Perineal Injury in Males
On this page:
- What is perineal injury in males?
- How common are perineal injuries in males?
- Who is more likely to have a perineal injury?
- What are the complications of perineal injury?
- What are the signs and symptoms of perineal injury in males?
- What causes perineal injury in males?
- How do health care professionals diagnose perineal injury in males?
- Can I prevent a perineal injury?
- Clinical Trials for Perineal Injury in Males
What is perineal injury in males?
Perineal injury is an injury to the perineum, the area of the body between the anus and the scrotum. It is a type of genital injury.
What is the perineum and why is it important?
In males, the perineum lies just below the pelvic floor muscles, which support the bladder and bowel. The perineum protects the pelvic floor muscles and the blood vessels that supply the genitals and urinary tract. The perineum also protects the nerves used to urinate or have an erection.
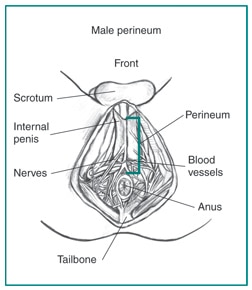
Types of perineal injuries
Injuries to the perineum can happen suddenly, known as an acute injury, or gradually, known as a chronic injury.
Acute injuries include
- straddle injuries, which can happen if you fall with your legs on each side of an object or bar and hit your perineum when you land
- impalement injuries that occur when an object punctures the perineum
- burns
Acute injuries can also happen from violent trauma, during surgery, sexual abuse, or from some medical conditions.
Chronic injuries develop gradually from pressure on the perineum for a long time. Long-term pressure can come from certain seated activities, such as road cycling long distances.
How common are perineal injuries in males?
Injuries to the perineum are rare. One study found that the perineum was injured in 1 percent of motorcyclists and 3 percent of bicyclists involved in traffic accidents.1
Who is more likely to have a perineal injury?
Perineal injury is more likely for men who
- are in military combat
- have surgery in their genital region
- ride bicycles, motorcycles, or horses
- work in construction or on a farm
- engage in gymnastics
- have been sexually abused
What are the complications of perineal injury?
Bladder control problems or sexual problems may develop if the blood vessels, nerves, or muscles in the perineum are damaged. Infections may develop after a burn or wound.
Bladder control problems
Perineal trauma can injure nerves of the pelvis, causing bladder and bowel problems. The nerves in your bladder signal when it is full, and your brain directs your bladder and pelvic floor muscles to hold or release urine. Injury to those nerves can block or interfere with the signals, causing your bladder muscles to squeeze involuntarily at the wrong time or not to squeeze at all. Damage to your pelvic floor muscles can also cause bowel control problems.
Damage to the perineum could also injure an internal part of the penis containing the urethra. The urethra may tear or become narrower, or you may experience urinary incontinence.
Sexual problems
The perineal nerves carry signals between the genitals and the brain. Injury to those nerves can interfere with the sensations of sexual contact.
If the blood vessels in the perineum are damaged, you may develop erectile dysfunction (ED), the inability to achieve or maintain an erection firm enough for sexual intercourse. ED may also be caused by damage to the urethra.
In rare situations, a blunt injury to the perineum may burst a blood vessel inside the penis, causing a persistent partial erection that can last for days to weeks or longer. This condition is called high-flow priapism and, if not treated, may lead to ED.2
What are the signs and symptoms of perineal injury in males?
Signs of a perineal injury include
- bleeding or an open wound
- object embedded in the perineum
- burned skin
- bruising
- swelling
- fresh blood in urethral opening
- inability to urinate
Along with these signs, you may have symptoms such as pain in the genital, groin, or abdominal areas. In some cases, the pain may be severe.
Bicycle or motorcycle riders may also experience genital numbness. The level of numbness increases with longer or rougher rides.3
What causes perineal injury in males?
Acute perineal injuries
Causes of acute perineal injury in males include
Perineal surgery. A surgeon may need to cut the perineum during some types of surgery, such as
- surgery to remove the prostate
- surgery to repair a stricture, or narrowing, of the portion of the urethra that runs through the perineum
- colorectal or anal cancer surgery to remove a tumor
Straddle injuries. Straddle injuries include motorcycle- and bike-riding accidents, horseback riding accidents, or accidental falls onto stationary objects such as fence rails or gymnastic equipment.
Impalement. Impalement injuries may involve metal fence posts, rods, or weapons that pierce the perineum. Impalement injuries occur in combat situations or where moving equipment and pointed tools are in use, such as on farms or construction sites. Impalement can also result from a fall onto something sharp.
Sexual abuse. Forceful and inappropriate sexual contact can cause perineal injury.
Burns. Contact with hot objects or liquids could injure the perineum. These may occur in military combat4 or from contact with hot liquids5 or hot objects, such as personal grooming implements.6 Burns may also lead to infections.4
Other conditions. Fournier’s gangrene is an acute infection that occurs in the genital region and causes tissue death. It affects the perineum, scrotum, or penis in males. It is a rare disease and may be a complication from other types of urinary tract conditions, surgery, or trauma.7
Chronic perineal injuries
Chronic perineal injuries most often result from a job- or sport-related practice—such as riding a bicycle, motorcycle, or horse.
