Understanding Adult Overweight & Obesity
- Definition & Facts
- Factors Affecting Weight & Health
- Am I at a Healthy Weight?
- Health Risks
- Eating & Physical Activity
- Treatment
- Clinical Trials
Definition & Facts
What are overweight and obesity?
People whose weight is higher than what is considered healthy for their height are described as having overweight or obesity.1 Overweight and obesity can increase your risk for many health problems.
Body mass index
Overweight and obesity are defined by body mass index (BMI). BMI is a measurement that uses your weight and height to estimate overweight and obesity. The table below shows BMI ranges for overweight and obesity in adults ages 20 and older.
BMI of adults ages 20 and older
BMI |
Category |
|---|---|
18.5 to 24.9 |
Healthy weight |
25 to 29.9 |
Overweight |
30+ |
Obesity (including severe obesity) |
40+ |
Severe obesity |
Calculate your BMI with this online tool.
How common are overweight and obesity?
Overweight and obesity are common among U.S. adults ages 20 and older. According to estimates based on data from the 2017–2018 National Health and Nutrition Examination Survey (NHANES)2
- nearly 1 in 3 adults (30.7%) have overweight
- more than 2 in 5 adults (42.4%) have obesity, including about 1 in 11 adults (9.2%) with severe obesity
- nearly 3 in 4 adults (73.1%) have overweight or obesity
 More than 2 in 5 U.S. adults have obesity.
More than 2 in 5 U.S. adults have obesity.
Sex
Men are more likely than women to have overweight or obesity. Among adults ages 20 and older, 77.1% of men and 69.4% of women have overweight or obesity.2 But severe obesity, or having a BMI greater than 40, is more common among women (11.5%) than men (6.9%).
Race and ethnicity
Overweight and obesity rates also vary among racial and ethnic groups. According to 2017–2018 NHANES data, obesity affects2
- nearly 1 in 2 non-Hispanic Black adults (49.6%)
- more than 2 in 5 Hispanic adults (44.8%)
- more than 2 in 5 non-Hispanic White adults (42.2%)
- more than 1 in 6 non-Hispanic Asian adults (17.4%)
Other groups
Overweight and obesity also vary among other groups. For example, obesity is more common among people in rural areas than among those who live in urban areas.3
References
Factors Affecting Weight & Health
Many factors can affect your weight, including
- lifestyle habits
- where you live, work, play, and worship
- how much sleep you get
- medicines
- health problems
- family history and genes
Lifestyle habits
Lifestyle habits—including the foods and beverages you consume and how active you are in your daily life—can also affect your weight. If you take in more calories from food or beverages than you use during physical activity and through daily living, such as doing housework or walking to the store, your body may store some of these extra calories as fat. Lifestyle habits that may lead to weight gain include
- eating or drinking a lot of foods and beverages that are high in calories, sugar, and fat
- drinking a lot of beverages that are high in added sugars
- spending a lot of time sitting or lying down
Over time, if you continue to take in more calories than you use, you will likely gain weight.
Where you live, work, play, and worship
Where you live, work, play, and worship can also make a difference. It may be easier for you to make healthier lifestyle choices if
- you live near a grocery store that offers healthy affordable foods, including fruits and vegetables
- your workplace has a kitchen where you can store and prepare healthy meals you bring from home
- your job doesn’t require you to spend a lot of time sitting down
- your neighborhood has safe places to walk or do other types of physical activity
- your place of worship includes healthy food options at special events
How much sleep you get
 Adults ages 18 to 64 should get 7 to 9 hours of sleep a night.
Adults ages 18 to 64 should get 7 to 9 hours of sleep a night.Not getting enough sleep is also linked to weight gain. Experts recommend that adults ages 18 to 64 get 7 to 9 hours of sleep a night. Adults ages 65 and older should get 7 to 8 hours of sleep a night.4
Not getting enough sleep may make you feel hungrier, consume more calories, and be more likely to choose unhealthy foods and beverages instead of healthier options.5 Getting enough sleep may help prevent these problems and increase overall well-being.
