Cirrhosis
Return to Overview PageDefinition & Facts
In this section:
- What is cirrhosis?
- How common is cirrhosis?
- Who is more likely to develop cirrhosis?
- What are the complications of cirrhosis?
What is cirrhosis?
Cirrhosis is a condition in which the liver is scarred and permanently damaged. Scar tissue replaces healthy liver tissue and prevents the liver from working normally. Scar tissue also partly blocks the flow of blood through the liver. As cirrhosis gets worse, the liver begins to fail.
Many people are not aware they have cirrhosis, because they may not have any signs or symptoms until their liver is badly damaged.
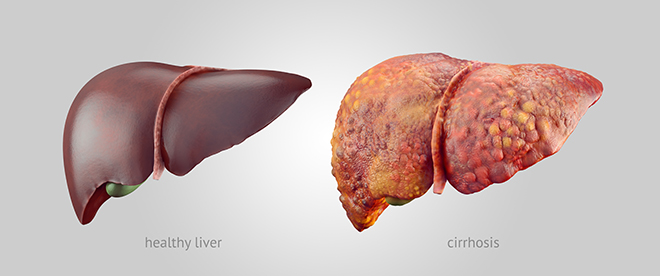 A healthy liver (left) and a liver with cirrhosis (right).
A healthy liver (left) and a liver with cirrhosis (right).How common is cirrhosis?
Researchers estimate that about 1 in 400 adults in the United States have cirrhosis.1 Researchers believe the actual numbers may be higher than that because many people with cirrhosis are not diagnosed. Many people with early stages of cirrhosis may not be diagnosed if they have few symptoms or do not feel ill.
Who is more likely to develop cirrhosis?
People are more likely to develop cirrhosis if they have health conditions that can cause cirrhosis. Cirrhosis is also more common in people who
- have a history of heavy alcohol use
- have overweight or obesity
- have type 2 diabetes
- are men
- are age 40 or older2
What are the complications of cirrhosis?
As the liver fails, complications may develop. In some people, complications may be the first sign they have cirrhosis.
Portal hypertension
Portal hypertension is a serious problem caused by cirrhosis and can lead to some of the most common complications of cirrhosis. Portal hypertension occurs when scar tissue in the liver slows the normal flow of blood, which causes high blood pressure in the portal vein. The portal vein is the large blood vessel that carries blood from the stomach, intestines, spleen, gallbladder, and pancreas to the liver.
When portal hypertension reaches a certain level, it can cause complications, such as
- buildup of fluid in the abdomen or belly, called ascites. Ascites can lead to a serious infection—called peritonitis —in the space that surrounds the liver and intestines.
- swelling in the legs, ankles, or feet, called edema.
- enlarged veins—called varices—in the esophagus, stomach, or intestines. These varices can lead to internal bleeding if the veins burst.
- confusion or difficulty thinking caused by a buildup of toxins in the brain, called hepatic encephalopathy.
Infections
Cirrhosis increases your chance of getting bacterial infections, such as urinary tract infections and pneumonia.
Liver cancer
Cirrhosis increases the chance of getting liver cancer.3 Most people who develop liver cancer already have cirrhosis.
Liver failure
Cirrhosis may eventually lead to liver failure, also called end-stage liver disease. With liver failure, the liver is badly damaged and stops working. People with liver failure may require a liver transplant.
Other complications
Other complications of cirrhosis may include
- bone diseases, such as osteoporosis
- gallstones
- problems with the bile ducts—the tubes that carry bile out of the liver
- malabsorption and malnutrition
- bruising and bleeding easily
- falls
- sensitivity to medicines
- insulin resistance and type 2 diabetes
References
Symptoms & Causes
What are the symptoms of cirrhosis?
You may have no symptoms in the earliest stage of cirrhosis. Symptoms of cirrhosis may not appear until the liver is badly damaged.
