Bladder Infection (Urinary Tract Infection—UTI) in Adults
Return to Overview PageDefinition & Facts
In this section:
- What is a bladder infection?
- Does bladder infection have another name?
- How common are bladder infections?
- Who is more likely to develop a bladder infection?
- What are the complications of a bladder infection?
What is a bladder infection?
A bladder infection is an illness most often caused by bacteria that enter your bladder and multiply. Bladder infections are the most common type of urinary tract infection (UTI). If untreated, bladder infections can spread to the kidneys and develop into a more serious infection.
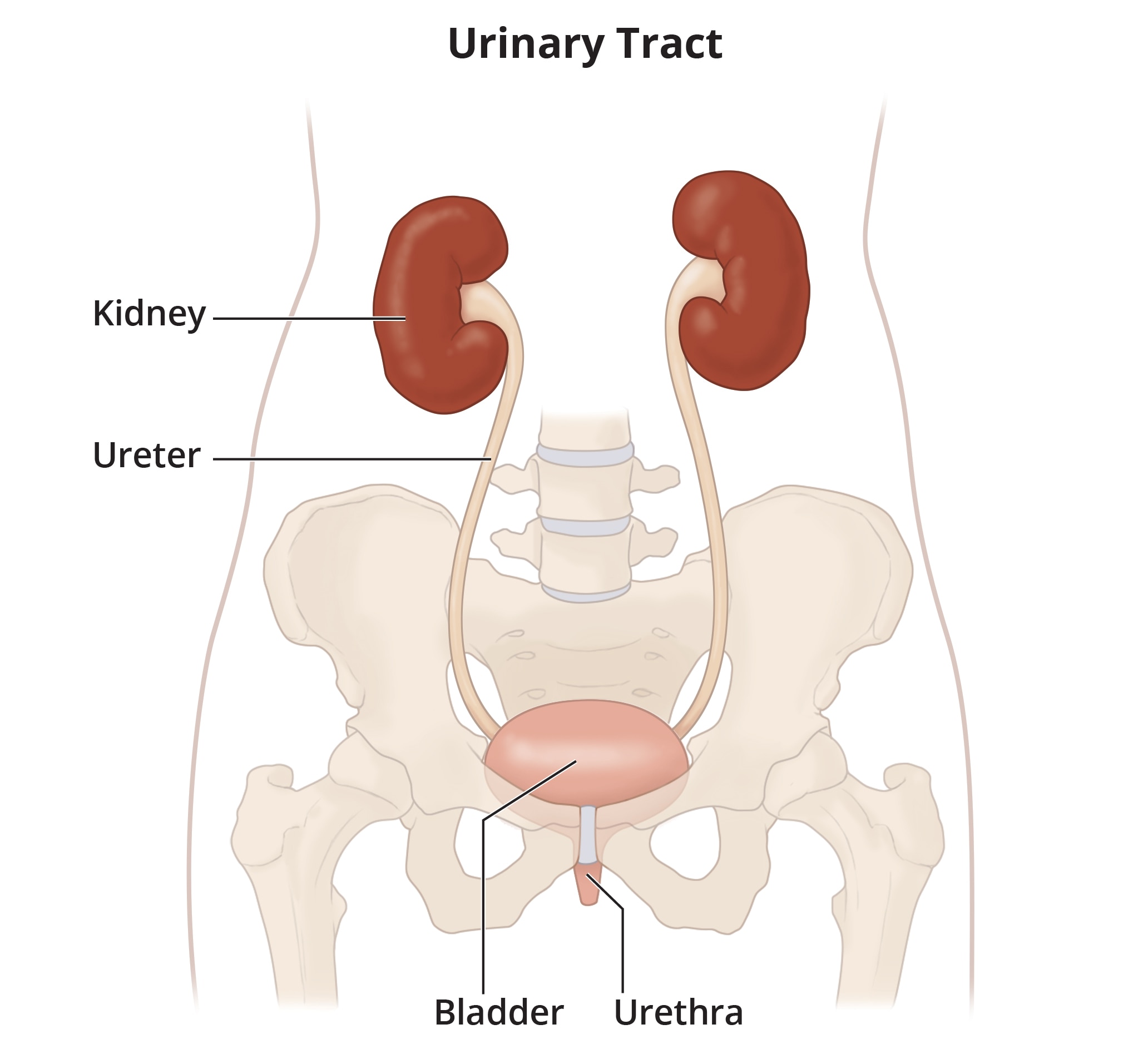 Bladder infections are the most common type of UTI.