Medicines
Some medicines can affect your energy balance by making you hungry or making your body burn fewer calories. Medicines that may contribute to weight gain include6
- some medicines used to treat epilepsy, depression, or psychotic disorders
- corticosteroids, also called steroids
- some diabetes medicines, such as insulin and sulfonylureas—a type of medicine that helps your pancreas release insulin into your blood
- some medicines used to treat high blood pressure and improve your body’s blood flow, such as beta-blockers, alpha-blockers, and calcium channel blockers
- some antihistamine medicines used to treat allergy symptoms
Health problems
Some health problems may also lead to obesity or weight gain. Examples include6
- some endocrine diseases, such as polycystic ovary syndrome (PCOS), Cushing’s syndrome, and hypothyroidism
- damage to your hypothalamus, a small area of your brain near the pituitary gland
- depression
- long-term stress
Some eating disorders, such as binge-eating disorder and bulimia nervosa, may also lead to obesity or weight gain. Both disorders involve eating a large amount of food while feeling a loss of control. In bulimia, people try to prevent weight gain in unhealthy ways, such as by vomiting or using laxatives.
Family history and genes
Your chances of having overweight or obesity are greater if one or both of your parents have overweight or obesity.7 Children whose mothers had obesity during pregnancy are also more likely to have obesity themselves.8 Children and adolescents who have obesity are more likely to have obesity as adults.
Your genes may also affect both the amount of fat you store in your body and where on your body you carry the extra fat. Genes may also play a role in your appetite and how physically active you are.
References
Am I at a Healthy Weight?
How can I tell if I am at a healthy weight?
Two measurements—your body mass index (BMI) and your waist size—can help you figure out if you’re at a healthy weight.
Body mass index
Body mass index (BMI) is a measurement that estimates if a person has a healthy weight, overweight, or obesity. Having overweight or obesity can increase your risk for many health problems. Adults can use a BMI calculator to estimate their BMI.
Your BMI is calculated based on your height and weight. It doesn’t directly measure the amount of fat in your body. As a result, for some people, it may not be the best way to assess health risks related to excess body fat. For example
- A person who is very muscular, like a bodybuilder, may have a high BMI without having a lot of body fat.
- Some people with Asian ancestry tend to store extra body fat around their waist. Storing extra fat around the abdomen, or belly, can increase their risk for weight-related health problems even if their BMI is not high.9
- Older adults tend to lose bone and muscle, and gain body fat, as they age. Gaining extra body fat as you get older can increase your risk for health problems, even if your BMI does not change.10
Waist size
Where your body stores fat matters. People who have overweight or obesity are more likely to have weight-related health problems if they have extra body fat in the upper body—especially around their abdomen.10
The following waist sizes increase the risk for obesity-related health problems11
- Women: 35 inches or more
- Men: 40 inches or more
 A large waist size can increase the risk for health problems related to obesity.
A large waist size can increase the risk for health problems related to obesity.Do I need to lose weight?
Your health care professional may recommend you lose weight if you have any of the following
- obesity, or a BMI of 30 or higher.
- a large waist size.
- heart disease or a family history of heart disease.
- overweight, or a BMI of 25 to 29.9, plus one or more factors that raise your chance of getting heart disease. These factors include
- diabetes
- prediabetes
- high blood pressure
- high levels of LDL cholesterol, low levels of HDL cholesterol, or high levels of triglycerides
References
Health Risks
In this section:
- Type 2 diabetes
- High blood pressure
- Heart disease
- Stroke
- Metabolic syndrome
- Fatty liver diseases
- Some cancers
- Breathing problems
- Osteoarthritis
- Gout
- Diseases of the gallbladder and pancreas
- Kidney disease
- Pregnancy problems
- Fertility problems
- Sexual function problems
- Mental health problems
Overweight and obesity may increase your risk for many health problems—especially if you carry extra fat around your waist. Reaching and staying at a healthy weight can help prevent these problems, stop them from getting worse, or even make them go away.
