News Around NIDDK
After tumultuous year, NIDDK remains steadfast in tackling COVID-19
More than a year into the pandemic, NIDDK continues to make and support important contributions to the fight against COVID-19. In recent months, NIDDK researchers and grantees published studies that deepened understanding of SARS-CoV2 – the virus that causes COVID-19 – and how it exacerbates health conditions and affects organs relevant to NIDDK’s mission. Recent research includes
- Cell-free DNA maps COVID-19 tissue injury and risk of death, and can cause tissue injury
- Assessment of acute kidney injury and longitudinal kidney function after hospital discharge among patients with and without COVID-19
- Continuous renal replacement therapy and the COVID pandemic
- Variability in digestive and respiratory tract Ace2 expression is associated with the microbiome
- Convalescent Plasma Antibody Levels and the Risk of Death from Covid-19
- COVID-19 Stress and Food Intake: Protective and Risk Factors for Stress-Related Palatable Food Intake in U.S. Adults

NIDDK-supported scientists also published a comprehensive review on post-acute COVID-19 syndrome, often called “long-haul COVID-19,” including considerations for clinical care of COVID-19 survivors.
In Arizona, staff from NIDDK’s Phoenix Epidemiology and Clinical Research Branch (PECRB) continue to volunteer at the Phoenix Indian Medical Center to help with clinical care during the COVID-19 patient surge. For example, since last August, PECRB’s Dr. Madhumita Sinha has been seeing patients in the hospital’s pediatric clinic. The experience, Sinha said, “has helped her understand the health needs of the American Indian/Alaska Native community, which has been severely impacted by the COVID-19 pandemic.”
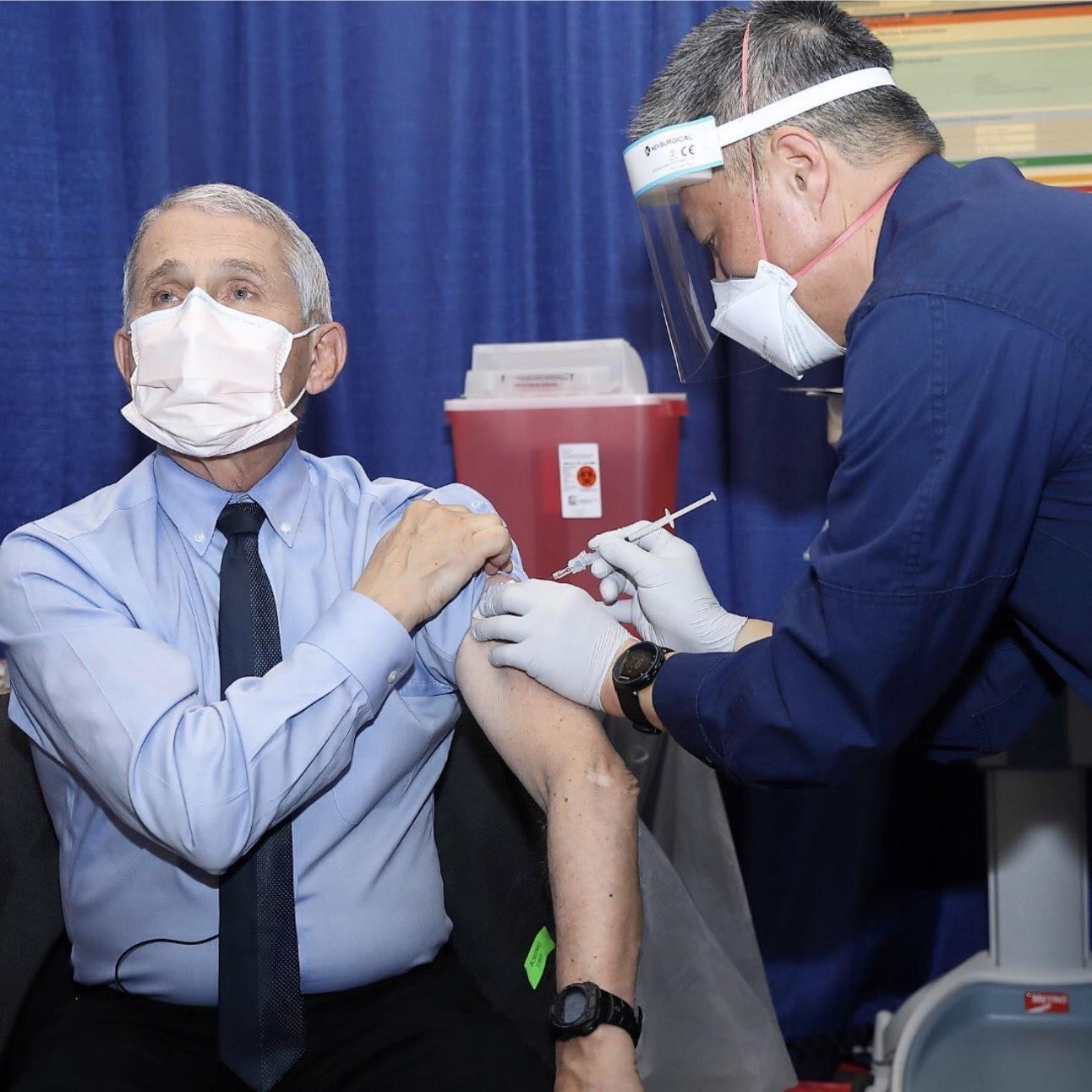
In May, NIDDK Director Dr. Griffin P. Rodgers hosted Dr. Anthony Fauci, director of NIH’s National Institute of Allergy and Infectious Diseases, on the Healthy Moments radio show for a series on COVID-19 vaccines. Rodgers also partnered with Dr. William Cefalu, director of NIDDK’s Division of Diabetes, Endocrinology, and Metabolic Diseases, to write about the racial and ethnic health disparities related to COVID-19 and metabolic diseases such as diabetes and obesity. Their perspective published in Cell Metabolism in March.
Through various funding mechanisms, NIDDK is also encouraging new research on the socio-economic factors underlying health disparities in NIDDK mission areas and how they may contribute to COVID-19 outcomes.