Early symptoms of cirrhosis may include
- feeling tired or weak
- itching of the skin
- poor appetite
- losing weight without trying
- nausea and vomiting
- mild pain or discomfort over the liver in the upper right side of the abdomen, or belly
- muscle loss and weakness
- muscle cramps
- sexual problems
As liver function gets worse, people with cirrhosis may have other symptoms, including
- bruising and bleeding easily
- confusion, difficulty thinking, memory loss, personality changes, or sleep disorders
- internal bleeding due to the bursting of enlarged veins—called varices—in the esophagus, stomach, or intestines
- swelling in the lower legs, ankles, or feet, called edema
- swelling of the abdomen from a buildup of fluid, called ascites
- severe itchy skin
- darkening of the color of the urine
- yellowish tint to the whites of the eyes and skin, called jaundice
What causes cirrhosis?
Cirrhosis has different causes. Some people with cirrhosis have more than one cause of liver damage. For some people, the cause of cirrhosis is not known.
Most common causes
The most common causes of cirrhosis are
- alcohol-associated liver disease, which is damage to the liver and its function from drinking too much alcohol
- buildup of fat in the liver, called nonalcoholic fatty liver disease, which is more common in people with overweight, obesity, or other diseases or health conditions such as metabolic syndrome or type 2 diabetes
- long-term, or chronic, infection with the hepatitis C or hepatitis B viruses
These health conditions don’t affect every person in the same way. Some people with these health conditions may have more liver damage than others. Research suggests that certain inherited genes affect how much these conditions damage the liver.
Less common causes
Some less common causes of cirrhosis include
- autoimmune hepatitis, a disease in which the immune system attacks the liver
- diseases that damage, destroy, or block bile ducts, such as primary biliary cholangitis and primary sclerosing cholangitis
- inherited liver diseases—diseases passed from parents to children through genes that affect how the liver works—such as Wilson disease, hemochromatosis, and alpha-1 antitrypsin deficiency
- long-term use of certain medicines and high doses of vitamin A daily
- chronic heart failure with liver congestion, a condition in which blood flow out of the liver is slowed
Diagnosis
How do doctors diagnose cirrhosis?
If your doctor suspects that you have cirrhosis, they may make a diagnosis based on your medical history, a physical exam, and the results of blood tests and imaging tests.
Family and medical history
 Your doctor will ask if you have a history of alcohol use or health conditions
that increase the risk of developing cirrhosis.
Your doctor will ask if you have a history of alcohol use or health conditions
that increase the risk of developing cirrhosis.Your doctor may ask about your symptoms and whether you have a history of health conditions that increase the risk of developing cirrhosis.
When taking your medical history, your doctor may ask about
- any recent changes in weight or appetite
- alcohol use
- prescription and over-the-counter medicines or herbal supplements you take
Your doctor may also ask if you have a family history of health conditions, including liver conditions.
Physical exam
In a physical exam, your doctor will
- look for jaundice, or a yellowish tint to the whites of your eyes and skin
- check your skin for rashes and legs for swelling
- use a stethoscope to listen to your heart, lungs, and abdomen—or belly
- tap or press on different areas of your abdomen to check for swelling or tenderness
- check to see if your liver has become larger
- check your outstretched hands for tremor
What tests do doctors use to diagnose cirrhosis?
Blood tests
 Your doctor can use blood tests to tell how serious cirrhosis is.
Your doctor can use blood tests to tell how serious cirrhosis is.Your doctor may recommend the following blood tests
- liver tests that can show if liver enzyme levels are higher or lower than normal, which may be a sign of liver damage. Your doctor may suspect cirrhosis if you have
- complete blood count, which can show signs of infection and anemia that may be caused by internal bleeding.
- tests for viral infections to see if you have hepatitis B or hepatitis C.
- tests for autoimmune liver conditions, which include the anti-nuclear antibody (ANA), anti-smooth muscle antibody (SMA), and anti-mitochondrial antibody (AMA) tests.
Based on the blood test results, your doctor may be able to diagnose certain causes of cirrhosis.
Your doctor can use blood tests to tell how serious cirrhosis is.
