Chronic Kidney Disease (CKD)
- What Is Chronic Kidney Disease in Adults?
- Causes of CKD
- Tests & Diagnosis
- Managing CKD
- Healthy Eating
- Preventing CKD
- What If My Kidneys Fail?
- Clinical Trials
What Is Chronic Kidney Disease in Adults?
In this section:
- How common is CKD in adults?
- Which adults are more likely to develop CKD?
- What are the complications of CKD in adults?
- What are the symptoms of CKD in adults?
- Clinical Trials for CKD in Adults
Chronic kidney disease (CKD) is a condition in which your kidneys are damaged or have a problem with their structure that prevents them from filtering blood the way they should. As a result, waste and extra fluid can build up in your body.
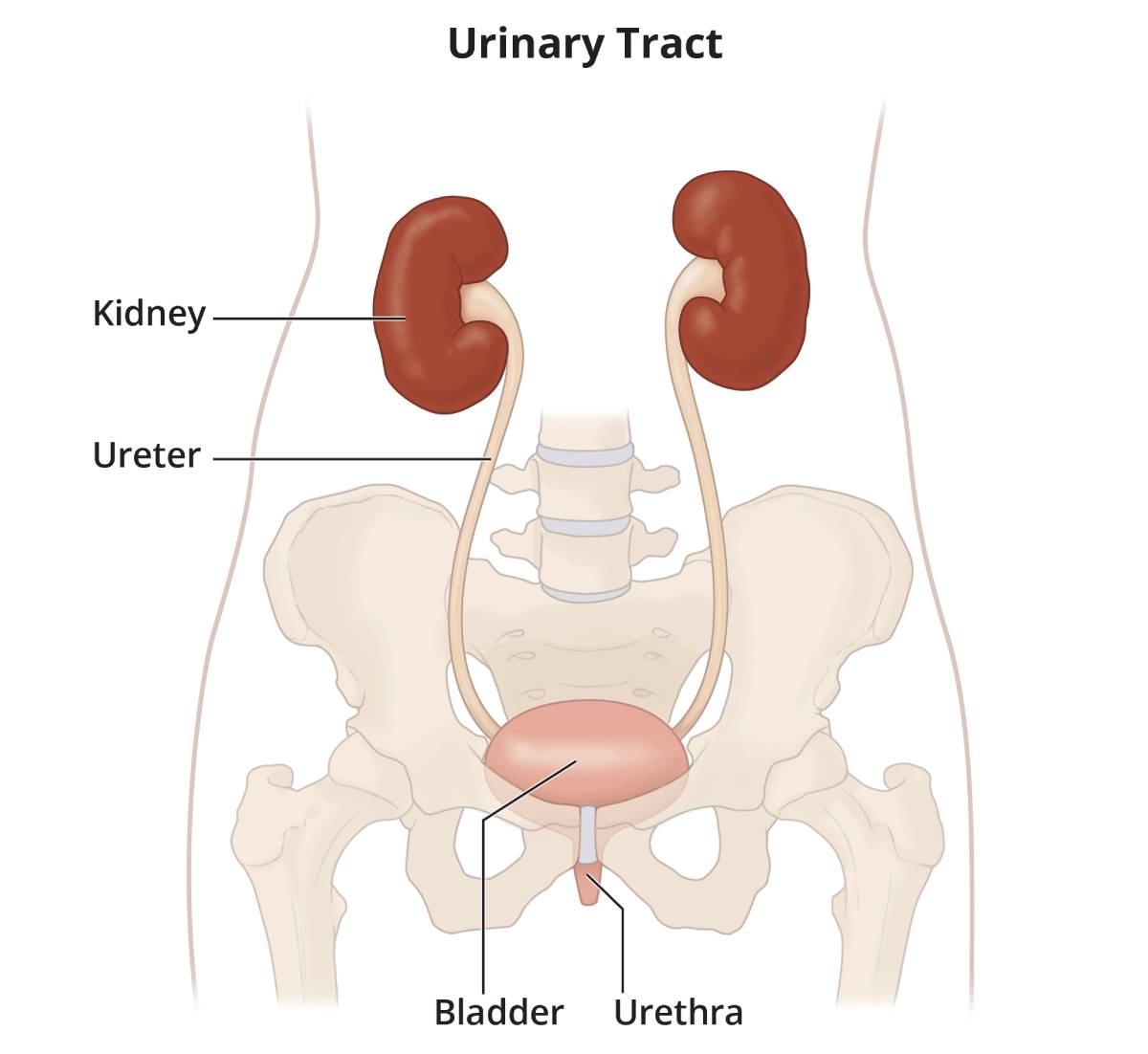 View full-sized image Kidneys filter your blood, removing waste and extra fluid from your body.
View full-sized image Kidneys filter your blood, removing waste and extra fluid from your body.
CKD often develops slowly. However, sometimes CKD can develop as a result of a sudden event. Advanced, long-lasting CKD typically can’t be reversed. In some people, CKD can lead to kidney failure. However, the sooner you find out you have CKD, the sooner you can make changes to protect your kidneys from further damage.
Preventing or managing health conditions that cause CKD, such as diabetes and high blood pressure, may help prevent CKD or slow its progression. Adopting healthy lifestyle habits, such as eating right, maintaining a healthy weight, staying physically active, and avoiding medicines that can injure the kidneys, may also help keep your kidneys healthier longer.
Watch a video to learn more about what the kidneys do.
How common is CKD in adults?
CKD is common among adults in the United States. Researchers estimate more than 35 million U.S. adults—more than 1 in every 7 adults—have CKD.1
Which adults are more likely to develop CKD?
You are at risk for developing CKD if you have
- diabetes
- high blood pressure
- heart and blood vessel disease, also called cardiovascular disease
- family history of kidney disease
Your risk for developing CKD increases with age.1 Also, the longer you’ve had diabetes, high blood pressure, or heart and blood vessel disease, the more likely you are to develop CKD.
 Talk with family members who may be at risk for kidney disease about the importance of getting tested.
Talk with family members who may be at risk for kidney disease about the importance of getting tested.
African Americans, Hispanic people, American Indians, Native Hawaiians, and other Pacific Islanders are more likely to have advanced kidney disease, including kidney failure.2 The rates of diabetes and high blood pressure that these groups experience may contribute to their kidney failure risk. Managing blood pressure, blood glucose levels, and weight if you have overweight or obesity can help slow the progression of CKD and prevent or delay kidney failure.
If you’re at risk for CKD, it’s important to get tested and take steps to prevent or slow kidney disease. Talk with family members about their kidney health, and encourage them to get tested if they’re at risk.
Learn more about kidney disease statistics.
What are the complications of CKD in adults?
