Research Updates
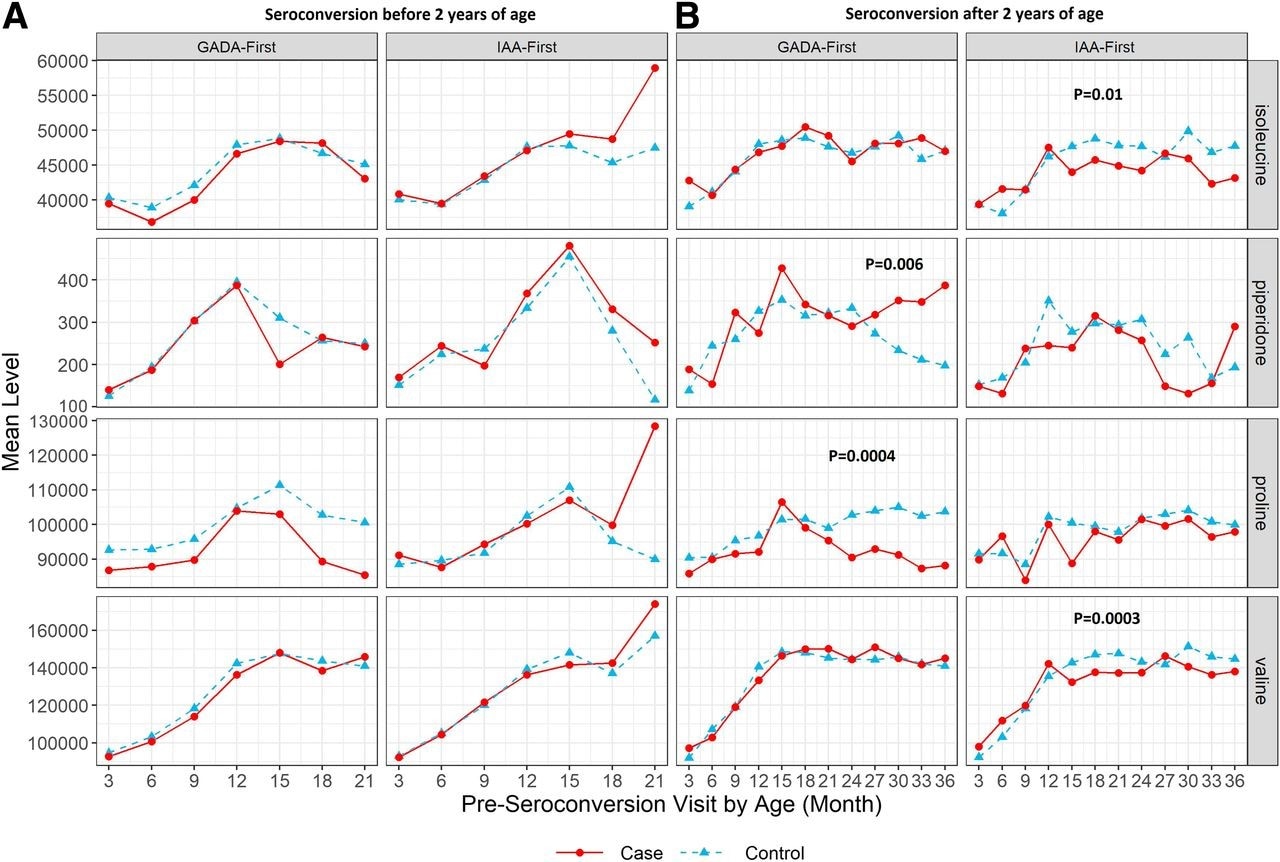
Researchers identify metabolite patterns in children that predict type 1 diabetes autoimmunity: Children at increased genetic risk for type 1 diabetes may have unique metabolomic profiles and biomarkers that could predict whether they will later develop antibodies to pancreatic islet cells. In a study of 2,062 children participating in The Environmental Determinants of Diabetes in the Young (TEDDY) study, the research team examined the patterns of 144 amino acid metabolites and 213 fatty acids in blood plasma samples collected from participants every three months from birth to age 4. The researchers found unique patterns of amino acids and lipids in children who later developed islet autoantibodies compared to those who did not. Additionally, they observed differences that were associated with the types of antibodies that developed first, and when they developed. This research was published in Diabetes in March.
NIDDK research explores role of microbiome in nutrient absorption: Investigators from the NIDDK Phoenix Epidemiology and Clinical Research Branch and their collaborators have found the first evidence in humans, based on directly measured calories, that the gut microbiome has a measurable role in metabolizing nutrients. The small, two-part study involved a controlled feeding study and a double-blind placebo-controlled trial with an antibiotic to alter the microbiome. The team found that participants lost more calories through stool during periods of underfeeding and when taking the antibiotic. The team also observed an increase in the gut bacterium Akkermansia muciniphila under the same conditions. These results suggest that the interventions caused changes in the gut microbiome that limited its ability to metabolize calories and harvest nutrients for the body. This research was published in Nature Medicine in March.
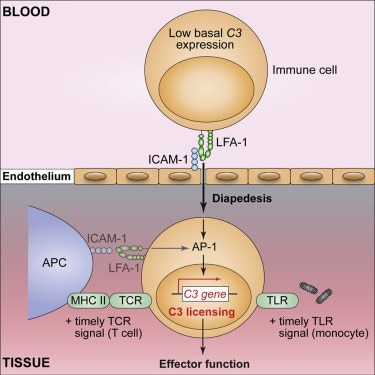
NIDDK-supported research identifies a biomarker of severity in autoimmunity: Researchers from the NIDDK Kidney Diseases Branch and collaborators discovered that the protein C3 plays a critical role in the function of immune cells in tissues. In one experiment using fluids from joint cavities of people with rheumatoid arthritis, researchers found that the more C3 produced by immune cells in the fluid, the more severe the inflammatory response. The team also studied participants with a rare immunodeficiency that causes recurrent infections and found that immune cells from these participants had a weakened inflammatory response and disruption of the transcription process resulting in higher levels of the C3 protein. The inflammatory response was improved by correcting the C3 levels within the cells. The results show that targeting the regulation of C3 and similar proteins in immune cells could help with treatment of autoimmune or inflammatory diseases. This research was published in Immunity in March.
NIDDK study explores differences in thermal biology between mice and humans: Scientists in NIDDK’s Diabetes, Endocrinology, and Obesity Branch found that mice have fundamentally different thermal physiology than humans - a discovery that could improve the use of mice as a model of human disease. In this study, the research team continuously monitored body temperature and metabolic rate in various mouse models at different environmental temperatures. They found that mice have only a discrete temperature, called a thermoneutral point, in which they can maintain their core body temperature without raising their metabolic rate. In contrast, humans have a broad thermoneutral zone. The results suggest that studying mice strictly at thermoneutrality is not possible, and that researchers should take the thermogenic characteristics of mouse models into account when planning studies. The findings were published in Cell Reports in April.

