Research Updates
Diabetes burden is projected to substantially increase among U.S. youth

The projected number of youth in the U.S. diagnosed with type 2 diabetes is expected to rise to 220,000 by 2060, an increase of nearly 700% from 2017, according to new study. The SEARCH for Diabetes in Youth study, funded by the Centers for Disease Control and Prevention and NIDDK, also found that the number of young people with type 1 diabetes could increase by as much as 65% in the next 40 years. These numbers reflect a higher burden of diabetes for Black, Hispanic/Latino, Asian, Pacific Islander, and American Indian/Alaska Native youth. The authors indicate that interventions focused on behavior change and on addressing social determinants of health could be important in preventing youth-onset type 2 diabetes. This research was published in Diabetes Care in December.
Early anti-VEGF treatment of diabetic retinopathy yields no benefit to visual acuity
While early treatment of diabetes-related eye disease slowed progression to severe disease, it did not improve visual acuity compared with treating more severe eye disease once it developed, according to a clinical study from the DRCR Retina Network. Visual acuity refers to how clearly a person can see and is often measured by the ability to discern letters at a given distance. Anti-vascular endothelial growth factor (anti-VEGF) drugs can substantially decrease the risk of vision loss from diabetic retinopathy. However, eye care providers have been unsure when treatment should start to achieve the best long-term outcome. The study showed that while preventive treatment reduced the risk of developing diabetic macular edema, it provided no evident benefit to vision over four years—suggesting that monitoring patients regularly for vision-threatening diabetes complications and treating eyes only as needed may be the best approach. The study was funded by NIH, including funds provided through the Special Diabetes Program, and published in the Journal of the American Medical Association in February.
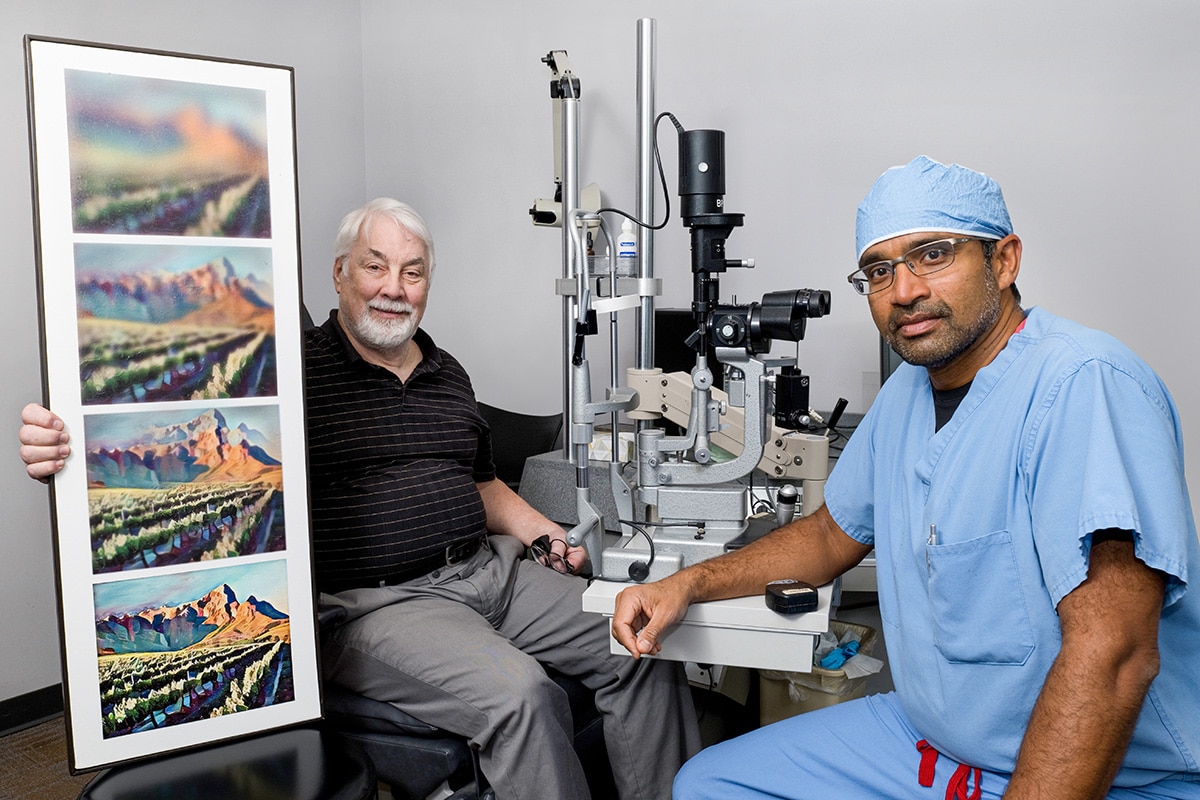 Raj Maturi, M.D., with a patient. Images illustrate vision improvement with treatment for diabetic retinopathy.
