IgA Vasculitis
On this page:
- What is immunoglobulin A (IgA) vasculitis?
- How common is IgA vasculitis?
- Who is more likely to develop IgA vasculitis?
- Are there long-term health problems from IgA vasculitis?
- What are the symptoms of IgA vasculitis?
- What causes IgA vasculitis?
- How do health care professionals diagnose IgA vasculitis?
- What tests do health care professionals use to diagnose or monitor IgA vasculitis?
- How do health care professionals treat IgA vasculitis?
- How can I prevent IgA vasculitis?
- How can my diet help prevent or relieve IgA vasculitis?
- Clinical Trials for IgA Vasculitis
What is immunoglobulin A (IgA) vasculitis?
IgA vasculitis, formerly called Henoch-Schönlein purpura or HSP, is a disease that causes the antibody immunoglobulin A to collect in small blood vessels, which then become inflamed and leak blood. Nearly all people with IgA vasculitis develop a red or purple rash. Some people with IgA vasculitis also develop problems with their gastrointestinal (GI) tract, joints, and kidneys because of inflamed blood vessels in the intestines, joints, and kidneys. In rare cases, the lungs, nervous system, or other organs may be affected.
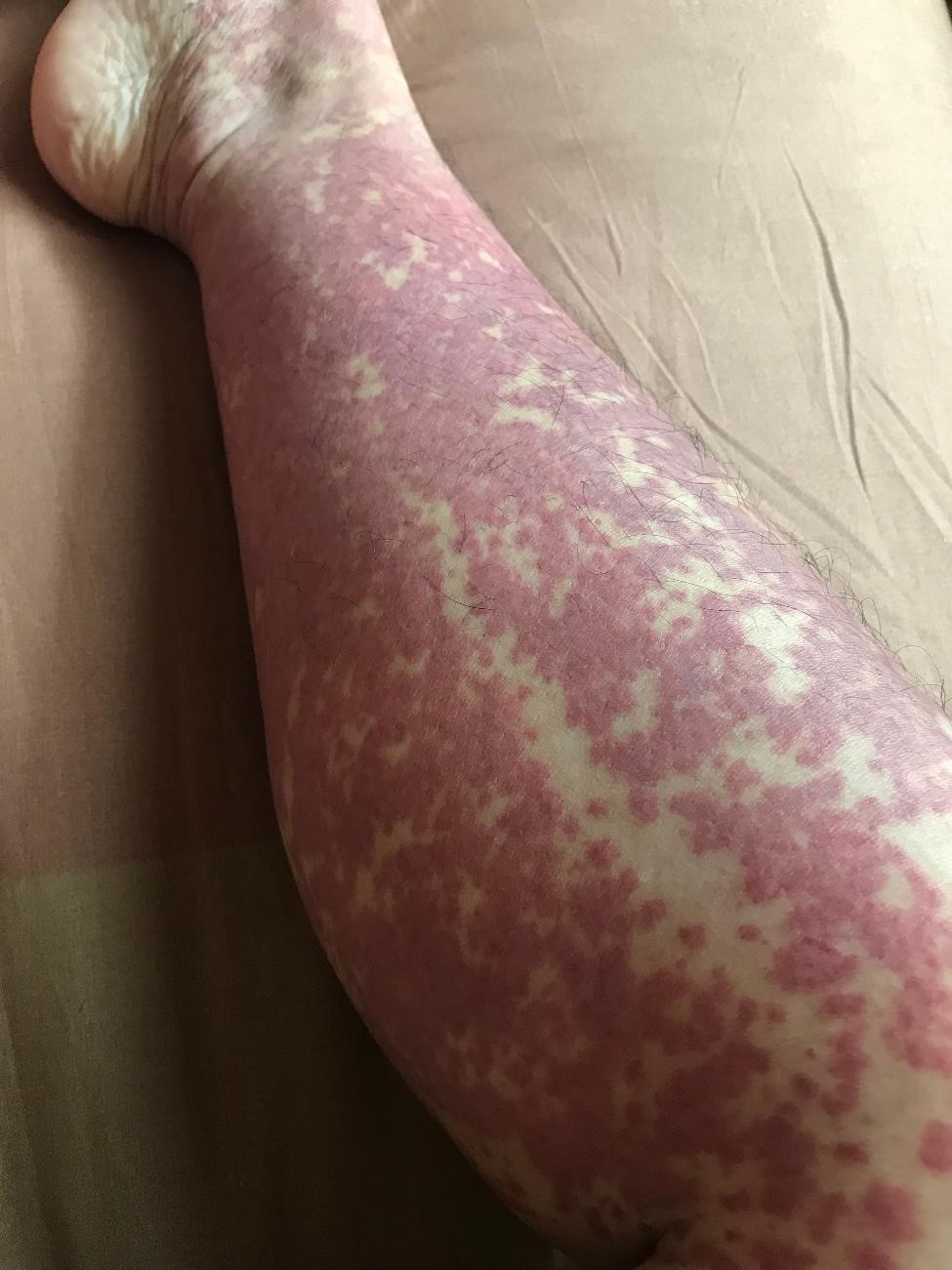 The primary symptom of IgA vasculitis is a raised rash.