Complications of CKD may include
- heart and blood vessel disease, including stroke and heart attack
- high blood pressure
- anemia
- mineral and bone disorder
- metabolic acidosis
- malnutrition
- electrolyte imbalances in the blood, especially high potassium
If you have CKD, you have a higher risk of developing acute kidney injury (AKI). AKI is a sudden loss of kidney function caused by illness, injury, or certain medicines. AKI may cause more kidney damage and worsen kidney function in the short and long term.
Living with CKD can be stressful. Talk with your health care professional about finding healthy ways to cope with stress and depression.
What are the symptoms of CKD in adults?
Symptoms of early CKD
Most people in the early stages of CKD do not have symptoms, and many people have no symptoms until their kidney disease is advanced. For many people, the only way to know if they have CKD is to get their kidneys checked with blood and urine tests.
People with CKD may get swelling, called edema. Edema can happen when the kidneys can’t remove extra fluid and salt from the body. Edema can occur in the legs, feet, ankles, or—less often—in the hands or face. Edema is more common when kidney disease is very advanced or when there’s a lot of protein leaking into the urine.
Symptoms of advanced CKD
As CKD becomes more advanced, symptoms may include
- loss of appetite, nausea, or vomiting
- feeling tired or having sleep problems
- trouble concentrating
- a change in how often you urinate
- foamy urine
- itching, numbness, dry skin, or darkened skin
- weight loss
- muscle cramps
- chest pain or shortness of breath
- worsening edema
Taking steps to manage your CKD, such as with lifestyle changes and medicines, may help reduce symptoms and complications.
Clinical Trials for CKD in Adults
NIDDK conducts and supports clinical trials in many diseases and conditions, including kidney disease. The trials look to find new ways to prevent, detect, or treat disease and improve quality of life.
What are clinical trials for CKD?
Clinical trials—and other types of clinical studies—are part of medical research and involve people like you. When you volunteer to take part in a clinical study, you help doctors and researchers learn more about disease and improve health care for people in the future.
Researchers are studying many aspects of CKD, such as
- genetics and CKD
- the relationship between kidney disease and heart disease
- new ways to slow or prevent progression of CKD
Find out if clinical studies are right for you.
Watch a video of NIDDK Director Dr. Griffin P. Rodgers explaining the importance of participating in clinical trials.
What clinical studies for CKD are looking for participants?
You can view a filtered list of clinical studies on CKD that are federally funded, open, and recruiting at ClinicalTrials.gov. You can expand or narrow the list to include clinical studies from industry, universities, and individuals; however, the National Institutes of Health does not review these studies and cannot ensure they are safe for you. Always talk with your health care provider before you participate in a clinical study.
What have we learned about CKD from NIDDK-funded research?
NIDDK has supported many research projects to learn more about CKD. For example, NIDDK’s Chronic Renal Insufficiency Study (CRIC) and Chronic Kidney Disease in Children Study (CKiD) are examining the risk factors for progression of CKD and the link between CKD and cardiovascular disease in adults and children. Additionally, NIDDK’s Kidney Precision Medicine Project is exploring novel therapies for the treatment of kidney disease.
References
Causes of CKD
What are the most common causes of CKD in adults?
The most common causes of chronic kidney disease (CKD) in adults are diabetes and high blood pressure.
Diabetes
High blood glucose levels, also called blood sugar levels, can damage your kidneys’ filters. Over time, your kidneys can become so damaged that they no longer do a good job filtering waste and extra fluid from your blood. Damaged kidneys can allow proteins your body needs to pass out of your blood and into your urine.
Kidney disease caused by diabetes is called diabetic kidney disease.
High blood pressure
High blood pressure can damage blood vessels and other parts of the filtering system in the kidneys. If these parts of the kidneys’ filtering system are damaged, your kidneys may not work as well to remove waste and extra fluid from your body. Extra fluid in your body can raise your blood pressure even more, creating a dangerous cycle.
 High blood pressure can damage blood vessels in your kidneys.
High blood pressure can damage blood vessels in your kidneys.
What else can cause CKD in adults?
Other causes of CKD in adults include
- acute kidney injury
- certain cancers and related conditions, such as multiple myeloma
- disorders in which the body’s immune system attacks its own cells and organs, such as systemic lupus erythematosus and anti-glomerular basement membrane, also called Goodpasture’s disease
- drugs that are toxic to the kidneys
- glomerular diseases, such as membranous nephropathy, focal segmental glomerulosclerosis, immunoglobulin A (IgA) nephropathy, and IgA vasculitis
- hemolytic uremic syndrome and thrombotic thrombocytopenic purpura
- hepatorenal syndrome and cardiorenal syndrome, in which liver disease or heart disease damages the kidneys
- infections
- kidney stones with complications
- metabolic syndrome
- polycystic kidney disease
- rare genetic conditions, such as Alport syndrome and uromodulin-associated kidney disease
- renal artery stenosis
- severe obesity
- sickle cell disease
Knowing the cause of your CKD can help you and your health care team develop a plan to manage your CKD and protect your kidneys from more damage. Taking steps to manage your CKD may also help to prevent or delay other health problems, such as heart disease.
Clinical Trials for CKD in Adults
NIDDK conducts and supports clinical trials in many diseases and conditions, including kidney disease. The trials look to find new ways to prevent, detect, or treat disease and improve quality of life.
What are clinical trials for CKD?
Clinical trials—and other types of clinical studies—are part of medical research and involve people like you. When you volunteer to take part in a clinical study, you help doctors and researchers learn more about disease and improve health care for people in the future.
Researchers are studying many aspects of the causes of CKD, such as
- disease pathways that lead to CKD
- how our environment and social factors affect gene variants linked to an increased risk of developing kidney disease
- rare, atypical, and other forms of kidney disease that we don’t fully understand yet
Find out if clinical studies are right for you.
Watch a video of NIDDK Director Dr. Griffin P. Rodgers explaining the importance of participating in clinical trials.
What clinical studies for CKD are looking for participants?
You can find clinical studies on the causes of CKD at ClinicalTrials.gov. In addition to searching for federally funded studies, you can expand or narrow the list to include clinical studies from industry, universities, and individuals; however, the National Institutes of Health does not review these studies and cannot ensure they are safe for you. Always talk with your health care provider before you participate in a clinical study.
Tests & Diagnosis
How can I tell if I have kidney disease?
Early kidney disease usually doesn’t have any symptoms. Testing is the only way to know how well your kidneys are working. Get checked for kidney disease if you have
- diabetes
- high blood pressure
- heart disease
- a family history of kidney failure
If you have diabetes, get checked every year. If you have high blood pressure, heart disease, or a family history of kidney failure, talk with your health care provider about how often you should get tested. The sooner you know you have kidney disease, the sooner you can get treatment to help protect your kidneys.