Raj Maturi, M.D., with a patient. Images illustrate vision improvement with treatment for diabetic retinopathy.
Credit: Raj Maturi, M.D.
Gut microbes may affect motivation to exercise
 Credit: Shutterstock
Credit: Shutterstock
NIH-supported research found that gut microbes play a role in determining how much mice exercise. The researchers from University of Pennsylvania first measured how long mice running on a treadmill took to exhaust themselves and how much the mice voluntarily ran on a wheel. The team found that dopamine levels increased after exercise in normal mice, but not in microbiome-depleted mice. Next, the team identified a class of compounds, called fatty acid amides (FAAs), which are produced by gut microbes. They found that supplementing the diets of microbiome-depleted mice with FAAs restored their exercise capacity. These results suggest that microbiome-produced FAAs in the gut stimulate sensory neurons. Signals from these sensory neurons lead to increased dopamine levels in the brain during exercise, which, in turn, enhance the desire for exercise. The findings suggest that the motivation to exercise—or lack thereof—might depend on the state of the gut microbiome and might be enhanced by stimulating this sensory pathway. The study appeared in Nature in December 2022 and was featured in NIH Research Matters.
Study identifies genetic variations in people with prediabetes that may influence metformin response
 Credit: Shutterstock
Credit: Shutterstock
NIDDK-supported research has identified genetic contributions that may influence metformin response in those with prediabetes. DNA from participants in the Diabetes Prevention Program (DPP) study, who were from diverse backgrounds and all at high risk for type 2 diabetes, was tested to locate genetic variants associated with the development of diabetes as well as indicators of response to metformin. People’s response to metformin—a diabetes drug that lowers blood sugar levels—can vary. While the team identified no new significant genetic variants associated with the incidence of diabetes, they found some variants related to ancestry that appear to affect metformin response. In the metformin treatment group, a genetic variant near the gene ENOSF1, was more common among African American participants and was associated with an increase in blood sugar levels and poorer response to metformin. Another variant, near the gene OMSR, was more common among American Indian participants and was associated with a weight-loss benefit from metformin. These results could potentially have implications for precision medicine for prediabetes. The study was published in Diabetes in December.
