Glomerular Disease
On this page:
- What is glomerular disease?
- How common is glomerular disease?
- Who is more likely to develop glomerular disease?
- What are the complications of glomerular disease?
- What are the symptoms of glomerular disease?
- What causes glomerular disease?
- How do health care professionals diagnose glomerular disease?
- How do health care professionals treat glomerular disease?
- How do eating, diet, and nutrition affect glomerular disease?
- Clinical Trials for Glomerular Disease
What is glomerular disease?
Glomerular disease is a condition that can damage your kidneys. The disease attacks tiny filters in your kidneys, called glomeruli, where your blood is cleaned. Damaged glomeruli can allow proteins and sometimes red blood cells to leak into your urine. One of the proteins in your blood is albumin. If too much albumin leaks into your urine, fluid can build up in your body, leading to swelling in your face, hands, feet, or legs. In some cases, glomerular disease can also prevent your kidneys from properly removing waste products, causing wastes to build up in your blood.
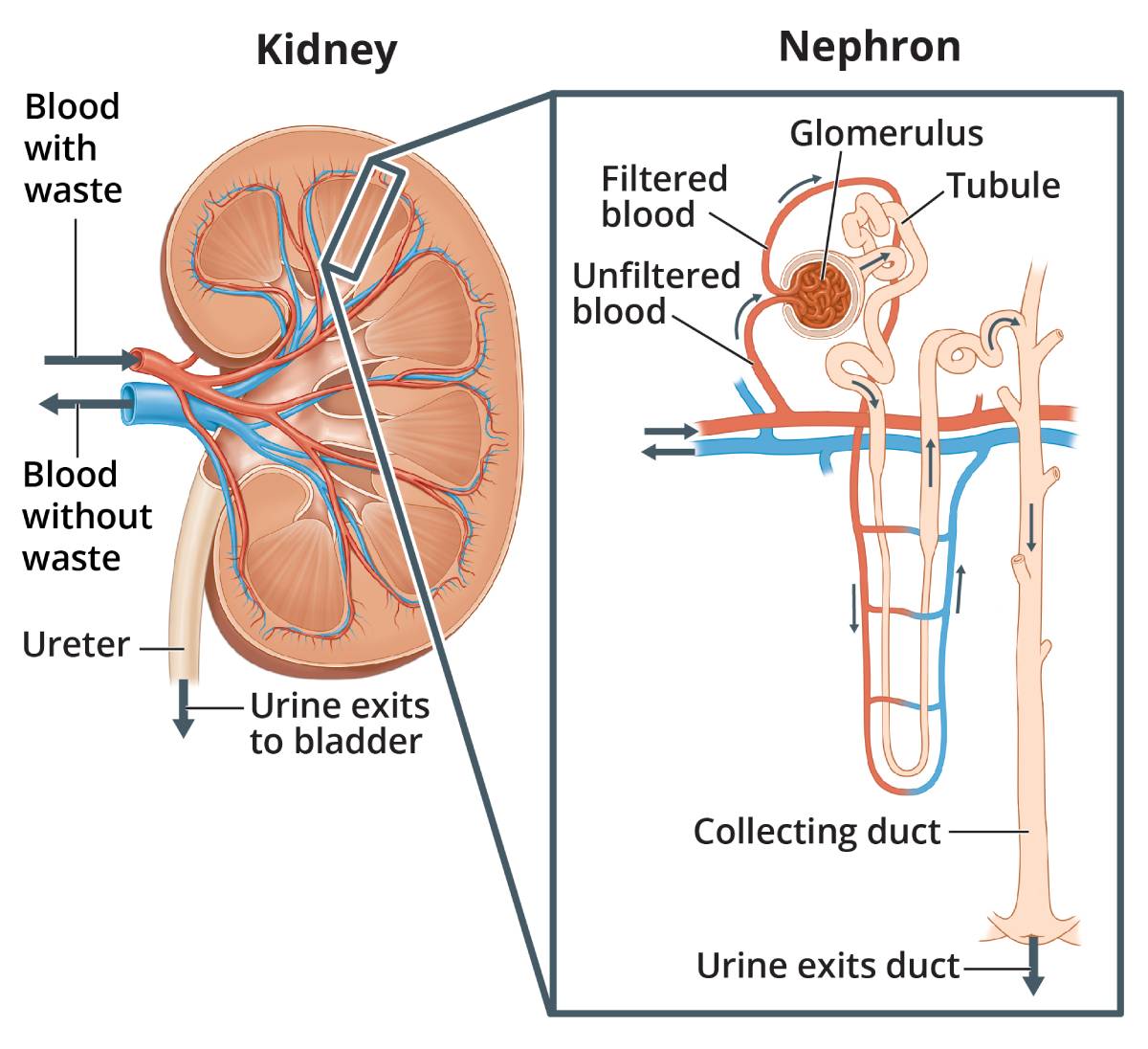 As blood passes through healthy kidneys, the glomeruli filter out waste products and allow the blood to keep the cells and proteins the body needs.