For more information on NIDDK research and funding opportunities related to COVID-19, visit the NIDDK COVID-19 Research Response page.
For past highlights of NIDDK’s COVID-19-related work, see recent articles in the NIDDK Director’s Update and NIH Record:
- NIDDK staff guide key COVID-19 research and serve on pandemic frontlines
- NIDDK continues to support COVID-19 efforts
- NIDDK tackles COVID-19 through research, funding, and clinical care
- NIDDK research shows the importance of wearing masks
For NIH COVID-19 updates, visit Covid19.nih.gov. For more information on COVID-19, visit the Centers for Disease Control and Prevention (CDC) coronavirus webpage.
Celebrating NIDDK’s diabetes research during the 100th anniversary of insulin’s discovery
In the summer of 1921 at the University of Toronto, after months of failed experiments, Drs. Frederick Banting and Charles Best made a profound discovery. They discovered that a pancreatic extract from heathy dogs reduced blood glucose in other animals with diabetes. By the following year, that extract was chemically refined and used in human clinical trials to treat people with type 1 diabetes. Called insulin, the extract would change type 1 diabetes from a fatal condition to one that could be managed.

In the 100 years since, tremendous progress has been made in diabetes research and care. By 1936, the glucose tolerance test was developed and two types of diabetes emerged – insulin-sensitive and insulin-insensitive – what is now known as type 1 and type 2 diabetes respectively.
From its very beginning in 1950, NIDDK conducted and supported laboratory, clinical, and population research to to understand diabetes, metabolic, endocrine, and related diseases.
“NIDDK has leveraged the discovery of insulin to play a critical role over the last 70 years in advancing diabetes research,” said Dr. Griffin P. Rodgers, NIDDK Director.
A new approach to type 1 diabetes
NIDDK-supported research has made an important impact on advancing understanding about type 1 diabetes. The Diabetes Control and Complications Trial (DCCT) started in 1983 to see if people with type 1 diabetes who kept their blood glucose levels as close to normal as could safely be achieved could delay development of diabetes-related complications such as eye, kidney, and nerve disease, compared with people who used the conventional treatment at the time of the study.
