctor’s help right away if you have any of the following signs or symptoms:
- severe pain or cramping in your abdomen
- blood glucose levels that are too high or too low
- red blood in your vomit, or vomit that looks like coffee grounds
- sudden, sharp stomach pain that doesn’t go away
- vomiting for more than an hour
- feeling extremely weak or fainting
- difficulty breathing
- fever
You should seek a doctor’s help if you have any signs or symptoms of dehydration, which may include
- extreme thirst and dry mouth
- urinating less than usual
- feeling tired
- dark-colored urine
- decreased skin turgor, meaning that when your skin is pinched and released, the skin does not flatten back to normal right away
- sunken eyes or cheeks
- light-headedness or fainting
You should seek a doctor’s help if you have any signs or symptoms of malnutrition, which may include
- feeling tired or weak all the time
- losing weight without trying
- feeling dizzy
- loss of appetite
- abnormal paleness of the skin
What causes gastroparesis?
In most cases, doctors aren’t able to find the underlying cause of gastroparesis, even with medical tests. Gastroparesis without a known cause is called idiopathic gastroparesis.
Diabetes is the most common known underlying cause of gastroparesis. Diabetes can damage nerves, such as the vagus nerve and nerves and special cells, called pacemaker cells, in the wall of the stomach. The vagus nerve controls the muscles of the stomach and small intestine. If the vagus nerve is damaged or stops working, the muscles of the stomach and small intestine do not work normally. The movement of food through the digestive tract is then slowed or stopped. Similarly, if nerves or pacemaker cells in the wall of the stomach are damaged or do not work normally, the stomach does not empty.
In addition to diabetes, other known causes of gastroparesis include
- injury to the vagus nerve due to surgery on your esophagus, stomach, or small intestine
- hypothyroidism
- certain autoimmune diseases, such as scleroderma
- certain nervous system disorders, such as Parkinson’s disease and multiple sclerosis
- viral infections of your stomach
Diagnosis
How do doctors diagnose gastroparesis?
Doctors diagnose gastroparesis based on your medical history, a physical exam, your symptoms, and medical tests. Your doctor may also perform medical tests to look for signs of gastroparesis complications and to rule out other health problems that may be causing your symptoms.
Medical history
Your doctor will ask about your medical history. He or she will ask for details about your current symptoms and medicines, and current and past health problems such as diabetes, scleroderma, nervous system disorders, and hypothyroidism.
Your doctor may also ask about
- the types of medicines you are taking. Be sure to tell your doctor about all prescription medicines, over-the-counter medicines, and dietary supplements you are taking.
- whether you’ve had surgery on your esophagus, stomach, or small intestine
- whether you’ve had radiation therapy on your chest or stomach area
Physical exam
During a physical exam, your doctor will
- check your blood pressure, temperature, and heart rate
- check for signs of dehydration and malnutrition
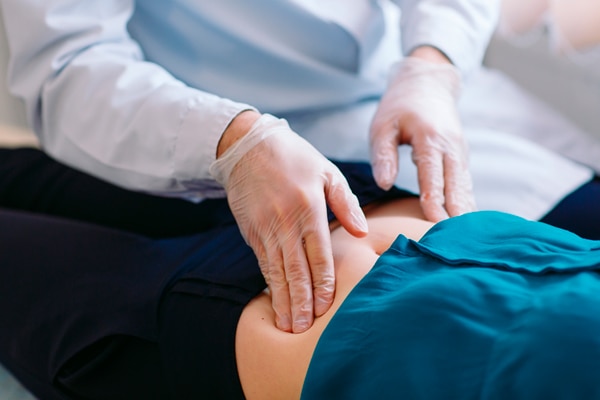
- check your abdomen for unusual sounds, tenderness, or pain
What medical tests do doctors use to diagnose gastroparesis?
Doctors use lab tests, upper gastrointestinal (GI) endoscopy, imaging tests, and tests to measure how fast your stomach is emptying its contents to diagnose gastroparesis.
Lab tests
Your doctor may use the following lab tests:
- Blood tests can show signs of dehydration, malnutrition, inflammation, and infection. Blood tests can also show whether your blood glucose levels are too high or too low.
- Urine tests can show signs of diabetes, dehydration, infection, and kidney problems.
Upper GI endoscopy
Your doctor may perform an upper GI endoscopy to look for problems in your upper digestive tract that may be causing your symptoms.
Imaging tests
Imaging tests can show problems, such as stomach blockage or intestinal obstruction, that may be causing your symptoms. Your doctor may perform the following imaging tests:
- upper GI series
- ultrasound of your abdomen
Tests to Measure Stomach Emptying
Your doctor may perform one of more of the following tests to see how fast your stomach is emptying its contents.