Type 2 diabetes
Type 2 diabetes is a disease that occurs when your blood glucose, also called blood sugar, is too high. Nearly 9 in 10 people with type 2 diabetes have overweight or obesity.12 Over time, high blood glucose can lead to heart disease, stroke, kidney disease, eye problems, nerve damage, and other health problems.
If you are at risk for type 2 diabetes, you may be able to prevent or delay diabetes by losing at least 5% to 7% of your starting weight.13,14 For instance, if you weigh 200 pounds, your goal would be to lose about 10 to 14 pounds.
High blood pressure
 Overweight and obesity may raise your risk for high blood pressure.
Overweight and obesity may raise your risk for high blood pressure.High blood pressure, also called hypertension, is a condition in which blood flows through your blood vessels with a force greater than normal. Having a large body size may increase blood pressure because your heart needs to pump harder to supply blood to all your cells. Excess fat may also damage your kidneys, which help regulate blood pressure.
High blood pressure can strain your heart, damage blood vessels, and raise your risk of heart attack, stroke, kidney disease, and death.10 Losing enough weight to reach a healthy body mass index range may lower high blood pressure and prevent or control related health problems.
Heart disease
Heart disease is a term used to describe several health problems that affect your heart, such as a heart attack, heart failure, angina, or an abnormal heart rhythm. Having overweight or obesity increases your risk of developing conditions that can lead to heart disease, such as high blood pressure, high blood cholesterol, and high blood glucose. In addition, excess weight can also make your heart have to work harder to send blood to all the cells in your body. Losing excess weight may help you lower these risk factors for heart disease.
Stroke
A stroke happens when a blood vessel in your brain or neck is blocked or bursts, cutting off blood flow to a part of your brain. A stroke can damage brain tissue and make you unable to speak or move parts of your body.
Overweight and obesity are known to increase blood pressure—and high blood pressure is the leading cause of strokes. Losing weight may help you lower your blood pressure and other risk factors for stroke, including high blood glucose and high blood cholesterol.
Metabolic syndrome
Metabolic syndrome is a group of conditions that increase your risk for heart disease, diabetes, and stroke. To be diagnosed with metabolic syndrome, you must have at least three of the following conditions
- large waist size
- high level of triglycerides in your blood
- high blood pressure
- high level of blood glucose when fasting
- low level of HDL cholesterol —the “good” cholesterol—in your blood
Metabolic syndrome is closely linked to overweight and obesity and to a lack of physical activity. Healthy lifestyle changes that help you control your weight may help you prevent and reduce metabolic syndrome.
Fatty liver diseases
Fatty liver diseases develop when fat builds up in your liver, which can lead to severe liver damage, cirrhosis, or even liver failure. These diseases include nonalcoholic fatty liver disease (NAFLD) and nonalcoholic steatohepatitis (NASH).
NAFLD and NASH most often affect people who have overweight or obesity. People who have insulin resistance, unhealthy levels of fat in the blood, metabolic syndrome, type 2 diabetes, and certain genes can also develop NAFLD and NASH.
If you have overweight or obesity, losing at least 3% to 5% of your body weight may reduce fat in the liver.15
Some cancers
Cancer is a collection of related diseases. In all types of cancer, some of the body’s cells begin to grow abnormally or out of control. The cancerous cells sometimes spread to other parts of the body.
Overweight and obesity may raise your risk of developing certain types of cancer. Men with overweight or obesity are at a higher risk for developing cancers of the colon, rectum, and prostate.10 Among women with overweight or obesity, cancers of the breast, lining of the uterus, and gallbladder are more common.