Imaging tests
Imaging tests can show the size, shape, and texture of the liver and show how much fat is in the liver. Some tests can also measure the stiffness of the liver. Cirrhosis increases liver stiffness. Your doctor may use one or more of the following imaging tests
- ultrasound uses a hand-held device, called a transducer, that bounces safe, painless sound waves off organs to create an image of their structure.
- magnetic resonance imaging (MRI) uses radio waves and magnets to produce detailed images of organs and soft tissues without using x-rays.
- x-ray tests, such as computed tomography (CT) scans, use a combination of x-rays and computer technology to create images of the liver.
- elastography, a special test that measures the stiffness of the liver. An increase in liver stiffness may be a sign of fibrosis, or scarring. Your doctor can use stiffness measures to see if you may have cirrhosis and whether liver scarring is getting better or worse.
Liver biopsy
Your doctor may perform a liver biopsy to see how much scarring is in your liver. A liver biopsy can diagnose cirrhosis when the results of other tests are uncertain. The biopsy may also help your doctor identify the cause of cirrhosis and determine whether you need treatment.
During a liver biopsy, a doctor will use a needle to take small pieces of tissue from the liver. A pathologist will examine the tissue under a microscope.
Treatment
In this section:
- How do doctors treat cirrhosis?
- How do doctors treat the causes of cirrhosis?
- How do doctors treat the complications of cirrhosis?
- What can I do to help keep my cirrhosis from getting worse?
- When do doctors consider a liver transplant for cirrhosis?
How do doctors treat cirrhosis?
Doctors do not have specific treatments that can cure cirrhosis and reverse damage to the liver. However, treating the causes of cirrhosis may prevent cirrhosis or slow the liver damage. Treating the complications of cirrhosis may keep them from getting worse and prevent liver failure.
How do doctors treat the causes of cirrhosis?
To treat the causes of cirrhosis, doctors often recommend lifestyle changes or prescribe medicines to prevent more liver damage. Doctors may recommend that people with cirrhosis stop activities, such as drinking alcohol and taking certain medicines, that may have caused cirrhosis or can make cirrhosis worse. For people who have cirrhosis and have overweight or obesity, doctors may recommend trying to lose weight.
Treatment of alcohol-associated liver disease
For people who have alcohol-associated liver disease, or damage to the liver and its function from drinking too much alcohol, doctors will recommend that they completely stop drinking alcohol and may refer them for alcohol treatment.
Treatment of nonalcoholic fatty liver disease
To treat nonalcoholic fatty liver disease (NAFLD), doctors may recommend weight loss. For people who have overweight or obesity and NAFLD, weight loss can help reduce fat in the liver, inflammation, and scarring. Some people with cirrhosis can lose weight through healthy meal planning and regular physical activity, and doctors sometimes recommend additional weight-loss treatments such as medicines or surgery.
Treatment of chronic hepatitis C
To treat a chronic, or long-term, infection of the hepatitis C virus, doctors may prescribe one or more antiviral medicines that attack the virus. Studies have shown that these medicines can cure more than 95% of people with chronic hepatitis C in 8 to 12 weeks.4
Treatment of chronic hepatitis B
To treat a chronic infection of the hepatitis B virus, doctors may prescribe antiviral medicines that slow or stop the virus from further damaging your liver.
Treatment of autoimmune hepatitis
Doctors treat autoimmune hepatitis with medicines that suppress, or decrease the activity of, the immune system.
Treatment of diseases that damage, destroy, or block bile ducts
Doctors usually treat diseases that damage, destroy, or block bile ducts using medicines or medical procedures to open bile ducts that have become narrow or blocked. Diseases that damage, destroy, or block bile ducts include primary biliary cholangitis and primary sclerosing cholangitis.
Treatment of inherited liver diseases
Treatment of inherited liver diseases depends on the disease. Treatments may help prevent, improve, or manage symptoms and complications such as cirrhosis.