What tests do doctors use to diagnose and monitor kidney disease?
To check for kidney disease, health care providers use
- a blood test that checks how well your kidneys are filtering your blood, called GFR. GFR stands for glomerular filtration rate.
- a urine test to check for albumin. Albumin is a protein that can pass into the urine when the kidneys are damaged.
If you have kidney disease, your health care provider will use the same two tests to help monitor your kidney disease and make sure your treatment plan is working.
Watch a video on how to check for kidney disease.
Blood test for GFR
Your health care provider will use a blood test to check your kidney function. The results of the test mean the following:
- a GFR of 60 or more is in the normal range. Ask your health care provider when your GFR should be checked again.
- a GFR of less than 60 may mean you have kidney disease. Talk with your health care provider about how to keep your kidney health at this level.
- a GFR of 15 or less is called kidney failure. Most people below this level need dialysis or a kidney transplant. Talk with your health care provider about your treatment options.
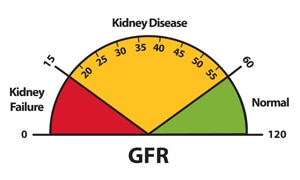
You can’t raise your GFR, but you can try to keep it from going lower. Learn more about what you can do to keep your kidneys healthy.
Creatinine. Creatinine is a waste product from the normal breakdown of muscles in your body. Your kidneys remove creatinine from your blood. Providers use the amount of creatinine in your blood to estimate your GFR. As kidney disease gets worse, the level of creatinine goes up.
Urine Test for Albumin
If you are at risk for kidney disease, your provider may check your urine for albumin.
Albumin is a protein found in your blood. A healthy kidney doesn’t let albumin pass into the urine. A damaged kidney lets some albumin pass into the urine. The less albumin in your urine, the better. Having albumin in the urine is called albuminuria.
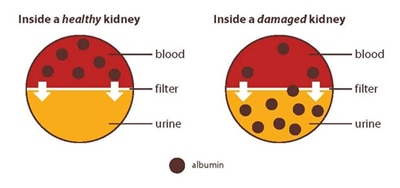
A health care provider can check for albumin in your urine in two ways:
Dipstick test for albumin. A provider uses a urine sample to look for albumin in your urine. You collect the urine sample in a container in a health care provider’s office or lab. For the test, a provider places a strip of chemically treated paper, called a dipstick, into the urine. The dipstick changes color if albumin is present in the urine.
Urine albumin-to-creatinine ratio (UACR). This test measures and compares the amount of albumin with the amount of creatinine in your urine sample. Providers use your UACR to estimate how much albumin would pass into your urine over 24 hours. A urine albumin result of
- 30 mg/g or less is normal
- more than 30 mg/g may be a sign of kidney disease
If you have albumin in your urine, your provider may want you to repeat the urine test one or two more times to confirm the results. Talk with your provider about what your specific numbers mean for you.
If you have kidney disease, measuring the albumin in your urine helps your provider know which treatment is best for you. A urine albumin level that stays the same or goes down may mean that treatments are working.
How do I know if my kidney disease is getting worse?
You can keep track of your test results (PDF, 262 KB) over time. You can tell that your treatments are working if your
- GFR stays the same
- urine albumin stays the same or goes down
Your health care provider will work with you to manage your kidney disease.
Managing CKD
If you have chronic kidney disease (CKD), you can take steps to protect your kidneys from more damage.
The sooner you know you have kidney disease, the better. The steps you take to protect your kidneys from damage also may help prevent heart disease—and improve your health overall. Making these changes when you have no symptoms may be hard, but it’s worthwhile.
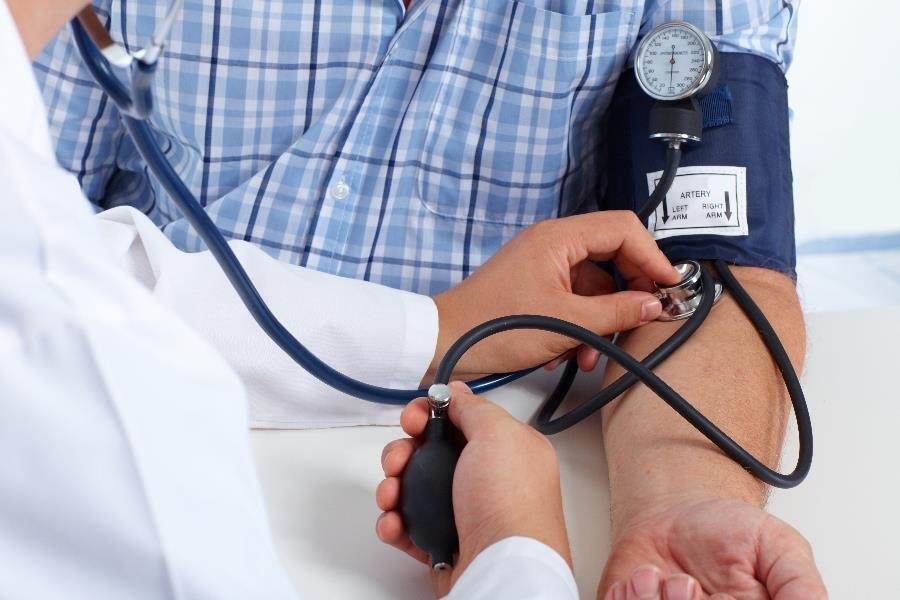
Control your blood pressure
The most important step you can take to treat kidney disease is to control your blood pressure. High blood pressure can damage your kidneys. You can protect your kidneys by keeping your blood pressure at or less than the goal set by your health care provider. For most people, the blood pressure goal is less than 140/90 mm Hg.
Work with your health care provider to develop a plan to meet your blood pressure goals. Steps you can take to meet your blood pressure goals may include eating heart-healthy and low-sodium meals, quitting smoking, being active, getting enough sleep, and taking your medicines as prescribed.
Meet your blood glucose goal if you have diabetes
To reach your blood glucose goal, check your blood glucose level regularly. Use the results to guide decisions about food, physical activity, and medicines. Ask your health care provider how often you should check your blood glucose level.
Your health care provider will also test your A1C. The A1C is a blood test that measures your average blood glucose level over the past 3 months. This test is different from the blood glucose checks you do regularly. The higher your A1C number, the higher your blood glucose levels have been during the past 3 months. Stay close to your daily blood glucose numbers to help you meet your A1C goal.
The A1C goal for many people with diabetes is below 7 percent. Ask your health care provider what your goal should be. Reaching your goal numbers will help you protect your kidneys. Learn more about how to manage diabetes.