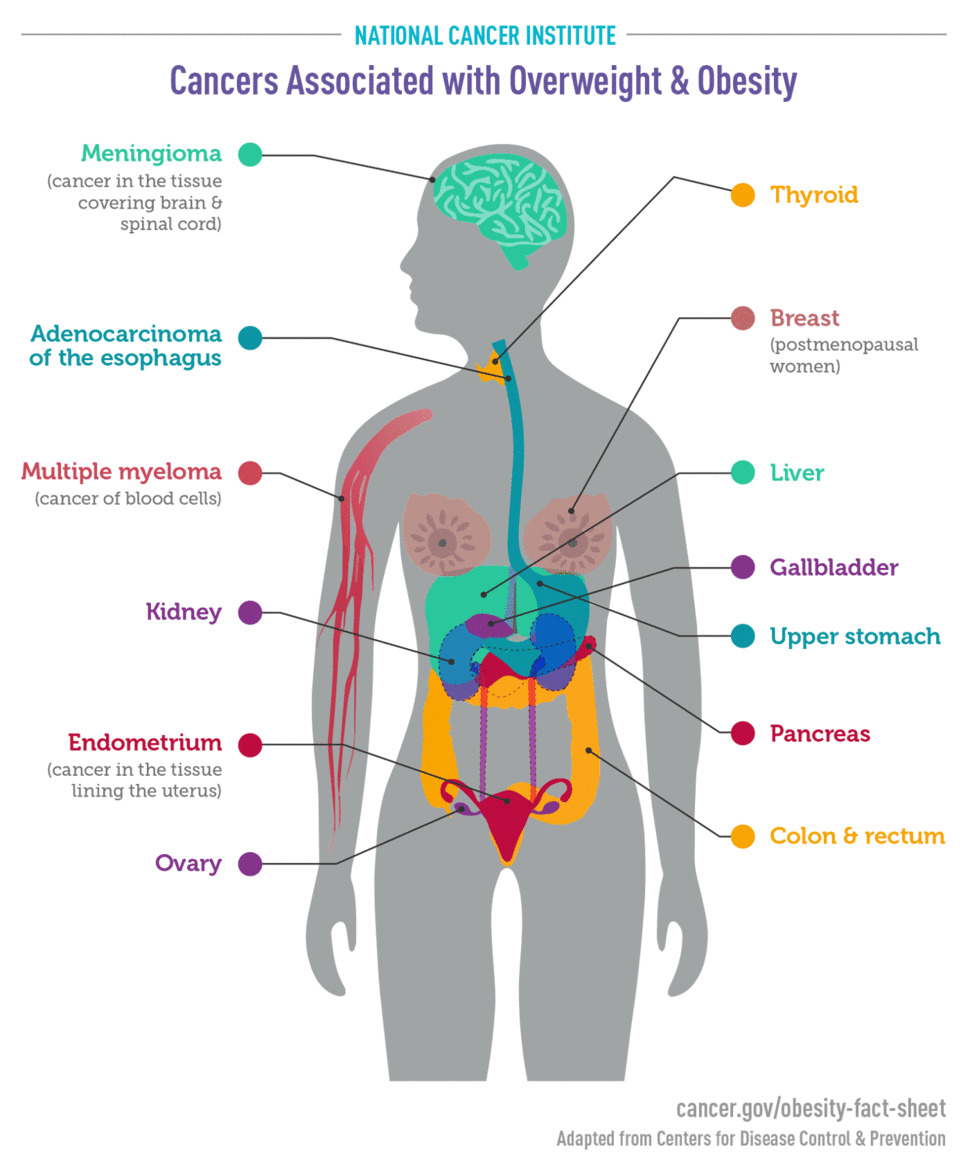 Overweight and obesity may increase risk of developing many types of cancer.
Overweight and obesity may increase risk of developing many types of cancer.
Adults who gain less weight as they get older have lower risks of many types of cancer, including colon, kidney, breast, and ovarian cancers.16
Breathing problems
Overweight and obesity can also affect how well your lungs work, and excess weight increases your risk for breathing problems.17
Sleep apnea
Sleep apnea is a common problem that can happen while you are sleeping. If you have sleep apnea, your upper airway becomes blocked, causing you to breathe irregularly or even stop breathing altogether for short periods of time. Untreated sleep apnea may raise your risk for developing many health problems, including heart disease and diabetes.
Obesity is a common cause of sleep apnea in adults.18 If you have overweight or obesity, you may have more fat stored around your neck, making the airway smaller. A smaller airway can make breathing difficult or cause snoring. If you have overweight or obesity, losing weight may help reduce sleep apnea or make it go away.
