Cystoscopy & Ureteroscopy
On this page:
- What are cystoscopy and ureteroscopy?
- Why do health care professionals perform cystoscopy?
- Why do health care professionals perform ureteroscopy?
- How do I prepare for a cystoscopy or ureteroscopy?
- How do health care professionals perform cystoscopy or ureteroscopy?
- What should I expect after a cystoscopy or ureteroscopy?
- What are the risks of cystoscopy and ureteroscopy?
What are cystoscopy and ureteroscopy?
Cystoscopy and ureteroscopy are common procedures performed by a urologist to look inside the urinary tract.
Cystoscopy is a procedure that uses a cystoscope to look inside the urethra and bladder. A cystoscope is a long, thin optical instrument with an eyepiece at one end, a rigid or flexible tube in the middle, and a tiny lens and light at the other end of the tube. A urologist fills the bladder with fluid and looks at detailed images of the urethra and bladder linings on a computer monitor.
Ureteroscopy is a procedure that uses a ureteroscope to look inside the ureters and kidneys. Like a cystoscope, a ureteroscope has an eyepiece at one end, a rigid or flexible tube in the middle, and a tiny lens and light at the other end of the tube. However, a ureteroscope is longer and thinner than a cystoscope so the urologist can see detailed images of the lining of the ureters and kidneys.
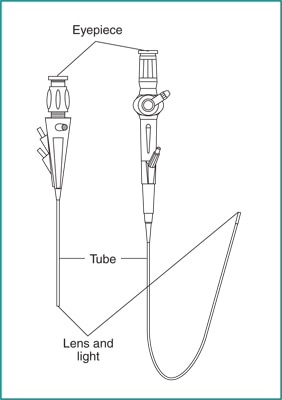 Cystoscope (left) and ureteroscope (right)
Cystoscope (left) and ureteroscope (right)Why do health care professionals perform cystoscopy?
A urologist performs a cystoscopy to find the cause of, and sometimes treat, urinary tract problems such as
- frequent urinary tract infections (UTIs)
- blood in the urine, called hematuria
- urinary frequency, urinary urgency, or urinary incontinence
- urinary retention
- pain or burning before, during, or after urination
- trouble starting urination, completing urination, or both
- abnormal cells, such as cancer cells, found in a urine sample
During a cystoscopy, a urologist can see
- stones—solid pieces of material in the bladder formed by high concentrations of minerals in the urine
- abnormal tissue, tumors, or cancer in the urethra or bladder
- stricture, a narrowing of the urethra—a possible sign of an enlarged prostate in men or of scar tissue in the urethra
- secondary signs of obstruction (or blockage), such as an enlarged prostate gland
- other congenital or acquired abnormalities such as duplicated ureters, ureterocele, or diverticulum
During a cystoscopy, a urologist can sometimes treat problems, such as bleeding in the bladder and blockage in the urethra. A urologist may also use a cystoscopy to
- remove a stone in the bladder or urethra
- remove or treat abnormal tissue and tumors
- take a sample of the urethra or bladder tissue for a biopsy
- inject material into the wall of the urethra to treat urinary leakage or prevent vesicoureteral reflux
- inject medicines into the bladder to treat urinary leakage
- obtain urine samples from the ureters
- perform retrograde pyelography—an x-ray procedure in which a urologist injects a special dye into the urinary tract to create images of urinary flow, to show obstructions such as kidney stones and tumors
- remove a stent that was placed in the ureter after a ureteroscopy with biopsy or stone removal
Why do health care professionals perform ureteroscopy?
A urologist performs a ureteroscopy to find the cause of urine blockage in a ureter or to evaluate other problems inside the ureters or kidneys. During a ureteroscopy, a urologist can see
- a stone in a ureter or kidney
- problematic tissue, tumors, or cancer in a ureter or in the lining of a kidney
During a ureteroscopy, a urologist can treat problems such as urine blockage in a ureter. The urologist can also
- remove a stone from a ureter or kidney
- remove or treat abnormal tissue and tumors
- take a sample of ureter or kidney tissue for a biopsy
How do I prepare for a cystoscopy or ureteroscopy?
Your urologist will ask about your medical history to determine whether you need a cystoscopy or ureteroscopy. You may need to give a urine sample to test for a UTI. If you have a UTI, you may need to take antibiotics before either procedure.