Work with your health care team to monitor your kidney health
The tests that health care providers use to test for kidney disease can also be used to track changes to kidney function and damage. Kidney disease tends to get worse over time. Each time you get checked, ask your provider how the test results compare to the last results. Your goals will be to
- keep your GFR the same
- keep your urine albumin the same or lower
Your health care provider will also check your blood pressure and, if you have diabetes, your A1C level, to make sure you are meeting your blood pressure and blood glucose goals.
Bring this document to your appointment to help keep track of your kidney test results (PDF, 262 KB) .
How can I prepare for visits with my health care provider?
The more you plan for your visits, the more you will be able to learn about your health and treatment options.
Make a list of questions
It’s normal to have a lot of questions. Write down your questions as you think of them so that you can remember everything you want to ask when you see your health care provider. You may want to ask about what tests are being done, what test results mean, or the changes you need to make to your diet and medicines.
Sample questions to ask your provider for people with kidney disease
About your tests
- What is my GFR? What does that mean?
- Has my GFR changed since last time?
- What is my urine albumin? What does it mean?
- Has my urine albumin changed since the last time it was checked?
- Is my kidney disease getting worse?
- Is my blood pressure where it needs to be?
About treatment and self-care
- What can I do to keep my disease from getting worse?
- Do any of my medicines or doses need to be changed?
- What time of day should I take each of my medicines?
- Do I need to change what I eat?
- Will you refer me to a dietitian for diet counseling?
- When will I need to see a nephrologist (kidney specialist)?
- Do I need to worry about dialysis or a kidney transplant?
- What do I need to do to protect my veins?
About complications
- What other health problems may I face because of my kidney disease?
- Should I be looking for any symptoms? If so, what are they?
Bring a friend or relative with you for support
A trusted friend or family member can take notes, ask questions you may not have thought of, offer support, and help remember what the provider said during the visit. Talk ahead of time about what you want to get out of the visit and the role you would like your friend or relative to play.
Who is part of my health care team?
The following health care providers may be part of the health care team involved in your treatment:

Primary care provider. Your primary care provider (PCP)—doctor, nurse practitioner, or physician assistant—is the person you see for routine medical visits. Your PCP may monitor your kidney health and help you manage your diabetes and high blood pressure. A PCP also prescribes medicines and may refer you to specialists.
Nurse. A nurse may help with your treatment and teach you about monitoring and treating kidney disease, as well as managing your health conditions. Some nurses specialize in kidney disease.
Registered dietitian. A registered dietitian is a food and nutrition expert who helps people create a healthy eating plan when they have a health condition such as kidney disease. Dietitians can help you by creating an eating plan based on how your kidneys are doing. “Renal dietitians” often work in dialysis centers and are specially trained to work with people with kidney failure.
Diabetes educator. A diabetes educator teaches people with diabetes how to manage their disease and handle diabetes-related problems.
Pharmacist. A pharmacist educates you about your medicines and fills your prescriptions. An important job for the pharmacist is to review all of your medicines, including over-the-counter (OTC) medicines, and supplements, to avoid unsafe combinations and side effects.
Social worker. When you are close to needing dialysis, you may have a chance to meet with a social worker. A dialysis social worker helps people and their families deal with the life changes and costs that come with having kidney disease and kidney failure. A dialysis social worker also can help people with kidney failure apply for help to cover treatment costs.
Nephrologist. A nephrologist is a doctor who is a kidney specialist. Your PCP may refer you to a nephrologist if you have a complicated case of kidney disease, your kidney disease is quickly getting worse, or your kidney disease is advanced.
Take medicines as prescribed
Many people with CKD take medicines prescribed to lower blood pressure, control blood glucose, and lower cholesterol.
Two types of blood pressure medicines, ACE inhibitors and ARBs, may slow kidney disease and delay kidney failure, even in people who don’t have high blood pressure. The names of these medicines end in –pril or –sartan.
Many people need to take two or more medicines for their blood pressure. You may also need to take a diuretic, sometimes called a water pill. The aim is to meet your blood pressure goal. These medicines may work better if you limit your salt intake.
Know that your medicines may change over time
Your health care provider may change your medicines as your kidney disease gets worse. Your kidneys don’t filter as well as they did in the past, and this can cause an unsafe buildup of medicines in your blood. Some medicines can also harm your kidneys. As a result, your provider may tell you to
- take a medicine less often or take a smaller dose
- stop taking a medicine or switch to a different one
Your pharmacist and health care provider need to know about all the medicines you take, including OTC medicines, vitamins, and supplements.

Be careful about the over-the-counter medicines you take
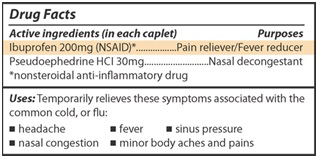
If you take OTC or prescription medicines for headaches, pain, fever, or colds, you may be taking nonsteroidal anti-inflammatory drugs (NSAIDs). NSAIDs include commonly used pain relievers and cold medicines that can damage your kidneys and lead to acute kidney injury, especially in those with kidney disease, diabetes, and high blood pressure.
Ibuprofen and naproxen are NSAIDs. NSAIDs are sold under many different brand names, so ask your pharmacist or health care provider if the medicines you take are safe to use.
You also can look for NSAIDs on Drug Facts labels like the one below:
Watch a video explaining how NSAIDs can harm your kidneys.
If you have been taking NSAIDs regularly to control chronic pain, you may want to ask your health care provider about other ways to treat pain, such as meditation or other relaxation techniques. You can read more about pain management at the NIH National Center for Complementary and Integrative Health website.
Tips for managing your medicines
The next time you pick up a prescription or buy an OTC medicine or supplement, ask your pharmacist how the product may
- affect your kidneys
- affect other medicines you take
Fill your prescriptions at only one pharmacy or pharmacy chain so your pharmacist can
- keep track of your medicines and supplements
- check for harmful interactions
Keep track of your medicines and supplements:
- Keep an up-to-date list of your medicines and supplements in your wallet. Take your list with you, or bring all of your medicine bottles, to all health care visits.

Work with a dietitian to develop a meal plan
What you eat and drink can help you
- protect your kidneys
- reach your blood pressure and blood glucose goals
- prevent or delay health problems caused by kidney disease
As your kidney disease gets worse, you may need to make more changes to what you eat and drink.
A dietitian who knows about kidney disease can work with you to create a meal plan that includes foods that are healthy for you and that you enjoy eating. Cooking and preparing your food from scratch can help you eat healthier.
Nutrition counseling from a registered dietitian to help meet your medical or health goals is called medical nutrition therapy (MNT). If you have diabetes or kidney disease and a referral from your primary care provider, your health insurance may cover MNT. If you qualify for Medicare, MNT is covered.