- Gastric emptying scan, also called gastric emptying scintigraphy. For this test, you eat a bland meal—such as eggs or an egg substitute—that contains a small amount of radioactive material. A camera outside your body scans your abdomen to show where the radioactive material is located. By tracking the radioactive material, a health care professional can measure how fast your stomach empties after the meal. The scan usually takes about 4 hours.
- Gastric emptying breath test. For this test, you eat a meal that contains a substance that is absorbed in your intestines and eventually passed into your breath. After you eat the meal, a health care professional collects samples of your breath over a period of a few hours—usually about 4 hours. The test can show how fast your stomach empties after the meal by measuring the amount of the substance in your breath.
- Wireless motility capsule, also called a SmartPill. The SmartPill is a small electronic device that you swallow. The capsule moves through your entire digestive tract and sends information to a recorder hung around your neck or clipped to your belt. A health care professional uses the information to find out how fast or slow your stomach empties, and how fast liquid and food move through your small intestine and large intestine. The capsule will pass naturally out of your body with a bowel movement.
Treatment
How do doctors treat gastroparesis?
How doctors treat gastroparesis depends on the cause, how severe your symptoms and complications are, and how well you respond to different treatments. Sometimes, treating the cause may stop gastroparesis. If diabetes is causing your gastroparesis, your health care professional will work with you to help control your blood glucose levels. When the cause of your gastroparesis is not known, your doctor will provide treatments to help relieve your symptoms and treat complications.
Changing eating habits
Changing your eating habits can help control gastroparesis and make sure you get the right amount of nutrients, calories, and liquids. Getting the right amount of nutrients, calories, and liquids can also treat the disorder’s two main complications: malnutrition and dehydration.
Your doctor may recommend that you
- eat foods low in fat and fiber
- eat five or six small, nutritious meals a day instead of two or three large meals
- chew your food thoroughly
- eat soft, well-cooked foods
- avoid carbonated, or fizzy, beverages
- avoid alcohol
- drink plenty of water or liquids that contain glucose and electrolytes, such as
- low-fat broths or clear soups
- naturally sweetened, low-fiber fruit and vegetable juices
- sports drinks
- oral rehydration solutions
- do some gentle physical activity after a meal, such as taking a walk
- avoid lying down for 2 hours after a meal
- take a multivitamin each day
If your symptoms are moderate to severe, your doctor may recommend drinking only liquids or eating well-cooked solid foods that have been processed into very small pieces or paste in a blender.
Controlling blood glucose levels
If you have gastroparesis and diabetes, you will need to control your blood glucose levels, especially hyperglycemia. Hyperglycemia may further delay the emptying of food from your stomach. Your doctor will work with you to make sure your blood glucose levels are not too high or too low and don’t keep going up or down. Your doctor may recommend
- taking insulin more often, or changing the type of insulin you take
- taking insulin after, instead of before, meals
- checking your blood glucose levels often after you eat, and taking insulin when you need it
Your doctor will give you specific instructions for taking insulin based on your needs and the severity of your gastroparesis.
Medicines
Your doctor may prescribe medicines that help the muscles in the wall of your stomach work better. He or she may also prescribe medicines to control nausea and vomiting and reduce pain.
Your doctor may prescribe one or more of the following medicines:
- Metoclopramide. This medicine increases the tightening, or contraction, of the muscles in the wall of your stomach and may improve gastric emptying. Metoclopramide may also help relieve nausea and vomiting.
- Domperidone. This medicine also increases the contraction of the muscles in the wall of your stomach and may improve gastric emptying. However, this medicine is available for use only under a special program administered by the U.S. Food and Drug Administration.
- Erythromycin. This medicine also increases stomach muscle contraction and may improve gastric emptying.
- Antiemetics. Antiemetics are medicines that help relieve nausea and vomiting. Prescription antiemetics include ondansetron , prochlorperazine , and promethazine. Over-the-counter antiemetics include bismuth subsalicylate and diphenhydramine . Antiemetics do not improve gastric emptying.
- Antidepressants. Certain antidepressants, such as mirtazapine, may help relieve nausea and vomiting. These medicines may not improve gastric emptying.
- Pain medicines. Pain medicines that are not narcotic pain medicines may reduce pain in your abdomen due to gastroparesis.

Oral or nasal tube feeding
In some cases, your doctor may recommend oral or nasal tube feeding to make sure you’re getting the right amount of nutrients and calories. A health care professional will put a tube either into your mouth or nose, through your esophagus and stomach, to your small intestine. Oral and nasal tube feeding bypass your stomach and deliver a special liquid food directly into your small intestine.