Asthma
Asthma is a chronic, or long-term, condition that affects the airways in your lungs. The airways are tubes that carry air in and out of your lungs. If you have asthma, the airways can become inflamed and narrow at times. You may wheeze, cough, or feel tightness in your chest.
Obesity can increase your risk of developing asthma, experiencing worse symptoms, and having a harder time managing the condition.19 Losing weight can make it easier for you to manage your asthma. For people who have severe obesity, weight-loss surgery—also called metabolic and bariatric surgery—may improve asthma symptoms.17
Osteoarthritis
Osteoarthritis is a common, long-lasting health problem that causes pain, swelling, stiffness, and reduced motion in your joints. Obesity is a leading risk factor for osteoarthritis in the knees, hips, and ankles.20
Having overweight or obesity may raise your risk of getting osteoarthritis by putting extra pressure on your joints and cartilage. If you have excess body fat, your blood may have higher levels of substances that cause inflammation. Inflamed joints may raise your risk for osteoarthritis.
 Having overweight or obesity may raise your risk of getting osteoarthritis in your knees.
Having overweight or obesity may raise your risk of getting osteoarthritis in your knees.
If you have overweight or obesity, losing weight may decrease stress on your knees, hips, and lower back and lessen inflammation in your body. If you have osteoarthritis, losing weight may improve your symptoms. Research shows that exercise is one of the best treatments for osteoarthritis. Exercise can improve mood, decrease pain, and increase flexibility.
Gout
Gout is a kind of arthritis that causes pain and swelling in your joints. Gout develops when crystals made of a substance called uric acid build up in your joints. Risk factors include having obesity, being male, having high blood pressure, and eating foods high in purines.21 These foods include red meat, liver, and anchovies.
Gout is treated mainly with medicines. Losing weight may also help prevent and treat gout.22
Diseases of the gallbladder and pancreas
Overweight and obesity may raise your risk of getting gallbladder diseases, such as gallstones and cholecystitis. People who have obesity may have higher levels of cholesterol in their bile, which can cause gallstones. They may also have a large gallbladder that does not work well.
Having a large amount of fat around your waist may raise your risk for developing gallstones. But losing weight quickly also increases your risk. If you have obesity, talk with your health care professional about how to lose weight safely.
Obesity can also affect your pancreas, a large gland behind your stomach that makes insulin and enzymes to help you digest food. People who have obesity have a higher risk of developing inflammation of the pancreas, called pancreatitis. High levels of fat in your blood can also raise your risk of having pancreatitis. You can lower your chances of getting pancreatitis by sticking with a low-fat, healthy eating plan.
Kidney disease
Kidney disease means your kidneys are damaged and can’t filter your blood as they should. Obesity raises the risk of developing diabetes and high blood pressure, which are the most common causes of chronic kidney disease (CKD). Even if you don’t have diabetes or high blood pressure, having obesity may increase your risk of developing CKD and speed up its progress.23
If you have overweight or obesity, losing weight may help you prevent or delay CKD. If you are in the early stages of CKD, consuming healthy foods and beverages, being active, and losing excess weight may slow the progress of the disease and keep your kidneys healthier longer.24
Pregnancy problems
 Overweight and obesity raise the risk of developing health problems that can affect the pregnancy and the baby’s health.
Overweight and obesity raise the risk of developing health problems that can affect the pregnancy and the baby’s health.