Bladder infections are the most common type of UTI.Does bladder infection have another name?
Bladder infections may also be called cystitis. Sometimes people use the more general term, urinary tract infection or UTI, to mean a bladder infection. However, UTIs can occur in other parts of your urinary tract, including the urethra and kidneys.
How common are bladder infections?
Bladder infections are more common in women than in men.
Research shows that about half of all women will develop a bladder infection in their lifetime. About a quarter of those women will have repeat infections.1
Men under age 50 rarely get bladder infections.2
Who is more likely to develop a bladder infection?
Females are more likely to develop bladder infections than males due to their anatomy. Females have a short urethra located close to the anus, a source of bacteria. Therefore, bacteria from the anus may more easily enter the female urinary tract and cause a bladder infection. However, anyone with a bladder can develop a bladder infection, including children.
You are more likely to develop a bladder infection if you
- are sexually active or have gone through menopause
- use certain types of birth control, such as a diaphragm or spermicide
- had a UTI in the past
- have difficulty emptying your bladder completely
- use, or have recently used, a urinary catheter
- have a urinary tract blockage, such as a kidney stone or enlarged prostate
- have an abnormality in the urinary tract, such as vesicoureteral reflux
- have diabetes or problems with your immune system
What are the complications of a bladder infection?
When diagnosed early and treated properly, most bladder infections don’t lead to complications.
If untreated, a bladder infection can spread to one or both of your kidneys. Kidney infections are often very painful. Without treatment, kidney infections can cause serious health problems, such as permanent kidney damage.
Bladder infections that occur during pregnancy are more likely to spread to the kidneys. If you are pregnant, your health care professional may test your urine for bacteria. Regular testing can help your health care professional diagnose and treat a bladder infection before it leads to complications.
References
Symptoms & Causes
What are the symptoms of a bladder infection?
Symptoms of a bladder infection may include
- a burning feeling when you urinate
- frequent or intense urges to urinate, even when you have little urine to pass
- pain or discomfort in the lower abdomen
- cloudy, bloody, or strong-smelling urine
 Bladder infection symptoms may include pain or discomfort in the lower abdomen.
Bladder infection symptoms may include pain or discomfort in the lower abdomen.When should I seek a health care professional’s help?
Contact a health care professional if you have symptoms of a bladder infection.
Bladder infections can spread to one or both kidneys. Quick treatment is important if you have symptoms of a kidney infection, such as
Kidney infections may cause severe pain and serious health problems if not treated early.
What causes a bladder infection?
Bladder infections are most often caused by bacteria. Rarely, fungi may cause a bladder infection.
Normally, the body keeps bacteria in the urinary tract in balance. Emptying your bladder, or urinating, is one way the body helps keep a healthy number of bacteria in your bladder.
Diagnosis
Health care professionals use your medical history, a physical exam, and lab tests to diagnose a bladder infection. In some cases, a health care professional may use other tests to help find the cause of a bladder infection.
 Your health care professional will use your medical history, a physical exam, and lab and other tests to diagnose a bladder infection.
Your health care professional will use your medical history, a physical exam, and lab and other tests to diagnose a bladder infection.What tests do health care professionals use to diagnose a bladder infection?
Health care professionals may use lab tests to test your urine or your blood. Lab tests include urinalysis, urine culture, and blood tests. Your health care professional may also use imaging or other tests.
Lab tests
Urinalysis
Urinalysis checks your urine sample for blood in the urine and white blood cells. Your body produces white blood cells when it is fighting infection caused by bacteria.
Urine culture
Urine culture identifies some common types of bacteria in your urine. This test may help to see whether antibiotics are a treatment option. You will typically get your test results in a few days.
Blood tests
Blood tests look for a more serious infection, such as a kidney infection. A blood test may also show how well your kidneys are working.
Imaging and other tests
If you have repeat bladder infections, your health care professional may also use
- urinary tract imaging to help identify the cause of your infection, such as a kidney stone
- cystoscopy to look inside the urethra and bladder
Treatment
How do health care professionals treat a bladder infection?
If you have a bladder infection caused by bacteria, your health care professional will likely prescribe antibiotics. You can help speed up your recovery and ease your symptoms by drinking more liquids. Drinking more liquids helps flush the bacteria out of your urinary tract.
Your health care professional may also prescribe over-the-counter pain relievers to help with pain. You may be asked to use medicine such as ibuprofen or acetaminophen.
