IgA Nephropathy
On this page:
- What is immunoglobulin A (IgA) nephropathy?
- How common is IgA nephropathy?
- Who is more likely to have IgA nephropathy?
- What are the complications of IgA nephropathy?
- What are the symptoms of IgA nephropathy?
- What causes IgA nephropathy?
- How do health care professionals diagnose IgA nephropathy?
- How do health care professionals treat IgA nephropathy?
- Can I prevent IgA nephropathy?
- How do eating, diet, and nutrition affect IgA nephropathy?
- Clinical Trials for IgA Nephropathy
What is immunoglobulin A (IgA) nephropathy?
IgA nephropathy is an autoimmune disease that occurs when clumps of antibodies are deposited in your kidneys, causing inflammation and kidney damage. Clumps of immunoglobulin A (IgA) and other antibodies damage the glomeruli, tiny blood vessels in your kidneys that filter blood, causing your kidneys to leak blood and protein into your urine. The damage may also lead to the scarring of the nephrons, the filtering units where the glomeruli are located.
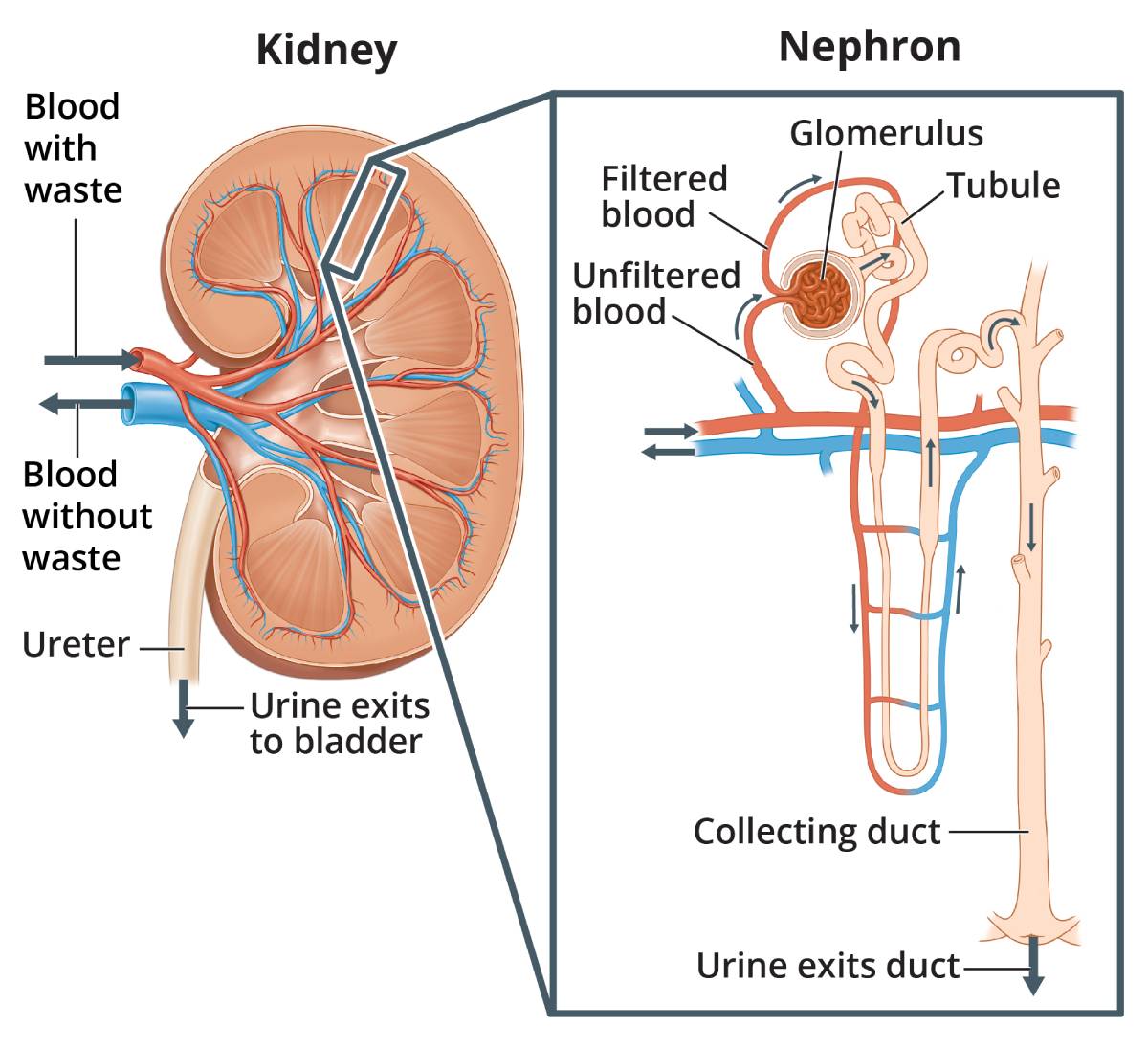 The glomeruli are sets of looping blood vessels in nephrons—the tiny working units of your kidneys that filter wastes and remove extra fluids from your blood.
The glomeruli are sets of looping blood vessels in nephrons—the tiny working units of your kidneys that filter wastes and remove extra fluids from your blood.
Does IgA nephropathy have another name?
IgA nephropathy is also known as Berger’s disease.