Your health care provider may be able to refer you to a dietitian. You can also find a registered dietitian online through the Academy of Nutrition and Dietetics. Work closely with your dietitian to learn to eat right for CKD.
Make physical activity part of your routine
Be active for 30 minutes or more on most days. Physical activity can help you reduce stress, manage your weight, and achieve your blood pressure and blood glucose goals. If you are not active now, ask your health care provider about the types and amounts of physical activity that are right for you.
View physical activity and weight-management resources to help you get and stay motivated.
Aim for a healthy weight
Being overweight makes your kidneys work harder and may damage your kidneys. The NIH Body Weight Planner is an online tool to help you tailor your calorie and physical activity plans to achieve and stay at a healthy weight.
Get enough sleep
Aim for 7 to 8 hours of sleep each night. Getting enough sleep is important to your overall physical and mental health and can help you meet your blood pressure and blood glucose goals. You can take steps to improve your sleep habits.
Stop smoking
Cigarette smoking can make kidney damage worse. Quitting smoking may help you meet your blood pressure goals, which is good for your kidneys, and can lower your chances of having a heart attack or stroke. For tips on quitting, go to Smokefree.gov.
Find healthy ways to cope with stress and depression
Long-term stress can raise your blood pressure and your blood glucose and lead to depression. Some of the steps that you are taking to manage your kidney disease are also healthy ways to cope with stress. For example, physical activity and sleep help reduce stress. Listening to your favorite music, focusing on something calm or peaceful, or meditating may also help you. Learn more about healthy ways to cope with stress.
Depression is common among people with a chronic, or long-term, illness. Depression can make it harder to manage your kidney disease. Ask for help if you feel down. Seek help from a mental health professional. Talking with a support group, clergy member, friend, or family member who will listen to your feelings may help.
Healthy Eating
In this section:
- Why is healthy eating important for adults with CKD?
- What aspects of nutrition are important for adults with CKD?
- How can I eat healthy with CKD?
- What is medical nutrition therapy?
- Clinical Trials for Healthy Eating for Adults with CKD
Why is healthy eating important for adults with CKD?
Healthy kidneys balance salts and minerals in the blood. When you have chronic kidney disease (CKD), the kidneys can’t filter your blood the way they should. What you eat and drink can help your kidneys maintain a healthy balance of salts and minerals in your body and help you feel better.
Choosing healthy foods and beverages—and avoiding foods high in sodium, potassium, and phosphorus—may prevent or delay some health problems from CKD. What you eat and drink may also affect how well your kidney disease treatments work. Understanding how different nutrients and liquids affect the body is important for people with CKD.
As CKD advances, nutritional needs change. Your health care professional may recommend you choose foods more carefully and may suggest you work with a registered dietitian, if possible, to create an eating plan for your individual needs. You can find a registered dietitian who specializes in kidney disease through the Academy of Nutrition and Dietetics online or through your health care professional.
What aspects of nutrition are important for adults with CKD?
Calories
The foods and beverages you eat and drink give your body energy. The energy is measured in calories. If you consume fewer calories than your body uses, you may lose weight. Losing too much weight can make you sicker.
Fat
Fat gives your body energy, helps control your cholesterol and blood pressure levels, and helps your body absorb vitamins. Fat also provides nutrients your body needs and is an important part of a healthy eating plan.
Everyone needs some fat in their diet, but too much fat or choosing foods higher in saturated fat or trans fat may cause buildup in your blood vessels, heart, and kidneys. People with CKD have a higher risk of developing heart and blood vessel disease and should focus on consuming healthier unsaturated fats while limiting saturated and trans fats.
Liquids
Your body needs liquids to function properly. However, people with CKD may need to limit how much liquid they consume because damaged kidneys can’t remove extra fluid. Talk with your health care professional about how much liquid you should have each day.
Phosphorus
Damaged kidneys can’t remove phosphorus from the blood as well as healthy kidneys can. Phosphorus can build up in the blood in people with CKD. Too much phosphorus in your blood can harm your blood vessels and make your bones thin, weak, and more likely to break. High levels of phosphorus in your blood can also cause itchy skin and bone and joint pain.
Potassium
CKD can make it harder for the kidneys to remove potassium from the blood, and the potassium levels in the blood can become very high. Having too little or too much potassium in your blood can cause heart and muscle problems. For this reason, it’s important to work with a dietitian or health care professional to help find the right amount of potassium for you.
Protein
Protein helps build and maintain muscle, bone, skin, connective tissue, internal organs, and blood. Protein also helps fight disease and heal wounds.
As your body uses protein, the protein breaks down into waste. Your kidneys remove this waste from the blood. Some people with CKD may need to consume moderate amounts of protein so waste doesn’t build up in the blood. However, too little protein may lead to malnutrition, a condition that occurs when your body doesn’t get enough nutrients. Work with a dietitian or health care professional to find the right balance of protein to make sure you are properly nourished without causing strain to your kidneys.
Sodium
Sodium is a mineral that helps control the amount of fluids in your body. Sodium is found in table salt and in many processed foods.
Too much sodium causes your blood to retain—or hold on to—fluids. When your body retains fluids, it can cause high blood pressure and swelling, putting stress on your kidneys and heart. Be aware of the amount of sodium in the foods and beverages you consume and work with your dietitian or health care professional to determine your sodium limit.
 Eating healthy with CKD can help your kidneys maintain a healthy balance of salts and minerals in your body and can help you feel better.
Eating healthy with CKD can help your kidneys maintain a healthy balance of salts and minerals in your body and can help you feel better.
How can I eat healthy with CKD?
There is no single meal plan for everyone with CKD. In the early stages of CKD, you may have few limits to what you can eat and drink. As your CKD advances and your nutritional needs change, you may need to make more changes to your diet.
Talk with your health care team about challenges you may have finding healthy food. A health care professional, dietitian, or social worker may be able to recommend resources that can help you. The U.S. Department of Agriculture also has a list of resources for finding and affording healthy food.
Pay attention to calories
People with CKD may avoid eating because they don’t feel hungry or because foods or beverages don’t taste the same. If you find that you don’t feel like eating, talk with a dietitian or health care professional to make sure you are getting enough calories and that the calories are from nutritious sources. Your dietitian or health care professional can help you find healthy ways to get the calories your body needs.
Choose heart-healthy foods
You may protect your heart health and lower your chance of developing heart and blood vessel disease by replacing saturated fats and trans fats in your diet with healthier unsaturated fats, which include monounsaturated fats and polyunsaturated fats.
Monounsaturated fats and polyunsaturated fats—found in foods such as canola oil, safflower oil, avocados, nuts, and seeds—are healthy alternatives to saturated fats and trans fats. Saturated fats and trans fats can raise cholesterol levels and clog blood vessels.