As blood passes through healthy kidneys, the glomeruli filter out waste products and allow the blood to keep the cells and proteins the body needs.
How common is glomerular disease?
Most of the diseases that cause glomerular disease are rare. But one of them, diabetic kidney disease, affects more than 1 in 3 U.S. adults who have diabetes.1 Diabetic kidney disease is also the leading cause of end-stage kidney disease, which is kidney failure that is treated with dialysis or a kidney transplant.
Who is more likely to develop glomerular disease?
Glomerular disease affects men and women of all ages and all racial and ethnic groups. Having a family member who has glomerular disease increases your risk.
What are the complications of glomerular disease?
Glomerular disease often progresses slowly, causing no symptoms for many years. But, over time, it can cause serious health problems such as
- high blood pressure, also called hypertension.
- nephrotic syndrome, a group of symptoms that indicate your kidneys are not working properly. These symptoms include too much protein in your urine, low levels of albumin in your blood, swelling in parts of your body, and high levels of cholesterol in your blood.
- chronic kidney disease, the gradual loss of kidney function, when your kidneys are no longer able to process and remove toxic waste products from your body.
- kidney failure, the loss of about 85% or more of kidney function, which often leads to symptoms such as appetite loss, nausea, vomiting, and worsening swelling.
In some cases, glomerular disease can cause rapid kidney failure that may lead to confusion and death if not treated immediately.
What are the symptoms of glomerular disease?
Symptoms of glomerular disease vary and are related to the type of damage to your glomeruli. Some people with less damage may have few or no symptoms, whereas people with more severe damage may have more noticeable symptoms. Symptoms can include
- high blood pressure, which may develop or get worse.
- swelling. Also called edema, swelling can affect many parts of your body including your hands, ankles, legs, and around your eyes.
- weight gain. As fluid builds up in your body, your weight can increase.
- proteinuria. Too much protein in your urine, called proteinuria, can cause bubbles or foam to appear in your urine.
- blood in your urine. Also called hematuria, blood in the urine can make your urine look pink or cola-colored. The blood can usually only be seen under a microscope.
One or more of these symptoms can be the first sign of kidney disease.
What causes glomerular disease?
- diabetic kidney disease, a type of kidney disease caused by diabetes. Over several years, high levels of blood glucose, also called blood sugar, can damage your glomeruli.
- focal segmental glomerulosclerosis (FSGS), a disease that causes scar tissue to form in some of your kidneys’ glomeruli. FSGS has several causes, including genes, autoimmune diseases, and diseases that cause pressure to build in the glomeruli, such as obesity and sleep apnea.
- lupus nephritis, a kidney disease caused by systemic lupus erythematosus (lupus). Lupus is an autoimmune disease that affects many parts of the body. The disease can cause antibodies to build up in your glomeruli, causing inflammation that can keep your kidneys from working properly and lead to scarring over time.
- membranous nephropathy, a disease that causes antibodies to build up in a part of your kidney called the glomerular basement membrane. As a result, your glomeruli can become thick and inflamed. Causes can include infection, cancer, and autoimmune diseases.
- IgA nephropathy, also called Berger’s disease, an autoimmune disease that causes an antibody called immunoglobulin A (IgA) to build up in your glomeruli, causing inflammation and damage.
- minimal change disease, also called nil disease. This kidney disease causes changes to your glomeruli that can only be seen under a very powerful microscope, called an electron microscope.
- anti-GBM (Goodpasture’s) disease, an autoimmune disease in which antibodies attack your glomeruli, causing damage and inflammation. The disease can also affect your lungs.