The primary symptom of IgA vasculitis is a raised rash.Most people recover from IgA vasculitis completely. However, the disease is sometimes more severe and can lead to acute kidney injury, which can progress to chronic kidney disease (CKD).
How common is IgA vasculitis?
IgA vasculitis is rare. The number of new cases of IgA vasculitis is approximately 3 to 27 cases per 100,000 in children and infants and fewer than 2 new cases per 100,000 each year in adults.1, 2
Who is more likely to develop IgA vasculitis?
IgA vasculitis is most common in young children between the ages of 4 and 7,3 but people of all ages can be affected.
You may be more likely to develop IgA vasculitis if you have a family history of the disease.
Are there long-term health problems from IgA vasculitis?
Most people recover from IgA vasculitis completely without treatment. The symptoms usually go away within a few weeks to months. The symptoms may return one or more times—usually within the first year—but typically go away again on their own.
The most common and serious long-term health problem caused by IgA vasculitis is CKD. Severe kidney damage is rare but, if it does occur, it may require aggressive treatment. Adults are much more likely than children to develop CKD.
Women who have had IgA vasculitis and become pregnant are more likely to develop high blood pressure and have protein in their urine during pregnancy. High blood pressure in pregnancy causes health risks for the mother and baby. Pregnant women with a history of IgA vasculitis should be closely monitored by their health care professional.
 Women with a history of IgA vasculitis who become pregnant should be monitored regularly for high blood pressure and protein in the urine.
Women with a history of IgA vasculitis who become pregnant should be monitored regularly for high blood pressure and protein in the urine.What are the symptoms of IgA vasculitis?
The symptoms of IgA vasculitis include
- Rash. Leaking blood vessels cause a rash that looks like red or purple bruises or small red dots. The rash usually appears on the legs and buttocks, but may also appear on the arms, torso, and face. The rash is raised and does not disappear or turn pale when pressed. The rash is not painful and does not itch.
- GI tract problems. Abdominal pain can range from mild to severe, with nausea or vomiting. Blood may appear in the stool, although the bleeding is usually not severe. In rare cases, more serious problems can occur such as intussusception—a condition in which a section of the bowel folds into itself like a telescope, causing the bowel to become blocked.
- Joint pain and swelling. Pain and swelling often occur in the knees and ankles, and sometimes occur in the elbows, wrists, and small joints of the fingers.
- Kidney problems. Hematuria—blood in the urine—is a common sign that IgA vasculitis has affected the kidneys. Proteinuria—large amounts of protein, including albumin, in the urine—and development of high blood pressure are signs of more severe kidney problems.
- Other symptoms. In some cases, boys with IgA vasculitis develop swelling of the testicles. Symptoms affecting the central nervous system, such as seizures, and lungs, such as pneumonia, have been seen in rare cases.
Rash, abdominal pain, and joint pain and swelling are often the first symptoms to appear, and they can occur in any order. Symptoms involving the kidneys rarely develop first.
What causes IgA vasculitis?
IgA vasculitis occurs when your body’s immune system attacks its own cells and organs. Researchers don’t know what causes this unusual immune system response. However, many people have an infection of the upper respiratory tract—the nose, nasal cavity, pharynx, and larynx—before developing IgA vasculitis. IgA vasculitis has also been linked with
- bacteria and viruses
- foods
- immunizations
- insect bites
- medicines
Certain genes may increase the risk for IgA vasculitis.
How do health care professionals diagnose IgA vasculitis?
Health care professionals use your medical history, a physical exam, and lab tests to confirm your diagnosis of IgA vasculitis.
What tests do health care professionals use to diagnose or monitor IgA vasculitis?
Your health care professional may perform a skin or kidney biopsy, blood and urine tests, and sometimes an ultrasound of the kidneys or abdomen to confirm the diagnosis and monitor your health. In some cases, a kidney biopsy may be used to asses and monitor the severity of the disease. Depending on the organs affected, your health care professional may suggest other tests.
Skin biopsy
Your health care professional may obtain a skin biopsy to test for antibody deposits on your skin and confirm a diagnosis of IgA vasculitis. To do a skin biopsy, the health care professional removes skin cells from your body to examine under a microscope. You will be given a local anesthetic so you don’t feel any pain.