Saturated fats, which are found in animal products such as red meat, poultry, and butter, are usually solid at room temperature. Trans fats can be found in fast foods, fried foods, commercially produced baked goods, and other foods cooked with partially hydrogenated or hydrogenated oil or shortening.
Tips for following a heart-healthy diet include
- Choose heart-healthy foods, including plenty of fruits and vegetables.
- Grill, broil, bake, roast, air-fry, or stir-fry foods, instead of deep-frying.
- Cook with nonstick cooking spray or a small amount of olive oil instead of butter.
- Trim fat from meat and remove skin from poultry before eating.
- Limit saturated and trans fats. Look for the amount of saturated fat and trans fat on the Nutrition Facts label.
- Limit alcohol. Ask your health care professional how much alcohol is safe for you.
Talk with your dietitian or health care professional about healthy ways you can include fat in your diet.
Track your liquids
You may need to adjust how much liquid you have each day, depending on your kidney function. A dietitian or health care professional can work with you to determine how much liquid you should have each day. Contact your health care professional if you notice any swelling in your face, arms, legs, or abdomen.
Choose foods and drinks with less phosphorus
Phosphorus is found naturally in foods that are rich in protein, such as meat, dairy products, and beans. Phosphorus is also added to many foods. Phosphorus additives are the primary source of phosphorus for many people.
Tips to reduce phosphorus in your diet include
- Limit or avoid packaged and processed foods and drinks that have added phosphorus, such as deli meats, flavored drinks, and other processed foods.
- Check Nutrition Facts labels for added phosphorus. Look for “phosphorus” or words with “PHOS,” such as phosphoric acid, disodium phosphate, and monosodium phosphate on the ingredient list.
- Eat larger portions of fruits and vegetables, which are naturally low in phosphorus, and smaller portions of foods high in phosphorus.
- Keep in mind, your body absorbs more phosphorus from animal-based foods, such as meat and poultry, than from plant-based foods, such as beans and seeds.
- Some packaged meats and poultry have added phosphorus. Ask someone who works in the meat department to show you which meats do not have added phosphorus.
A health care professional can check your blood phosphorus level using a blood test. Foods and drinks with added phosphorus may cause your blood phosphorus level to go up more than foods and drinks that naturally contain phosphorus. Your dietitian or health care professional may suggest changes to what you eat and drink to help keep your phosphorus level in a healthy range.
As kidney disease advances, you may need to take a phosphate binder with meals to lower the amount of phosphorus in your blood. A phosphate binder is a medicine that acts like a sponge to soak up, or bind, phosphorus while it is in the stomach. Because it is bound, the phosphorus does not get into your blood. Instead, your body removes the phosphorus through your stool.
Choose foods that help keep your potassium level in the goal range
Your food and drink choices can help you keep your potassium level in a healthy range.
If your potassium level is high, your health care professional may recommend you
- Limit serving sizes of foods that contain potassium. Keep in mind that a large serving of a lower-potassium food may have more potassium than a small serving of a higher-potassium food.
- Use spices and herbs instead of salt substitutes, which can be high in potassium.
- Limit foods with potassium chloride on the ingredient list. Potassium chloride is sometimes used in place of salt in some packaged foods.
- Drain canned fruits and vegetables and throw out the liquid, which is often high in potassium.
- Use food preparation and cooking methods, such as boiling and leaching, that can lower the amount of potassium in certain vegetables.
- If you have diabetes and your blood glucose level—also called blood sugar level—gets low, choose apple, grape, or cranberry juice instead of other fruit juices that are higher in potassium, such as orange juice.
A health care professional can check your potassium level using a blood test. Talk with your dietitian or health care professional about ways you can adjust your food and drink choices to meet your potassium goal.
Your health care professional may suggest you take a potassium binder to lower the amount of potassium in your blood. Similar to phosphate binders, potassium binders are medicines that prevent some potassium from getting into the blood. The potassium is removed from the body through your stool.
Taking certain medicines, as well as skipping dialysis treatments, can also raise your potassium level. Your health care professional may adjust the medicines you take if your potassium level is too high. If you receive dialysis treatments, be sure to attend all dialysis sessions to help prevent potassium from building up in your blood.
 Talk with your dietitian or health care professional about changes you can make to what you eat and drink if your CKD gets worse.
Talk with your dietitian or health care professional about changes you can make to what you eat and drink if your CKD gets worse.
Choose the amount and types of protein your body needs
Protein is in many foods you eat, including foods from plants and animals. You may need to adjust the amount of protein in your diet to help keep your kidneys healthier longer. Your protein needs may also change over time.
Work with your dietitian or health care professional to find the amount and sources of
protein you should include in your diet. Your health care professional may recommend you
- limit how much meat and dairy foods you consume
- get the rest of your protein from plant-based foods
- choose lean, or low-fat, meats that also are low in phosphorus
If you don’t eat animal products, eat a variety of plant-based proteins to meet your body’s protein needs.
People with CKD who are on dialysis may need to eat more protein because the dialysis treatment removes protein from the blood. The amount of protein removed from the blood depends on the type of dialysis treatment. For example, peritoneal dialysis removes more protein than hemodialysis.
 Talk with your dietitian or health care professional about the amount and sources of protein you should include in your diet.
Talk with your dietitian or health care professional about the amount and sources of protein you should include in your diet.
Choose and prepare foods with less salt and sodium
Most Americans consume more sodium than they should. Much of this sodium comes from packaged, prepared, and restaurant foods, not from a saltshaker. Even foods that don’t taste salty can be high in sodium.
Canned foods, some frozen foods, and most processed meats contain large amounts of salt. Snack foods such as chips and crackers are also high in salt. Table salt, some seasonings, ketchup, mustard, and certain sauces such as barbecue, soy, and teriyaki sauces are high in sodium.
The 2020–2025 Dietary Guidelines for Americans recommends adults limit their sodium to no more than 2,300 milligrams per day.1 Many people with CKD need to limit their sodium even more. Your health care professional can determine your sodium limit, based on your kidney health.
Tips to reduce sodium in your diet include
- Limit the amount of prepared, packaged, and fast foods you eat.
- Choose unprocessed meats instead of processed meats.
- Check for sodium on the Nutrition Facts label of food packages. A % Daily Value of 20% or more means the food is high in sodium, and a value of 5% or less means the food is low in sodium.
- Look for foods labeled sodium free, salt free, very low sodium, low sodium, reduced or less sodium, no salt added, unsalted, or lightly salted.
- Eat more fresh, frozen, and canned fruits and vegetables without added sauce, seasonings, sodium, or salt.
- Drain and rinse canned vegetables, beans, meats, and fish with water to remove extra salt.
