Zollinger-Ellison Syndrome
On this page:
- What is Zollinger-Ellison syndrome?
- How common is Zollinger-Ellison syndrome?
- Who is more likely to have Zollinger-Ellison syndrome?
- What are the complications of Zollinger-Ellison syndrome?
- What are the symptoms of Zollinger-Ellison syndrome?
- What causes Zollinger-Ellison syndrome?
- How do doctors diagnose Zollinger-Ellison syndrome?
- What tests do doctors use to diagnose Zollinger-Ellison syndrome?
- How do doctors treat Zollinger-Ellison syndrome?
- How do doctors prevent and treat the complications of Zollinger-Ellison syndrome?
- Clinical Trials for Zollinger-Ellison Syndrome
What is Zollinger-Ellison syndrome?
Zollinger-Ellison syndrome is a condition that occurs when one or more tumors—called gastrinomas, which are located mainly in your pancreas or duodenum—cause your stomach to make too much acid. Too much acid in your stomach can lead to symptoms, such as diarrhea, and health complications, including peptic ulcer disease and gastroesophageal reflux disease (GERD).
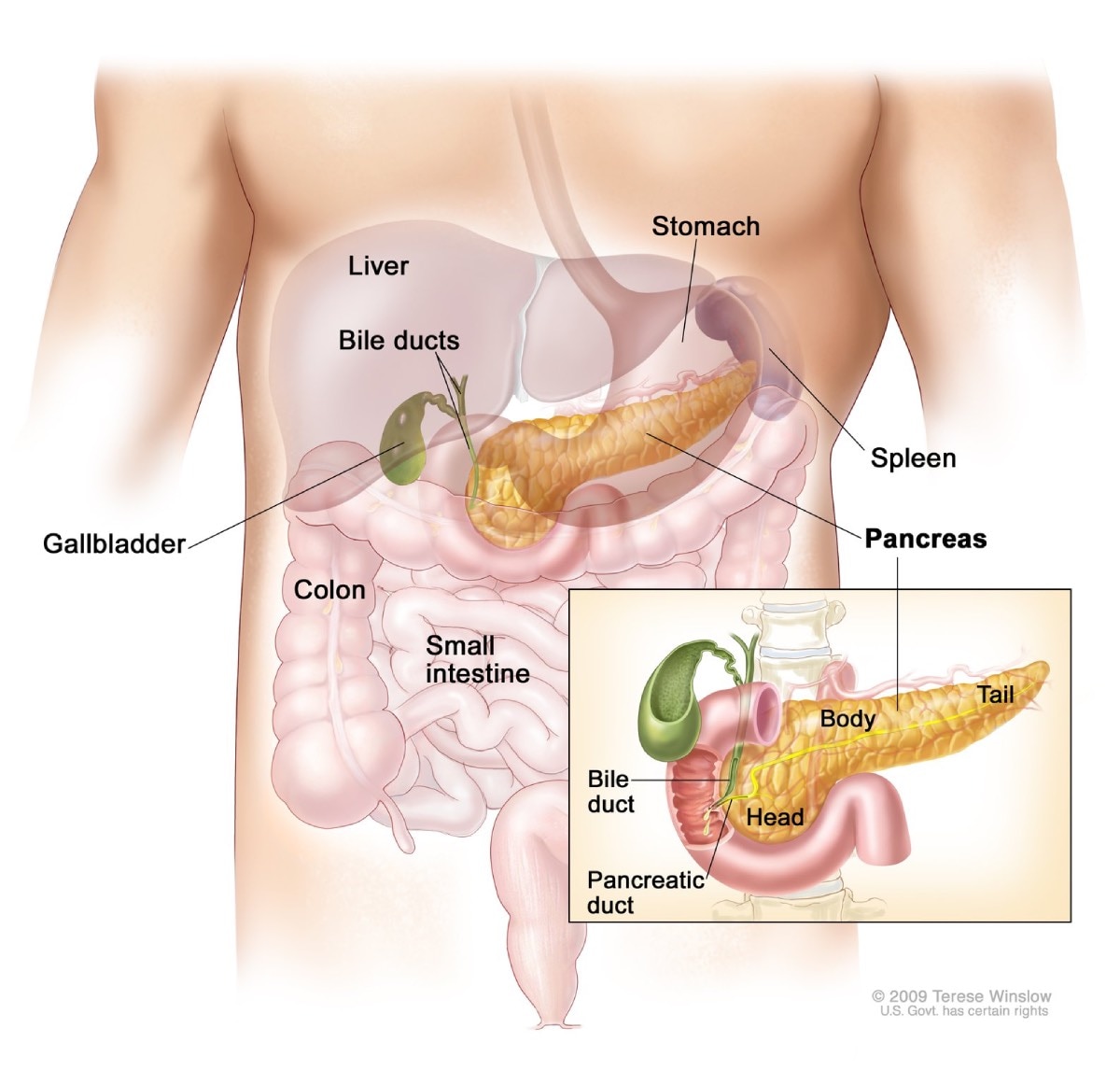 The pancreas and the first part of the small intestine, called the duodenum
The pancreas and the first part of the small intestine, called the duodenumHow common is Zollinger-Ellison syndrome?
