Penile Curvature (Peyronie's Disease)
On this page:
- What is Peyronie’s disease?
- How common is Peyronie’s disease?
- Who is more likely to have Peyronie’s disease?
- What are the complications of Peyronie’s disease?
- What are the signs and symptoms of Peyronie’s disease?
- What causes Peyronie’s disease?
- How do health care professionals diagnose Peyronie’s disease?
- How do health care professionals treat Peyronie’s disease?
- Can I prevent Peyronie’s disease?
- Clinical Trials for Peyronie’s disease
What is Peyronie’s disease?
Peyronie’s disease is a disorder in which scar tissue, called plaque, forms under the skin of the penis—the male organ used for urination and sex.
The plaque builds up inside the penis, in the thick elastic membrane called the tunica albuginea. The tunica albuginea helps keep the penis stiff during an erection. The plaque can develop anywhere along the penis.
As it develops, the plaque pulls on the surrounding tissues and causes the penis to curve or bend, usually during an erection. Curves in the penis can make erections painful and may make sexual intercourse painful, difficult, or impossible.
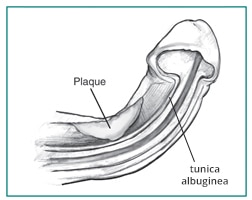
The plaque that develops in Peyronie’s disease
- is caused by injury to your penis or by an autoimmune disease
- is not the same plaque that can develop in a person’s arteries
- is benign—not cancerous and not a tumor
Peyronie’s disease occurs in two phases.
Acute phase
During the acute phase, the plaque forms, and this phase can last up to 18 months.1 During this phase
- Inflammation may occur and plaque forms on your penis.
- Your penis starts to curve.
- Your penis may hurt without an erection.
- Erections may become painful when scars develop.
Chronic phase
The chronic phase occurs after the plaque has formed. Usually, the chronic phase begins 12 to 18 months after your symptoms first appear.1 During this phase
- Plaque and penile curvature may stabilize and not get worse.
- The pain in your penis may lessen.
- Erectile dysfunction (ED) may develop or become worse.
How common is Peyronie’s disease?
Approximately 1 in 100 men in the United States over the age of 18 have been diagnosed with Peyronie’s disease. However, based on studies of men who reported having symptoms of Peyronie’s disease, researchers estimate that the actual number of men who have Peyronie’s disease is more than 1 in 10.2,3
The chance of developing Peyronie’s disease increases with age.1 It is less common for men in their 20s and 30s to have Peyronie’s disease.1
Who is more likely to have Peyronie’s disease?
You may be at higher risk of developing Peyronie’s disease if you
- engage in vigorous sexual or nonsexual activities that cause micro-injuries to the penis
- have certain connective tissue and autoimmune disorders
- have a family history of Peyronie’s disease
- are older
- have diabetes and erectile dysfunction
- have a history of prostate cancer treatment with surgery
Vigorous sexual and nonsexual activities
Men whose sexual or nonsexual activities (such as sports) cause micro-injuries to the penis are more likely to develop Peyronie’s disease.
Connective tissue and autoimmune disorders
If you have certain connective tissue or autoimmune disorders, you may have a higher chance of developing Peyronie’s disease.
Connective tissue is specialized tissue that supports, joins, or separates different types of tissues and organs in your body. Connective tissue disorders may affect your joints, muscles, and skin. Some disorders associated with Peyronie’s disease include
- Dupuytren’s disease, also known as Dupuytren’s contracture. In this condition, the connective tissue in the palms of the hands shortens and thickens. This results in the permanent bending of the outer fingers. It is not clear why men with Peyronie’s disease are more likely to develop Dupuytren’s disease.
- plantar fasciitis, which is inflammation of the thick tissue on the bottom of the foot that creates the arch of the foot.
- scleroderma, which is the abnormal growth of thick, hard patches of connective tissue. Scleroderma can also cause swelling or pain in muscles and joints.
In autoimmune disorders, the body’s immune system attacks the body’s own cells and organs. Autoimmune disorders associated with Peyronie’s disease include
- systemic lupus erythematosus, which causes inflammation and damage to various body tissues including the joints, skin, kidneys, heart, lungs, blood vessels, and brain
- Sjögren’s syndrome, which causes inflammation and damage to the glands that make tears and saliva
- Behçet’s disease, which causes inflammation of the blood vessels
Family history of Peyronie’s disease
Medical experts believe that Peyronie’s disease may run in some families. For example, if your father or brother has Peyronie’s disease, you may have an increased chance of getting the disease too.