The study became a landmark success. The DCCT ended after 10 years in 1993—a year earlier than planned—when the study showed that participants could significantly lower their chances of developing diabetes-related complications by keeping their blood glucose levels close to normal. Its long-term follow-up study, called the Epidemiology of Diabetes Interventions and Complications (EDIC), has followed DCCT participants since the trial ended and showed that continuing the tight management of blood glucose levels helps people with type 1 diabetes live a normal-length life.

“The DCCT/EDIC findings were paradigm changing and were quickly adopted worldwide and incorporated into the standards of care for people living with diabetes, said Dr. William Cefalu, director of NIDDK’s Division of Diabetes, Endocrinology, and Metabolic Diseases (DEM). “This NIDDK-supported research favorably changed the way we review the management of diabetes forever.”
Much of NIDDK’s type 1 diabetes research funding comes from the Special Statutory Funding Program for Type 1 Diabetes Research, or Special Diabetes Program (SDP). This special appropriation approved by Congress has provided more than $3 billion over 24 years to support innovative trials and research networks for the prevention, treatment, and cure of type 1 diabetes.
The SDP has supported the development of cutting-edge technologies that have made daily management of diabetes easier, such as the continuous glucose monitor (CGM). In the last few years, artificial pancreas technology has eased the management burden. The devices automatically monitor and regulate blood glucose using a CGM and insulin pump programmed with dosing algorithms tailored to the user. Through decades of NIDDK-supported clinical testing and trials, multiple artificial pancreas devices have been approved by the Food and Drug Administration.
Breaking through on type 2 diabetes

While NIDDK-supported research made its mark in the type 1 diabetes field, the institute’s role in type 2 research had an earlier start. By the 1960s, NIDDK began the first long-term population study among American Indians to understand causes and risk factors for type 2 diabetes and its complications. One of the first collaborations of its kind, the study was conducted in partnership with the Gila River Indian Community, the Indian Health Service, and other academic partners.
NIDDK’s Dr. William Knowler, chief of the NIDDK Diabetes Epidemiology and Clinical Research Section in Phoenix, was a principal investigator with the study, which uncovered the alarmingly disproportionate burden of diabetes and its complications among American Indians.
“One of our important early observations was that type 2 diabetes occurs in American Indian children,” said Dr. Knowler. “It was previously assumed that almost all diabetes in children was type 1 diabetes, which has a different pathogenesis from type 2 diabetes that was previously thought to occur only in adults. Type 2 diabetes is now recognized as a major form of diabetes in U.S. children, especially those from certain racial and minority groups.”
The study also revealed risk factors for type 2 diabetes, some of which – such as obesity – had the potential to be modified to reduce risk or delay onset in those at high risk for type 2 diabetes.
To test this, the NIDDK-funded Diabetes Prevention Program (DPP) was launched in the 1990s to examine whether an intensive lifestyle intervention for weight loss or the medicine metformin would delay or prevent type 2 diabetes among people at high risk for the disease.

Three years into the four-year study, the trial stopped early because of the significant benefits seen among participants in both of the study’s treatment groups. The study found that people who are at high risk for type 2 diabetes can prevent or delay the disease by losing a modest amount of weight, about seven percent of their starting weight, through lifestyle changes – regular physical activity and a diet low in fat and calories. Participants in the lifestyle program reduced their incidence of diabetes by 58% during the 3-year study. The generic drug metformin also prevented the disease by about 31%.
“This was a very exciting time for all of us involved in the study. The large magnitude of the lifestyle effect was much greater than we had hoped for,” said Knowler, who also served as a principal investigator with DPP.“ And because the intervention effects were uniform among the participants from different racial and ethnic groups, and geographic areas, the results changed the way people approach type 2 diabetes prevention worldwide.”
Blazing a future of innovation and better health
As NIDDK continues to support innovative research, a new area of exploration focuses on the ways in which diabetes varies among people, even among those diagnosed with the same diabetes type. In fact, some forms of diabetes don’t fit any of the known types or causes.