Treatment of cirrhosis due to long-term use of certain medicines
If taking certain medicines causes cirrhosis, the only treatment is usually to stop taking the medicines that caused the problem. Talk with your doctor before you stop taking any medicines.
How do doctors treat the complications of cirrhosis?
Treatments for the complications of cirrhosis may include the following.
Portal hypertension
Doctors treat portal hypertension with medicines to lower high blood pressure in the portal vein. Doctors may also treat the following complications of portal hypertension.
Buildup of fluid in the abdomen
A buildup of fluid in the abdomen, or belly, is called ascites. To treat ascites, doctors may prescribe medicines that remove fluid from the body. Doctors may also recommend that people with cirrhosis limit the amount of sodium they eat or drink. If large amounts of fluid build up in the abdomen, doctors may use a needle or tube to drain the fluid and check the fluid for signs of infection. Doctors may prescribe medicines to treat infection or prevent infection.
Swelling in the legs, ankles, or feet
To treat swelling in the legs, ankles, or feet—called edema—doctors may prescribe medicines that remove fluid from the body. Doctors may also recommend that people with cirrhosis limit how much sodium they eat or drink.
Enlarged veins in the esophagus or stomach
Enlarged veins in the esophagus or stomach are called varices. To treat varices, doctors may prescribe medicines to lower the blood pressure in the veins. Lowering the pressure in the veins reduces the chance that the veins will become enlarged and burst, causing internal bleeding. People who vomit blood or have black or bloody stools should go to a hospital right away. Doctors may perform procedures during an upper GI endoscopy or use surgical procedures to stop the bleeding.
Buildup of toxins in the brain
A buildup of toxins in the brain, called hepatic encephalopathy, can cause confusion, difficulty thinking, memory loss, personality changes, or sleep disorders. Doctors may prescribe medicines that help lower the levels of toxins in the brain and improve brain function.
Infections
Doctors will prescribe antibiotics to treat bacterial infections.
Liver cancer
If you have cirrhosis, your doctor may suggest blood tests and an ultrasound or another type of imaging test to check for liver cancer. Doctors may recommend checking for liver cancer every 6 months.5 Finding cancer at an early stage improves the chance of curing the cancer.
For people who develop liver cancer, doctors may treat the cancer with medical procedures that remove or destroy cancer cells, such as surgery, radiation therapy, and chemotherapy. Doctors may also treat liver cancer with a liver transplant.
Liver failure
Liver failure, also called end-stage liver disease, happens when the liver stops working. The only treatment for liver failure is a liver transplant.
Other complications
Doctors may treat other complications through changes in medicines, diet, or physical activity. Doctors may also recommend surgery.
What can I do to help keep my cirrhosis from getting worse?
If you have cirrhosis, you can take steps to help keep cirrhosis from getting worse.
- Do not drink alcohol or use illegal drugs.
- Talk with your doctor before taking
- prescription medicines.
- over-the-counter medicines, including pain relievers, such as nonsteroidal anti-inflammatory drugs (NSAIDs) and acetaminophen, and sleep aids.
- dietary supplements, including herbal supplements.
- complementary and alternative medicines.
- Take your medicines as directed by your doctor.
- Get a vaccine for hepatitis A, hepatitis B, flu, pneumonia caused by certain bacteria, and shingles.
- Get a screening blood test for hepatitis C.
- Consume healthy foods and drinks.
- Avoid raw or undercooked shellfish, fish, and meat.
- Try to reach and stay at a healthy body weight.
When do doctors consider a liver transplant for cirrhosis?
 Talk with your doctor about whether a liver transplant is right for you.
Talk with your doctor about whether a liver transplant is right for you.Doctors will consider a liver transplant when cirrhosis leads to liver failure. Doctors consider liver transplants only after they have ruled out all other treatment options. A successful liver transplant can be a life-saving procedure for people with liver failure. Talk with your doctor about whether a liver transplant is right for you.
References
Eating, Diet, & Nutrition
How does cirrhosis affect eating, diet, and nutrition?