- Cook foods from scratch. When you prepare your own food, you control what goes into it.
- Use spices, herbs, and sodium-free seasonings in place of salt. Use alternative seasonings, such as lemon juice, herbs, and hot peppers.
Try slowly reducing the amount of sodium in your diet over time. Your taste buds will gradually adjust, and you won’t notice the change in flavor.
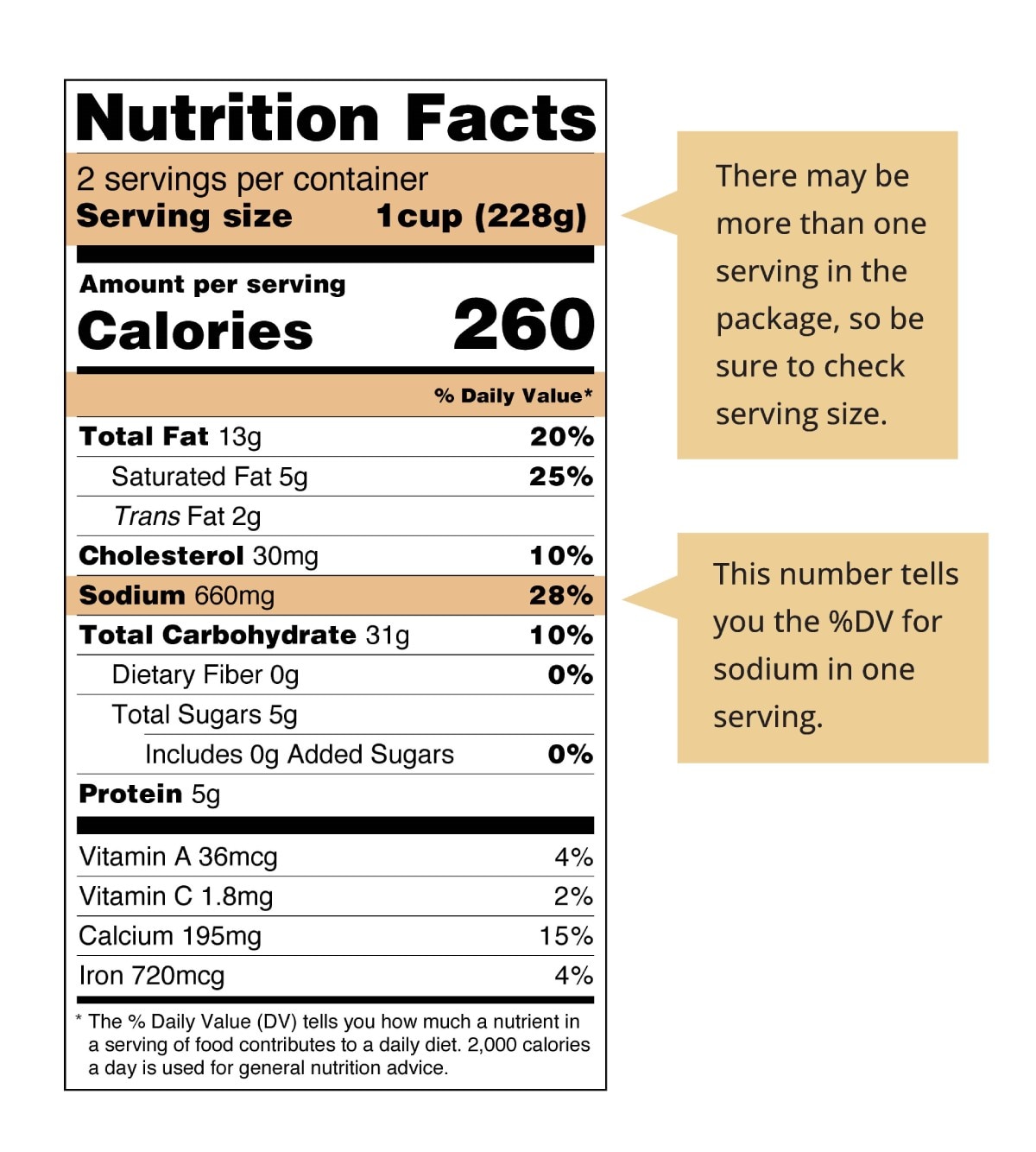 Look for the serving size and sodium on the Nutrition Facts label. A label showing % Daily Value (%DV) of 5% or less per serving is considered low in sodium.
Look for the serving size and sodium on the Nutrition Facts label. A label showing % Daily Value (%DV) of 5% or less per serving is considered low in sodium.
What is medical nutrition therapy?
Medical nutrition therapy (MNT) is nutrition counseling from a registered dietitian to help meet your medical or health goals. MNT can help delay CKD progression, prevent or treat complications, and improve your quality of life.
Medicare and insurance coverage for MNT
If you are enrolled in Medicare and have CKD, Medicare will cover MNT services. You will need a written referral from a doctor, and the MNT must be provided by a registered dietitian.
If you have health insurance, check your insurance company’s website or call customer service to find out if your insurance will pay for some or all MNT. If you don’t have insurance or Medicare, ask a health care professional about the cost of a dietitian’s services. A health care professional may be able to connect you with organizations that can help cover the cost of nutrition counseling.
Clinical Trials for Healthy Eating for Adults with CKD
NIDDK conducts and supports clinical trials in many diseases and conditions, including kidney disease. The trials look to find new ways to prevent, detect, or treat disease and improve quality of life.
What are clinical trials for healthy eating for adults with CKD?
Clinical trials—and other types of clinical studies—are part of medical research and involve people like you. When you volunteer to take part in a clinical study, you help doctors and researchers learn more about disease and improve health care for people in the future.
Researchers are studying many aspects of healthy eating for adults with CKD, such as
- the impact of MNT on CKD progression
- how anti-inflammatory diets affect patients with CKD
- the relationship between protein intake and CKD progression
Find out if clinical studies are right for you.
Watch a video of NIDDK Director Dr. Griffin P. Rodgers explaining the importance of participating in clinical trials.
What clinical studies for healthy eating for adults with CKD are looking for participants?
You can find clinical studies on CKD at ClinicalTrials.gov. In addition to searching for federally funded studies, you can expand or narrow your search to include clinical studies from industry, universities, and individuals; however, the National Institutes of Health does not review these studies and cannot ensure they are safe for you. Always talk with your health care provider before you participate in a clinical study.
Reference
Preventing CKD
You are more likely to develop kidney disease if you have
- diabetes
- high blood pressure
- heart disease
- a family history of kidney failure
What can I do to keep my kidneys healthy?
You can protect your kidneys by preventing or managing health conditions that cause kidney damage, such as diabetes and high blood pressure. The steps described below may help keep your whole body healthy, including your kidneys.