Your urologist will also ask about any medicines you are taking, ask if you have any allergies, talk about anesthesia, give instructions for what to do before the procedure, and discuss what to expect afterward. In some cases, you won’t need special preparations for a cystoscopy. In other cases, your instructions may include
- when to stop certain medicines, such as blood thinners
- when to stop eating and drinking or, conversely, when to drink plenty of liquids
- when to empty your bladder before the procedure
- whether to arrange for a ride home after the procedure
 To prepare for a cystoscopy or ureteroscopy, your urologist will talk with you about anesthesia, give you instructions for what to do before the procedure, and discuss what to expect afterward.
To prepare for a cystoscopy or ureteroscopy, your urologist will talk with you about anesthesia, give you instructions for what to do before the procedure, and discuss what to expect afterward.How do health care professionals perform cystoscopy or ureteroscopy?
A urologist can perform your cystoscopy during an office visit, in an outpatient center, or at a hospital. Ureteroscopies are usually performed in an operating room under anesthesia. A simple exploratory procedure takes about 15 to 30 minutes, including preparation. The procedure can be longer if your urologist performs additional work like taking a biopsy or removing stones from the bladder or ureters.
An anesthetic gel may be applied around the urethral opening, or a local anesthetic may be injected into the urethra.
Sedatives and general anesthesia are often given for a
- ureteroscopy
- cystoscopy with biopsy
- cystoscopy to inject material into the wall of the urethra or ureters
- cystoscopy to inject medicine into the bladder
Sedation helps you relax and be comfortable. General anesthesia puts you into a deep sleep during the procedure.
The health care team will monitor your vital signs and make you as comfortable as possible.