Overweight and obesity raise the risk of developing health problems during pregnancy that can affect the pregnancy and the baby’s health. Pregnant women who have obesity may have a greater chance of 10
- developing gestational diabetes, or diabetes that occurs during pregnancy
- having preeclampsia, or high blood pressure during pregnancy, which can cause severe health problems for the pregnant woman and baby if left untreated
- needing a caesarean delivery—or c-section—and, as a result, taking longer to recover after giving birth
- having complications from surgery and anesthesia, especially if they have severe obesity
- gaining more weight or continuing to have overweight or obesity after the baby is born
Having obesity or gaining too much weight during pregnancy can also increase health risks for the baby, including25
- being born larger than expected based on the sex of the baby or the duration of the pregnancy
- developing chronic diseases as adults, including type 2 diabetes, obesity, heart disease, and asthma
Talk with your health care professional about how to
- reach a healthy weight before pregnancy
- gain a healthy amount of weight during pregnancy
- safely lose weight after your baby is born
Fertility problems
Obesity increases the risk of developing infertility. Infertility in women means not being able to get pregnant after a year of trying, or getting pregnant but not being able to carry a pregnancy to term. For men, it means not being able to get a woman pregnant.26
Obesity is linked to lower sperm count and sperm quality in men.27 In women, obesity is linked to problems with the menstrual cycle and ovulation.26 Obesity can also make it harder to become pregnant with the help of certain infertility treatments or procedures.26
Women with obesity who lose 5% of their body weight may increase their chances of having regular menstrual periods, ovulating, and becoming pregnant.28
Sexual function problems
Obesity may also increase the risk of developing sexual function problems.29 Having overweight or obesity increase the risk of developing erectile dysfunction (ED), a condition in which males are unable to get or keep an erection firm enough for satisfactory sexual intercourse.
Few studies have looked at how obesity may affect female sexual function by contributing to problems such as loss of sexual desire, being unable to become or stay aroused, being unable to have an orgasm, or having pain during sex.30 But research suggests that healthy eating, increased physical activity, and weight loss may help reduce sexual function problems in people with obesity.29,30
Mental health problems
In addition to increasing the risk for developing physical health problems, obesity can also affect mental health, increasing the risk for developing31
- long-term stress
- body image problems
- low self-esteem
- depression
- eating disorders
Studies show that people with overweight or obesity are also likely to face weight-related bias at school and work, which may cause long-term harm to their quality of life.31 Losing excess weight has been found to improve body image and self-esteem and reduce symptoms of depression.32
References
Eating & Physical Activity
How can a healthy eating plan and physical activity help me lose or maintain weight?
The key to losing weight is choosing a healthy eating plan that you can maintain over time. Being physically active will help you use more calories and maintain your weight loss.
Follow a healthy eating plan
The 2020–2025 Dietary Guidelines for Americans notes that adults who want to lose weight and keep it off should reduce the number of calories they take in from foods and beverages. The guidelines recommend a healthy eating plan that includes
- vegetables of all types
- fruits, especially whole fruits rather than fruit juices
- whole grains, such as brown rice, oats, and whole-wheat bread
- dairy, including fat-free or low-fat milk, yogurt, and cheese, or similar products such as soy beverages with added calcium, vitamin A, and vitamin D
- protein from foods such as lean meats, poultry, and eggs; seafood; beans, peas, and lentils; and nuts, seeds, and soy products
- certain oils, such as olive oil and oils found in seafood, nuts, and avocados
 A healthy eating plan includes a variety of healthy, nutritious foods.
A healthy eating plan includes a variety of healthy, nutritious foods.
The guidelines also note that adults should limit
- added sugars to less than 10% of calories per day
- saturated fat to less than 10% of calories per day
- sodium, or salt, to less than 2,300 milligrams per day
Get regular physical activity
Physical activity can help you lose excess weight and stay at a healthy weight. Being active is also linked to many other health benefits. Regular aerobic activity can help prevent and reduce health problems, such as high blood pressure and high blood glucose, also called blood sugar. Aerobic activity can also improve mental health.32
The Physical Activity Guidelines for Americans, 2nd edition (PDF, 14.8 MB) recommend that healthy adults take part in
- moderate-intensity aerobic activity, such as brisk walking or dancing, for at least 150 minutes a week. A moderate-intensity aerobic activity makes your heart beat faster and makes you breathe harder but does not overwork you.
- muscle-strengthening activities that involve all major muscle groups on two or more days a week.