A new NIDDK-funded study called RADIANT (the Rare and Atypical Diabetes Network) seeks people with these unknown or uncommon forms of diabetes to help understand the broad spectrum of diabetes.
“Through RADIANT and other studies like it, we hope to gain insight into the more common differences present within the current diagnostic criteria for diabetes”
“Through RADIANT and other studies like it, we hope to gain insight into the more common differences present within the broad spectrum of type 2 diabetes and develop diagnostic criteria for new forms of diabetes,” said Dr. Christine Lee, program director in DEM and project scientist for RADIANT. “Precision medicine will play a key role in the future of personalized diabetes care. Because we know that one size doesn’t fit all, having precise information on prognosis and therapies for a given person will help them form diabetes care plans to meet their individual goals and preferences.”

Many of the last 100 years of advances would not have been possible without the altruism of study participants. Elena Ennis, a study participant with type 1 diabetes who tested artificial pancreas technology, spoke about her experience volunteering in a trial.
“Before I had participated in my first clinical trial, I was very newly diagnosed and everything was so new to me. I was worried about what my future would look like,” she said. “Participating in these trials really has given me a sense of hope as far as the future of living with diabetes. I feel like I have a large support group behind me cheering me on, because researchers are really working so hard to make things better for those of us with diabetes.”
As the century since Banting and Best’s discovery comes to a close, the future of diabetes research – and better prevention, management and, one day, a cure, looks bright. “NIDDK and the diabetes research community as a whole have made great progress,” Rodgers said. “But our work is not done, and NIDDK will continue working toward finding prevention methods, better treatments and, one day, a cure for all types of diabetes.”

Joint symposium on June 2-3 marks insulin’s 100 years
To commemorate the discovery of insulin and global advances in diabetes research over the last 100 years, on June 2-3, NIDDK and the Institute of Nutrition, Metabolism and Diabetes (INMD), part of the Canadian Institutes of Health Research, have partnered to host a free, virtual symposium titled, “Heterogeneity of Diabetes: Beta Cells, Phenotypes and Precision Medicine.”
Worldwide leaders in diabetes research will discuss the past, present and future of insulin-related discoveries. “NIDDK is thrilled to partner with our Canadian counterparts to host this event,” said Cefalu. INMD Scientific Director Dr. Norman Rosenblum added, “the event promises to promote insightful discussion about the great challenges and opportunities in advancing diabetes research today.”
For more information about the symposium and to register, visit https://www.niddk.nih.gov/news/meetings-workshops/2021/heterogeneity-diabetes-beta-cells-phenotypes-precision-medicine
Getting to Know: Dr. Gary Felsenfeld

Dr. Gary Felsenfeld, section chief in the Laboratory of Molecular Biology, and major contributor to our understanding of the relationship between chromatin structure and gene expression, Zoomed with Katie Clark, sharing details of his career at the NIH, advice to those beginning their research career, and hopes for the future of research in physical chemistry.
What do you enjoy most about working at the NIH?
At the NIH, I can work at my lab bench and experiment all day long. I’m able to remain constantly invested in the science. The freedom to try unusual new experiments and explore out of the ordinary ideas is something that is hard to find in the scientific world. Here, it’s science full-time, with no distractions.
What inspired you to study chromatin?
As a physical chemist, I started to study multistranded nucleic acids as part of my earliest research here at the NIH. I worked on understanding the electrostatic forces that stabilized nucleic acid structures, beginning with magnesium ion, and then moving on to larger positively charged molecules and proteins.
At some point, I realized I was interested most in what is going on inside the cell. Then I started to work with real cells, real nuclei, and with chromatin — the package of DNA with charged proteins and other molecules that modify its behavior.
What do you hope for the future of your field in the next 10 years and beyond?
I hope that in the future, we will know much more than we know today about neural mechanisms. Neurobiology is a field that is very attractive to someone like me who grew up in a time when there were enormous scientific questions which we had few tools to address. Now we are just at the beginning of understanding how the nervous system works, an exciting time.
What advice do you have for people beginning their research career?
