Ostomy Surgery of the Bowel
View or Print All Sections
Definition & Facts
Ostomy surgery of the bowel is an operation that changes the way intestinal contents leave your body when part or all of your bowel is diseased, injured, or missing. During ostomy surgery of the bowel, surgeons connect the large or small intestine to the skin on the outside of your abdomen.
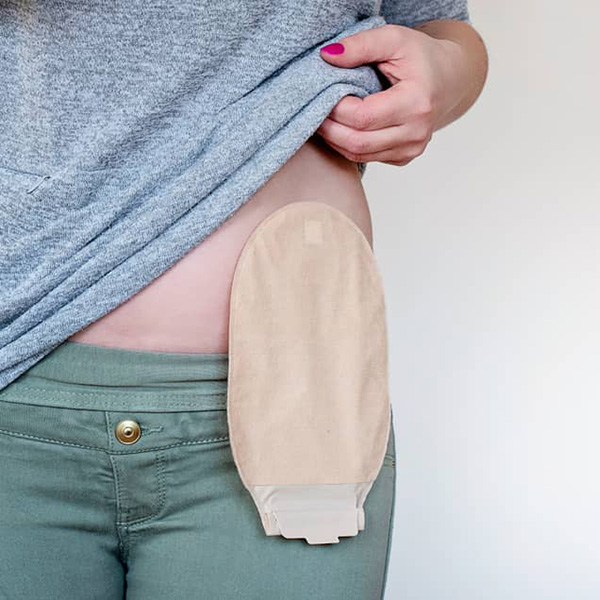
Types of Ostomy Surgery of the Bowel
The most common types of ostomy surgery of the bowel include ileostomy, colostomy, and continent ileostomy. Ileoanal pouch surgery is another type of bowel surgery that usually requires a temporary ileostomy. The type of ostomy surgery your doctor recommends may depend on why you need surgery and other factors.
What to Expect Before & During Ostomy Surgery of the Bowel
Your surgeon and an ostomy nurse may help you prepare for ostomy surgery of the bowel. An ostomy nurse can provide information about surgery, how ostomy pouches work, and how to adjust to life with a stoma. Health care professionals also help choose the best location for your stoma.
After Ostomy Surgery of the Bowel
Most people are able to lead full and active lives and return to most of the activities they enjoyed before ostomy surgery. Your ostomy nurse can provide education, support, and advice as you adjust to life after your ostomy surgery.
Complications of Ostomy Surgery of the Bowel
Like any major surgery, ostomy surgery may lead to complications, such as bleeding and infection. Some risks depend on the type of ostomy surgery you have and the reasons you need surgery. Contact your doctor or ostomy nurse if you notice any unusual signs and symptoms any time after ostomy surgery.
Clinical Trials
The NIDDK conducts and supports clinical trials in many diseases and conditions, including digestive diseases. The trials look to find new ways to prevent, detect, or treat disease and improve quality of life.
Related Conditions & Diseases
Your Digestive System & How It Works
The digestive system is made up of the gastrointestinal (GI) tract—also called the digestive tract—and the liver, pancreas, and the gallbladder. The GI tract is a series of hollow organs joined in a long, twisting tube from the mouth to the anus.
Related Research
See more about digestive diseases research at NIDDK.
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
The NIDDK would like to thank:
Samantha Hendren, M.D., M.P.H., University of Michigan