Zollinger-Ellison syndrome is rare. Only 0.5 to 3 out of every 1 million people are diagnosed with Zollinger-Ellison syndrome each year.1
Who is more likely to have Zollinger-Ellison syndrome?
While anyone can have Zollinger-Ellison syndrome, the condition is most often diagnosed in people ages 20 to 50 years old.2 Zollinger-Ellison syndrome is slightly more common in men than in women.1
About 80% of cases of Zollinger-Ellison syndrome is unrelated to other conditions, but 20% to 25% of cases occur in people who have a rare, genetic disorder called multiple endocrine neoplasia type 1 (MEN1).3 People with a family history of MEN1 are more likely to have MEN1 and Zollinger-Ellison syndrome.
What are the complications of Zollinger-Ellison syndrome?
The extra stomach acid caused by Zollinger-Ellison syndrome can lead to peptic ulcer disease or GERD. Without treatment, these diseases can lead to complications such as
- bleeding or perforation in the upper digestive tract
- a blockage that can stop food from moving from your stomach into your duodenum
- esophagitis or esophageal stricture
The tumors that cause Zollinger-Ellison syndrome are sometimes cancerous and may spread to other parts of your body. If the cancer spreads, it most often spreads to lymph nodes near the tumor and later to the liver and bones.
What are the symptoms of Zollinger-Ellison syndrome?
Extra stomach acid can cause symptoms similar to those of peptic ulcer disease and GERD, as well as other symptoms. Common symptoms of Zollinger-Ellison syndrome include
- diarrhea, which may sometimes be the only symptom
- burning or dull pain in the abdomen, or belly, between the navel and middle of the chest
- heartburn
- nausea or vomiting
- weight loss
 Common symptoms of Zollinger-Ellison syndrome include abdominal pain and heartburn.
Common symptoms of Zollinger-Ellison syndrome include abdominal pain and heartburn.You should see a doctor right away if you have symptoms such as
- chest pain
- persistent vomiting
- problems breathing
- problems or pain while swallowing
- signs of bleeding in the digestive tract
- sudden, sharp stomach pain that doesn’t go away
- weakness or feeling faint
These could be signs of a complication or another serious health problem.
What causes Zollinger-Ellison syndrome?
Tumors, called gastrinomas, that form mainly in the pancreas and duodenum cause Zollinger-Ellison syndrome. Gastrinomas release large amounts of a hormone called gastrin. Normally, your body releases a small amount of gastrin after you eat, and gastrin triggers your stomach to make acid. When gastrinomas release large amounts of gastrin, your stomach makes too much acid, which leads to Zollinger-Ellison syndrome.
In most cases of Zollinger-Ellison syndrome, experts don’t know what causes the gastrinomas to form. In about 20% to 25% of cases, a rare genetic disorder called MEN1 causes gastrinomas to form.3
How do doctors diagnose Zollinger-Ellison syndrome?
Doctors will perform a physical exam and ask about your symptoms, medical history, and family medical history. Your doctor may suspect you have Zollinger-Ellison syndrome if you have certain symptoms and signs, such as
- chronic diarrhea that occurs along with GERD or peptic ulcer disease
- peptic ulcer disease that usually is chronic, comes back repeatedly, and is severe or leads to complications
- peptic ulcer disease without Helicobacter pylori (H. pylori) infection or without a history of nonsteroidal anti-inflammatory drug (NSAID) use
- personal or family history of MEN1 or MEN1 symptoms
If your doctor suspects you may have Zollinger-Ellison syndrome, he or she will order tests to diagnose this condition.
What tests do doctors use to diagnose Zollinger-Ellison syndrome?
Doctors may order the following tests to diagnose Zollinger-Ellison syndrome and find the tumors that cause this condition.
Blood tests
For a blood test, a health care professional will take a blood sample from you and send the sample to a lab.
Doctors may order a blood test to check gastrin levels in your blood after you fast—have nothing to eat or drink except water—for several hours. High gastrin levels could be a sign of Zollinger-Ellison syndrome. Doctors may order another blood test to check gastrin levels after you receive intravenous (IV) secretin—a hormone that causes gastrinomas to produce more gastrin.
Your doctor may ask you to stop or change the medicines you take before these tests. Certain medicines, such as proton pump inhibitors (PPIs), may raise your gastrin levels.
Stomach acid tests
Doctors may order a test to check the pH—or acidity—of your stomach fluids. A health care professional will insert a tube through your nose, down your throat, and into your stomach to take a sample of fluid. Doctors may also measure your stomach acid pH during an upper gastrointestinal (GI) endoscopy.