Jejunostomy tube feeding
If you aren’t getting enough nutrients and calories from other treatments, your doctor may recommend jejunostomy tube feeding. Jejunostomy feedings are a longer term method of feeding, compared to oral or nasal tube feeding.
Jejunostomy tube feeding is a way to feed you through a tube placed into part of your small intestine called the jejunum. To place the tube into the jejunum, a doctor creates an opening, called a jejunostomy, in your abdominal wall that goes into your jejunum. The feeding tube bypasses your stomach and delivers a liquid food directly into your jejunum.
Parenteral nutrition
Your doctor may recommend parenteral, or intravenous (IV), nutrition if your gastroparesis is so severe that other treatments are not helping. Parenteral nutrition delivers liquid nutrients directly into your bloodstream. Parenteral nutrition may be short term, until you can eat again. Parenteral nutrition may also be used until a tube can be placed for oral, nasal, or jejunostomy tube feeding. In some cases, parental nutrition may be long term.
Venting gastrostomy
Your doctor may recommend a venting gastrostomy to relieve pressure inside your stomach. A doctor creates an opening, called a gastrostomy, in your abdominal wall and into your stomach. The doctor then places a tube through the gastrostomy into your stomach. Stomach contents can then flow out of the tube and relieve pressure inside your stomach.
Gastric electrical stimulation
Gastric electrical stimulation (GES) uses a small, battery-powered device to send mild electrical pulses to the nerves and muscles in the lower stomach. A surgeon puts the device under the skin in your lower abdomen and attaches wires from the device to the muscles in the wall of your stomach. GES can help decrease long-term nausea and vomiting.
GES is used to treat people with gastroparesis due to diabetes or unknown causes only, and only in people whose symptoms can’t be controlled with medicines.
How can I prevent gastroparesis?
Gastroparesis without a known cause, called idiopathic gastroparesis, cannot be prevented.
If you have diabetes, you can prevent or delay nerve damage that can cause gastroparesis by keeping your blood glucose levels within the target range that your doctor thinks is best for you. Meal planning, physical activity, and medicines, if needed, can help you keep your blood glucose levels within your target range.
Eating, Diet, & Nutrition
How can my diet help prevent or relieve gastroparesis?
What you eat can help prevent or relieve your gastroparesis symptoms. If you have diabetes, following a healthy meal plan can help you manage your blood glucose levels. What you eat can also help make sure you get the right amount of nutrients, calories, and liquids if you are malnourished or dehydrated from gastroparesis.
What should I eat and drink if I have gastroparesis?
If you have gastroparesis, your doctor may recommend that you eat or drink
- foods and beverages that are low in fat
- foods and beverages that are low in fiber
- five or six small, nutritious meals a day instead of two or three large meals
- soft, well-cooked foods
If you are unable to eat solid foods, your doctor may recommend that you drink
- liquid nutrition meals
- solid foods puréed in a blender
Your doctor may also recommend that you drink plenty of water or liquids that contain glucose and electrolytes, such as
- low-fat broths and clear soups
- low-fiber fruit and vegetable juices
- sports drinks
- oral rehydration solutions
If your symptoms are moderate to severe, your doctor may recommend drinking only liquids or eating well-cooked solid foods that have been processed into very small pieces or paste in a blender.
What should I avoid eating and drinking if I have gastroparesis?
If you have gastroparesis, you should avoid
- foods and beverages that are high in fat
- foods and beverages that are high in fiber
- foods that can’t be chewed easily
- carbonated, or fizzy, beverages
- alcohol
Your doctor may refer you to a dietitian to help you plan healthy meals that are easy for you to digest and give you the right amount of nutrients, calories, and liquids.
Clinical Trials
The National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) and other components of the National Institutes of Health (NIH) conduct and support research into many diseases and conditions.
What are clinical trials and are they right for you?
Clinical trials are part of clinical research and at the heart of all medical advances. Clinical trials look at new ways to prevent, detect, or treat disease. Researchers also use clinical trials to look at other aspects of care, such as improving the quality of life for people with chronic illnesses. Find out if clinical trials are right for you.
Watch a video of NIDDK Director Dr. Griffin P. Rodgers explaining the importance of participating in clinical trials.
What clinical trials are open?
Clinical trials that are currently open and are recruiting can be viewed at ClinicalTrials.gov.
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
The NIDDK would like to thank:
Michael Camilleri, M.D., Mayo Clinic, Rochester