Sometimes, your health care professional cannot confirm a diagnosis based on symptoms and test results. You may not need antibiotics. Instead, your health care professional will work to find the cause and another way to treat your symptoms.
Self-care at home
Drink lots of liquids to stay hydrated and help healing. Water is best.
Talk with your health care professional if you can’t drink a lot of liquids due to other health problems. Some problems may include urinary incontinence, kidney failure, or heart disease. Your health care professional will help you decide the amount of liquids that is right for you.
A heating pad on your back or abdomen may help you ease pain from a bladder infection.
Medicines
Your health care professional may select an antibiotic based on the type of bacteria causing your infection. Your health care professional will consider any allergies you may have to antibiotics.
The length of antibiotic treatment depends on
- how severe your infection is
- whether your symptoms and infection go away
- whether you have repeat infections
- whether you have problems with your urinary tract
Men may need to take antibiotics longer than women because bacteria can move into the prostate. If bacteria get into the prostate, the infection may be more difficult to fight.
If needed, your health care professional may suggest other medicines to relieve any pain or discomfort caused by your bladder infection.
 Follow your health care professional’s instructions carefully when taking antibiotics to treat an infection.
Follow your health care professional’s instructions carefully when taking antibiotics to treat an infection.How do health care professionals treat the complications of a bladder infection?
If a bladder infection leads to a kidney infection, your health care professional will prescribe antibiotics. If you are very sick from the kidney infection, you may need antibiotics through an intravenous (IV) tube. You might go to a hospital or receive IV antibiotics at home.
How can I prevent a bladder infection?
Sometimes, you may be able to help prevent a bladder infection by taking the steps below.
Keep your urinary tract healthy
You can help keep your urinary tract healthy by
- drinking enough liquids
- developing healthy bathroom habits, including wiping front to back
- using the bathroom when you feel the urge to urinate
- taking the time to fully empty your bladder when urinating
Wear loose-fitting clothing
Consider wearing cotton underwear and loose-fitting clothes that don’t trap moisture. Some health care professionals think that too much moisture increases the risk of infection.
Consider switching birth control methods
Talk with your health care professional about switching your birth control if you have repeat bladder infections. Some forms of birth control such as diaphragms, unlubricated condoms, or spermicide may increase your chances of getting a bladder infection.
Consider using vaginal estrogen
If you are in perimenopause or menopause and you have repeat bladder infections, your health care professional may prescribe low-dose, vaginal estrogen. Vaginal estrogen increases good bacteria and helps prevent infection.
Eating, Diet, & Nutrition
Can diet help prevent or treat bladder infections?
Researchers don’t think your diet can help prevent or treat bladder infections. Cranberry products—including cranberry juice, extract, or pills—do not treat existing bladder infections. Some research says that cranberry products may help prevent bladder infections, but there isn’t enough evidence to be sure.3
For safety reasons, talk with your health care professional before using dietary supplements, such as vitamins, or any complementary or alternative medicines or medical practices.
Can drinking liquids help prevent or relieve bladder infections?
Drinking enough liquids can keep you hydrated and help prevent or relieve bladder infections. Water is best.
 Drink lots of liquids to help prevent bladder infections. Water is best.
Drink lots of liquids to help prevent bladder infections. Water is best.Reference
Clinical Trials
NIDDK conducts and supports clinical trials in many diseases and conditions, including urologic diseases. The trials look to find new ways to prevent, detect, or treat disease and improve quality of life.
What are clinical trials for bladder infection in adults?
Clinical trials—and other types of clinical studies—are part of medical research and involve people like you. When you volunteer to take part in a clinical study, you help doctors and researchers learn more about disease and improve health care for people in the future.
Researchers are studying many aspects of bladder infections, such as
- supplements that may prevent repeat bladder infections
- antibiotic alternatives for treating and preventing bladder infections
- shorter-term antibiotics to treat urinary tract infections
Find out if clinical studies are right for you.
Watch a video of NIDDK Director Dr. Griffin P. Rodgers explaining the importance of participating in clinical trials.
What clinical studies for bladder infection in adults are looking for participants?
You can view a filtered list of clinical studies on bladder infections in adults that are open and recruiting at ClinicalTrials.gov. You can expand or narrow the list to include clinical studies from industry, universities, and individuals; however, the National Institutes of Health does not review these studies and cannot ensure they are safe for you. Always talk with your health care provider before you participate in a clinical study.
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
NIDDK would like to thank:
Linda Brubaker, M.D., University of California San Diego