The urologist will position you and make sure the anesthesia is working. The urologist will then gently insert the cystoscope into your urethra and slowly guide it to the bladder. A sterile liquid called saline will be used to slowly fill the bladder, so the urologist has a better view of the bladder wall. As the bladder fills with liquid, you may feel some discomfort and the urge to urinate. The urologist may remove some of the liquid from the bladder during the procedure.
During a cystoscopy, the urologist will examine the lining of the urethra and bladder and may insert small instruments through the cystoscope to treat problems in the urethra and bladder or perform a biopsy.
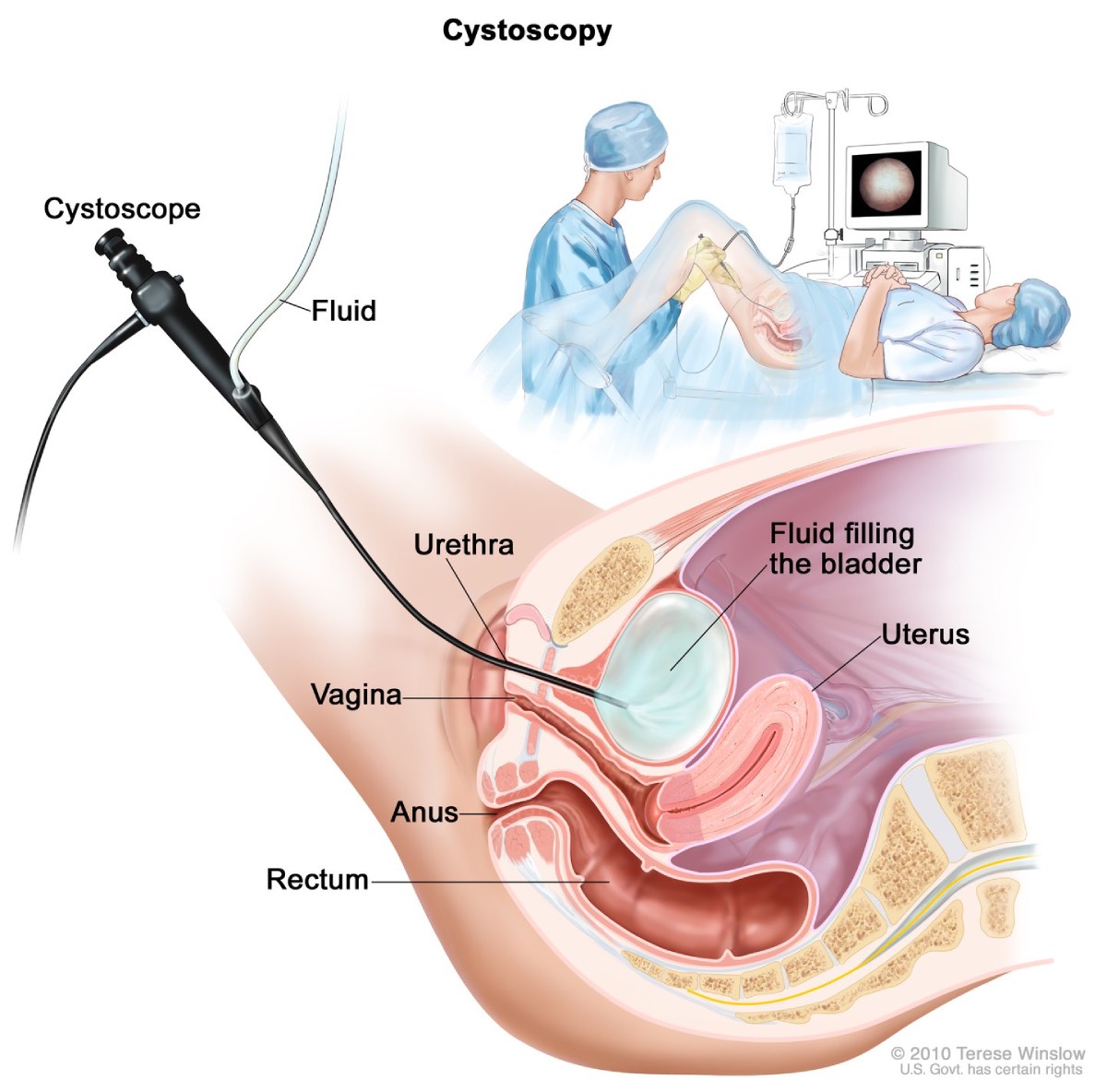 During a cystoscopy, a cystoscope is inserted through the urethra into the bladder.
During a cystoscopy, a cystoscope is inserted through the urethra into the bladder.During a ureteroscopy, the urologist will focus on viewing the ureter and lining of the kidney, known as the renal pelvis. The urologist may also insert small instruments through the ureteroscope to treat problems in the ureter or kidney, perform a biopsy, or cauterize a bleeding area.
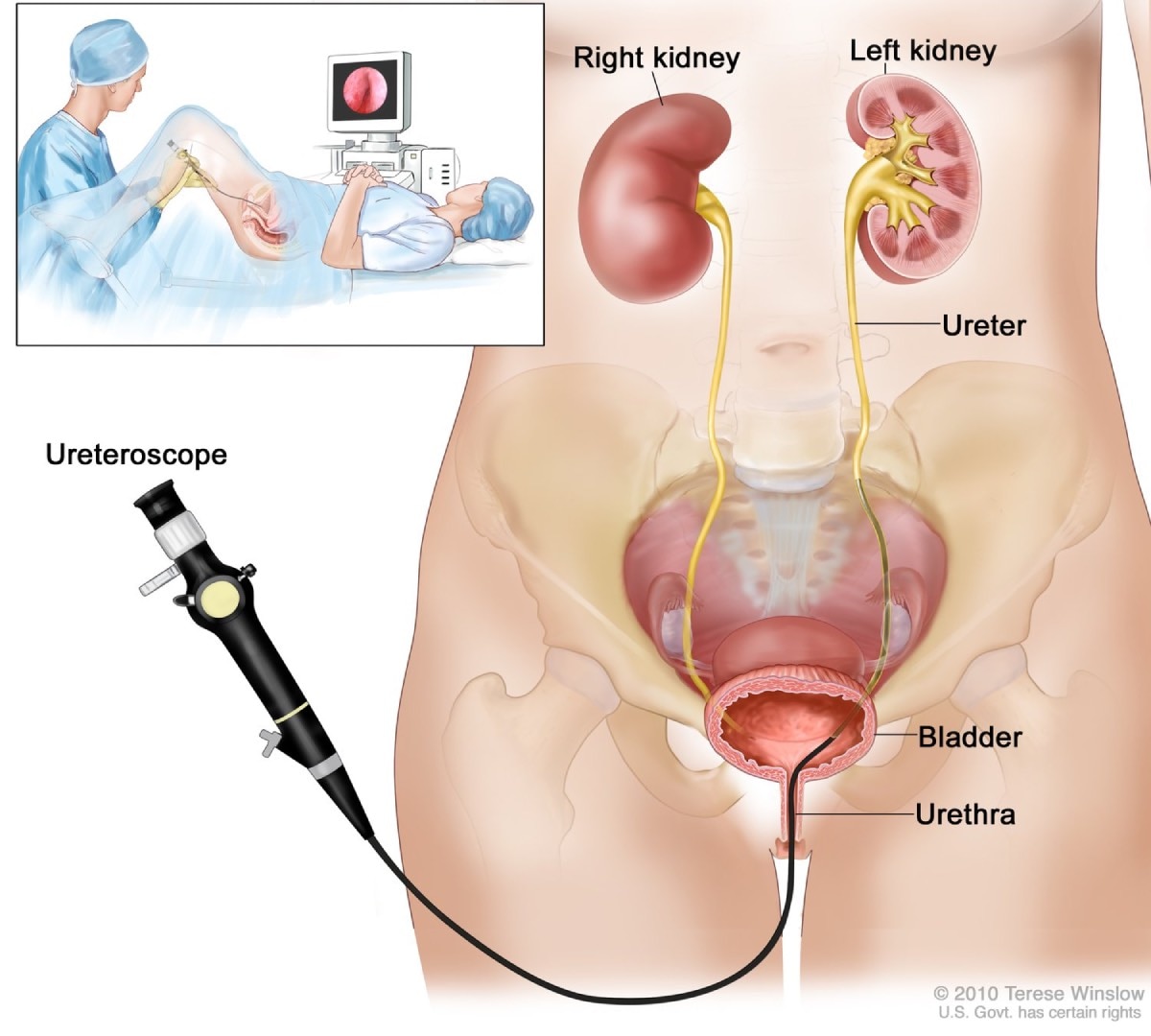 During a ureteroscopy, a ureteroscope is inserted through the urethra and into the ureter.
During a ureteroscopy, a ureteroscope is inserted through the urethra and into the ureter.After either procedure, the urologist may remove the liquid from the bladder, or you may empty your bladder.
What should I expect after a cystoscopy or ureteroscopy?
You will be able to go home after almost any cystoscopy performed in an outpatient office setting. If it is performed in an operating room, you will most likely go home the same day as the procedure, depending on what type of anesthesia you receive. If you receive general anesthesia, you may have to wait 1 to 4 hours before going home. In some cases, you may need to stay overnight in the hospital.
Before leaving, try to use the restroom to make sure you can urinate. You’ll be given discharge instructions for rest, driving, and physical activities after the procedure.
Depending on your procedure and what was done, you may