Bicycle, motorcycle, and horseback riding. Sitting on a narrow, saddle-style bike seat—which has a protruding “nose” in the front—places far more pressure on the perineum than sitting in a regular chair. In a regular chair, the flesh and bone of the buttocks partially absorb the pressure of sitting, and the pressure occurs farther toward the back than on a bike seat. The straddling position on a narrow seat pinches the perineal blood vessels and nerves, possibly causing blood vessel and nerve damage over time. Research shows wider, noseless seats reduce perineal pressure.8
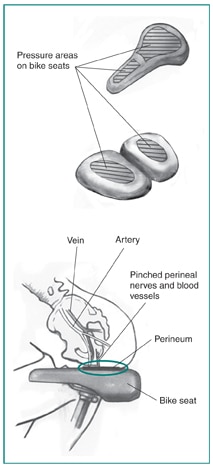
Cycling has many cardiovascular benefits that improve overall sexual and urinary health. There is controversy whether long-distance cycling leads to modest, increased risk of ED. ED may be caused by repetitive pressure on blood vessels, which constricts them and results in plaque buildup in the vessels. Genital numbness has been noted in male cyclists who engage in long-distance cycling events. Cyclists should aim to ride in a way that avoids acute genital numbness. Long distance riders should get their bike professionally fit to their body, consider using seats that minimize perineal pressure, and spend less time engaged with the saddle during long rides.
How do health care professionals diagnose perineal injury in males?
Health care professionals diagnose perineal injury based on the circumstances and severity of the injury. In general, a health care professional will conduct a physical exam and order one or more imaging tests.
Physical exam
During a physical exam, your health care professional looks for wounds, swelling, or bruises and may use a digital rectal exam to feel for internal injuries. Your health care professional also may conduct a neurologic exam to test skin sensation.
Imaging tests
Your health care professional may order one or more imaging tests to check for internal injuries.
- Computed tomography (CT) scans can show traumatic injury to the perineum.
- Magnetic resonance imaging (MRI) can show damage to blood vessels and muscles.
- Ultrasound can show damage to blood vessels in the perineum.
- X-rays that include the addition of a special dye can show if your urethra is damaged.
Injury evaluation
When health care professionals evaluate injuries, they typically ask how the injury occurred and when was the last time you urinated. In cases of genital injuries, these questions may make you feel uncomfortable because, in addition to other causes, genital injuries can be caused by sexual abuse, and health care professionals are required by law to report cases of sexual abuse that come to their attention.
How do health care professionals treat perineal injuries in males?
Treatments for perineal injury vary with the severity and type of injury. If you are bleeding, your health care professional will take immediate steps to minimize blood loss and repair the injury. Tears or incisions may require stitches, and burns may require ointment. Traumatic or piercing injuries may require surgery to repair damaged pelvic floor muscles, blood vessels, and nerves. In case of a urethral injury, your urine may need to be collected through a tube called a catheter. Treatment for these acute injuries may also include antibiotics to prevent infection.
After a health care professional stabilizes an acute injury so blood loss is no longer a concern, some long-term effects of the injury, such as bladder control and sexual function problems, may persist. Injuries to the urethra could cause it to become narrower, and it may need to be treated. A health care professional can treat high-flow priapism caused by a blunt injury to the perineum with medication or surgery.
For people with a chronic perineal injury, a health care professional will work with you to treat the condition and any complications.
Can I prevent a perineal injury?
You can take steps to protect your perineum and reduce the chance of accidental injury.
Bicycle, motorcycle, or horseback riding. Use seats or saddles that minimize pressure on the perineum and shift pressure to the buttocks. The National Institute for Occupational Safety and Health, part of the Centers for Disease Control and Prevention, recommends noseless seats for people who ride bikes as part of their job.8
You can also adjust the height of the handlebars, pedals, or seat, and wear padded shorts to reduce pressure and chafing of your perineum.10 In addition, increasing the time you stand while cycling may decrease numbness.11

Construction, agricultural, or factory work. Wear appropriate protective gear, such as coveralls or body suits, if you are around moving equipment or sharp objects.12 Be aware of your surroundings and potential hazards.
Military combat and first responders. People engaged in military combat should use pelvic personal protective equipment to limit penetration and reduce the rate of injury.13 Police and other first responders may want to use similar equipment as specific jobs and situations warrant.12
Surgery. While surgeons try to avoid procedures that can damage your blood vessels, perineal nerves, and muscles, sometimes a perineal incision may be needed to achieve the best result. Discuss the risks of any planned surgery with your health care professional so you can make an informed decision and understand what to expect after the operation.
Clinical Trials for Perineal Injury in Males
The NIDDK conducts and supports clinical trials in many diseases and conditions, including urologic diseases. The trials look to find new ways to prevent, detect, or treat disease and improve quality of life.
What are clinical trials for perineal injury?
Clinical trials—and other types of clinical studies—are part of medical research and involve people like you. When you volunteer to take part in a clinical study, you help doctors and researchers learn more about disease and improve health care for people in the future.
Researchers are studying many aspects of perineal injuries in males, such as
- the effect of bicycle seats on blood flow in the perineum in males
- treatments for chronic perineal pain
Find out if clinical studies are right for you.
Watch a video of NIDDK Director Dr. Griffin P. Rodgers explaining the importance of participating in clinical trials.
What clinical studies for perineal injuries are looking for male participants?
You can view a filtered list of clinical studies on perineal injuries that are open and recruiting males at ClinicalTrials.gov. You can expand or narrow the list to include clinical studies from industry, universities, and individuals; however, the National Institutes of Health does not review these studies and cannot ensure they are safe. Always talk with your health care professional before you participate in a clinical study.
References
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
The NIDDK would like to thank:
Benjamin Breyer, M.D., M.A.S., University of California San Francisco School of Medicine