Figure out how your personality fits with different scientific problems. Some people love detail. Others prefer to tackle a messy problem, clear away the brush and let someone else work out the details. Both personality types are valued and able to make great contributions, but if you are stuck in the wrong channel, that’s when it doesn’t work. A good mentor will help you to figure out what kind of person you are. A separate piece of advice: When you make a discovery, stop what you’re doing and enjoy that moment.
When off duty, what are your hobbies?
Since I was 12 years old, I’ve thoroughly enjoyed photography. I started developing prints from a young age and still enjoy printing and mounting images I’ve taken throughout the years. I also enjoy reading history, particularly Mesopotamian, Assyrian, Sumerian, and Akkadian history. But of course, science is the greatest hobby, and you are never off duty.
NIDDK diversifies science workforce through decades-long efforts
NIDDK office helps change the face of biomedical research
By Lisa Yuan
Diversity strengthens science. That’s been a guiding principle of NIDDK’s Office of Minority Health Research Coordination (OMHRC) for 21 years. Its programs stem from the recognition that diverse teams bolster problem-solving and creativity, ultimately leading to better science.
“Our mission is to train the next generation of scientists, especially those from minority and underrepresented groups, who can draw from their diverse experiences to tackle the myriad of health challenges this country faces,” said OMHRC Director Dr. Lawrence Agodoa.
 OMHRC staff: Morgan Moore, Robert Rivers, Fanta Kamara, Lawrence Agodoa, Katrina Serrano, Winnie Martinez.
OMHRC staff: Morgan Moore, Robert Rivers, Fanta Kamara, Lawrence Agodoa, Katrina Serrano, Winnie Martinez.NIDDK has been working to diversify the biomedical research workforce for several decades, through programs dating back to the 1970s. In 2000, NIDDK established OMHRC to manage these programs and implement additional efforts to train and support aspiring scientists from minority or disadvantaged groups, as well as those with disabilities. Overall, in the past 40-plus years, NIDDK has helped more than 7,000 people from diverse backgrounds to pursue – and excel in – careers in science.
Wendy Osei-Bonsu is one such participant. From 2016 to 2018, she took part in OMHRC’s Short-Term Research Experience for Underrepresented Persons (STEP-UP) program, which provides high school and college students with mentored, hands-on experience in research labs throughout the United States and its Atlantic and Pacific territories.

As an undergraduate, Osei-Bonsu spent three summers in a University of Pennsylvania medical school lab, studying disorders such as diabetes and pre-term birth. This experience, made possible through STEP-UP, showed her how she could apply her love of science to making a difference in people’s lives.
“My work through the STEP-UP program strengthened my dedication to pursue a career in medicine and research to further improve care for underserved communities,” said Osei-Bonsu, now a third-year medical student.
STEP-UP not only provided Osei-Bonsu with critical training in research and science communication, it also connected her with a network of mentors, some with backgrounds similar to hers, who continue to provide guidance and support.
“The mentors and network I have built because of STEP-UP remain an essential part of my accomplishments so far, as well as my continued growth as a student and future physician and scientist,” she said.
Mentoring is also a key component of OMHRC’s Network of Minority Health Research Investigators (NMRI) program, created in 2003 to encourage minority investigators to pursue research in NIDDK disease areas. With over 700 members and growing, the network thrives on the dedication of its senior members, who mentor junior members in career development areas such as completing grant applications and advancing towards tenure.
Another OMHRC program helping scientists advance their careers is the Small Grants for New Investigators to Promote Diversity in Health-Related Research (R21), which supports early-career investigators from diverse backgrounds to conduct small research projects on NIDDK-relevant diseases and on health disparities. The data produced from these projects can be used to apply for higher-level funding. In fact, many R21 awardees have gone on to receive R01 grants, the most competitive grant type.