Kidney biopsy
You may also need a kidney biopsy. A kidney biopsy can confirm the diagnosis of IgA vasculitis and provide information on the amount of kidney damage. Your health care professional will use the results of the kidney biopsy to help develop a treatment plan. The kidney biopsy is performed in a hospital with local anesthetic and, in some children, sedation.
Blood and urine tests
Your health care professional may use blood and urine tests to check the health of your kidneys. A urine sample can be used to determine whether there is blood or protein in your urine, which is a sign that the IgA vasculitis is affecting your kidneys. A blood test can check how well your kidneys are working.
Ultrasound
Depending on your symptoms, your health care professional may want you to have an ultrasound to check for GI or kidney problems.
Your health care professional will monitor your symptoms to determine if they are getting better. You may continue to have blood and urine tests to check your kidney function for at least 6 months after most of your symptoms disappear. Your health care professional will monitor you more closely if your tests show kidney damage, as this puts you at greater risk for developing CKD.
How do health care professionals treat IgA vasculitis?
There is no specific treatment for IgA vasculitis. The disease usually goes away on its own. However, your health care professional may suggest certain medicines to relieve symptoms such as abdominal pain, joint pain, and swelling. If your kidneys are involved, the treatment goal will be to prevent CKD.
If you are taking a medicine that may have caused the IgA vasculitis, you will stop taking that medicine.
Treatments for different symptoms
Rash. Your rash will usually go away without any specific treatment. In some people, the rash returns, but even the returning rash will go away without medicine.
GI tract problems. To ease abdominal pain, your health care professional may prescribe a corticosteroid—a medicine that lowers immune system activity and decreases swelling. In rare cases when intussusception occurs, health care professionals can correct the problem with a lower GI series, also called a barium enema, that uses air or barium to gently push the telescoped part of the intestine into its proper position or correct the problem with surgery.
 Abdominal pain is a common symptom of IgA vasculitis. If your pain is severe, talk to your health care professional about how to manage the pain.
Abdominal pain is a common symptom of IgA vasculitis. If your pain is severe, talk to your health care professional about how to manage the pain.Joint pain and swelling. Your health care professional may prescribe a nonsteroidal anti-inflammatory drug (NSAID), such as ibuprofen, or a corticosteroid to ease joint pain and swelling. You should not take NSAIDs if you have decreased kidney function or you suspect your kidneys have been affected.
Kidney involvement. In IgA vasculitis, the unusual activity of the immune system causes inflammation, which can lead to kidney damage. You may need to take a corticosteroid or other immunosuppressive medicine to reduce the inflammation, which can help prevent your immune system from causing more damage.
If you have protein in your urine, your health care professional may prescribe an angiotensin-converting enzyme (ACE) inhibitor or an angiotensin receptor blocker (ARB). ACE inhibitors and ARBs are blood pressure medicines that have been shown to reduce proteinuria and slow the progression of kidney disease.
Scrotum or testicles. If you are experiencing pain in the scrotum or testicles, your health care professional will recommend pain relief measures including bed rest, applying ice or a cool-pack, and placing a cushion under the scrotum to provide support.
How can I prevent IgA vasculitis?
Experts have not yet found a way to prevent IgA vasculitis. If your kidneys have been affected by the disease, treatments may be available to help prevent serious kidney problems. Talk with your health care professional about treatments, and follow the treatment plan your health care professional recommends.
How can my diet help prevent or relieve IgA vasculitis?
Diet and nutrition have not been shown to play a role in causing or preventing IgA vasculitis.
Clinical Trials for IgA Vasculitis
The NIDDK conducts and supports clinical trials in many diseases and conditions, including kidney disease. The trials look to find new ways to prevent, detect, or treat disease and improve quality of life.
What are clinical trials for IgA vasculitis?
Clinical trials—and other types of clinical studies—are part of medical research and involve people like you. When you volunteer to take part in a clinical study, you help health care professionals and researchers learn more about disease, and improve health care for people in the future.
Researchers are studying many aspects of IgA vasculitis, such as
- improved understanding of the causes of IgA vasculitis
- new treatments for this condition
- genes that increase the risk of developing IgA vasculitis
- pregnancy characteristics and outcomes among women with this condition
Find out if clinical studies are right for you.
What clinical studies for IgA vasculitis are looking for participants?
You can view a filtered list of clinical studies on IgA vasculitis that are open and recruiting at
ClinicalTrials.gov. You can expand or narrow the list to include clinical studies from industry, universities, and individuals; however, the National Institutes of Health does not review these studies and cannot ensure they are safe. Always talk with your health care professional before you participate in a clinical study.
References
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
The NIDDK would like to thank:
Joseph Flynn, M.D., University of Washington, and Tej K. Mattoo, M.D., D.C.H., F.R.C.P., F.A.A.P., Wayne State University School of Medicine