Cirrhosis can lead to malnutrition, meaning that your body is not getting the right amount of the vitamins, minerals, and other nutrients it needs to stay healthy. Research suggests that 50% to 90% of people with cirrhosis have malnutrition.6
People with cirrhosis are at risk for malnutrition for several reasons. The symptoms of cirrhosis, such as nausea and vomiting, may cause people with cirrhosis to eat and drink less. Cirrhosis also affects how the liver works. When the liver isn’t working well, the body may have problems digesting foods and drinks or absorbing nutrients.
What should I eat or drink if I have cirrhosis?
What you eat and drink is important. Your doctor may refer you to a registered dietitian to help create healthy meal plans that fit your nutrition needs.
Meal plans will vary depending on how severe cirrhosis is and other factors. Health care professionals can recommend a meal plan that will provide the amount of calories and nutrients, especially protein, that your body needs. Health care professionals may recommend that people who do not get enough nutrients, or who have low levels of some vitamins and minerals, take certain dietary supplements. If you have cirrhosis, talk with your doctor before taking dietary supplements, including herbal supplements.
Cirrhosis changes the way the body stores nutrients and uses them for energy. People with cirrhosis should avoid fasting, or going without food, for too long. Health care professionals may recommend7
- having smaller, more frequent meals
- eating every 3 or 4 hours while awake
- having a snack before going to sleep at night or having an early breakfast after waking up
Ask your doctor about the cost of a registered dietitian’s services. If you have health insurance, check your insurance company’s website or call customer service to find out if they will pay for some or all of these services.
What should I avoid eating and drinking if I have cirrhosis?
Avoid eating raw or undercooked shellfish, fish, and meat, and unpasteurized milk and milk products. Bacteria or viruses from these foods may cause severe infections in people with cirrhosis.
Your doctor may recommend limiting sodium in foods and drinks.
You should completely stop drinking alcohol because it can cause more liver damage.
References
Clinical Trials
NIDDK conducts and supports clinical trials in many diseases and conditions, including liver diseases. The trials look to find new ways to prevent, detect, or treat disease and improve quality of life.
What are clinical trials for cirrhosis?
Clinical trials—and other types of clinical studies—are part of medical research and involve people like you. When you volunteer to take part in a clinical study, you help doctors and researchers learn more about disease and improve health care for people in the future.
Researchers are studying many aspects of cirrhosis, such as
- new treatments to prevent cirrhosis from getting worse
- new ways to prevent liver cancer in people with cirrhosis
- improved treatments for cirrhosis complications, such as hepatic encephalopathy
Find out if clinical studies are right for you.
Watch a video of NIDDK Director Dr. Griffin P. Rodgers explaining the importance of participating in clinical trials.
What clinical studies for cirrhosis are looking for participants?
You can view a filtered list of clinical studies on cirrhosis that are federally funded, open, and recruiting at ClinicalTrials.gov. You can expand or narrow the list to include clinical studies from industry, universities, and individuals; however, NIH does not review these studies and cannot ensure they are safe. Always talk with your health care provider before you participate in a clinical study.
What have we learned about cirrhosis from NIDDK-funded research?
NIDDK has supported many research projects to learn more about cirrhosis causes, complications, and treatments. Recent examples of research projects include the Liver Cirrhosis Network (LCN), funded by NIDDK, the National Cancer Institute, and the National Institute on Alcohol Abuse and Alcoholism. The network is conducting research to better understand factors that increase the risk of developing cirrhosis complications. LCN will also study treatments that may improve the health of people with cirrhosis. NIDDK also funds the Nonalcoholic Steatohepatitis Clinical Research Network (NASH CRN) and its research on nonalcoholic steatohepatitis (NASH), a liver disease that can cause cirrhosis. NASH CRN has conducted studies to learn more about the causes, development, complications, and treatment of NASH in children and adults.
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
NIDDK would like to thank:
Bilal Hameed, M.B.B.S., University of California, San Francisco