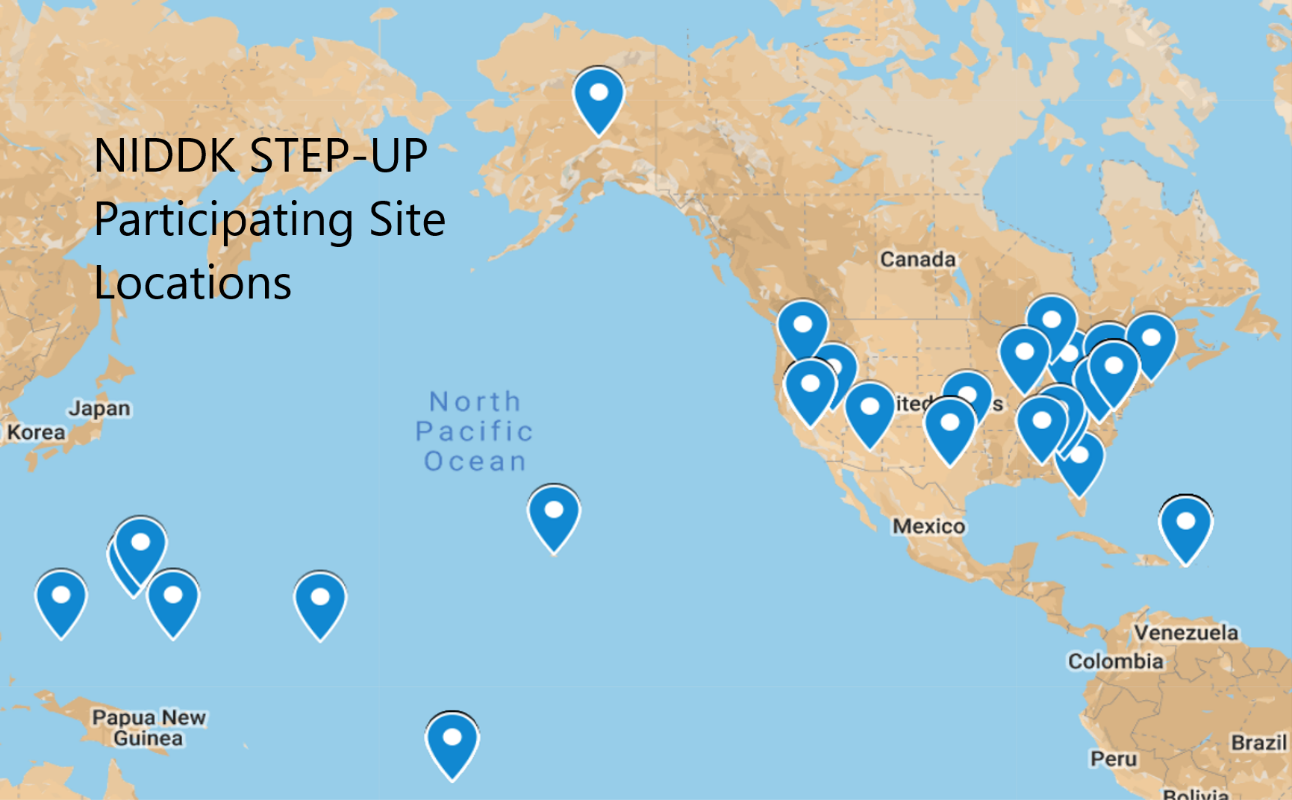 NIDDK’s STEP-UP program has sites across the United States and Territories.
NIDDK’s STEP-UP program has sites across the United States and Territories.“NIDDK was the first NIH institute to come up with this program to support new and diverse investigators,” said OMHRC’s Dr. Katrina Serrano, who oversees the R21 program. “It shows how innovative and committed NIDDK has been to advancing diversity in health research.”
OMHRC staff will maintain this forward-thinking approach as they continue to work towards eliminating enduring health disparities and structural racism. The office is also evaluating the many existing programs in their robust portfolio, a few of which were highlighted here, to ensure that resources are being used as effectively as possible.
“At NIDDK, our goal is to improve health for all people. To get there, we must redouble our efforts to ensure the research workforce fully represents the populations most afflicted by the diseases we study,” said NIDDK Director Dr. Griffin P. Rodgers. “OMHRC is at the forefront of those efforts, and therefore, integral to the mission of NIDDK.”
16th annual scientific conference unites NIDDK fellows virtually
On April 1 and 2, the Annual NIDDK Scientific Conference, organized by the NIDDK Fellows Advisory Board (FAB), was held to share research, professional development opportunities, and other resources available at NIH within the fellows’ community.