Adults with chronic health conditions or people with disabilities who cannot meet these guidelines should take part in regular physical activities that they can do safely. If you have a health condition such as heart disease, high blood pressure, or diabetes, talk with your health care professional before you start regular physical activity. Your health care professional can help you find activities you can do safely and will benefit you the most.
How can I adopt healthier habits?
Adopting a healthy eating plan and getting more physical activity every day may be difficult. But with effort, regular support, and patience, you can make changes that will help you lose weight and improve your health over the long term.
Be prepared for setbacks—they are normal
After a setback, such as overeating at a family or workplace gathering, try to regroup and focus on getting back to your healthy eating plan as soon as you can. Try to eat only when you’re sitting in your dining room or at your kitchen table. Try to keep snack foods and higher calorie options out of your home or stored in a cabinet or pantry—not out on the counter. At work, avoid areas where treats may be available. Follow your progress using online trackers or smartphone apps that can help you keep track of the foods you eat, your physical activity, and your weight. These tools may help you stick with your plan and stay motivated.
Set goals
Having specific goals can help you stay on track. Rather than “be more active,” set a goal to walk 15 to 30 minutes before work or at lunch on Mondays and Fridays. If you miss a walk on Monday, pick it up again Tuesday. Using tools such as the Body Weight Planner may help you set realistic goals to consume fewer calories and be more physically active.
Seek support
Ask for help or encouragement from your family, friends, or health care professionals. You can get support in person, through email or text, or by phone. You can also join a support group. Specially trained health professionals can help you change your lifestyle.
How can I maintain weight loss?
 Continue to make healthy food choices to stay at a healthy weight.
Continue to make healthy food choices to stay at a healthy weight.Keeping the weight off can be hard. Your metabolism slows down during weight loss, and your body needs fewer calories at your new, lower weight. Changes in your hormones and other factors may also make it hard to keep the weight off.
Stick to your healthy eating plan
Continue to make healthy food choices and follow your healthy eating plan as a lifelong habit. Find healthy food options that you prefer and enjoy, as this will make you more likely to stick with your eating plan.
Continue regular physical activity
Regular physical activity may help you keep the weight you’ve lost from coming back.32 To prevent weight regain, aim for at least 300 minutes a week of moderate-intensity physical activity.33 Make regular physical activity a lifelong habit.
Keep track of your weight
Weigh yourself regularly and try to keep a record of changes to your weight. Recording your progress may help you stay focused and catch setbacks in meeting your goals. Remember—a setback does not mean you have failed. Everyone experiences setbacks. The key is to get back on track as soon as you can.
References
Treatment
Most often, health care professionals treat overweight and obesity by helping you adopt lifestyle changes that may help you lose excess weight safely and keep it off over the long term. In some cases, other treatments such as weight-loss medicines or weight-loss surgery can be helpful.
How much weight should I lose?
If you need to lose weight, work with a health care professional to set a weight-loss goal and time frame that will work best for you. For example, losing 5% of your body weight over a period of 6 months may be a good initial goal.34 If you weigh 200 pounds, this would mean losing 10 pounds.
Losing excess weight may help lower your chances of developing health problems related to overweight and obesity. If you already have weight-related health problems, such as high blood pressure or diabetes, losing weight may help improve your health.
How do health care professionals treat overweight and obesity?
Lifestyle changes
Health care professionals often treat overweight and obesity by recommending lifestyle changes, such as adopting a healthy eating plan and increasing your physical activity, to help you lose weight safely. These lifestyle changes can help you reduce the calories you take in from food and beverages and increase the calories you use up by being active.
Tailored weight-loss program
In some cases, your health care professional may refer you to a health care specialist or a health care team trained in weight management. These specialists will design a plan just for you and help you carry out your plan.
Safe and successful weight-loss programs typically include32
- 14 or more weight-loss counseling sessions conducted over 6 months
- an eating plan based on the calories and nutrients your body needs
- at least 150 minutes per week of moderate-intensity aerobic physical activity, such as brisk walking or cycling
- daily monitoring of food intake and physical activity, and weekly monitoring of weight
- regular feedback and support from specialists
You may work with the specialists in individual or group sessions. The sessions might be held in person or online using smartphones, computers, or other devices. The specialists may contact you regularly by telephone or email to help support your plan. Smartphone apps and other tools may help you track how well you are sticking with your plan.