Other causes of glomerular disease include
- infections, including strep throat, bacterial endocarditis, HIV/AIDS, hepatitis B, and hepatitis C
- some drugs and medicines that can harm the kidneys, such as nonsteroidal anti-inflammatory drugs
- genetic disorders that affect the kidneys, such as Alport syndrome and Fabry disease
In some cases, the exact cause of a glomerular disease is unknown.
How do health care professionals diagnose glomerular disease?
Health care professionals diagnose glomerular disease by ordering tests, such as
- urinalysis, which examines a sample of your urine to find out if levels of protein and red blood cells are too high.
- blood tests, which can measure the levels of products in your blood, such as creatinine, urea nitrogen, and a protein called cystatin C, to find out how well your kidneys are working. Blood tests can also check for low levels of a protein in your blood, called albumin, which can happen when too much of that protein passes from your blood into your urine.
- imaging tests, such as an ultrasound or computed tomography (CT) scan, which can show the shape or size of your kidneys.
- kidney biopsy, in which a health care professional examines a small piece of tissue from your kidney under a microscope to look for signs of kidney damage. A kidney biopsy can confirm you have glomerular disease and help find the cause.
How do health care professionals treat glomerular disease?
Treatment for glomerular disease varies by symptoms, causes, and how badly the kidneys are damaged. In some cases, glomerular disease may go away once its cause has been treated. In other cases, the disease may go away but later return. Less often, glomerular disease may not respond to treatment and lead to kidney failure over time.
Medicines
Health care professionals often treat glomerular disease with medicines, such as
- an angiotensin-converting enzyme (ACE) inhibitor or an angiotensin II receptor blocker (ARB). These medicines can reduce protein loss, lower blood pressure, and slow the progression of kidney disease.
- diuretics (water pills), which reduce swelling by helping the kidneys remove sodium—or salt—and water from your blood.
- statins, which lower blood cholesterol and can reduce the risk for certain types of heart disease that can develop among people with glomerular disease.
- sodium-glucose transporter 2 (SGLT2) inhibitors, medicines originally used to treat diabetes, can also slow the progression of kidney disease.
- medicines that make your immune system less active—such as corticosteroids, antimetabolites, alkylating agents, or monoclonal antibodies, which can reduce inflammation.
Other treatments
If kidney disease advances to kidney failure, your health care professional may suggest treatment options such as
- hemodialysis, a procedure that filters your blood outside of your body, using an external filter called a dialyzer
- peritoneal dialysis, a procedure that filters your blood inside your body, using the lining of your abdomen, or belly
- kidney transplant, a surgery that places a healthy kidney from another person inside your body
How do eating, diet, and nutrition affect glomerular disease?
Eating, diet, and nutrition have not been shown to play a role in causing or preventing glomerular disease. But if you have glomerular disease, your health care professional may recommend you
- limit sodium intake
- reduce calories if your health care professional advises you to lose excess weight
- limit saturated fats if your cholesterol is high
Clinical Trials for Glomerular Disease
NIDDK conducts and supports clinical trials in many diseases and conditions, including kidney diseases. The trials look to find new ways to prevent, detect, or treat disease and improve quality of life.
What are clinical trials for glomerular disease?
Clinical trials—and other types of clinical studies—are part of medical research and involve people like you. When you volunteer to take part in a clinical study, you help doctors and researchers learn more about disease and improve health care for people in the future.
Researchers are studying many aspects of glomerular disease in children and adults, such as
- causes of glomerular disease, including genes
- complications of glomerular disease, including infection and heart disease
- quality of life among people with glomerular disease
- how to best treat glomerular disease
Find out if clinical studies are right for you.
Watch a video of NIDDK Director Dr. Griffin P. Rodgers explaining the importance of participating in clinical trials.
What clinical studies for glomerular disease are looking for participants?
You can view a filtered list of clinical studies on glomerular disease that are federally funded, open, and recruiting at ClinicalTrials.gov. You can expand or narrow the list to include clinical studies from industry, universities, and individuals; however, the National Institutes of Health does not review these studies and cannot ensure they are safe. Always talk with your health care provider before you participate in a clinical study.
References
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
NIDDK would like to thank:
Amy Mottl, M.D., M.P.H., FASN, University of North Carolina School of Medicine

