Gallstones
Return to Overview PageDefinition & Facts
In this section:
- What are gallstones?
- Do gallstones have another name?
- What is the biliary tract?
- How common are gallstones?
- Who is more likely to develop gallstones?
- What are the complications of gallstones?
What are gallstones?
Gallstones are hard, pebble-like pieces of material, usually made of cholesterol or bilirubin, that form in your gallbladder. Gallstones can range in size from a grain of sand to a golf ball. The gallbladder can make one large gallstone, hundreds of tiny stones, or both small and large stones.
When gallstones block the bile ducts of your biliary tract, the gallstones can cause sudden pain in your upper right abdomen. This pain is called a gallbladder attack, or biliary colic. If your symptoms continue and they’re left untreated, gallstones can cause serious complications.
However, most gallstones don’t cause blockages and are painless, also called “silent” gallstones. Silent gallstones usually don’t need medical treatment.
Types of gallstones
The two main types of gallstones are
- cholesterol stones
- pigment stones
Cholesterol stones are usually yellow-green in color and are made of mostly hardened cholesterol. In some countries, cholesterol stones make up about 75 percent of gallstones.1
Pigment stones are dark in color and are made of bilirubin. Some people have a mix of both kinds of stones.

Do gallstones have another name?
Cholelithiasis is the name doctors sometimes call gallstones.
What is the biliary tract?
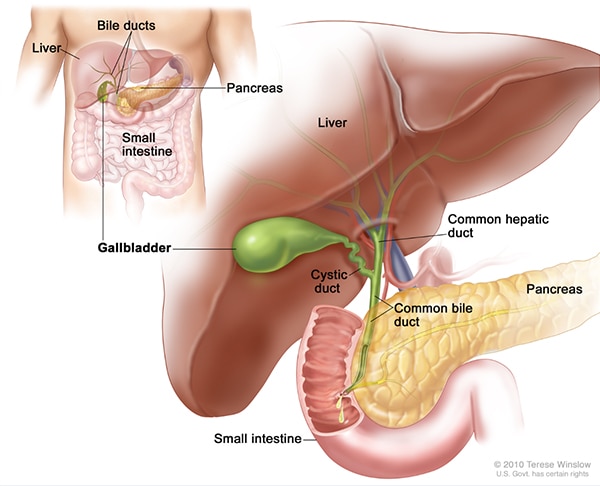
Your biliary tract, which is made up of your gallbladder and bile ducts, helps with digestion by releasing bile.
The gallbladder is a small, pear-shaped organ that stores bile and is located in your upper right abdomen, below your liver.
The bile ducts of your biliary tract include the hepatic ducts, common bile duct, and cystic duct. Bile ducts also carry waste and digestive juices from the liver and pancreas to the duodenum.
Your liver produces bile, which is mostly made of cholesterol, bile salts, and bilirubin. Your gallbladder stores the bile until it’s needed. When you eat, your body signals your gallbladder to empty bile into your duodenum to mix with food. The bile ducts carry the bile from your gallbladder to the duodenum.
How common are gallstones?
Gallstones are very common, affecting 10 to 15 percent of the U.S. population, which is almost 25 million people. About a quarter of the nearly 1 million people diagnosed with gallstones each year will need to be treated, usually with surgery.2
Who is more likely to develop gallstones?
Certain groups of people have a higher risk of developing gallstones than others.3
- Women are more likely to develop gallstones than men. Women who have extra estrogen in their body due to pregnancy, hormone replacement therapy, or birth control pills may be more likely to produce gallstones.
- Older people are more likely to develop gallstones. As you age, the chance that you’ll develop gallstones becomes higher.
- People with a family history of gallstones have a higher risk.
- American Indians have genes that raise the amount of cholesterol in their bile, and have the highest rate of gallstones in the United States.
- Mexican Americans are also at higher risk of developing gallstones.

People with certain health conditions
You are more likely to develop gallstones if you have one of the following health conditions:
- cirrhosis, a condition in which your liver slowly breaks down and stops working due to chronic, or long-lasting, injury
- infections in the bile ducts, which can also be a complication of gallstones
- hemolytic anemias, conditions in which red blood cells are continuously broken down, such as sickle cell anemia
- some intestinal diseases that affect normal absorption of nutrients, such as Crohn’s disease
- high triglyceride levels
- low HDL cholesterol
- metabolic syndrome, which can also raise the risk of gallstone complications
- diabetes and insulin resistance
People with diet- and weight-related health concerns
You are more likely to develop gallstones if you
- have obesity, especially if you are a woman
- have had fast weight loss, like from weight-loss surgery, also called metabolic and bariatric surgery
- have been on a diet high in calories and refined carbohydrates and low in fiber
Learn more about dieting and gallstones.