Dietary nitrate increases muscle force during exercise
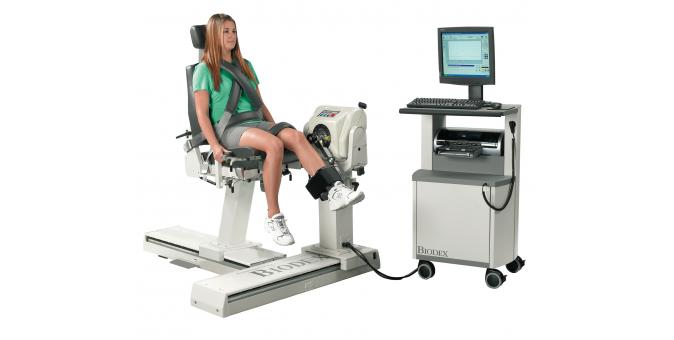
Researchers found that consuming dietary nitrate can increase muscle force by 7% compared to a placebo. Dietary nitrate, a nutrient found in some vegetables, increases the body’s level of nitric oxide, a vital molecule that affects many aspects of health. In the study, led by researchers at NIDDK and the University of Exeter, 10 healthy participants were asked to perform quadricep (upper thigh) contractions at maximum intensity for five minutes one hour after consuming nitrate. The researchers tested the participants’ levels and distribution of nitric oxide metabolites in the saliva, blood, muscle, and urine before and after the exercise. They found that nitrate accumulates in muscle and is utilized when exercising, demonstrated through increased muscle nitrate levels and improved muscle performance among the participants who consumed the dietary nitrate. The results, published in Acta Physiologica in January, have implications for the exercise science field, as well as potentially other areas examining neuromuscular and metabolic diseases related to nitric oxide deficiency.
Two new technologies provide new insights for polycystic kidney disease
An NIH study using two cutting-edge technologies revealed that blood glucose plays a role in promoting cyst growth in polycystic kidney disease (PKD), a genetic disease affecting millions of people worldwide and a common cause of kidney failure. NIDDK-supported researchers used a kidney organoid—a living, miniaturized organ grown in a laboratory dish—and an “organ-on-a-chip”—a miniaturized device engineered to mimic the 3D tissue structure and basic biology of a kidney.
Using this one-two approach at the lab bench, the researchers modeled in just a few weeks different aspects of the fluid-filled cysts that form PKD—an impossibility before now. Researchers also found the cysts were absorbing glucose and taking in water from the fluid passing over them, causing the cysts to expand. Although scientists had known that kidneys absorb glucose, they’d never connected this process to the formation of cysts in PKD.
These findings may lead to new treatments for preventing PKD or slowing its progression. The research published in Nature Communications in December and was featured in a NIH Director’s Blog post in January.
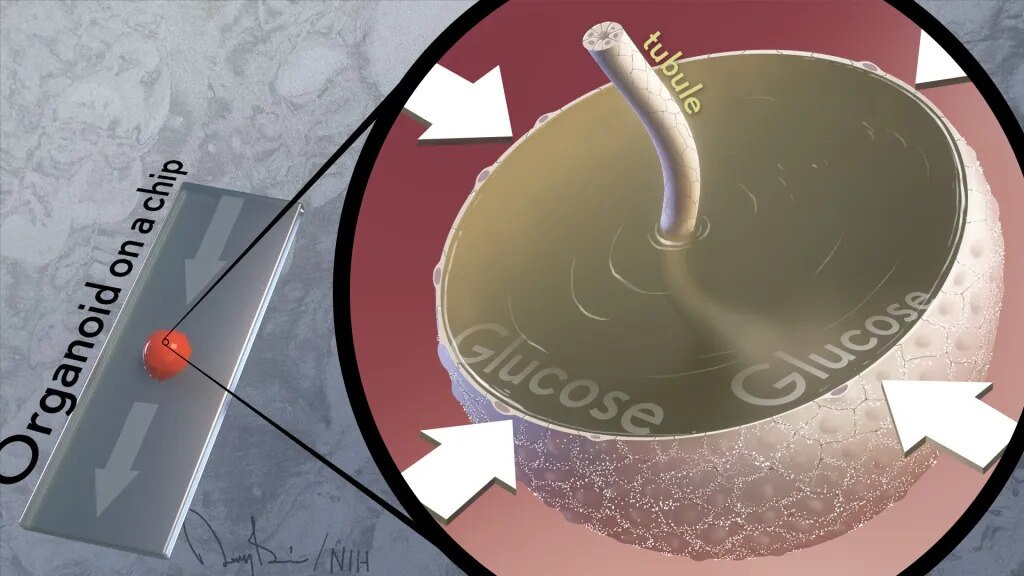 Credit: NIH
Credit: NIH