 When combined with healthy eating, regular physical activity may help you lose weight and stay at a healthy weight.
When combined with healthy eating, regular physical activity may help you lose weight and stay at a healthy weight.
Weight-loss medicines
Weight loss can be difficult to achieve and maintain. When lifestyle changes are not enough, your health care professional may prescribe medicines to treat overweight and obesity. Some medicines can also be used to help you maintain weight loss. You should try to stick with your healthy eating plan and stay physically active while taking weight-loss medicines.
Weight-loss surgery
Weight-loss surgery, also called metabolic and bariatric surgery, includes several types of operations that help you lose weight by making changes to your digestive system. Your doctor may recommend weight-loss surgery if you have a body mass index (BMI) of 35 or higher. Some doctors and professional groups recommend weight-loss surgery for people with a lower BMI if they have a serious health problem related to obesity, such as type 2 diabetes or sleep apnea.35,36
Weight-loss devices
Your health care professional may consider weight-loss devices if you haven’t been able to lose weight or keep off the weight you lost using other treatments. Because weight-loss devices have only recently been approved by the U.S. Food and Drug Administration, researchers don’t know the long-term risks and benefits.
References
Clinical Trials
NIDDK conducts and supports clinical trials in many diseases and conditions, including overweight and obesity. The trials look to find new ways to prevent, detect, or treat disease and improve quality of life.
What are clinical trials for overweight and obesity?
Clinical trials—and other types of clinical studies—are part of medical research and involve people like you. When you volunteer to take part in a clinical study, you help health care professionals and researchers learn more about disease and improve health care for people in the future.
Researchers are studying many aspects of overweight and obesity, such as
- why some people find it harder than other people to maintain weight loss over time
- new medicines that could help people with obesity lose weight and keep it off
- different treatments that may prevent weight regain after weight-loss surgery, also called metabolic and bariatric surgery
- why storing excess fat in some parts of your body—such as in your abdomen, or belly—rather than other parts of your body may increase the risk of developing health problems such as type 2 diabetes
- how weight-loss surgery may lower long-term health costs for adults with obesity
Find out if clinical studies are right for you.
Watch a video of NIDDK Director Dr. Griffin P. Rodgers explaining the importance of participating in clinical trials.
What clinical studies for overweight or obesity are looking for participants?
You can view a filtered list of clinical studies on overweight or obesity that are federally funded, open, and recruiting at ClinicalTrials.gov. You can expand or narrow the list to include clinical studies from industry, universities, and individuals; however, the National Institutes of Health does not review these studies and cannot ensure they are safe. Always talk with your health care provider before you participate in a clinical study.
What have we learned about overweight and obesity from NIDDK-funded research?
NIDDK has supported many research projects to learn more about overweight and obesity.
The Look AHEAD: Action for Health in Diabetes study showed that people who had type 2 diabetes and were overweight or had obesity can lose weight and maintain that weight loss through a program of healthy eating and increased physical activity. The study also showed that weight loss provides other health benefits, such as better physical mobility and improved blood glucose, blood pressure, and cholesterol levels. The trial was extended to study the long-term effects in older adults with type 2 diabetes.
The Longitudinal Assessment of Bariatric Surgery (LABS) study looked at the effects of two types of weight-loss surgery in adults, gastric bypass and adjustable gastric band. LABS found that weight-loss surgery is relatively safe when performed by experienced surgeons. It can also lead to significant weight loss and may improve many weight-related health problems. After 7 years, the average weight loss of patients who had gastric bypass surgery was 84 pounds, or about 28% of their starting weight. The average weight loss of patients who had gastric band surgery was 41 pounds, or about 15% of their starting weight. Because gastric band surgery is less effective than other types of weight-loss surgery, it is not often performed.
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
NIDDK would like to thank:
Kelly Costello Allison, Ph.D., University of Pennsylvania