What are the complications of gallstones?
Complications of gallstones can include
- inflammation of the gallbladder
- severe damage to or infection of the gallbladder, bile ducts, or liver
- gallstone pancreatitis, which is inflammation of the pancreas due to a gallstone blockage
Many people do not have symptoms of gallstones until they have complications.
If left untreated, gallstones can be deadly. Treatment for gallstones usually involves gallstone surgery.
References
Symptoms & Causes
What are the symptoms of gallstones?
If gallstones block your bile ducts, bile could build up in your gallbladder, causing a gallbladder attack, sometimes called biliary colic. Gallbladder attacks usually cause pain in your upper right abdomen, sometimes lasting several hours. Gallbladder attacks often follow heavy meals and usually occur in the evening or during the night. If you’ve had one gallbladder attack, more attacks will likely follow.
Gallbladder attacks usually stop when gallstones move and no longer block the bile ducts. However, if any of your bile ducts stay blocked for more than a few hours, you may develop gallstone complications. Gallstones that do not block your bile ducts do not cause symptoms.
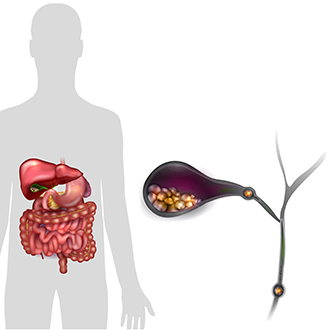
Silent gallstones
Most people with gallstones do not have symptoms. Gallstones that do not cause symptoms are called silent gallstones. Silent gallstones don’t stop your gallbladder, liver, or pancreas from working, so they do not need treatment.
Seek care right away for a gallbladder attack
See a doctor right away if you are having these symptoms during or after a gallbladder attack:
- pain in your abdomen lasting several hours
- nausea and vomiting
- fever—even a low-grade fever—or chills
- yellowish color of your skin or whites of your eyes, called jaundice
- tea-colored urine and light-colored stools
These symptoms may be signs of a serious infection or inflammation of the gallbladder, liver, or pancreas. Gallstone symptoms may be similar to symptoms of other conditions, such as appendicitis, ulcers, pancreatitis, and gastroesophageal reflux disease, all of which should be treated by a doctor as soon as possible.
Gallstone complications can occur if your bile ducts stay blocked. Left untreated, blockages of the bile ducts or pancreatic duct can be fatal.
What causes gallstones?
Gallstones may form if bile contains too much cholesterol, too much bilirubin, or not enough bile salts. Researchers do not fully understand why these changes in bile occur. Gallstones also may form if the gallbladder does not empty completely or often enough. Certain people are more likely to have gallstones than others because of their risk factors for gallstones, including obesity and certain kinds of dieting.
Dieting
In this section:
- How does weight affect gallstones?
- How does my fast weight loss affect gallstones?
- Is weight cycling a problem?
- How can I safely lose weight to lower my chances of getting gallstones?
How does weight affect gallstones?
Being overweight or having obesity may make you more likely to develop gallstones, especially if you are a woman. Researchers have found that people who have obesity may have higher levels of cholesterol in their bile, which can cause gallstones. People who have obesity may also have large gallbladders that do not work well. Some studies have shown that people who carry large amounts of fat around their waist may be more likely to develop gallstones than those who carry fat around their hips and thighs.
Losing weight very quickly may raise your chances of forming gallstones, however. Talk with your health care professional about how to lose weight safely.
How does my fast weight loss affect gallstones?
When you don’t eat for a long period of time or you lose weight quickly, your liver releases extra cholesterol into the bile. Fast weight loss can also prevent the gallbladder from emptying properly. Weight-loss surgery, also called metabolic and bariatric surgery, may lead to fast weight loss and higher risk of gallstones.
Your chances of developing gallstones may depend on the type of weight-loss treatment you choose. Diets or surgeries that cause fast weight loss may be more likely to lead to gallstone problems than diets or surgeries that lead to slower weight loss. If you have silent gallstones, you may also be more likely to develop gallstone symptoms.