How common is IgA nephropathy?
IgA nephropathy is a common kidney disease, and an important cause of chronic kidney disease and kidney failure.1 About 1 in 10 kidney biopsies in the United States show IgA nephropathy.2
Who is more likely to have IgA nephropathy?
IgA nephropathy is more common in people who1–3
- have a family history of the disease or of IgA vasculitis
- have certain health conditions, such as celiac disease, hepatitis, cirrhosis, and HIV infection
- are ages 10 to 40
- are of East Asian or white European ancestry
- are male
What are the complications of IgA nephropathy?
Complications of IgA nephropathy can include3
- high blood pressure, also called hypertension. Damage to your kidneys caused by IgA nephropathy can increase blood pressure. High blood pressure can further damage your kidneys.
- chronic kidney disease—the slow loss of kidney function over many years—which can lead to heart disease or stroke.
- nephrotic syndrome—a group of symptoms that point to kidney damage, including high urine protein levels, low blood protein levels, and high levels of cholesterol and other lipids (fats) in your blood, called hyperlipidemia.
- kidney failure—when your kidneys don’t work well enough to support your body’s needs. Kidney failure can be sudden and temporary—called acute kidney failure—or develop over a long time and be permanent. About 1 in 5 people with IgA nephropathy develop kidney failure within 10 years of diagnosis.2
What are the symptoms of IgA nephropathy?
Symptoms can vary and may not appear for years or even decades. Common signs and symptoms include
- pink or cola-colored urine due to blood in your urine, called gross hematuria or visible hematuria
- foamy urine from protein leaking into your urine, called proteinuria
- swelling due to extra fluid in the legs, feet, ankles, or other parts of your body, called edema
These symptoms are common across diseases and do not, by themselves, suggest that you have IgA nephropathy.
What causes IgA nephropathy?
The cause of IgA nephropathy is unknown, but research suggests that genes and the environment may play a role.2 In some people, the first signs or symptoms of the disease may become noticeable after a cold, sore throat, or other respiratory infection.
How do health care professionals diagnose IgA nephropathy?
Your health care professional will conduct a physical exam, review your symptoms and family history, and order urine and blood tests to find out how well your kidneys are working.
To make a diagnosis, your health care professional will order a kidney biopsy.1 The biopsy can
- show IgA deposits in your glomeruli
- indicate the amount of damage to your kidneys
- help to predict how the disease will affect your kidneys
- help guide treatment
How do health care professionals treat IgA nephropathy?
Health care professionals—in most cases, kidney experts called nephrologists—treat IgA nephropathy with1, 4
- medicines that help reduce blood pressure and loss of protein in the urine. In most cases, your health care professional will prescribe an angiotensin-converting enzyme (ACE) inhibitor or an angiotensin receptor blocker (ARB).
- medicines that lower cholesterol and help prevent heart disease, called statins.
- lifestyle changes. Your health care professional may recommend that you limit sodium (salt) in your diet and quit smoking.
 Health care professionals treat IgA nephropathy with medicines and lifestyle changes.
Health care professionals treat IgA nephropathy with medicines and lifestyle changes.
In some cases, your health care professional may also prescribe immunosuppressants, including corticosteroids. But these medicines can cause serious side effects, such as weight gain or a weakened immune system.
Although researchers have not yet found a cure for IgA nephropathy, treatment can help prevent or delay damage to your kidneys. New treatments are under development, and several are being evaluated in clinical trials.
In many cases, IgA nephropathy does not get worse over time. But if the disease progresses to kidney failure, you may need a kidney transplant or blood-filtering treatments called dialysis.
Can I prevent IgA nephropathy?
You can’t prevent IgA nephropathy. If you have a family history of the disease, ask your health care professional how to keep your kidneys healthy.
How do eating, diet, and nutrition affect IgA nephropathy?
Researchers have not found evidence that eating, diet, and nutrition play a role in causing or preventing IgA nephropathy. If you have IgA nephropathy, limiting the amount of salt in your diet may help reduce swelling and lower blood pressure. Your health care professional may suggest other changes to your diet based on your symptoms, lab test results, and personal needs.
Clinical Trials for IgA Nephropathy
NIDDK conducts and supports clinical trials in many diseases and conditions, including kidney diseases. The trials look to find new ways to prevent, detect, or treat disease and improve quality of life.
What are clinical trials for IgA nephropathy?
Clinical trials—and other types of clinical studies —are part of medical research and involve people like you. When you volunteer to take part in a clinical study, you help doctors and researchers learn more about disease and improve health care for people in the future.
Researchers are studying many aspects of IgA nephropathy, such as
- the role of genes in IgA nephropathy
- why IgA builds up in your kidneys
- new medicines to treat IgA nephropathy
Find out if clinical trials are right for you.
Watch a video of NIDDK Director Dr. Griffin P. Rodgers explaining the importance of participating in clinical trials.
What clinical studies for IgA nephropathy are looking for participants?
You can view a filtered list of clinical studies on IgA nephropathy that are open and recruiting at ClinicalTrials.gov. You can expand or narrow the list to include clinical studies from industry, universities, and individuals; however, NIH does not review these studies and cannot ensure they are safe. Always talk with your health care provider before you participate in a clinical study.
References
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
NIDDK would like to thank:
Bruce A. Julian, M.D., School of Medicine, University of Alabama at Birmingham