More than 100 fellows shared their research through poster and oral presentations in a virtual, but interactive, environment. In addition to fellows’ presentations, NIDDK’s Drs. Susanne Neumann, Katherine McJunkin, Leslie Baier, and Anne Sumner served as session chairs and presented research from their labs. Invited speakers discussed coronavirus research, career consulting, NIH facilities and resources available to fellows, and opportunities offered by Foundation for Advanced Education in the Sciences (FAES). The conference hosted two keynote speeches: Dr. Rommie Amaro describing the SARS-CoV2 at atomic detail and Dr. Sydnee & Justin McElroys from a comedic medical podcast Sawbones: A Marital Tour of Misguided Medicine.
“The scientific conference continues to be a great platform to get to know what other labs are doing in NIDDK, to foster a sense of community, and to create potential collaborations,” said FAB chair Dr. Sezen Meydan, a fellow in NIDDK’s Laboratory of Biochemistry and Genetics. “This year’s conference was yet another success. Despite ongoing challenges of the pandemic, the conference showed that the NIDDK community relentlessly continues doing amazing science.”
Learn more about NIDDK fellowships. If you are an NIDDK fellow and interested in participating in the FAB, contact Rits Sarkar (rits.sarkar@nih.gov) for more information.
2021 NIDDK Scientific Conference winners
Oral Presentations:
Dr. Benedikt Hild
Dr. Shannon Ohlemacher
Elevator Talks:
Winner: Dr. Valerie Darcey
Honorable mentions: Samantha Matta, Megan Onyundo
Poster Presentations:
Session I: Dr. Daniel Chauss, Dr. Paola Oliva, Lauren Wedekind
Session II: Dr. Yusuke Okuno, Dr. Annemarie Wentzel, Alex Schick
NIDDK staff updates Congress on research advances, opportunities
On April 14, NIDDK staff participated in a congressional briefing organized by the Friends of NIDDK to update Congress on research advances and emerging opportunities highlighted in the Institute’s most recent annual report. NIDDK Director Dr. Griffin P. Rodgers gave an overview of the report and described cross-cutting research areas of importance to the Institute.

An area of importance Rodgers described is the demonstrated health disparities associated with many diseases and disorders in the NIDDK mission. “Health disparities are exacerbated by the COVID-19 pandemic,” said Rodgers. “There are increased rates of COVID-19 infection and poor outcomes seen in people with conditions in the NIDDK mission.” He then discussed NIDDK efforts to combat COVID-19 and achieve health equity.
The briefing highlighted the critical role of research participants in NIDDK-supported clinical studies. Ms. Pamela Taylor talked about her decades-long ongoing participation in the landmark Diabetes Prevention Program (DPP)/DPP Outcomes Study, which she also described in NIDDK’s 2021 annual report. She stressed the importance of including minority participants in clinical research studies and said that the scientific community needs to meet people where they live and work in order to increase participation in these studies.
In addition, directors from three NIDDK divisions presented research highlights and programs from across NIDDK mission areas. For example, the Human Pancreas Analysis Program aims to unravel basic mechanisms of the disease processes that underlie type 1 and type 2 diabetes; the Childhood Liver Disease Research Network collaboratively studies rare forms of pediatric liver disease, such as biliary atresia; and the Kidney Precision Medicine Project is analyzing kidney biopsies from people with kidney disease using cutting-edge technologies to identify new therapeutic targets.
Results are in…NIDDK continues to rank No. 1 in employee survey

2020 Federal Employee Viewpoint Survey (FEVS), is a government-wide survey for federal employees to share perceptions of their work experiences and leadership. This year, nearly 75% of eligible NIDDK employees took part in the survey, a new record for participation. Staff responses led to NIDDK ranking first in employee engagement, global satisfaction, and belief in action across the entire NIH. “With this encouraging evaluation, NIDDK will continue to strive to create an environment where all can be effective, safe, and valued – a place where everyone can flourish,” said NIDDK Director, Dr. Griffin P. Rodgers.