Several factors may raise your chances of having problems with gallstones after weight-loss surgery or a very low-calorie diet. These factors include
- gallstones that you had before your weight-loss surgery or before you went on a very low-calorie diet, especially if the stones caused symptoms
- a large amount of extra weight before you have weight-loss surgery or go on a very low-calorie diet
- very quick weight loss after the surgery or a very low-calorie diet
If you are starting a very low-calorie diet or having weight-loss surgery, talk with your doctor about how to lower your chances of developing gallstones. The medicine ursodiol can help prevent gallstones in people who lose weight rapidly through very low-calorie diets or weight-loss surgery.

Is weight cycling a problem?
Weight cycling, or losing and regaining weight repeatedly, may also lead to gallstones. The more weight you lose and regain during a cycle, the greater your chances of developing gallstones.
Stay away from "crash diets" that promise to help you drop the pounds quickly. Aim for losing weight at a slower pace and keeping it off over time.
How can I safely lose weight to lower my chances of getting gallstones?
Losing weight at a slow pace may make it less likely that you will develop gallstones. For people who are overweight or have obesity, experts recommend beginning with a weight loss of 5 to 10 percent of your starting weight over a period of 6 months.4 In addition, weight loss may bring you other benefits such as better mood, more energy, and positive self-image.
When making healthy food choices to help you lose weight, you can choose food that may also lower your chances of developing gallstones.
Regular physical activity, which will improve your overall health, may also lower your chances of developing gallstones. To improve health or prevent weight gain, aim for at least 150 minutes a week of moderate-intensity physical activity, like brisk walking or fast dancing. Adults also need muscle-strengthening activity, like lifting weights or doing push-ups, at least 2 days a week.5
Talk with your doctor before you start an eating and physical activity plan to improve your health or maintain your weight loss. View weight management resources from the NIDDK.
References
Diagnosis
How do doctors diagnose gallstones?
Doctors use your medical history, a physical exam, and lab and imaging tests to diagnose gallstones.
A health care professional will ask you about your symptoms. He or she will ask if you have a history of health conditions or health concerns that make you more likely to get gallstones. The health care professional also may ask if you have a family history of gallstones and what you typically eat. During a physical exam, the health care professional examines your body and checks for pain in your abdomen.

What tests do health care professionals use to diagnose gallstones?
Health care professionals may use lab or imaging tests to diagnose gallstones.
Lab tests
A health care professional may take a blood sample from you and send the sample to a lab to test. The blood test can show signs of infection or inflammation of the bile ducts, gallbladder, pancreas, or liver.
Imaging tests
Health care professionals use imaging tests to find gallstones. A technician performs these tests in your doctor’s office, an outpatient center, or a hospital. A radiologist reads and reports on the images. You usually don’t need anesthesia or a medicine to keep you calm for most of these tests. However, a doctor may give you anesthesia or a medicine to keep you calm for endoscopic retrograde cholangiopancreatography (ERCP).
Ultrasound. Ultrasound is the best imaging test for finding gallstones. Ultrasound uses a device called a transducer, which bounces safe, painless sound waves off your organs to create an image or picture of their structure. If you have gallstones, they will be seen in the image. Sometimes, health care professionals find silent gallstones when you don’t have any symptoms.
Computed tomography (CT) scan. CT scans use a combination of x-rays and computer technology to create images of your pancreas, gallbladder, and bile ducts. CT scans can show gallstones, or complications such as infection and blockage of the gallbladder or bile ducts. However, CT scans also can miss gallstones that you may have.
Magnetic resonance imaging (MRI). MRI machines use radio waves and magnets to produce detailed images of your organs and soft tissues without x-rays. MRIs can show gallstones in the ducts of the biliary tract.
Cholescintigraphy. Cholescintigraphy—also called a hydroxyl iminodiacetic acid scan, HIDA scan, or hepatobiliary scan—uses a safe radioactive material to produce pictures of your biliary tract. You’ll lie on a table while a health care professional injects a small amount of the radioactive material into a vein in your arm. The health care professional may also inject a substance that causes your gallbladder to squeeze. A special camera takes pictures of the radioactive material as it moves through your biliary tract. Doctors use cholescintigraphy to diagnose abnormal contractions of your gallbladder or a blockage in the bile ducts.