During your next medical visit, you may want to ask your health care provider about your kidney health. Early kidney disease may not have any symptoms, so getting tested may be the only way to know your kidneys are healthy. Your health care provider will help decide how often you should be tested.
See a provider right away if you develop a urinary tract infection (UTI), which can cause kidney damage if left untreated.
Make healthy food choices
Choose foods that are healthy for your heart and your entire body: fresh fruits, fresh or frozen vegetables, whole grains, and low-fat or fat-free dairy products. Eat healthy meals, and cut back on salt and added sugars. Aim for less than 2,300 milligrams of sodium each day. Try to have less than 10 percent of your daily calories come from added sugars.

Tips for making healthy food choices
- Cook with a mix of spices instead of salt.
- Choose veggie toppings such as spinach, broccoli, and peppers for your pizza.
- Try baking or broiling meat, chicken, and fish instead of frying.
- Serve foods without gravy or added fats.
- Try to choose foods with little or no added sugar.
- Gradually work your way down from whole milk to 2 percent milk until you’re drinking and cooking with fat-free (skim) or low-fat milk and milk products.
- Eat foods made from whole grains—such as whole wheat, brown rice, oats, and whole-grain corn—every day. Use whole-grain bread for toast and sandwiches; substitute brown rice for white rice for home-cooked meals and when dining out.
- Read food labels. Choose foods low in saturated fats, trans fats, cholesterol, salt (sodium), and added sugars.
- Slow down at snack time. Eating a bag of low-fat popcorn takes longer than eating a slice of cake. Peel and eat an orange instead of drinking orange juice.
- Try keeping a written record of what you eat for a week. It can help you see when you tend to overeat or eat foods high in fat or calories.
Research has shown that the DASH eating plan may help you lower your blood pressure. If you have diabetes, high blood pressure, or heart disease, you may want to locate and work with a dietitian to create a meal plan that meets your needs.
Make physical activity part of your routine
Be active for 30 minutes or more on most days. If you are not active now, ask your health care provider about the types and amounts of physical activity that are right for you. Add more activity to your life with these tips to help you get active.
Aim for a healthy weight
The NIH Body Weight Planner is an online tool to help you tailor your calorie and physical activity plans to achieve and stay at a healthy weight.
If you are overweight or have obesity, work with your health care provider or dietitian to create a realistic weight-loss plan. View more weight control and physical activity resources to help you get and stay motivated.
Get enough sleep
Aim for 7 to 8 hours of sleep each night. If you have trouble sleeping, take steps to improve your sleep habits.
Stop smoking
If you smoke or use other tobacco products, stop. Ask for help so you don’t have to do it alone. You can start by calling the national quitline at 1-800-QUITNOW or 1-800-784-8669. For tips on quitting, go to Smokefree.gov.
Limit alcohol intake
Drinking too much alcohol can increase your blood pressure and add extra calories, which can lead to weight gain. If you drink alcohol, limit yourself to one drink per day if you are a woman and two drinks per day if you are a man. One drink is:
- 12 ounces of beer
- 5 ounces of wine
- 1.5 ounces of liquor
Explore stress-reducing activities
Learning how to manage stress, relax, and cope with problems can improve emotional and physical health. Physical activity can help reduce stress, as can mind and body practices such as meditation, yoga, or tai chi.
Manage diabetes, high blood pressure, and heart disease
If you have diabetes, high blood pressure, or heart disease, the best way to protect your kidneys from damage is to
Keep blood glucose numbers close to your goal. Checking your blood glucose, or blood sugar, level is an important way to manage your diabetes. Your health care team may want you to test your blood glucose one or more times a day.
Keep your blood pressure numbers close to your goal. The blood pressure goal for most people with diabetes is below 140/90 mm Hg. Read more about high blood pressure.
Take all your medicines as prescribed. Talk with your health care provider about certain blood pressure medicines, called ACE inhibitors and ARBs, which may protect your kidneys. The names of these medicines end in –pril or –sartan.
Be careful about the daily use of over-the-counter pain medications. Regular use of nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen and naproxen, can damage your kidneys. Learn more about over-the-counter medicines and your kidneys.
To help prevent heart attacks and stroke, keep your cholesterol levels in the target range. There are two kinds of cholesterol in your blood: LDL and HDL. LDL or “bad” cholesterol can build up and clog your blood vessels, which can cause a heart attack or stroke. HDL or “good” cholesterol helps remove the “bad” cholesterol from your blood vessels. A cholesterol test also may measure another type of blood fat called triglycerides.
Ask your health care provider questions
Ask your health care provider the following key questions about your kidney health during your next medical visit. The sooner you know you have kidney disease, the sooner you can get treatment to help protect your kidneys.
Key questions for your health care provider:
- What is my glomerular filtration rate (GFR)?
- What is my urine albumin result?
- What is my blood pressure?
- What is my blood glucose (for people with diabetes)?
- How often should I get my kidneys checked?
Other important questions:
- What should I do to keep my kidneys healthy?
- Do I need to be taking different medicines?
- Should I be more physically active?
- What kind of physical activity can I do?
- What can I eat?
- Am I at a healthy weight?
- Do I need to talk with a dietitian to get help with meal planning?
- Should I be taking ACE inhibitors or ARBs for my kidneys?
- What happens if I have kidney disease?
What If My Kidneys Fail?
Some people live with kidney disease for years and are able to maintain kidney function. Others progress quickly to kidney failure.
Kidney failure means that your kidneys have lost most of their ability to function—less than 15 percent of normal kidney function. If your kidney function drops to this level, you may have symptoms from the buildup of waste products and extra water in your body.
To replace your lost kidney function, you may have one of three treatment options:
End-stage renal disease (ESRD) is kidney failure that is treated by dialysis or kidney transplant.
Some people with kidney failure choose not to have dialysis or a transplant but continue to receive care from their health care team, take medicines, and monitor their diet and lifestyle choices.
Work with your health care team and family to consider your options and choose a treatment that is right for you.
Clinical Trials
The National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) and other components of the National Institutes of Health (NIH) conduct and support basic and clinical research into many diseases and conditions.
What are clinical trials and are they right for you?
Clinical trials are part of clinical research and at the heart of all medical advances. Clinical trials look at new ways to prevent, detect, or treat disease. Researchers also use clinical trials to look at other aspects of care, such as improving the quality of life for people with chronic illnesses. Find out if clinical trials are right for you.
Watch a video of NIDDK Director Dr. Griffin P. Rodgers explaining the importance of participating in clinical trials.
What clinical trials are open?
Clinical trials that are currently open and are recruiting can be viewed at ClinicalTrials.gov.
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