Aging
Your chance of getting Peyronie’s disease increases with age. Age-related changes in the tissues in the penis may cause it to be more easily injured and less likely to heal well.
Diabetes with erectile dysfunction
Men with diabetes-associated ED have a 4 to 5 times higher chance of developing Peyronie’s disease compared with the general population.4
Prostate cancer treatment with surgery
Your chance of getting Peyronie’s disease increases after surgery for prostate cancer. Medical experts believe this is related to ED developed after surgery for prostate cancer.5
What are the complications of Peyronie’s disease?
Complications of Peyronie’s disease may include
- the inability to have sexual intercourse due to penile curvature
- ED
- emotional distress, depression, or anxiety about sexual abilities or the appearance of the penis
- stress in a relationship with a sexual partner
- problems fathering a child because intercourse is difficult
What are the signs and symptoms of Peyronie’s disease?
The signs and symptoms of Peyronie’s disease may include
- hard lumps on one or more sides of the penis
- pain during sexual intercourse or during an erection
- a curve in the penis with or without an erection
- changes in the shape of the penis, such as narrowing or shortening
- ED
These may develop slowly or appear quickly and can be mild to severe. In many cases, the pain decreases over time, although the curve in the penis may remain.1 Problems with intercourse or ED can occur during either phase.
What causes Peyronie’s disease?
Medical experts do not know the exact cause of Peyronie’s disease but believe that it may be the result of
- acute or chronic injury to the penis
- autoimmune disease
Peyronie’s disease is not contagious or caused by any known transmittable disease.
Injury to the penis
Medical experts believe that hitting or bending the penis may injure the tissues inside. These injuries can happen during sex, athletic activity, or an accident. It can happen once, an acute injury, or repeatedly over time, a chronic injury.
The injury may cause bleeding and swelling inside the elastic membrane in the penis, or the tunica albuginea. When the injury heals, scar tissue may form, and a plaque can develop. The hard plaque pulls at the surrounding tissues and causes the penis to curve.
You may not be aware of micro-injuries to your penis when they occur. Researchers have found that many patients are unable to recall a specific incident just before symptoms started.1
Autoimmune disease
Men who have an autoimmune disease may develop Peyronie’s disease if the immune system attacks cells in the penis. This can lead to inflammation in the penis. Scar tissue may form and develop into plaque. See connective tissue and autoimmune disorders for more on autoimmune disorders associated with Peyronie’s disease.
How do health care professionals diagnose Peyronie’s disease?
Men with Peyronie’s disease are usually referred to a urologist—a doctor who specializes in sexual and urinary problems.
A urologist diagnoses Peyronie’s disease based on your medical and family history and a physical exam.
Imaging tests are usually not necessary to diagnose Peyronie’s disease but may be used to gather additional information about the plaque.
Medical and family history
The urologist will ask about your medical and family history. Some questions might be
- When did your symptoms begin?
- Do you feel pain during an erection or at other times?
- Do you have erection problems or problems with sexual intercourse?
- Does anyone in your family have Peyronie’s disease or other medical conditions?
- Are you taking any medicines? If so, what are they?
- Do you have other medical problems or conditions?

Physical exam
A urologist can usually feel plaques in the penis whether it is erect or not.
If the urologist needs to examine your penis during an erection, you will receive an injectable medicine that will cause an erection. Your urologist may also ask you to take pictures of your erect penis at home to evaluate the curvature during your follow-up visits.
How do health care professionals treat Peyronie’s disease?
The goal of treatment is to reduce pain, attain a straight or close-to-straight penis, and restore and maintain the ability to have intercourse.
Not all men with Peyronie’s disease need treatment. In a very few cases, Peyronie’s disease goes away without treatment.1
Also, you may not need treatment if you have6
- small plaques
- little or no curve to your penis
- no pain
- no problems with sexual intercourse
- no urinary problems
If you need treatment, your urologist may recommend nonsurgical treatments or surgery depending on the severity of your symptoms, how much your penis curves, and whether your Peyronie’s disease is in the acute or chronic phase.
Your urologist will discuss your treatment options with you and review possible side effects and outcomes.
Besides treatment, your urologist may recommend lifestyle changes to reduce the risk of ED associated with Peyronie’s disease.
Nonsurgical treatments
Nonsurgical treatments include injections, oral medicines, and medical therapies. They may be used when Peyronie’s disease is in the acute phase.