- have a mild burning feeling when urinating
- see small amounts of blood in the urine
- have mild discomfort in the bladder area or kidney area when urinating
- need to urinate more frequently or urgently
These problems should not last more than 24 hours. Tell a health care professional right away if bleeding or pain is severe, if you cannot urinate, or if problems last more than a day.
Once you are at home, your health care professional may recommend you
- drink 16 ounces of water each hour for a few hours after the procedure
- take a warm bath to relieve any burning feeling
- hold a warm, damp washcloth over the urethral opening to relieve discomfort
- take an over-the-counter pain reliever
- take an antibiotic for 1 or 2 days to prevent an infection
If you had a ureteroscopy and needed a temporary stent placed in the ureter to drain urine while swelling goes away, the stent may cause some pain, discomfort in the kidney or bladder area, or the need to urinate frequently and urgently. The discomfort is generally mild. However, these sensations may be present during the entire time you have the stent. The stent may be left in the ureter for a few days to a week or more. Your urologist may need to perform a cystoscopy to remove the stent in the ureter.
What are the risks of cystoscopy and ureteroscopy?
The risks of cystoscopy and ureteroscopy include
- UTIs
- abnormal bleeding
- abdominal pain or a burning feeling or pain while urinating
- the inability to urinate swelling
- injury to the urethra, bladder, or ureters
- urethral narrowing due to scar tissue formation
- complications from anesthesia
Seek care right away
After a cystoscopy or ureteroscopy, call or see a health care professional right away if you
- can’t urinate and feel like your bladder is full
- have burning or painful urination that lasts more than 2 days
- see bright red urine or blood clots in the urine
- have a fever, with or without chills
- feel severe discomfort
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
The NIDDK would like to thank:
Brian T. Helfand M.D., Ph.D., NorthShore University HealthSystem