Endoscopic retrograde cholangiopancreatography (ERCP). ERCP combines upper gastroendoscopy and x-rays to treat problems of your bile and pancreatic ducts. ERCP helps the health care professional locate the affected bile duct and the gallstones. This test is more invasive—or involves more instruments inside your body—than other tests. Doctors use it selectively, usually to remove a gallstone that is stuck in the common bile duct.
Treatment
How do health care professionals treat gallstones?
If your gallstones are not causing symptoms, you probably don’t need treatment. However, if you are having a gallbladder attack or other symptoms, contact your doctor. Although your symptoms may go away, they may appear again and you may need treatment. Your doctor may refer to you a gastroenterologist or surgeon for treatment.
The usual treatment for gallstones is surgery to remove the gallbladder. Doctors sometimes can use nonsurgical treatments to treat cholesterol stones, but pigment stones usually require surgery.
Surgery
Surgery to remove the gallbladder, called cholecystectomy, is one of the most common operations performed on adults in the United States. The gallbladder is not an essential organ, which means you can live normally without a gallbladder.
A health care professional will usually give you general anesthesia for surgery. Once the surgeon removes your gallbladder, bile flows out of your liver through the hepatic duct and common bile duct and directly into the duodenum, instead of being stored in the gallbladder.
Surgeons perform two types of cholecystectomy:
Laparoscopic cholecystectomy. Almost all surgeons perform cholecystectomies with laparoscopy. Surgeons perform many laparoscopic cholecystectomies on an outpatient basis, meaning you may be able to go home the same day. You will probably be able to return to normal physical activity in about a week.
Open cholecystectomy. A surgeon performs an open cholecystectomy when your gallbladder is severely inflamed, infected, or scarred from other operations. Your doctor may perform a cholecystectomy if problems occur during a laparoscopic cholecystectomy. After the surgery, you may need to stay in the hospital for up to a week. You will probably be able to return to normal physical activity after about a month.
What happens after gallbladder removal?
A small number of people have softer and more frequent stools after gallbladder removal, because bile now flows into your duodenum more often. Changes in bowel habits are usually temporary; however, discuss them with your doctor.
All surgeries come with a possible risk of complications; however, gallbladder surgery complications are very rare. The most common complication is injury to the bile ducts, which can cause infection. You may need one or more additional operations to repair the bile ducts.
Nonsurgical treatments
Doctors use nonsurgical treatments for gallstones only in special situations, like if you have cholesterol stones and you have a serious medical condition that prevents surgery. Even with treatment, gallstones can return. Therefore, you may have to be regularly treated for gallstones for a very long time, or even for the rest of your life.
A doctor may use the following types of nonsurgical treatments to remove or break up cholesterol gallstones:
Endoscopic retrograde cholangiopancreatography (ERCP). Sometimes doctors use ERCP to remove a gallstone that is stuck in the common bile duct.
Oral dissolution therapy. Ursodiol (Actigall) and chenodiol (Chenix) are medicines that contain bile acids that can break up gallstones. These medicines work best to break up small cholesterol stones. You may need months or years of treatment to break up all stones.
Shock wave lithotripsy. A doctor can use shock wave lithotripsy to blast gallstones into small pieces. Doctors use this procedure only rarely, and sometimes along with ursodiol.
How can I help prevent gallstones?
You can help prevent gallstones by
- adjusting your eating plan to include more foods high in fiber and healthy fats, fewer refined carbohydrates, and less sugar
- losing weight safely if you are overweight or have obesity
- maintaining a healthy weight through healthy eating and regular physical activity
Eating, Diet, & Nutrition
Can what I eat help prevent gallstones?
You can lower your risk of gallstones by following a healthy eating plan and getting regular physical activity to help you reach and maintain a healthy weight.
Experts recommend the following to help prevent gallstones:
- Eat more foods that are high in fiber, such as
- fruits, vegetables, beans, and peas.
- whole grains, including brown rice, oats, and whole wheat bread.
- Eat fewer refined carbohydrates and less sugar.
- Eat healthy fats, like fish oil and olive oil, to help your gallbladder contract and empty on a regular basis.
- Avoid unhealthy fats, like those often found in desserts and fried foods.

Talk with your health care professional before you make any changes to your eating plan. Losing weight too quickly may cause health problems. Very low-calorie diets and weight-loss surgery, also called metabolic and bariatric surgery, can lead to rapid weight loss and raise your risk of gallstones. Learn more about weight-loss, dieting, and gallstones.
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