Injections. Injecting a medicine directly into plaques, called intralesional injections, can be done in the acute phase. The injection site is often numbed before the shot. These treatments can be done in the doctor’s office.
- Collagenase. Intralesional collagenase injections (Xiaflex) are currently the only FDA-approved treatment for Peyronie’s disease. Collagenase is an enzyme that helps break down the substances that make up plaques. Breaking down the plaques reduces penile curving and improves erectile function. This treatment is approved for men with penises curving more than 30 degrees.7
- Verapamil. Verapamil is used to treat high blood pressure and may reduce penis pain and curving when injected into the plaque.1
- Interferon-alpha 2b. Interferon is a protein made by white blood cells. Studies show that it reduces pain, penile curving, and plaque size.7
Oral medicines. There are no oral medicines that effectively treat penile curvature at this time.7 However, potassium para-aminobenzoate is used to treat Dupuytren’s contracture and may reduce plaque size. It has no effect on penile curving.
If you feel pain, your urologist may suggest you take nonsteroidal anti-inflammatory drugs (NSAIDS).
Nondrug medical therapies. Other medical therapies to treat Peyronie’s disease are still being studied to see if they work.7 These therapies include
- mechanical traction and vacuum devices—aimed at stretching or bending the penis to reduce curving
- shockwave therapy—focused, low-intensity electroshock waves directed at the plaque may be used to reduce pain1
Surgery
A urologist may recommend surgery to remove plaque or help straighten the penis during an erection. Surgery may be recommended for men who have Peyronie’s disease when
- symptoms have not improved
- erections or intercourse, or both, are painful
- the curve in the penis prevents sexual intercourse
Medical experts recommend you don’t have surgery until your plaque and penis curving stabilize.1
Several types of surgeries treat Peyronie’s disease. Your urologist will examine the plaque on your penis and consider the best type of surgery for you. An ultrasound will show the exact location and size of the plaque.
Some men may develop complications after surgery, and sometimes surgery does not correct some effects of Peyronie’s disease such as the shortening of the penis.
Grafting. In this surgery, your urologist will remove the plaque and replace it with a patch of tissue that was taken from another part of your body, such as skin or a vein from your leg; grown in a laboratory; or from organ donors.
This procedure may straighten the penis and restore some length that was lost due to Peyronie’s disease.
Some men may experience numbness of the penis and ED after the procedure.
Plication. In plication surgery, your urologist will remove or pinch a piece of the tunica albuginea from the side of the penis opposite the plaque to help straighten the penis.
This procedure is less likely to cause numbness or ED.
Plication cannot restore the length or girth of the penis, and the penis may become shorter.
Device implantation. Penile implants may be considered if a man has both Peyronie’s disease and ED.
A urologist implants a device into the penis that can cause an erection. The device may help straighten the penis during an erection.
In some cases, the implant alone will straighten the penis adequately. If the implant alone does not straighten the penis, a urologist may combine implantation with one of the other two surgeries.
Can I prevent Peyronie’s disease?
Researchers do not know how to prevent Peyronie’s disease. At this time, diet and nutrition have not been found to play a role in preventing Peyronie’s disease.1
Clinical Trials for Peyronie’s disease
The NIDDK conducts and supports clinical trials in many diseases and conditions, including urologic diseases. The trials look to find new ways to prevent, detect, or treat disease and improve quality of life.
What are clinical trials for Peyronie’s disease?
Clinical trials—and other types of clinical studies—are part of medical research and involve people like you. When you volunteer to take part in a clinical study, you help doctors and researchers learn more about disease and improve health care for people in the future.
Researchers are studying many aspects of treating Peyronie’s disease including the efficacy of
- different medicines
- other types of nonsurgical treatment
Find out if clinical studies are right for you.
What clinical studies for Peyronie’s disease are looking for participants?
You can view a filtered list of clinical studies on Peyronie’s disease that are open and recruiting at ClinicalTrials.gov. You can expand or narrow the list to include clinical studies from industry, universities, and individuals; however, the NIH does not review these studies and cannot ensure they are safe. Always talk with your health care professional before you participate in a clinical study.
What have we learned about Peyronie’s disease from NIDDK-funded research?
The NIDDK has supported research projects to learn more about how plaque develops and the role of genes.
References
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
The NIDDK would like to thank:
Run Wang, M.D., FACS, University of Texas McGovern Medical School at Houston and MD Anderson Cancer Center