In some cases, doctors may order additional tests to measure the amount of acid your stomach makes.
Upper GI endoscopy
Upper GI endoscopy is a procedure during which a doctor uses an endoscope—a flexible tube with a camera—to see the lining of your upper GI tract, including your esophagus, stomach, and duodenum. Upper GI endoscopy may show signs of Zollinger-Ellison syndrome or its complications. Doctors may also order this test to look for the tumors that cause Zollinger-Ellison syndrome.
ERCP
Endoscopic retrograde cholangiopancreatography (ERCP) is a procedure that combines upper GI endoscopy and x-rays to examine the bile ducts and pancreatic ducts.
Imaging tests
Doctors may order imaging tests to help find the tumors that cause Zollinger-Ellison syndrome. Small gastrinomas may be hard to see, and doctors may order several types of imaging tests, including
- computed tomography (CT), which uses a combination of x-rays and computer technology to create images
- magnetic resonance imaging (MRI), which takes pictures of your body’s internal organs and soft tissues without using x-rays
- radionuclide scanning, in which you receive an injection of a small amount of radioactive material, and a special camera takes pictures that highlight the radioactive material in gastrinomas
- endoscopic ultrasound, in which a doctor uses an endoscope with an ultrasound attachment to create pictures
- angiography, a special kind of x-ray in which a doctor threads a catheter through your large arteries to inject a special dye that will show up on x-rays
How do doctors treat Zollinger-Ellison syndrome?
Doctors treat Zollinger-Ellison syndrome with medicines and surgery.
Medicines
Doctors treat Zollinger-Ellison syndrome with PPIs. PPIs lower the amount of acid your stomach makes, which can relieve symptoms and promote healing. Doctors may prescribe a higher dose of PPIs when starting treatment and may lower the dose over time. Many people with Zollinger-Ellison syndrome need lifelong treatment with PPIs.
PPIs are generally safe and effective. Side effects, while uncommon, may include headache, diarrhea, and upset stomach. Long-term use of PPIs to treat Zollinger-Ellison syndrome may lead to low levels of vitamin B12. Experts are still studying the effects of taking PPIs for a long time or in high doses. Talk with your doctor about the risks and benefits of these medicines.
 Doctors treat Zollinger-Ellison syndrome with PPIs.
Doctors treat Zollinger-Ellison syndrome with PPIs.Surgery
Doctors may recommend surgery to remove the tumors that cause Zollinger-Ellison syndrome in people who don’t have MEN1. In some cases, removing the gastrinomas will cure Zollinger-Ellison syndrome and prevent the tumors from spreading to other parts of the body. After surgery, people may still need to take PPIs to control stomach acid.
In people who have MEN1, doctors don’t typically recommend surgery to remove the tumors that cause Zollinger-Ellison syndrome, especially if the gastrinomas are relatively small. People with MEN1 often have many small tumors, making it difficult for surgeons to find and remove them all. Doctors may recommend surgery to remove any larger tumors, which have a higher chance of spreading to other parts of the body.
How do doctors prevent and treat the complications of Zollinger-Ellison syndrome?
Treating Zollinger-Ellison syndrome reduces the amount of acid in the stomach, which can help prevent or treat complications related to peptic ulcers or acid reflux.
If gastrinomas are cancerous and spread to the liver, bone, or other parts of the body, doctors may recommend chemotherapy, surgery, or other cancer treatments.
Clinical Trials for Zollinger-Ellison Syndrome
The NIDDK conducts and supports clinical trials in many diseases and conditions, including digestive diseases. The trials look to find new ways to prevent, detect, or treat disease and improve quality of life.
What are clinical trials for Zollinger-Ellison syndrome?
Clinical trials—and other types of clinical studies—are part of medical research and involve people like you. When you volunteer to take part in a clinical study, you help doctors and researchers learn more about disease and improve health care for people in the future.
Researchers are studying many aspects of Zollinger-Ellison syndrome, including improved ways to diagnose and treat this condition.
Find out if clinical studies are right for you.
Watch a video of NIDDK Director Dr. Griffin P. Rodgers explaining the importance of participating in clinical trials.
What clinical studies for Zollinger-Ellison syndrome are looking for participants?
You can view a filtered list of clinical studies on Zollinger-Ellison syndrome that are federally funded, open, and recruiting at ClinicalTrials.gov. You can expand or narrow the list to include clinical studies from industry, universities, and individuals; however, the National Institutes of Health does not review these studies and cannot ensure they are safe. Always talk with your health care provider before you participate in a clinical study.
References
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
The NIDDK would like to thank:
Robert T. Jensen, M.D., Gastrointestinal Cell Biology Section, Digestive Diseases Branch, NIDDK

